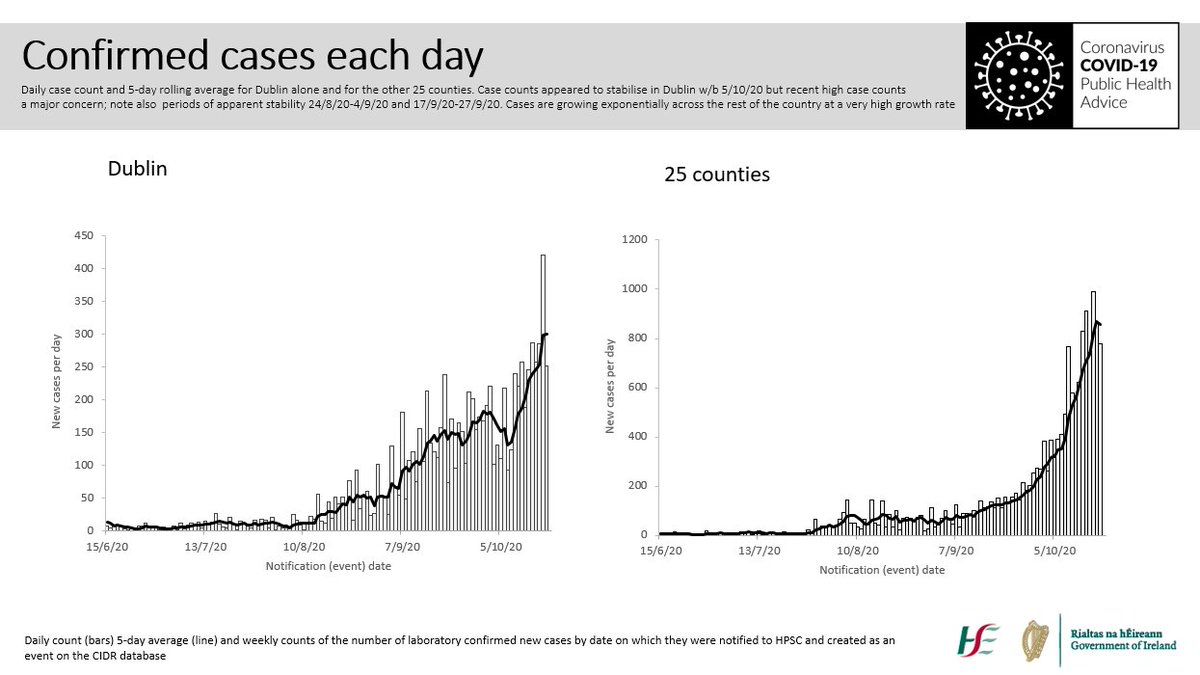
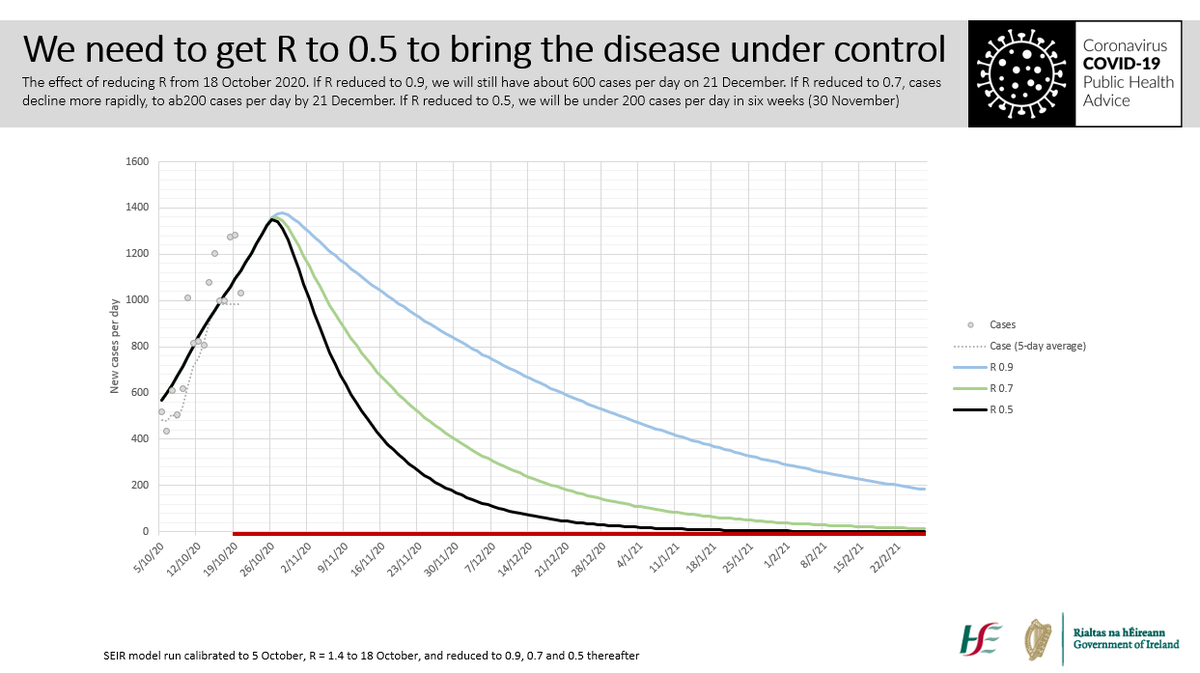
Let’s protect the vulnerable. Keep your contacts to a minimum between now and Christmas and then celebrate with a small circle. Meet outdoors if you can. If indoors: limit numbers and duration, use masks and keep your distance, gentle natural ventilation. 1/5 

It’s good that numbers in hospital and ICU are falling. Behind each number is a human story of illness and loss. Hospitalisations lag behind cases, and sadly what we are seeing now is the impact on older and vulnerable people infected towards the end of the recent surge. 2/5 



A semi-log plot clearly shows the delay between rising cases and rising hospitalisations, and equally the delay between the suppression of infections in the community and the decline in the number of severely ill people in hospital. 3/5 

This is why we worry about high case numbers, and the risk of a third wave in January. If we see a rise in cases we cannot wait around until we have increasing numbers of people in hospital and ICU to convince ourselves we have a problem. We’ll need to act quickly. 4/5 

The fundamental message: a small, safe, careful Christmas with those that matter the most to us will limit the levels of disease in January, and save lives. 5/5
• • •
Missing some Tweet in this thread? You can try to
force a refresh