Non-COVID #pulmonary teaching: a young man recently diagnosed with asthma comes to clinic with progressive dyspnea on exertion. Despite treatment with an inhaled corticosteroid (ICS) & short acting bronchodilator (SABA), he feels worse. CXR & spirometry are shown. #FOAMed
1/


1/



What would you like to do next?
2/
2/
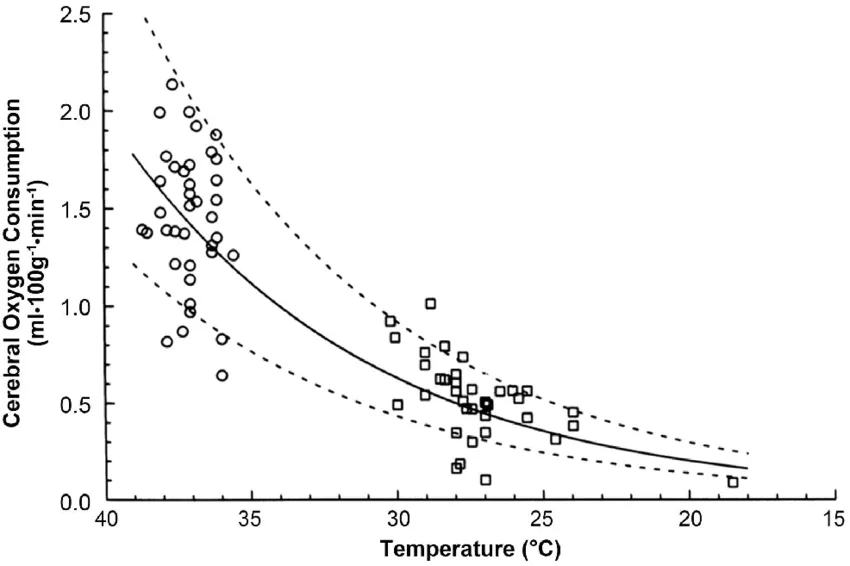
The key to this case is recognizing a distinctive abnormality in the flow-volume loop, specifically the truncation of both the inspiratory & expiratory flows.
This is characteristic of a fixed obstruction, which can occur with external compression or stenosis of the trachea.
3/

This is characteristic of a fixed obstruction, which can occur with external compression or stenosis of the trachea.
3/


Now back to our patient - what could be causing his obstruction?
Let’s inquire about B-symptoms (malignancy) and symptoms of hyper/hypothyrodism. We can also ask about prior intubations (a cause tracheal stenosis) or other past airway issues.
4/
Let’s inquire about B-symptoms (malignancy) and symptoms of hyper/hypothyrodism. We can also ask about prior intubations (a cause tracheal stenosis) or other past airway issues.
4/
A careful physical exam can also help diagnose a tracheal obstruction; in contrast to asthma
* wheezing may loudest over the central chest or neck
* wheezing may be polyphonic instead of monophonic
For example:
➡️
➡️
5/
* wheezing may loudest over the central chest or neck
* wheezing may be polyphonic instead of monophonic
For example:
➡️
➡️
5/
A careful thyroid & LN exam may identify abnormalities, in this case an asymmetric enlarged thyroid.
Have the patient lift their arms; if their face becomes plethoric it suggests thoracic inlet obstruction impairing venous return (Pemberton’s sign).
➡️academic.oup.com/jcem/article/9…
5/
Have the patient lift their arms; if their face becomes plethoric it suggests thoracic inlet obstruction impairing venous return (Pemberton’s sign).
➡️academic.oup.com/jcem/article/9…
5/

Next, a CT scan of the chest & neck revealed a large heterogenous anterior neck mass compressing the trachea.
The mass was biopsied and papillary thyroid cancer was diagnosed. He underwent resection and was cured. His dyspnea and wheezing resolved completely.
6/

The mass was biopsied and papillary thyroid cancer was diagnosed. He underwent resection and was cured. His dyspnea and wheezing resolved completely.
6/


Asthma is common but misdiagnosis is surprisingly common too. One study found up to 41% of “asthmatics” did not meet diagnostic criteria.
➡️pubmed.ncbi.nlm.nih.gov/15045041/
It is prudent to confirm the diagnosis w/ PFTs. Failure to respond to Tx should prompt consideration of mimics.
7/
➡️pubmed.ncbi.nlm.nih.gov/15045041/
It is prudent to confirm the diagnosis w/ PFTs. Failure to respond to Tx should prompt consideration of mimics.
7/
To summarize what we’ve learned:
* fixed airway obstruction can cause dyspnea & wheezing, mimicking asthma; history & exam can help differentiate
* look at flow volume loops on PFTs & remember the patterns seen w/ fixed obstruction
* confirm asthma dx before escalating therapy
8/
* fixed airway obstruction can cause dyspnea & wheezing, mimicking asthma; history & exam can help differentiate
* look at flow volume loops on PFTs & remember the patterns seen w/ fixed obstruction
* confirm asthma dx before escalating therapy
8/

Alternatively, we can boil this down to two proverbs:
* “Not all that wheezes is bronchial asthma”
- Chevalier Jackson (otolaryngologist)
* "Доверя́й, но проверя́й // Doveryáy, no proveryáy"
- translation: Trust but verify (Russian Proverb)
9/
* “Not all that wheezes is bronchial asthma”
- Chevalier Jackson (otolaryngologist)
* "Доверя́й, но проверя́й // Doveryáy, no proveryáy"
- translation: Trust but verify (Russian Proverb)
9/
• • •
Missing some Tweet in this thread? You can try to
force a refresh