"I had constantly bleeding colitis for more than a year, and when I took about 20 to 30 mg of lidocaine (in a 2% solution meant for oral, dental use) the symptoms stopped and haven’t returned in more than 30 years." - Ray Peat
Thread on the research👇
Thread on the research👇

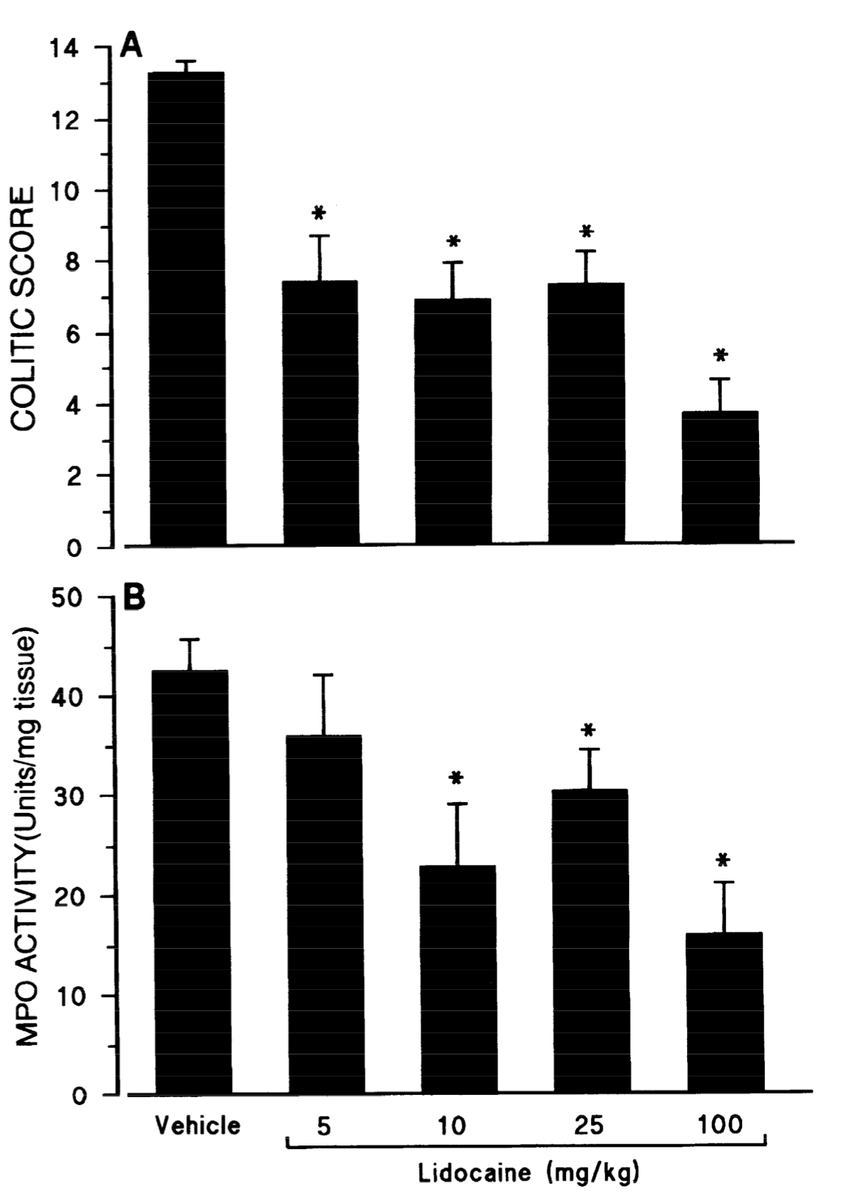
"Rats were given lidocaine intrarectally 30 min before TNBS administration."
TNBS induces colitis by triggering immune response and gut inflammation.
"Lidocaine dose dependently reduced the severity of colitis and the infiltration of granulocytes at 24 h and 7 days post-TNBS."
TNBS induces colitis by triggering immune response and gut inflammation.
"Lidocaine dose dependently reduced the severity of colitis and the infiltration of granulocytes at 24 h and 7 days post-TNBS."
"Treatment with lidocaine gel in 21 consecutive patients with ulcerative proctitis/proctosigmoiditis for 3-8 weeks caused a rapid decrease of subjective and objective symptoms. Mucosal integrity was restored, accompanied by depletion of OKT4/8 lymphocytes from the mucosa." 
