1/ #medtwitter #tweetorial Raise your hand if you have ever inappropriately checked an ammonia level.🙋
1. Why is ammonia ⬆️ in liver failure and how is this connected w/ encephalopathy?
2. When should levels be checked?
3. Aside from cirrhosis, what other conditions ⬆️ammonia?
1. Why is ammonia ⬆️ in liver failure and how is this connected w/ encephalopathy?
2. When should levels be checked?
3. Aside from cirrhosis, what other conditions ⬆️ammonia?
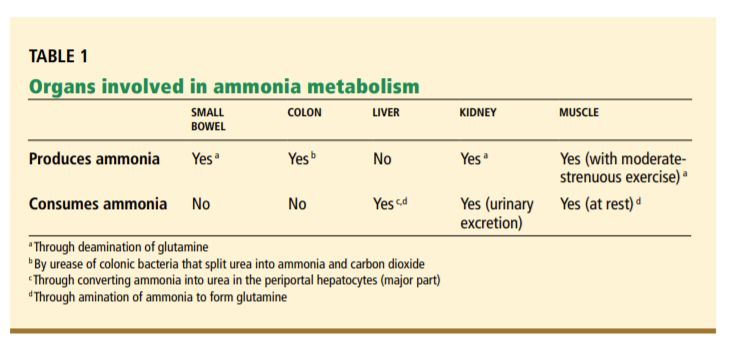
2/ Ammonia is primarily produced by bacteria w/ urease enz in intestines but is also produced in muscle and the kidneys.
Table source: ccjm.org/content/76/4/2…
Table source: ccjm.org/content/76/4/2…
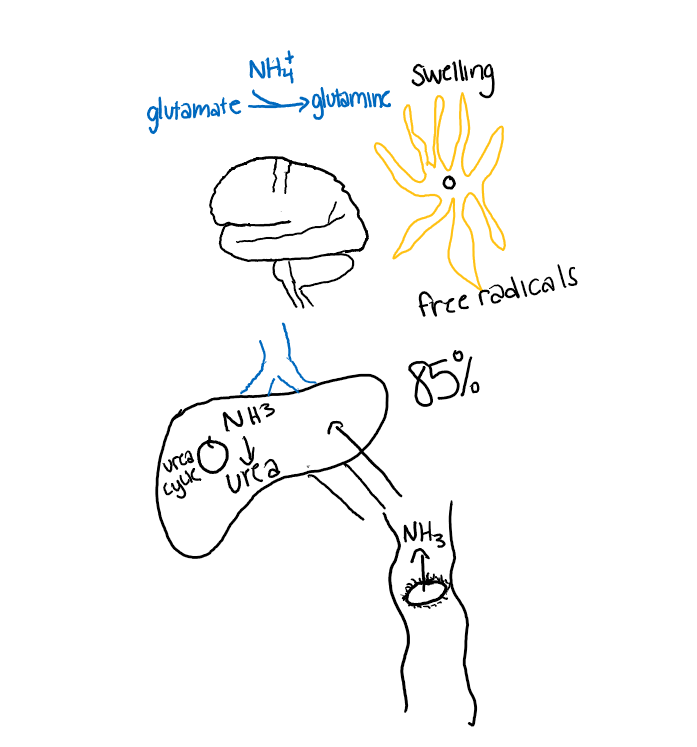
3/ 85% of ammonia is cleared by the liver through the urea cycle. 15% is cleared by muscle/kidneys. If the ammonia (/other nitrogenous waste) not metabolized it passes through the blood brain barrier glutamate>glutamine> astrocyte swelling and free radicals>encephalopathy. 
4/ Ammonia can build up though ⬆️production, ⬇️clearance, or combo. In both acute or chronic liver failure, ⬇️ urea cycle ⬆️ ammonia production. Portosystemic shunting can also ⬆️ ammonia since less passes though liver (why TIPS ⬆️ risk of encephalopathy).
