Latest preprint by @tianyangmao et al shows that a stem-loop RNA RIG-I agonist in mice can
1) Block viral replication and disease when given early after SARS-CoV-2 infection (including VOCs)
2)Eliminate chronic infection in immunodeficient mice
🧵(1/)
biorxiv.org/content/10.110…
1) Block viral replication and disease when given early after SARS-CoV-2 infection (including VOCs)
2)Eliminate chronic infection in immunodeficient mice
🧵(1/)
biorxiv.org/content/10.110…
We urgently need antiviral agents that can work against any viral threats. Here, we use a stem-loop RNA developed by @AnnaPyle to trigger interferon to stimulate antiviral state. Work by @MelissaLV14 et al demonstrated robust ISG induction in mice👇🏽 (2/)
advances.sciencemag.org/content/4/2/e1…
advances.sciencemag.org/content/4/2/e1…
First, we wanted to know if SLR can be used as a post-exposure prophylaxis. Mice infected with lethal dose of SARS-CoV-2 were treated with SLR 4 hours after exposure. SLR-treated mice had no detectable infectious virus 5 days later and most survived. (3/) 

Next, we asked whether interferon signaling is required for the SLR-mediated protection. Mice injected with blocking antibodies to IFNAR were no longer protected by SLR from SARS-CoV-2 infection. Thus, SLR-mediated protection depends on IFN-I signaling. (4/) 

How late can we administer SLR to observe protection? Compared to robust protection at 4 hours, injection of SLR 24 h and 48 h post exposure protected only partially, and at 72 h, no protection was observed. (Note: mouse disease course is accelerated compared to humans)(5/) 

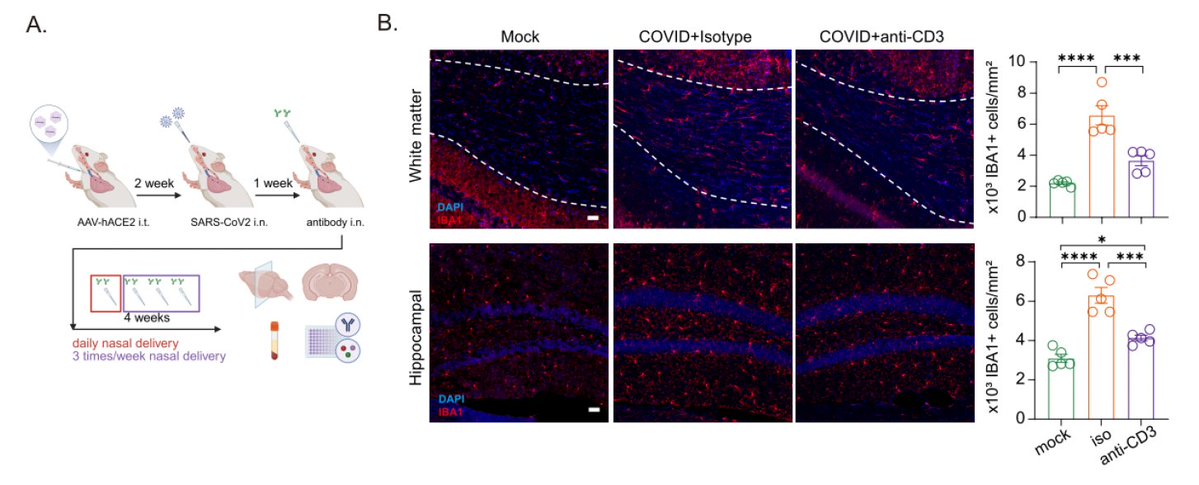
We also tested SLR in a mouse model of immunodeficiency. Here, we used RAG-deficient mice (devoid of T or B cells) that become persistently infected. In immunocompromised patients, prolonged SARS-CoV-2 infection has been widely reported (see @Primary_Immune’s tweets) (6/) 

What is remarkable is that a single injection of SLR in persistently infected animal was able to eliminate infectious virus in most of the treated mice. Thus, in the absence of adaptive immunity, robust IFN response is sufficient to eliminate persistent virus infection 🤯 (7/) 

Is SLR effective against the VOCs? SLR injection 4 hours post exposure with P.1, B.1.526, B.1.351 or B.1.1.7 led to significant protection from disease & death. Difference in effectiveness might reflect the IFN-resistance of these variants.
biorxiv.org/content/10.110…
(8/)
biorxiv.org/content/10.110…
(8/)

To sum up, the work led by @tianyangmao showed that a small RNA RIG-I agonist can be used in prophylactic, post exposure, and chronic infection settings to combat COVID-19. Since SLR works by triggering host innate immune defense, it works against a wide range of viruses. (9/)
To bring SLR to patients, @annapyle and I co-founded a company called #RIGImmune. For people interested in learning more about this technology, please attend the upcoming webinar hosted by @YaleOCR (10/)
yale.zoom.us/webinar/regist…
yale.zoom.us/webinar/regist…
As with all the work we do, this is a highly collaborative effort of many including @tianyangmao @BenIsraelow @carolilucas @VogelsChantal Olga Fedorova, Mallery Breban, Bridget Menasche, Huiping Dong, @MelissaLV14 @WilenLab Marie Landry @NathanGrubaugh @AnnaPyle 🙏🏼 (end)
• • •
Missing some Tweet in this thread? You can try to
force a refresh