1/
Just how much can ultrasonography reveal about the neurovascular health of the brain?
A whole freaking lot!!
A #ContinuumCase about a man with transient dizziness after doing heavy lifting in the yard. @ContinuumAAN @LyellJ
Just how much can ultrasonography reveal about the neurovascular health of the brain?
A whole freaking lot!!
A #ContinuumCase about a man with transient dizziness after doing heavy lifting in the yard. @ContinuumAAN @LyellJ

2/
There are a lot of way this case could unfold…
Was he just dehydrated?
Did he have a dissection?
Have a PE?
But with more questions, it becomes clear that this has happened before.
Whenever he is doing heavy lifting, his left arm becomes tingly & then the room spins 🤔
There are a lot of way this case could unfold…
Was he just dehydrated?
Did he have a dissection?
Have a PE?
But with more questions, it becomes clear that this has happened before.
Whenever he is doing heavy lifting, his left arm becomes tingly & then the room spins 🤔
3/
#NeuroTwitter, what's going on?
#NeuroTwitter, what's going on?
4/
The interesting thing about his symptoms are that they're stereotyped. Most vascular events are not stereotyped, maybe you get events that localize to the same hemisphere or vascular territory, but the exact same events??
Arm exercise and then dizziness??
The interesting thing about his symptoms are that they're stereotyped. Most vascular events are not stereotyped, maybe you get events that localize to the same hemisphere or vascular territory, but the exact same events??
Arm exercise and then dizziness??
6/
Contralaterally, things aren't really looking great either.
Thats a very tight stenosis of the R ICA.
Contralaterally, things aren't really looking great either.
Thats a very tight stenosis of the R ICA.

7/
TCDs demonstrate intracranial collateralization through the AComm, with inverted flow in the L A1.
So the L anterior circulation is largely supplied by the R critically stenosed ICA.😱😱
TCDs demonstrate intracranial collateralization through the AComm, with inverted flow in the L A1.
So the L anterior circulation is largely supplied by the R critically stenosed ICA.😱😱

8/
But…. The guy did not present with transient right arm weakness or aphasia- symptoms of poor perfusion to the left hemisphere
& while you could make a case for artery-to-arty embolization from the R ICA to the R hemisphere to explain the L arm parestheisas.... why recurrent?
But…. The guy did not present with transient right arm weakness or aphasia- symptoms of poor perfusion to the left hemisphere
& while you could make a case for artery-to-arty embolization from the R ICA to the R hemisphere to explain the L arm parestheisas.... why recurrent?
9/
And why the dizziness?
The answer…?
Inverted flow in the left vertebral artery!! And bidirection flow in the proximal basilar.

And why the dizziness?
The answer…?
Inverted flow in the left vertebral artery!! And bidirection flow in the proximal basilar.

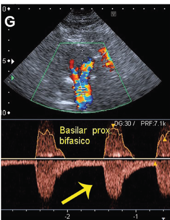
10/
What was happening?
MRA (not published in the issue, so I borrowed an example from our friends @radiopaedia.) confirmed severe stenosis of the proximal subclavian. His symptoms?
A subclavian steal effect!
What was happening?
MRA (not published in the issue, so I borrowed an example from our friends @radiopaedia.) confirmed severe stenosis of the proximal subclavian. His symptoms?
A subclavian steal effect!

11/
If subclavian steal is confusing, I like this diagram.
All suggested by a simple non-invasive, radiation free workup.
Patient underwent smoking cessation, lipid control and revascularization.
If subclavian steal is confusing, I like this diagram.
All suggested by a simple non-invasive, radiation free workup.
Patient underwent smoking cessation, lipid control and revascularization.

12/
12/
But wait!
There was one more thing!
Lets go back to the very first image... He had one more stroke risk factor.
Can you tell? (I know some of you probably did in the first poll!)
12/
But wait!
There was one more thing!
Lets go back to the very first image... He had one more stroke risk factor.
Can you tell? (I know some of you probably did in the first poll!)

13/
Yes! An irregular heart rate suggestive of (EKG confirmed) occult a fib! All that. Just from ultrasound. Isn’t it amazing what neurosonography can do?!
All about it in this issue of @ContinuumAAN
journals.lww.com/continuum/Full…
Yes! An irregular heart rate suggestive of (EKG confirmed) occult a fib! All that. Just from ultrasound. Isn’t it amazing what neurosonography can do?!
All about it in this issue of @ContinuumAAN
journals.lww.com/continuum/Full…
• • •
Missing some Tweet in this thread? You can try to
force a refresh