5/ You might be thinking based on above that if a patient comes in with cirrhosis, you should check an ammonia level to evaluate for HE However, there are several reasons why HE is a clinical diagnosis.
6/I will discuss some of the reasons outlined in these two articles which I highly suggest reading:
journalofhospitalmedicine.com/jhospmed/artic…
jamanetwork.com/journals/jama/…
journalofhospitalmedicine.com/jhospmed/artic…
jamanetwork.com/journals/jama/…
7/Ammonia is a difficult test to obtain. You may have tried to add this lab test on and been dismayed when you saw it required a new draw. Using a tourniquet can falsely ⬆️ values as can⬆️ time prior to processing. The collected sample also has to be place on ice.
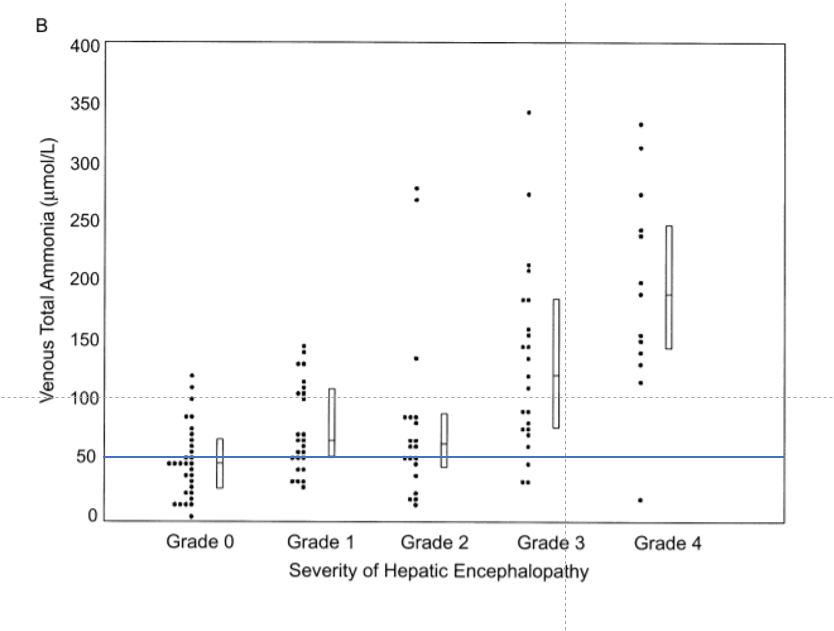
8/ In this study from 2003, arterial and venous ammonia levels where obtained to assess correlation with samples and degree of encephalopathy. There was a correleation between venous/arterial sample and degree of encephalopahy r = 0.56 for venous.
pubmed.ncbi.nlm.nih.gov/12637132/
pubmed.ncbi.nlm.nih.gov/12637132/
9/ The problem? The ULN for ammonia was 47 in this study. I used a cut off of 50 for ease. If you look at the sample a significant amount of pts with HE had normal ammonia levels and a significant amount w/o HE had ⬆️ ammonia levels. 
10/Another paper found that blood ammonia levels had a diagnostic accuracy of 59%, sensitivity 47%, specifity 78%. It certainly should not be used as a screening test as you would miss over 1/2 of cases of HE.
pubmed.ncbi.nlm.nih.gov/23293201/
pubmed.ncbi.nlm.nih.gov/23293201/
11/A recent propensity matched study showed that in cirrhotic pts w/ HE that lactulose dose was the same regardless of ammonia level. This points to the fact we likely are not using ammonia level to guide mng. Why check a lab you don't need?
pubmed.ncbi.nlm.nih.gov/31658104/
pubmed.ncbi.nlm.nih.gov/31658104/
12/ Although not helpful in cirrhosis, checking ammonia levels can be helpful in acute liver failure as ⬆️ levels are associated with worse prognosis.
