I still see the persistent, but incorrect, claim that control measures just delay - rather than reduce - the impact of an epidemic. A thread on the problem of 'overshoot'... 1/
This claim seems to arise from a misunderstanding about two related, but different metrics: the % of people infected during an epidemic, and the point at which immunity leads to a decline in transmission. 2/
In an uncontrolled epidemic, 'herd immunity' is reached at the peak (because R<1 after this point), which means the final % infected is generally much larger than the herd immunity threshold. (Below from: science.sciencemag.org/content/368/64…) 3/ 
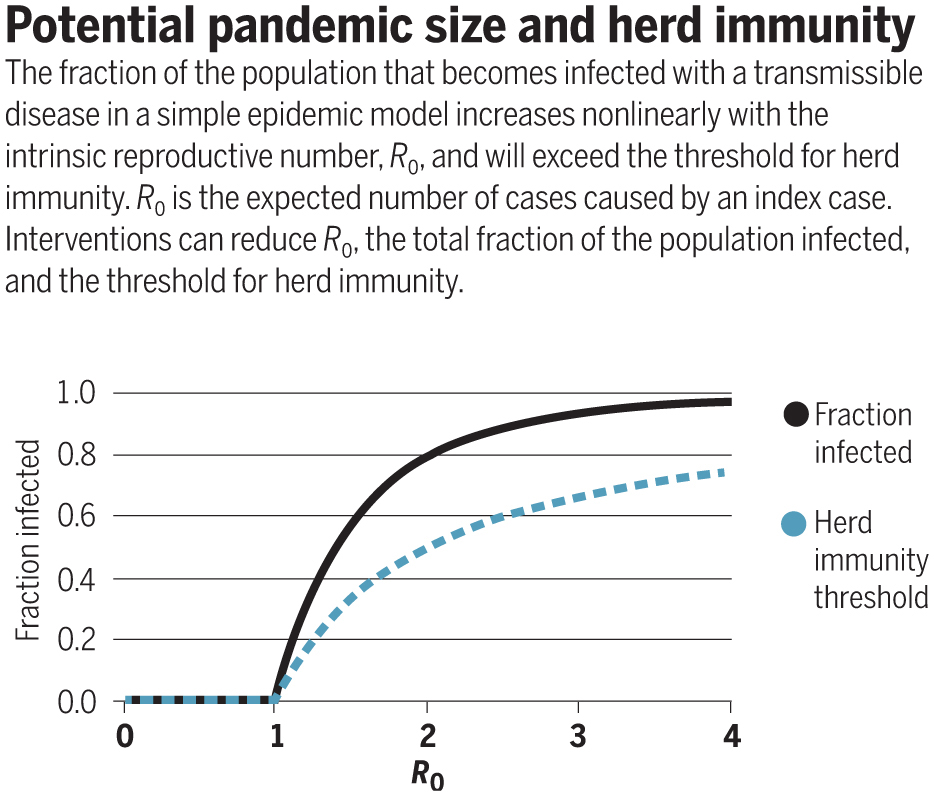
Population structure (e.g. variation in connectivity/susceptibility) can change these values - below shows difference variation can