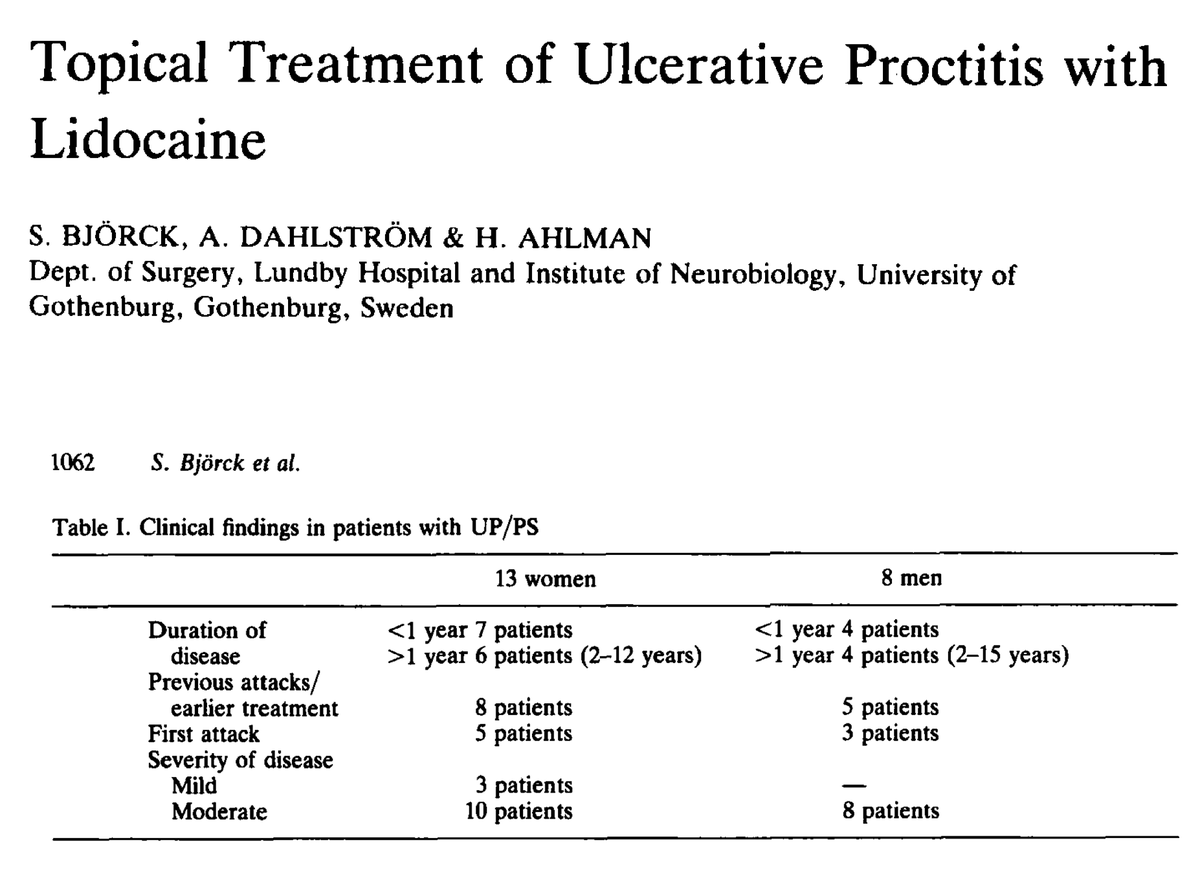
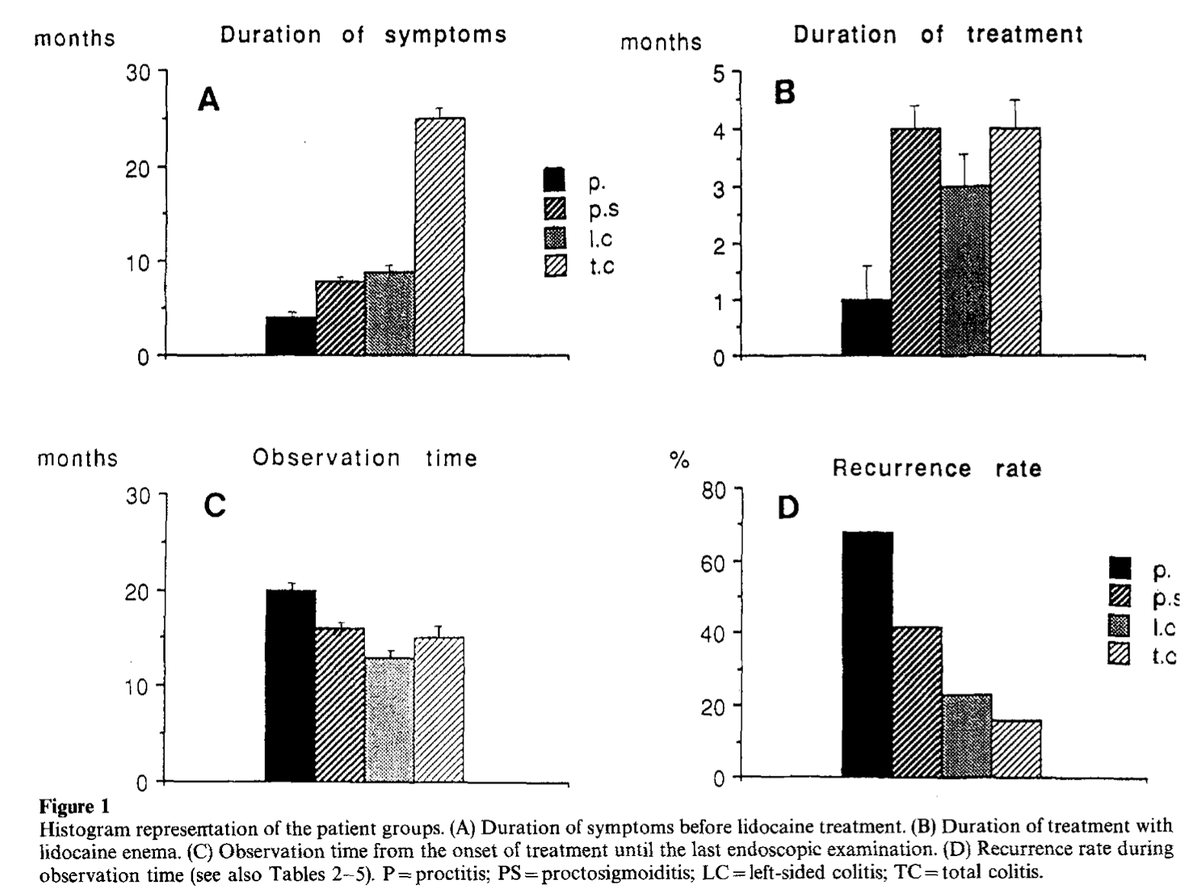
"52 patients with ulcerative proctitis or left-sided ulcerative colitis were studied."
"The patients instilled a lidocaine (2 %) gel (400 mg × 2) during 4 to 8 wk. Rectal biopsies were taken before and every 2 to 3 wk after onset of treatment."
"The patients instilled a lidocaine (2 %) gel (400 mg × 2) during 4 to 8 wk. Rectal biopsies were taken before and every 2 to 3 wk after onset of treatment."

“During continuous treatment all patients normalized their bowel function.
Topical treatment of the rectal mucosa with lidocaine in patients with UC/UP resulted in rapid symptomatic relief, restored mucosal integrity, and caused extravasal lymphocytes to disappear.”
Topical treatment of the rectal mucosa with lidocaine in patients with UC/UP resulted in rapid symptomatic relief, restored mucosal integrity, and caused extravasal lymphocytes to disappear.”

“A new paradigm for the treatment of ulcerative colitis has recently been presented: Treatment of the mucosa with lidocaine (2%) enemas for prolonged periods.”
“One hundred consecutive patients have now been treated and the results presented. The proctitis patients all responded to the treatment, despite previous therapeutic failures in more than two-thirds of the cases.”
“The patients were treated until the subsets of T-lymphocytes (OKT4+ and OKT8+) disappeared from the mucosa. This occurred in parallel with symptomatic relief and eventual healing in 83% of the patients after treatment for 6-34 weeks.”
