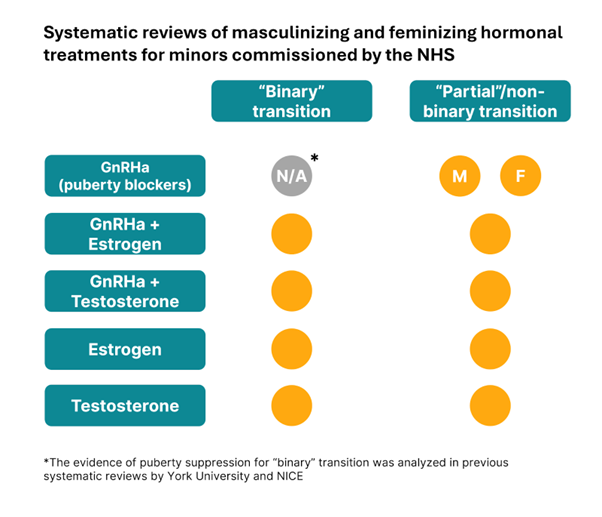
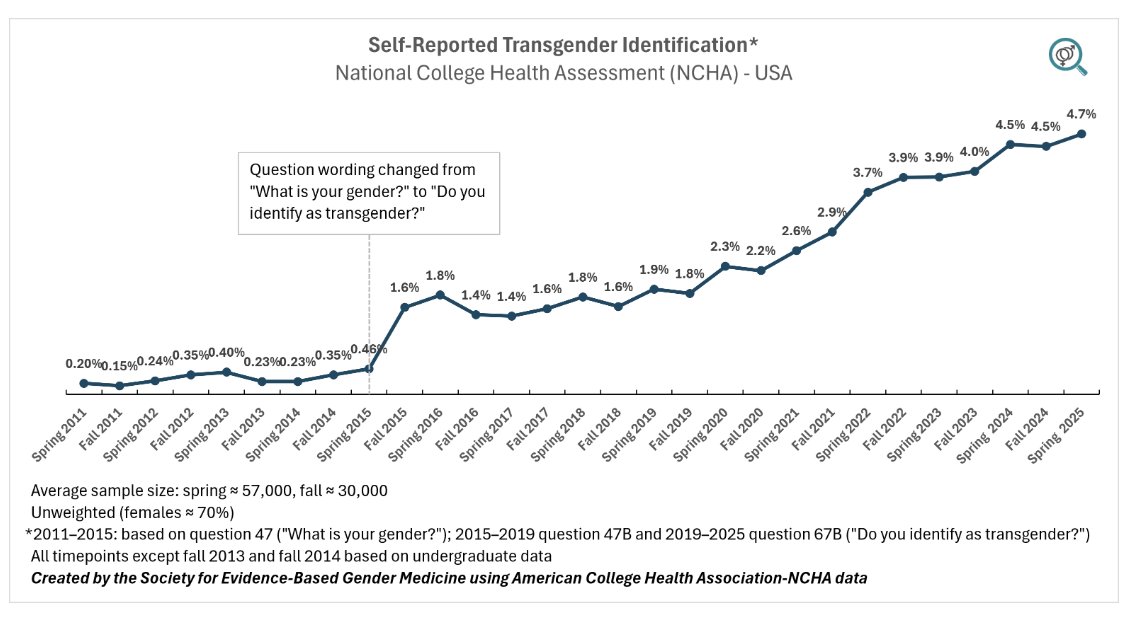
The @NHSEngland landmark decision to stop using puberty blockers for gender dysphoric youth raises a key question: what do we know about the effects of puberty blockers on adolescent development?
Prof. Sallie Baxendale explored this question at @segm_ebm 2023 conference./1🧵
Prof. Sallie Baxendale explored this question at @segm_ebm 2023 conference./1🧵
"Extraordinary claims demand extraordinary evidence" wrote Prof. Baxendale in a piece describing her research. "The only extraordinary evidence here is the gaping chasm of knowledge, or even apparent curiosity, of the clinicians who continue to chant 'safe and completely reversible' as they prescribe these medications to the children in their care." /2
unherd.com/2024/02/why-di…
unherd.com/2024/02/why-di…
Following the preview of her research at @segm_ebm conference, Prof. Baxendale published her findings about the known effects of puberty blockers
on neuropsychological function in a peer-reviewed journal.
Prof. Baxendale later shared that in her 3 decades of academic publishing, the submission of the paper was truly a unique experience. She was not concerned that the paper had been rejected 3 times prior to being accepted. Rather, it was the nature of the rejections, which appeared to be ideologically driven. /3
onlinelibrary.wiley.com/doi/full/10.11…
on neuropsychological function in a peer-reviewed journal.
Prof. Baxendale later shared that in her 3 decades of academic publishing, the submission of the paper was truly a unique experience. She was not concerned that the paper had been rejected 3 times prior to being accepted. Rather, it was the nature of the rejections, which appeared to be ideologically driven. /3
onlinelibrary.wiley.com/doi/full/10.11…

Dr. Baxendale's full presentation at @segm_ebm NYC 2023 conference is available below. We will also highlight some key moments in the rest of this thread. /4
Dr. Baxendale explores what happens when critical windows of brain development are missed, starting with her "surprise" at the assertion made by proponents of youth transitions that puberty blockers are "completely reversible." /5
Prof. Baxendale challenges the claim that puberty can be paused & resumed:
“If you deprive the brain of any input during the critical windows of opportunity, the brain will move on and whatever it was that was supposed to be developing, doesn't develop properly.” /6
“If you deprive the brain of any input during the critical windows of opportunity, the brain will move on and whatever it was that was supposed to be developing, doesn't develop properly.” /6
The process of pruning in the brain, which occurs during adolescence, is critical. It strengthens the executive function & social cognition. This process is hormonally driven: it depends on the pubertal stage, not on age. When puberty is stopped, brain development is affected./7
Prof. Baxendale's research was motivated by her surprise at the assertions by gender clinicians that "one can just pause puberty and then pick up 2-3 years later and nothing would happen," as this contradicted "everything we know about other windows of opportunity." /8
Dr. Baxendale found a paucity of studies on the effects of puberty blockers on human brains, so she turned to animal studies. What she found was that puberty blockers have “a detrimental impact on learning and the development of social behaviors and responses to stress." /9
Turning her attention to human studies, Prof. Baxendale found very few. Two studies were for the use of puberty blockers for early-onset puberty, and 3 were about stopping normally-timed puberty for gender-dysphoric youth. Several (low quality) studies signaled a drop in IQ. /10
Dr. Baxendale found no evidence that “you can pause a developmental stage and then restart it and everything will be okay.” Given all that is known about adolescent brain development, Dr. Baxendale asked a key question:
“How has this been allowed to develop as a treatment?”/11
“How has this been allowed to develop as a treatment?”/11
The @NHSEngland's decision to restrict the use of puberty blockers to clinical research, finalized this month, vindicates Prof. Baxendale, Dr. Biggs, and other researchers in the UK and worldwide who have been sounding the alarm about the proliferation of puberty blockers in general medical settings without an adequate evidence base. /12
The full lecture by Prof. Baxendale at SEGM's NYC 2023 conference is profiled on our website and our YouTube channel. See links below. /end
segm.org/NYC_2023
segm.org/NYC_2023
• • •
Missing some Tweet in this thread? You can try to
force a refresh