make in models (medrxiv.org/content/10.110…). But overall message is same – larger % is infected in uncontrolled epidemic than required to get R<1. 4/ 
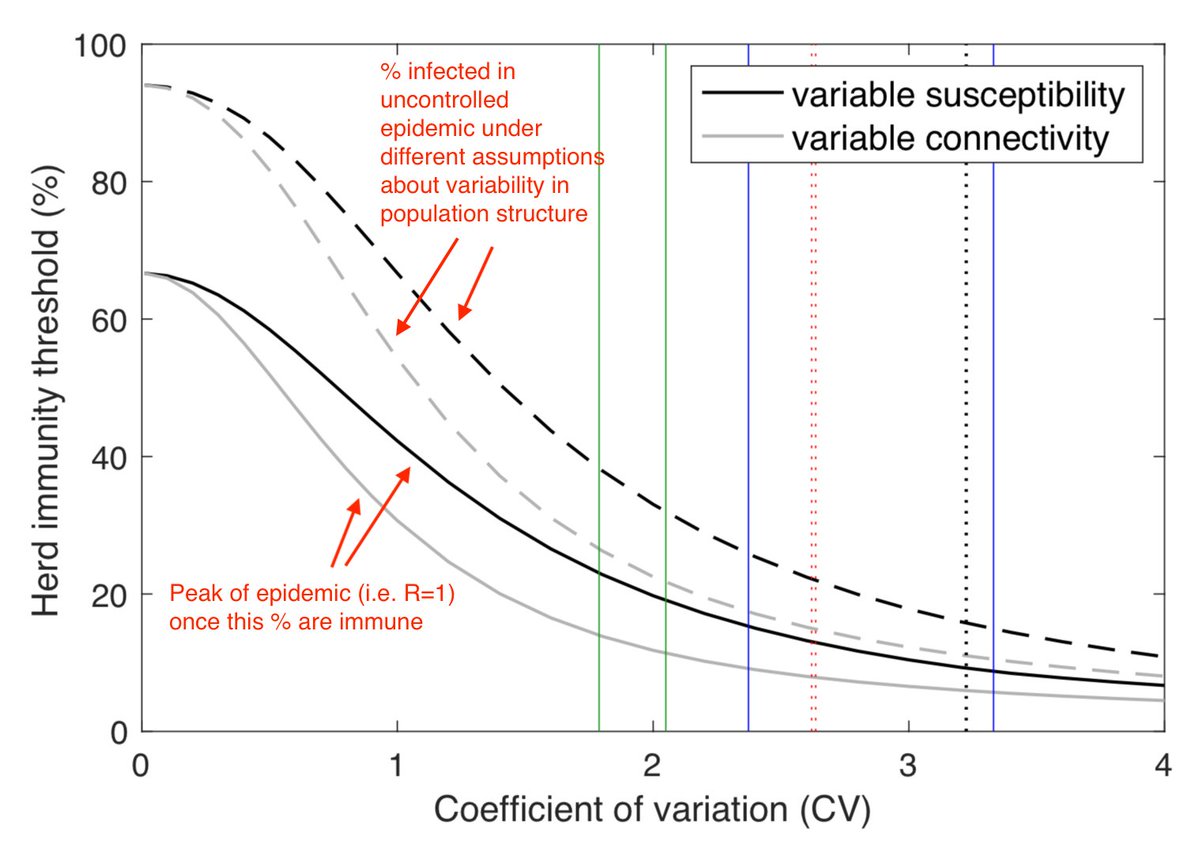
As a hypothetical example, suppose we have an epidemic that would have infected 60% of the population without control measures. For this example, both of above plots imply herd immunity would have been reached when 35-40% acquired immunity. 5/
As a hypothetical example, suppose we have an epidemic that would have infected 60% of the population without control measures. For this specific made-up example, both of above models imply herd immunity would have been reached once 35-40% acquired immunity. 5/ 

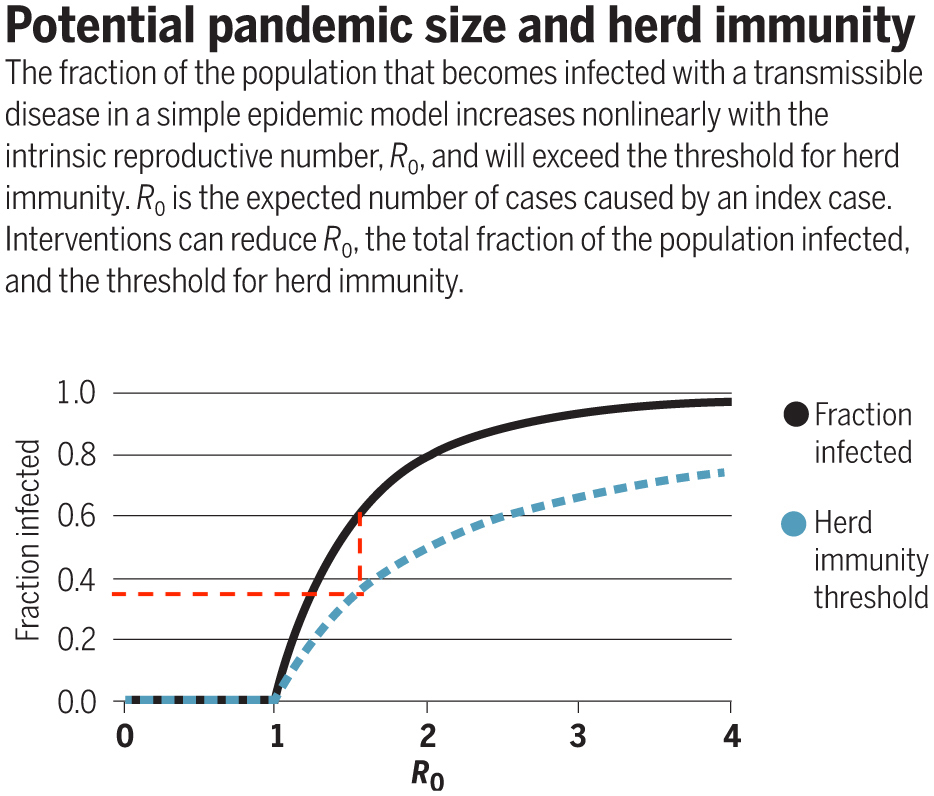
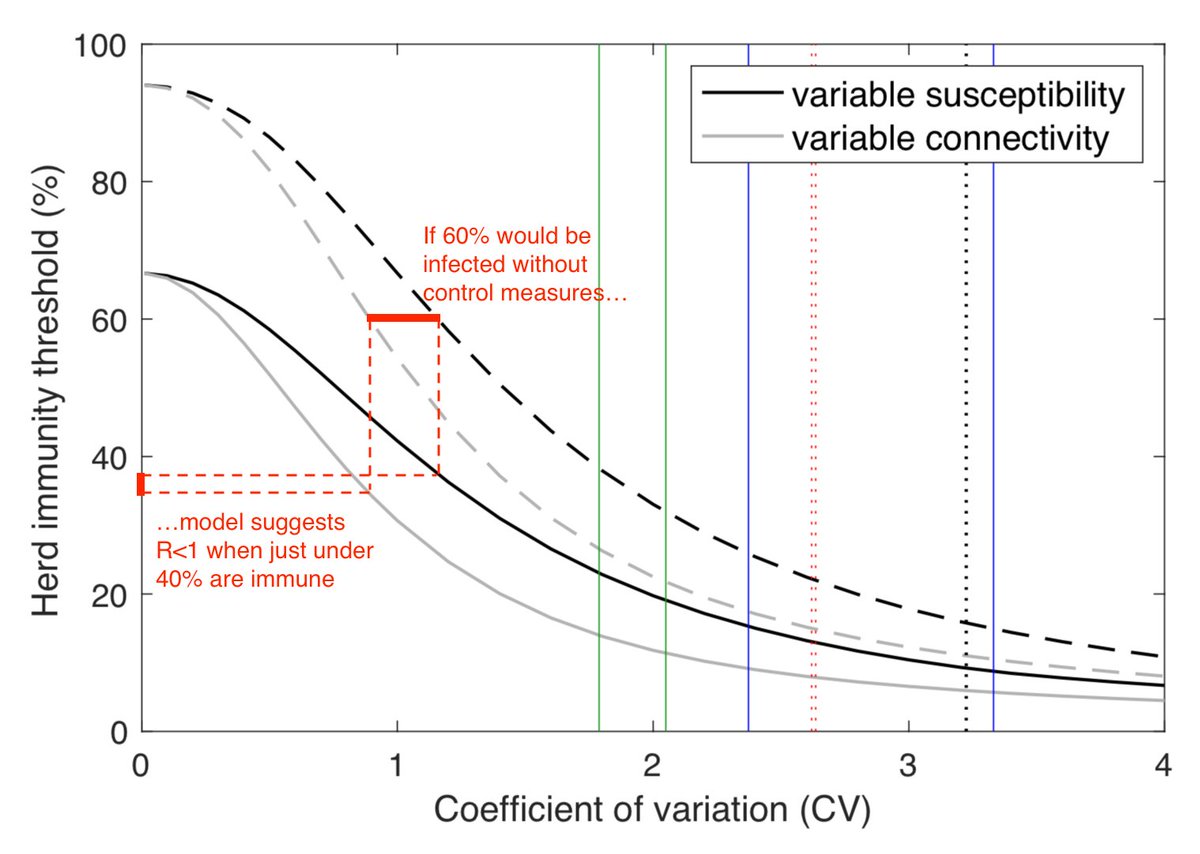