“Of the 17 patients with left-sided colitis, all went primarily into remission within 2-4 months, but 23% had a relapse (observation period 13 months). The 6 patients with total colitis had symptomatic relief and improvement of histology when treated over 3-8 months. One patient had recurrence after 12 months.”
DO NOT OVERDOSE ON LIDOCAINE
Ref:
Beneficial effects of local or systemic lidocaine in experimental colitis
Topical treatment of ulcerative proctitis with lidocaine
Topical Treatment with Lidocaine in Patients with Ulcerative Proctitis/Colitis.
Treatment of the mucosa with local anaesthetics in ulcerative colitis
“One hundred consecutive patients have now been treated and the results presented. The proctitis patients all responded to the treatment, despite previous therapeutic failures in more than two-thirds of the cases.”
“The patients were treated until the subsets of T-lymphocytes (OKT4+ and OKT8+) disappeared from the mucosa. This occurred in parallel with symptomatic relief and eventual healing in 83% of the patients after treatment for 6-34 weeks.”
“Of the 17 patients with left-sided colitis, all went primarily into remission within 2-4 months, but 23% had a relapse (observation period 13 months). The 6 patients with total colitis had symptomatic relief and improvement of histology when treated over 3-8 months. One patient had recurrence after 12 months.”
DO NOT OVERDOSE ON LIDOCAINE
Ref:
Beneficial effects of local or systemic lidocaine in experimental colitis
Topical treatment of ulcerative proctitis with lidocaine
Topical Treatment with Lidocaine in Patients with Ulcerative Proctitis/Colitis.
Treatment of the mucosa with local anaesthetics in ulcerative colitis
• • •
Missing some Tweet in this thread? You can try to
force a refresh













