79.3% of psychiatrists recommended immediate antidepressant treatment for a person with depression, but only 39.1% would follow that recommendation themselves.
🧵1/10
🧵1/10
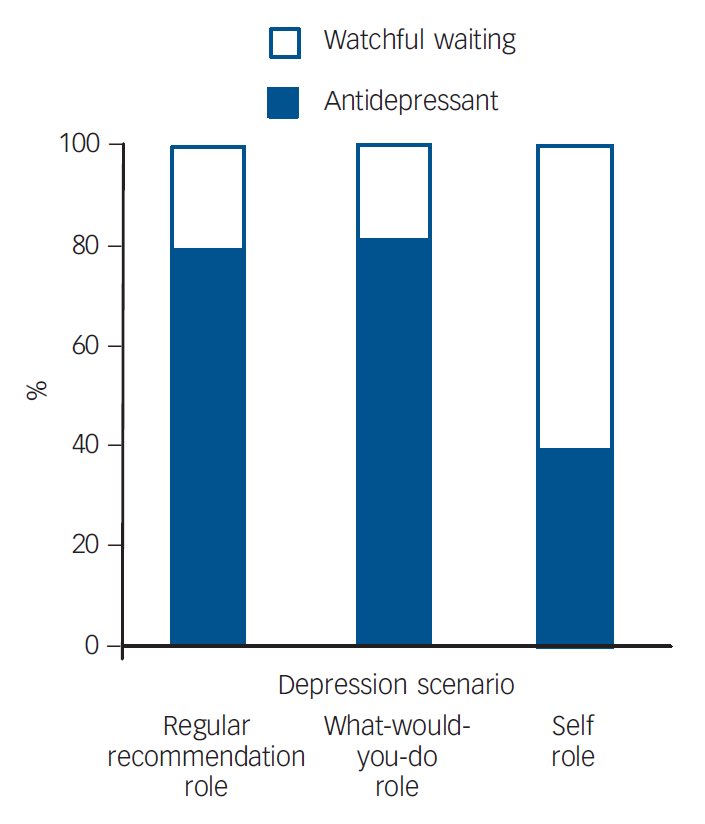
These findings are from a randomised experimental study of 515 psychiatrists in @thebjpsych which aimed to determine if the question, ‘What would you do if you were me, doctor?’ leads psychiatrists to reveal their personal preferences. 2/10 cambridge.org/core/journals/…


Psychiatrists were either asked to imagine: 1) treating an out-patient with depressive symptoms or 2) that they had depressive symptoms themselves and were being treated by a psychiatrist as an out-patient. 3/10
The two treatment options to choose from were immediate treatment with an antidepressant and watchful waiting. 4/10
In the regular recommendation role and the what-would-you-do role, psychiatrists were asked to indicate what kind of treatment they would recommend. In the self role, the psychiatrists were requested to decide what treatment option they would prefer if they had depression. 5/10
Psychiatrists in the what-would-you-do role and in the regular recommendation role more often chose an antidepressant than psychiatrists in the self role (what-would-you-do role 81.4%, regular recommendation role 79.3%, self role 39.1%). 6/10
Why do psychiatrists choose different treatments for themselves than for their patients? 7/10
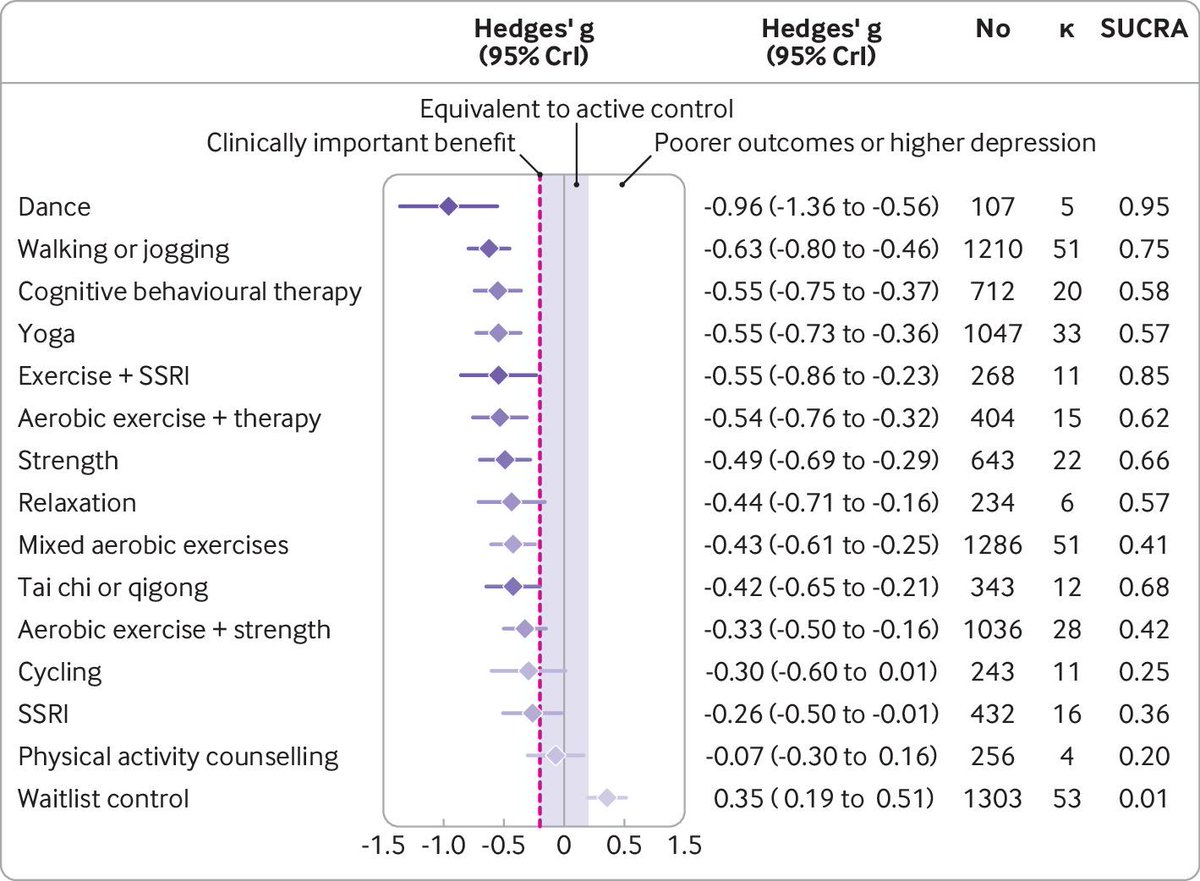
Alternative treatment options for mild to moderate depression, such as exercise, are not routinely taught during training and lead many clinicians to believe that antidepressants (or psychotherapy) are the only answer to treat depression. 8/10bmj.com/content/384/bm…
In fact, current Canadian guidelines recommend exercise and first-line monotherapy for mild- to moderate depression. 9/10journals.sagepub.com/doi/10.1177/07…
Therefore, we must provide our patients with all treatment options in order to devise a treatment plan that ensures optimal outcomes and minimizes the discrepancy of what we would recommend to ourselves vs. our patients. 10/10
• • •
Missing some Tweet in this thread? You can try to
force a refresh