Doctors at a major US insurance company deny tens of thousands of claims a month without even looking at patients’ files.
“We literally click & submit,” a former Cigna doctor told @ProPublica & @Capitol_Forum. “It takes all of 10 seconds to do 50 at a time.”
The inside story 🧵
“We literally click & submit,” a former Cigna doctor told @ProPublica & @Capitol_Forum. “It takes all of 10 seconds to do 50 at a time.”
The inside story 🧵
2/ Nick van Terheyden was puzzled when Cigna told him it wouldn’t cover the cost of a simple blood test, which it deemed “not medically necessary.”
“This was a clinical decision being second-guessed by someone with no knowledge of me."
“This was a clinical decision being second-guessed by someone with no knowledge of me."
3/ Nick's unease was justified. His claim was just one of ~60,000 rejected in just a month by Dr. Cheryl Dopke, a Cigna-employed medical director responsible for deciding whether patient claims will be paid or rejected.
propublica.org/article/cigna-…
propublica.org/article/cigna-…
4/ And Dopke wasn't alone. A review of internal Cigna records turned up multiple medical directors who were rejecting a large volume of claims. Here are the Jan. 2022 rejection stats for 3 Cigna-employed doctors: 
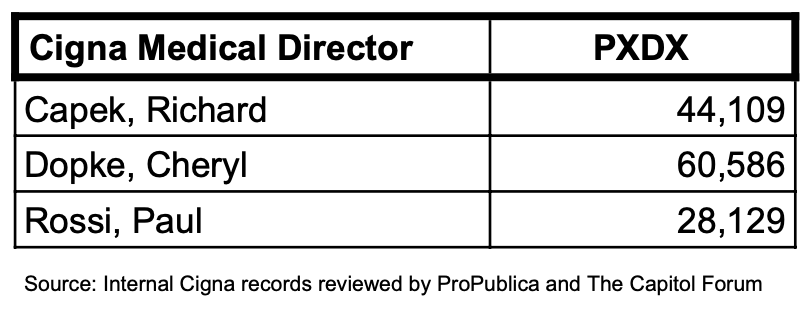
5/ How could these doctors possibly review and reject so many claims in a month?
With the help of a process called PXDX that allows Cigna docs to deny claims as medically unnecessary without having to open a patient's file.
With the help of a process called PXDX that allows Cigna docs to deny claims as medically unnecessary without having to open a patient's file.
6/ PXDX, short for procedure-to-diagnosis, uses a list of tests & procedures approved for use with certain illnesses.
It automatically approves claims that match the conditions, but also flags for denial treatments that don’t match one of the listed conditions.
It automatically approves claims that match the conditions, but also flags for denial treatments that don’t match one of the listed conditions.
7/ Medical directors can then approve the denials without opening a patient file.
In Jan. 2022 alone, Cigna medical directors used PXDX to reject more than 150,000 claims, spending an average of 1.2 seconds per denial.
In Jan. 2022 alone, Cigna medical directors used PXDX to reject more than 150,000 claims, spending an average of 1.2 seconds per denial.

8/ Laws & regulations in many states require doctors to review claims rejected for medical reasons. But in Cigna’s PXDX system, medical directors do not see any patient records or put their medical judgment to use, said former company employees familiar with the system.
9/ “We literally click and submit,” one former @Cigna doctor said. “It takes all of 10 seconds to do 50 at a time.”
propublica.org/article/cigna-…
propublica.org/article/cigna-…
10/ Why would Cigna use a system like PXDX?
Processing and reviewing claims takes time and costs the insurer money. For low-dollar claims, it used to be easier for Cigna to simply pay the bill.
Then came Dr. Alan Muney...
Processing and reviewing claims takes time and costs the insurer money. For low-dollar claims, it used to be easier for Cigna to simply pay the bill.
Then came Dr. Alan Muney...
11/ In 2010, Cigna brought in Muney, who managed the health care plans for companies acquired by private equity giant Blackstone, to spot savings in its operations.
Muney and his team developed what would become PXDX.
Muney and his team developed what would become PXDX.
12/ “The PXDX stuff is not reviewed by a doc or nurse or anything like that,” said Muney, adding that the system simply allowed Cigna to economically identify claims that it had a right to deny.
13/ Muney emphasized that the PXDX system allows for the patient to appeal a medical director’s decision to deny a claim.
But Cigna does not expect many appeals.
But Cigna does not expect many appeals.
14/ In one corporate document, Cigna estimated that only 5% of people would appeal a denial resulting from a PXDX review. 
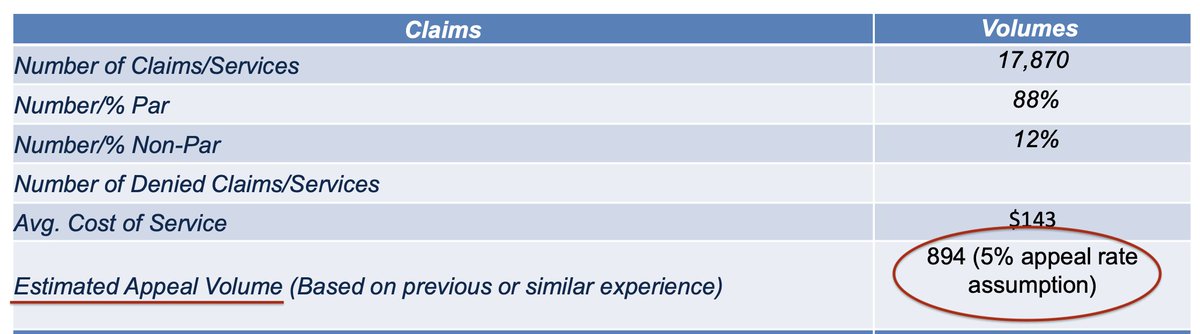
15/ In fact, when adding a new procedure to PXDX for automated denial, Cigna has calculated how many patients it expects to leave footing the bill.
16/ Cigna considered adding Autonomic Nervous System Testing to PXDX in 2014.
In a company presentation weighing the costs & benefits of the decision, it acknowledged the change would result in 17,870 rejected claims a year.
In a company presentation weighing the costs & benefits of the decision, it acknowledged the change would result in 17,870 rejected claims a year.

17/ That same document also predicted these automatic denials would “create a negative customer experience” and a “potential for increased out of pocket costs."
While allowing Cigna to save $2.4 million per year.
While allowing Cigna to save $2.4 million per year.

18/ Cigna said our description of PXDX is “incorrect,” and said the system was created to “accelerate payment of claims for certain routine screenings.”
(ProPublica employees’ health care insurance is provided by Cigna.)
(ProPublica employees’ health care insurance is provided by Cigna.)
19/ Cigna called our findings “biased and incomplete." The company declined to provide more details on its system.
20/ Read the full investigation from @PatrickMRucker @mayatmiller @DavidArmstrongX here:
propublica.org/article/cigna-…
propublica.org/article/cigna-…
21/ ProPublica and @Capitol_Forum are not done reporting, and could use your help.
Do you, or have you, worked in health insurance? Have a story to share about being denied care? Please get in touch here: propub.li/denials
Do you, or have you, worked in health insurance? Have a story to share about being denied care? Please get in touch here: propub.li/denials
22/ Reporters @PatrickMRucker and @mayatmiller will discuss this story in detail this Tuesday at “Medically Necessary,” a virtual panel discussion about America’s broken health insurance system.
RSVP for free:
propublica.org/events/medical…
RSVP for free:
propublica.org/events/medical…
• • •
Missing some Tweet in this thread? You can try to
force a refresh