Some thoughts on the evolutionary trajectory of SARS-CoV-2 so far, how it compares to other viruses, and what might happen next... 1/
For seasonal coronaviruses & flu, we see a pattern of 'antigenic turnover' over time - circulating viruses give rise to new variants that escape prior immunity against infection, immunity builds against these new variants, then these in turn spawn new variants... 2/
When infections evolve to escape immunity like this, we typically end up with an evolutionary tree that looks like a lopsided ladder as new variants sequentially replace their 'parent' variant lineages (below from: journals.plos.org/ploscompbiol/a…) 3/ 

For example, below shows trees for seasonal coronavirus 229E and seasonal flu virus A/H3N2
(below from @eguia_rachel @jbloom_lab et al journals.plos.org/plospathogens/… & @nextstrain) 4/

(below from @eguia_rachel @jbloom_lab et al journals.plos.org/plospathogens/… & @nextstrain) 4/


After the emergence of the 2009 pandemic influenza A/H1N1p virus, it settled into a similar pattern of antigenic turnover that has continued since (below from: nature.com/articles/s4159…) 5/ 

But so far we haven't seen this pattern for SARS-CoV-2... Omicron didn't emerge from the Delta lineage and Delta didn't emerge from the Alpha, Beta or Gamma lineages (below from nextstrain.org/ncov/gisaid/gl…) 6/ 
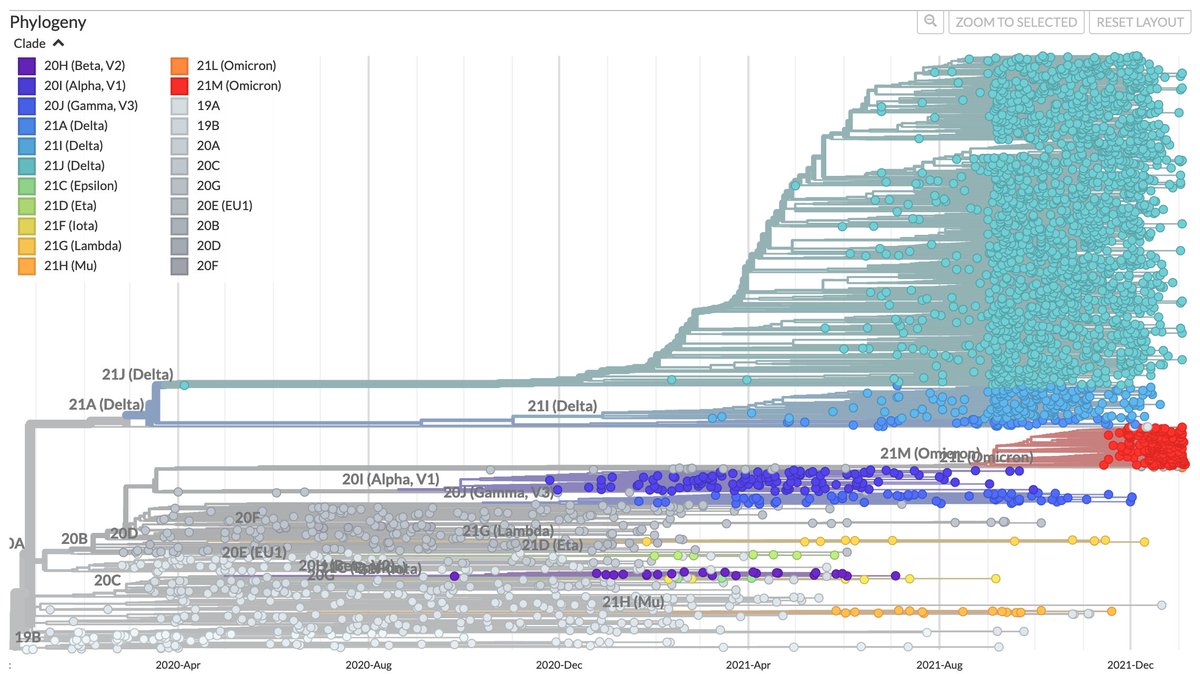
Given that we have to go far back to find a common ancestor between VOCs and other circulating variants, one hypothesis is that they emerged in individuals with a chronic infection:
https://twitter.com/MoritzGerstung/status/1464287402038640647?s=207/
Regardless of exact origins, this pattern means we shouldn't assume next variant of interest/concern will emerge from current circulating Omicron viruses - like other variants, it may well have already evolved (or be evolving) somewhere, from a much older ancestor lineage. 8/
I think seasonal coronaviruses and influenza are a sensible 'prior' to bear in mind for what long-term dynamics of antigenic turnover of SARS-CoV-2 could look like. But we also need to remember this process of sequential turnover isn't what's happened so far... 9/
Reduction in global travel may also have influenced variant dynamics globally so far – and subsequent reopening may change this, as there is less potential for 'evolutionary villages' that are relatively cut off from global dynamics. 10/
This uncertainty illustrates the importance of having good surveillance coverage of genomic variation of SARS-CoV-2 globally, optimised to make best use of resources (e.g. medrxiv.org/content/10.110…) as well as ongoing synthesis of available data. 11/11
Final note: above all refers to immunity that reduces transmission, as this is what shapes ability of new variants to spread (and hence successfully replace existing ones).
• • •
Missing some Tweet in this thread? You can try to
force a refresh
















