
Metatarsalgia Treatment:
A (Non-Exhaustive) Overview Thread 🧵
🔸Off loading
🔸Simple analgesia
🔸Physiotherapy
🔸Lifestyle changes
🔸Onwards referral
1/10
Link to diagnosis thread below 👇🏼

A (Non-Exhaustive) Overview Thread 🧵
🔸Off loading
🔸Simple analgesia
🔸Physiotherapy
🔸Lifestyle changes
🔸Onwards referral
1/10
Link to diagnosis thread below 👇🏼
https://twitter.com/lizbayleyphysio/status/1493845121875513346?s=21

Off Loading:
Rest/activity modification
No barefoot walking/No heels 👠
Possible air cast boot for Freiburg’s or stress #
Rocker bottom shoes ⬇️ pressure through MT heads. ‘Hoka’ are a more fashionable option 😎
General:
Go for flat, wide box, roomy shoes with stiff sole👟
2/10
Rest/activity modification
No barefoot walking/No heels 👠
Possible air cast boot for Freiburg’s or stress #
Rocker bottom shoes ⬇️ pressure through MT heads. ‘Hoka’ are a more fashionable option 😎
General:
Go for flat, wide box, roomy shoes with stiff sole👟
2/10

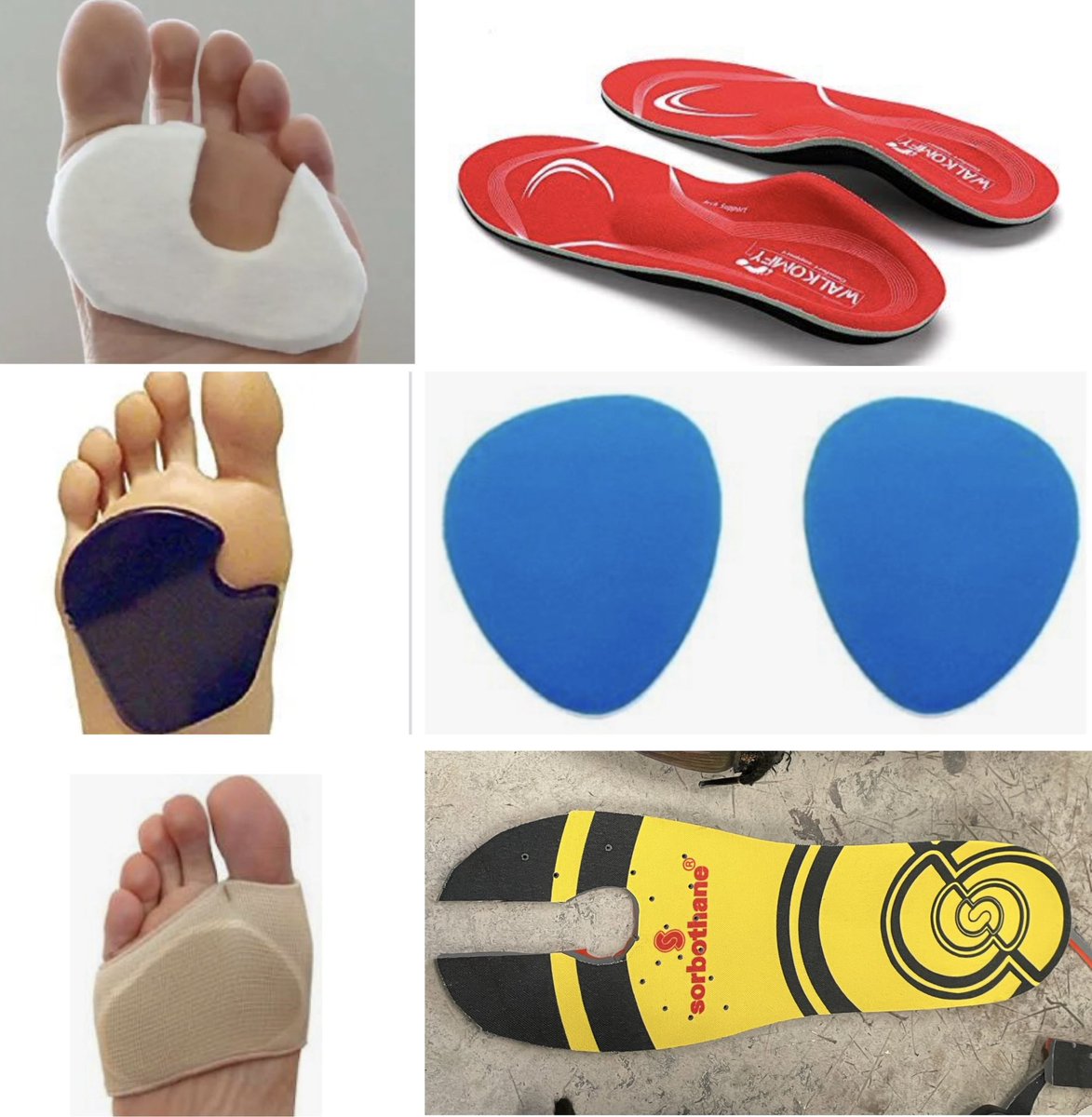
Orthotics work by changing the kinetics not the kinematics - the force but not the position. You can off load a structure without seeing a physical change🦶🏼
🔹MT dome pads (blue) placed proximal to MT heads
🔹Full or 3/4 insoles
🔹Cut out pads
🔹Gel pads for MT cushioning
3/10
🔹MT dome pads (blue) placed proximal to MT heads
🔹Full or 3/4 insoles
🔹Cut out pads
🔹Gel pads for MT cushioning
3/10
Analgesia:
Over-the-counter pain meds are useful in the initial stages of treatment when getting everything to settle down 💊 This podcast by @TPMPodcast is essential listening for any HCPs who want a better understanding of all things analgesic! podcasts.apple.com/gb/podcast/the…
4/10
Over-the-counter pain meds are useful in the initial stages of treatment when getting everything to settle down 💊 This podcast by @TPMPodcast is essential listening for any HCPs who want a better understanding of all things analgesic! podcasts.apple.com/gb/podcast/the…
4/10
Physio:
Advice + education
Calf stretching may improve MT pain because ⬇️ DF may ⬆️ load through the MT heads
While there’s evidence for stretching in plantar heel pain (@DrDylanM 2021), studies are inconclusive for its effect on MT plantar pressures pubmed.ncbi.nlm.nih.gov/31653364/
5/10
Advice + education
Calf stretching may improve MT pain because ⬇️ DF may ⬆️ load through the MT heads
While there’s evidence for stretching in plantar heel pain (@DrDylanM 2021), studies are inconclusive for its effect on MT plantar pressures pubmed.ncbi.nlm.nih.gov/31653364/
5/10