ncbi.nlm.nih.gov/pmc/articles/P…
ncbi.nlm.nih.gov/pmc/articles/P…
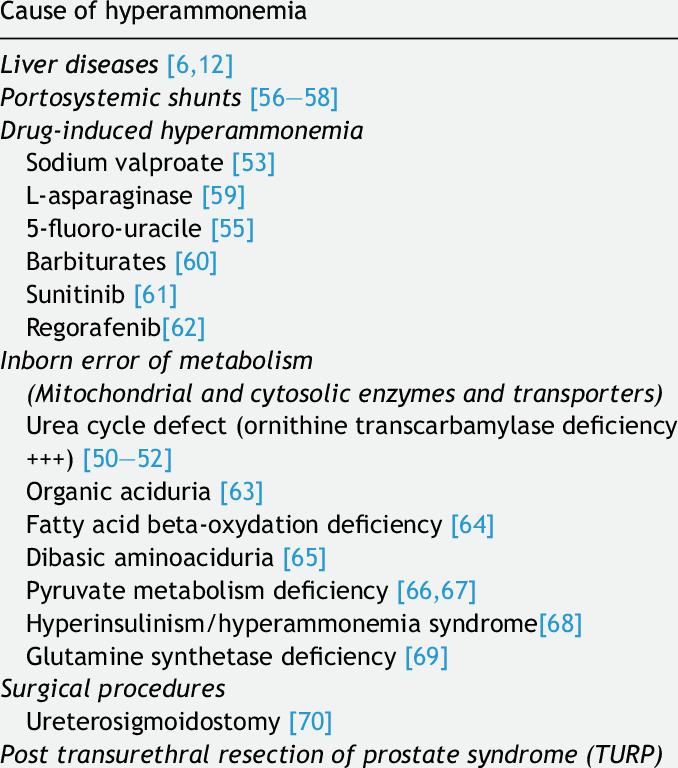
13/There are situations aside from liver failure in which ammonia ⬆️
1. Drug toxicity including valproic acid & chemo meds
2. Urea cycle disorder
3. Glycerin toxicity- historically caused TURP syndrome (now rarely used)
Table source: pubmed.ncbi.nlm.nih.gov/29551609/
1. Drug toxicity including valproic acid & chemo meds
2. Urea cycle disorder
3. Glycerin toxicity- historically caused TURP syndrome (now rarely used)
Table source: pubmed.ncbi.nlm.nih.gov/29551609/
4. SIBO with dehydration
14/ 4. SIBO with dehydration
5. Urease producing organisms including Ureaplasma urealyticum in an immunocompromised host academic.oup.com/ofid/article/6…
Mnemonic source: theindianmedicalstudent.com/3-mnemonics-fo…
5. Urease producing organisms including Ureaplasma urealyticum in an immunocompromised host academic.oup.com/ofid/article/6…
Mnemonic source: theindianmedicalstudent.com/3-mnemonics-fo…

15/Checking an ammonia level in these situations is helpful because it may guide specific treatment. Valproic acid can cause ⬆️ ammonia leading to AMS w/o liver failure or supratherapeutic levels. Being aware of it is important b/c treated w/ carnitine .
ncbi.nlm.nih.gov/pmc/articles/P…
ncbi.nlm.nih.gov/pmc/articles/P…
16/Conclusions:
1. While ⬆️ ammonia is common in cirrhosis, HE is a clinical diagnosis. Ammonia has poor sensitivity/specificity and diagnostic accuracy and has not been shown to change treatment of HE in cirrhosis.
2. ⬆️Ammonia can have prognostic implications in ALF.
1. While ⬆️ ammonia is common in cirrhosis, HE is a clinical diagnosis. Ammonia has poor sensitivity/specificity and diagnostic accuracy and has not been shown to change treatment of HE in cirrhosis.
2. ⬆️Ammonia can have prognostic implications in ALF.