In other words, there's overshoot of 20-25% in this example, i.e. people infected after the epidemic peaked and R was below 1. With control measures, initial R would be lower, which means peak occurs when % infected is below immunity threshold, reducing eventual overshoot. 6/
The exact % values aren't the key point here - the point is that *even if an epidemic isn't sustainably controllable in a population and will end in herd immunity, control measures can still massively reduce the disease burden sustained along the way*. 7/
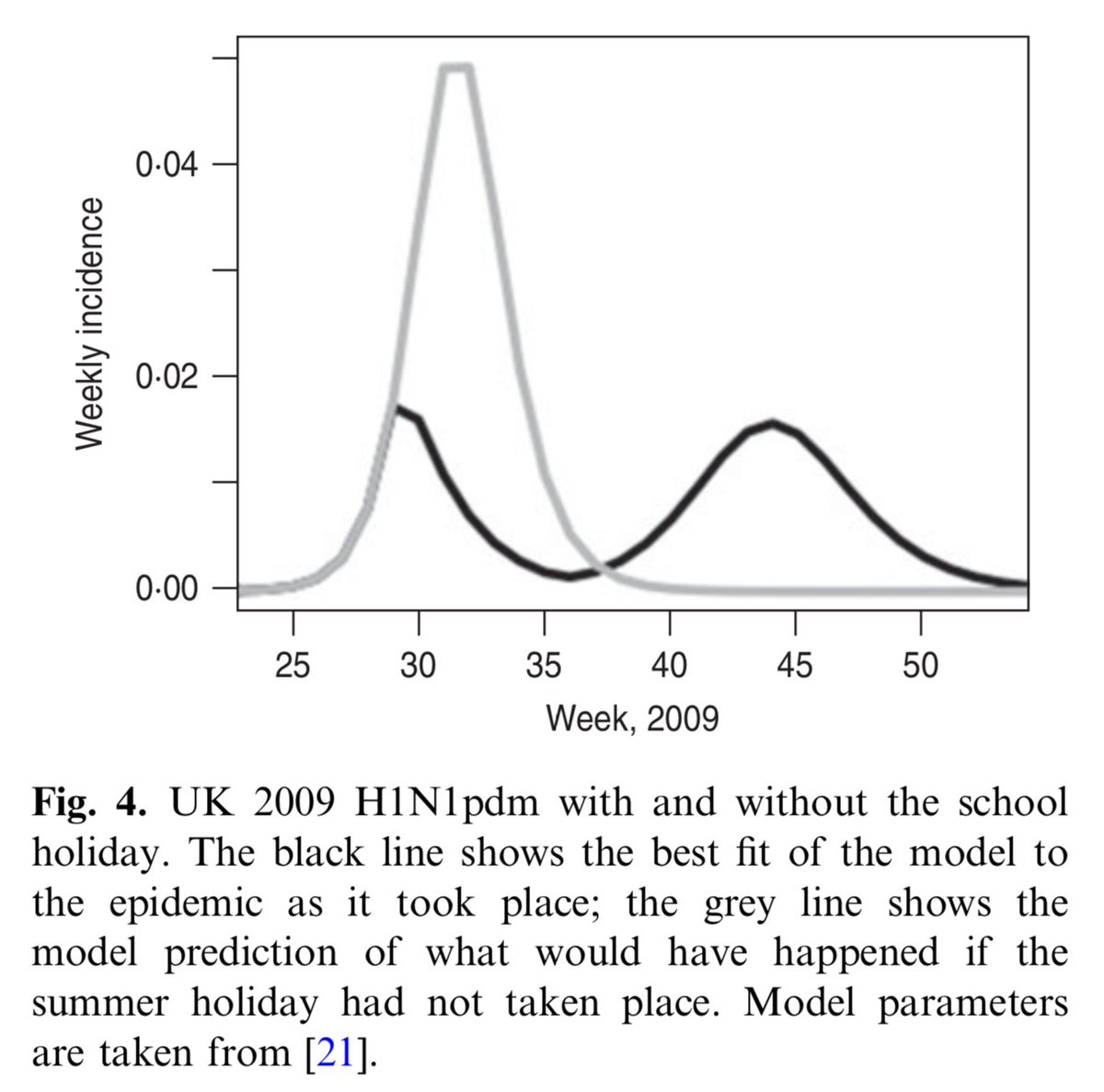
As a tangible example of behaviour change reducing overshoot, take the 2009 flu pandemic in UK, where school summer holidays interrupted transmission. Had this not happened, it's been estimated epidemic would've infected 20% more people than it did: cambridge.org/core/journals/… 8/ 
For context, there are now several reports where % of community with antibodies to SARS-CoV-2 is around the 40-70% range, e.g. parts of Mumbai (tifr.res.in/TSN/article/Mu…), Iquitos (researchgate.net/publication/34…), Ecuador (academic.oup.com/cid/advance-ar…), Maranhao (medrxiv.org/content/10.110…)... 9/
...Karachi (ncbi.nlm.nih.gov/pmc/articles/P…), Ischgl (medrxiv.org/content/10.110…), NYC (nytimes.com/2020/08/19/nyr…). But as above shows, it doesn't mean control measures made no difference. 10/
And finally, a note on what happens next in populations where a sufficient % have been infected to reduce R below 1:
https://twitter.com/AdamJKucharski/status/1282975978915012608?s=2011/11
• • •
Missing some Tweet in this thread? You can try to
force a refresh
