Cont:
Addressing impairments in the kinetic chain including foot strength & control may form part of a Rx plan 🦶🏼🏋️♀️
A graded return to activity is fundamental particularly in cases such as stress #
Taping can help to off load the MT head or foot arch:
6/10
Addressing impairments in the kinetic chain including foot strength & control may form part of a Rx plan 🦶🏼🏋️♀️
A graded return to activity is fundamental particularly in cases such as stress #
Taping can help to off load the MT head or foot arch:
https://twitter.com/lizbayleyphysio/status/1401578920013598721?s=21
6/10

Lifestyle:
Changes in diet & reduced alcohol consumption is recommended to help prevent flare ups in gout:
pubmed.ncbi.nlm.nih.gov/25591183/
Weight loss may be beneficial for compressive conditions such as Morton’s Neuroma.
7/10
Changes in diet & reduced alcohol consumption is recommended to help prevent flare ups in gout:
pubmed.ncbi.nlm.nih.gov/25591183/
Weight loss may be beneficial for compressive conditions such as Morton’s Neuroma.
7/10
Referral:
Consider referral to a podiatrist🦶🏼
For suspected inflamm. conditions refer direct to Rheumatology or to GP for further investigation & referral where appropriate.
Gout can be managed in primary care with meds such as Colchicine.
Joint aspiration will confirm Dx.
8/10
Consider referral to a podiatrist🦶🏼
For suspected inflamm. conditions refer direct to Rheumatology or to GP for further investigation & referral where appropriate.
Gout can be managed in primary care with meds such as Colchicine.
Joint aspiration will confirm Dx.
8/10