17/ 3. Other conditions such as drug toxicity (especially valproic acid), urea cycle disorder, and certain bacterial infections can also cause ⬆️ ammonia. It may be helpful to check ammonia levels in these conditions b/c it may change managment. /end
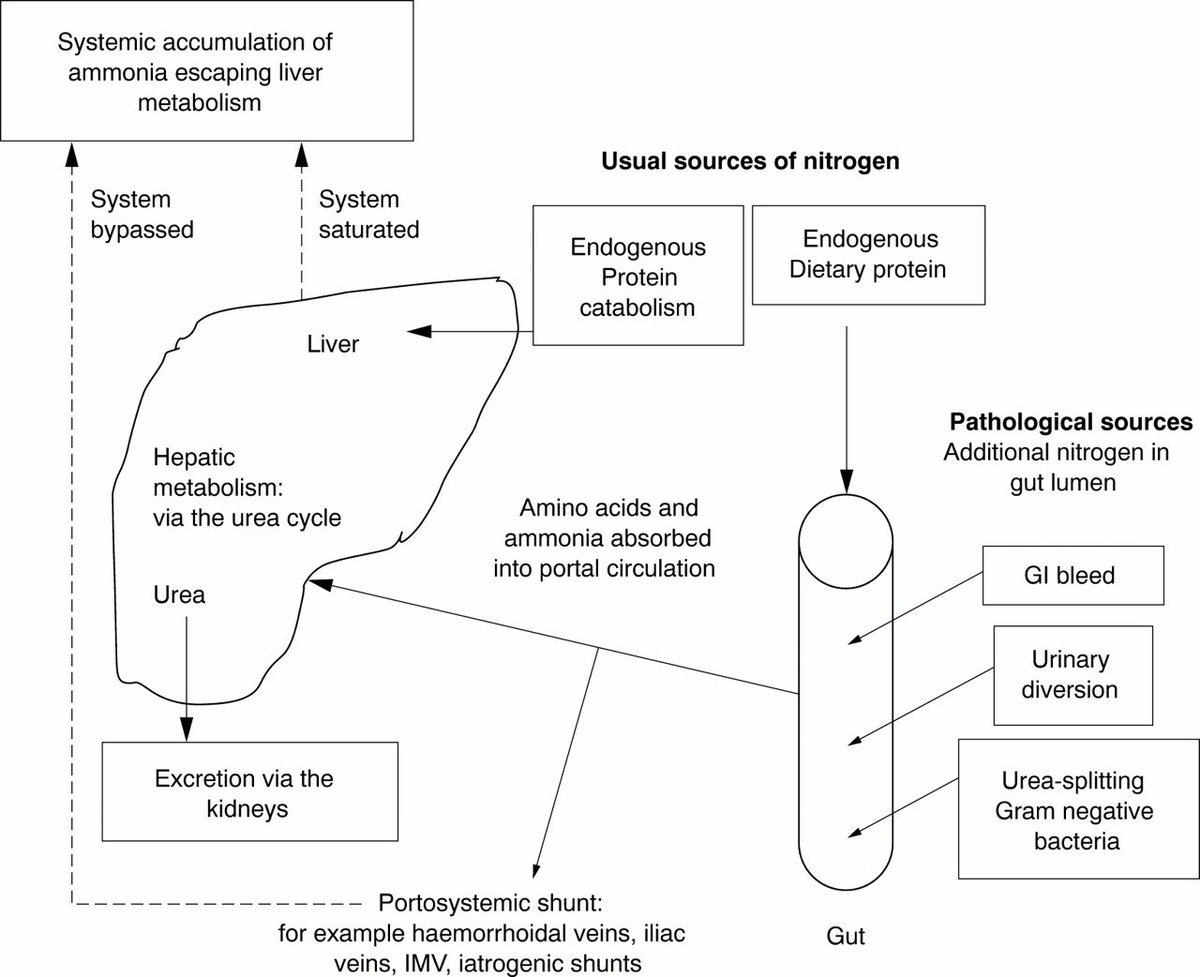
On related note, just saw this case report of 3 cases of non-hepatic hyperammonaemia with this great diagram.
pmj.bmj.com/content/77/913…
pmj.bmj.com/content/77/913…
• • •
Missing some Tweet in this thread? You can try to
force a refresh






