1/6
TRANSFUSION AS IRON THERAPY
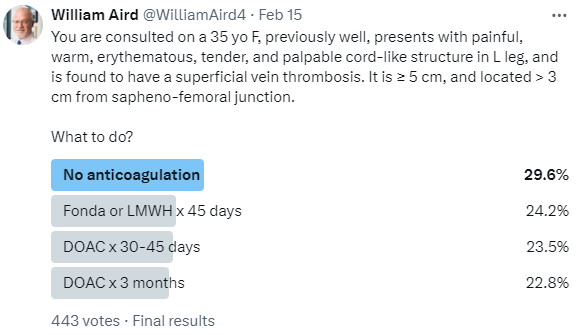
Yesterday I posted a poll showing CBC data from a patient with severe iron deficiency anemia and asked: assuming she receives 4 units pRBCs (which of course would be excessive here), does she need iron therapy on top of that?
70% answered YES.
TRANSFUSION AS IRON THERAPY
Yesterday I posted a poll showing CBC data from a patient with severe iron deficiency anemia and asked: assuming she receives 4 units pRBCs (which of course would be excessive here), does she need iron therapy on top of that?
70% answered YES.

2/6
Each unit of RBC contains about 250 mg Fe. So she will have received about 1000 mg of Fe, not far off from her total needs. However, such is iron is bound up in Hb inside the donor RBCs and is not readily accessible for erythropoiesis.
Each unit of RBC contains about 250 mg Fe. So she will have received about 1000 mg of Fe, not far off from her total needs. However, such is iron is bound up in Hb inside the donor RBCs and is not readily accessible for erythropoiesis.

3/6
I ran through some rough numbers (see graphic):
1. Oral iron will deliver about 20 mg Fe to the bone marrow each day.
I ran through some rough numbers (see graphic):
1. Oral iron will deliver about 20 mg Fe to the bone marrow each day.
4/6
2. IV iron will deliver its full payload (Fe sequestered in a carbohydrate shell) to macrophages, where Fe will leach out and be slowly released to the bone marrow (I can't find data on how much is released daily, but presumably >20 mg since response to IV Is faster vs PO).
2. IV iron will deliver its full payload (Fe sequestered in a carbohydrate shell) to macrophages, where Fe will leach out and be slowly released to the bone marrow (I can't find data on how much is released daily, but presumably >20 mg since response to IV Is faster vs PO).
5/6
3. RBCs have a turnover of about 1%/day. So if 1 L pRBCs are transfused (4 units), 10 ml will be endocytosed and processed by macrophages each day, releasing 10 mg Fe/day for use by the bone marrow (these numbers gradually diminish over time as donor cells are destroyed).
3. RBCs have a turnover of about 1%/day. So if 1 L pRBCs are transfused (4 units), 10 ml will be endocytosed and processed by macrophages each day, releasing 10 mg Fe/day for use by the bone marrow (these numbers gradually diminish over time as donor cells are destroyed).
6/6
Bottom line: while transfused RBCs provide a depot of iron, it is too little (unless >3-4 units are given) and its release is too slow to meet the demands of patients with severe iron deficiency in a timely manner - thus, such patients should also receive supplemental Fe.
Bottom line: while transfused RBCs provide a depot of iron, it is too little (unless >3-4 units are given) and its release is too slow to meet the demands of patients with severe iron deficiency in a timely manner - thus, such patients should also receive supplemental Fe.
• • •
Missing some Tweet in this thread? You can try to
force a refresh