Cont…
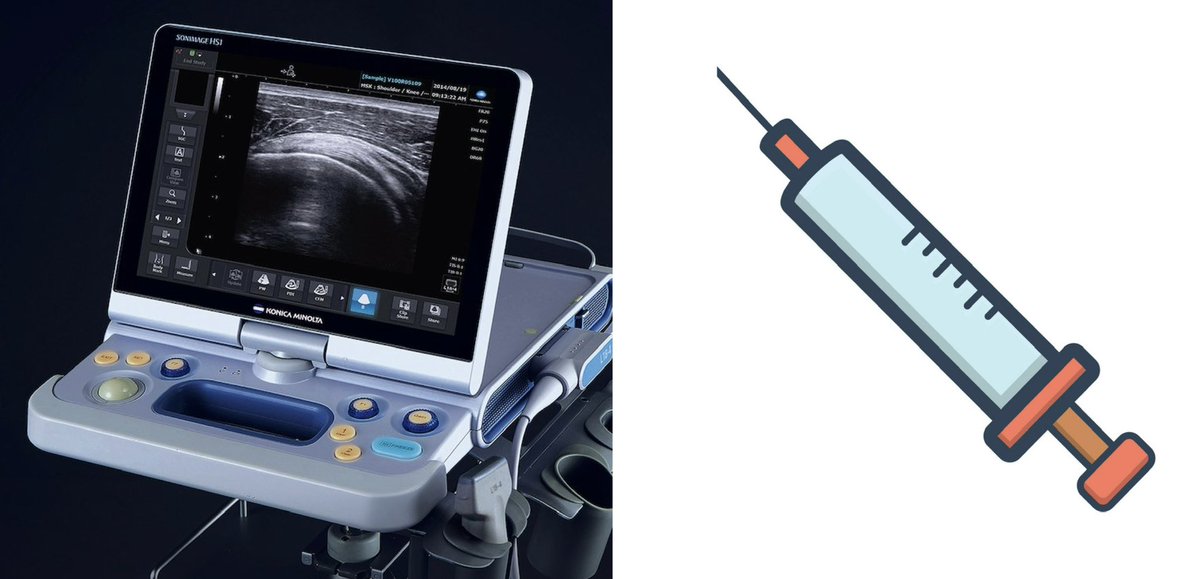
Consultant ortho/SEM/podiatrist can facilitate accurate diagnosis with POCUS/MRI and discuss surgical options. CSI can be useful e.g. neuroma, but in some cases risk outweighs benefits e.g. it might cause instability in already weakened joints - synovitis/Freiburg’s.
9/10
Consultant ortho/SEM/podiatrist can facilitate accurate diagnosis with POCUS/MRI and discuss surgical options. CSI can be useful e.g. neuroma, but in some cases risk outweighs benefits e.g. it might cause instability in already weakened joints - synovitis/Freiburg’s.
9/10
References:
pubmed.ncbi.nlm.nih.gov/29362036/
pubmed.ncbi.nlm.nih.gov/28109624/
pubmed.ncbi.nlm.nih.gov/31653364/
pubmed.ncbi.nlm.nih.gov/25591183/
bjsm.bmj.com/content/55/19/…
Thanks for reading 🤓👉🏼🦶🏼👈🏼
10/10
pubmed.ncbi.nlm.nih.gov/29362036/
pubmed.ncbi.nlm.nih.gov/28109624/
pubmed.ncbi.nlm.nih.gov/31653364/
pubmed.ncbi.nlm.nih.gov/25591183/
bjsm.bmj.com/content/55/19/…
Thanks for reading 🤓👉🏼🦶🏼👈🏼
10/10
🦶🏼
@chandlerscottPT @SurgeonFRCPodS @Joeod86 @laurenswakamisa @drvenkimdrd @AshimaMakol @dflemosmd @noelthatcher @drchrisnorris @pipwhitept @DrJN_SportsMed @arranz_jimenez @k8purcellphysio @WestbyPT @mcrebbin @EguezMaphfer @surajbafna91 @lillyscott04 @LisaHoglund1 @FraserMckinney
@chandlerscottPT @SurgeonFRCPodS @Joeod86 @laurenswakamisa @drvenkimdrd @AshimaMakol @dflemosmd @noelthatcher @drchrisnorris @pipwhitept @DrJN_SportsMed @arranz_jimenez @k8purcellphysio @WestbyPT @mcrebbin @EguezMaphfer @surajbafna91 @lillyscott04 @LisaHoglund1 @FraserMckinney
@threadreaderapp unroll please 😋🌀
• • •
Missing some Tweet in this thread? You can try to
force a refresh





