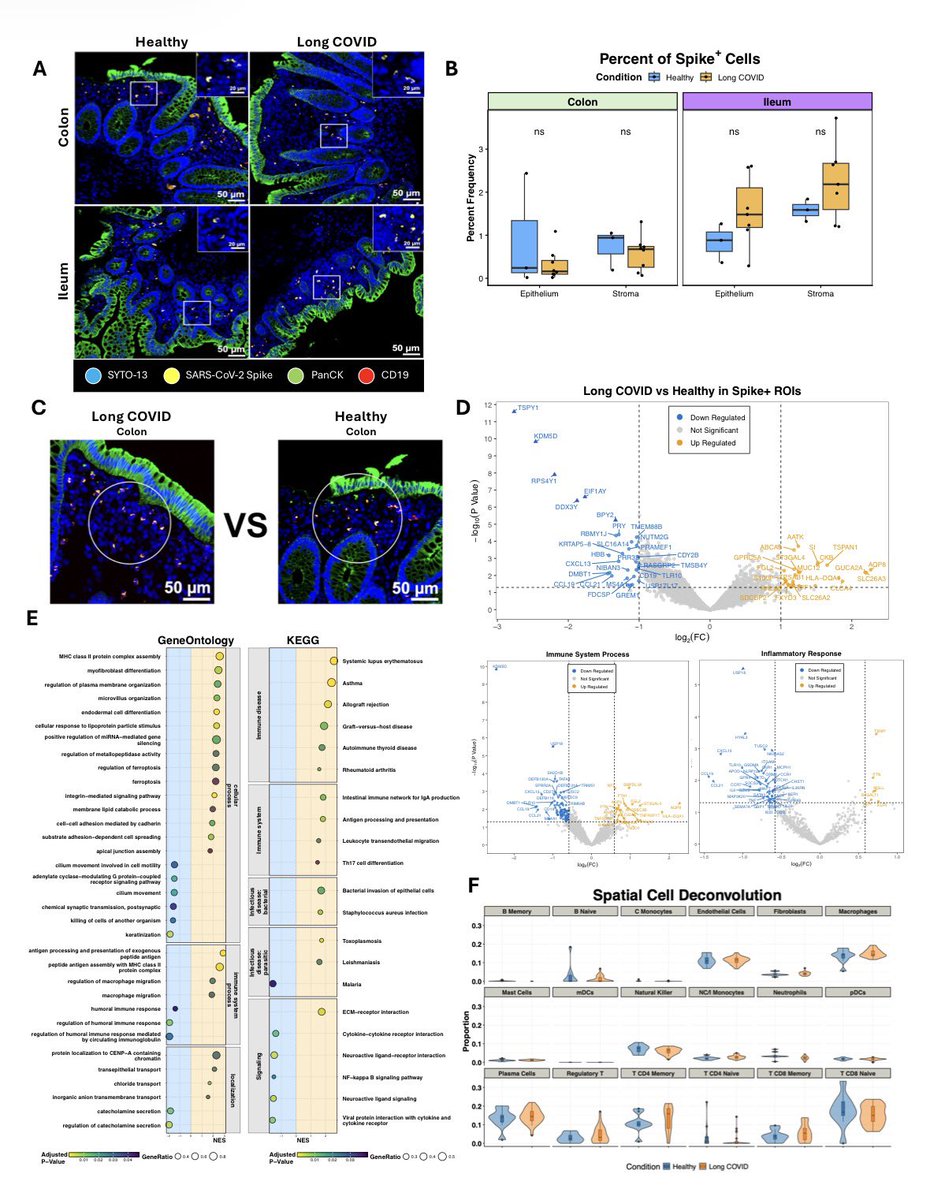
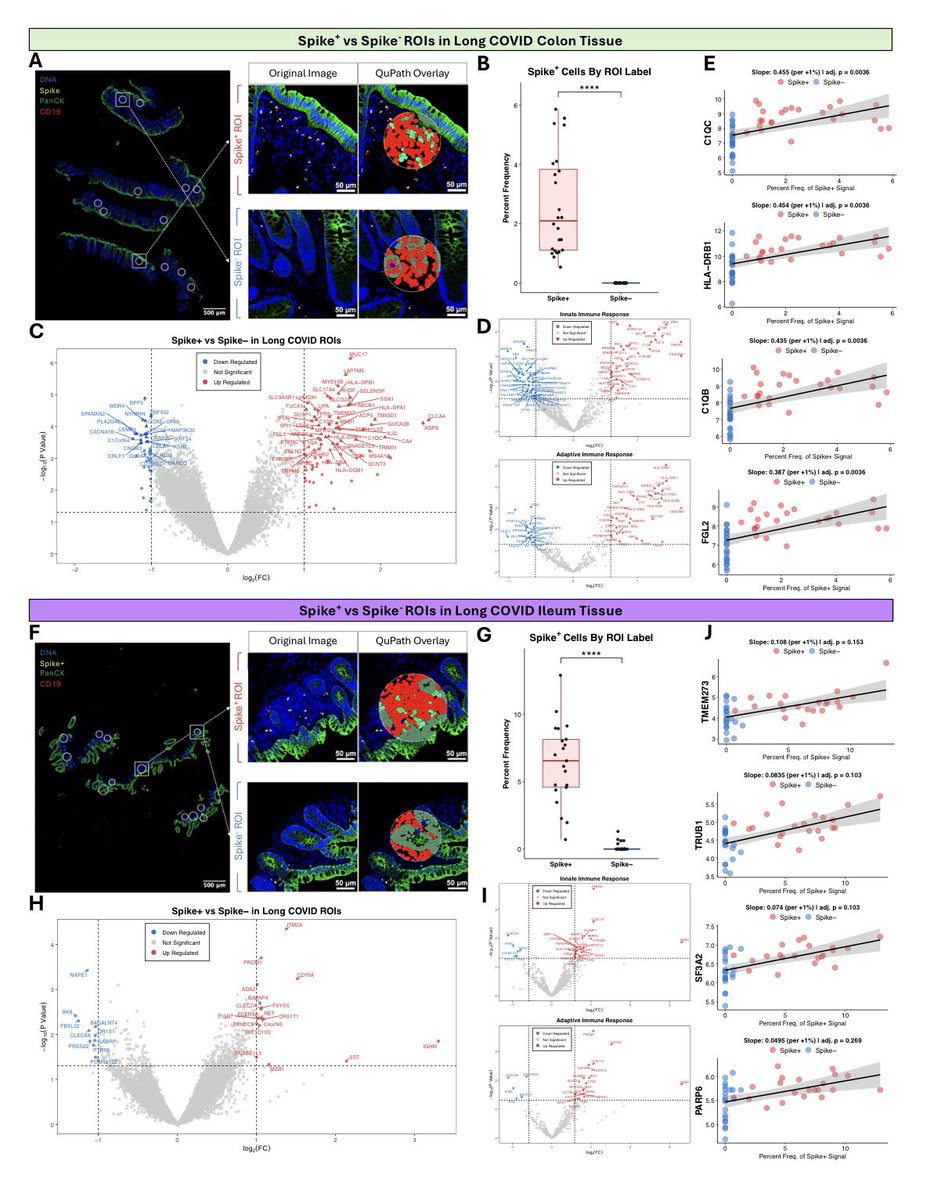
Globally, NB.1.8.1 is now the dominant variant. The WHO has issued a warning about rising COVID-19 activity in the Western Pacific, Southeast Asia, and Eastern Mediterranean, driven by NB.1.8.1 this week.
H/T: @RajlabN
H/T: @RajlabN

Classified as a "variant under monitoring" by the WHO & “ Nimbus” by @TRyanGregory, NB.1.8.1 has triggered a seventh consecutive week of surges in Southeast Asia. Taiwan has seen ER visits double again this week. 2/
focustaiwan.tw/society/202505…
focustaiwan.tw/society/202505…
@TRyanGregory China is reporting widespread infections with NB.1.8.1 causing severe throat pain described as “razor blade throat.”
However, the #Nimbus aka NB.1.8.1 wave in Hong Kong and Singapore may have peaked. 3/
However, the #Nimbus aka NB.1.8.1 wave in Hong Kong and Singapore may have peaked. 3/

@TRyanGregory A new surge is going on in India too. Still early days…active Covid-19 cases have risen to 3,758, with Kerala reporting the highest at 1,400 cases.
One death is also reported from my own district though no uptick is noticed in children so far. 4/4
indtoday.com/covid-19-cases…
One death is also reported from my own district though no uptick is noticed in children so far. 4/4
indtoday.com/covid-19-cases…

@TRyanGregory And what about vaccines?
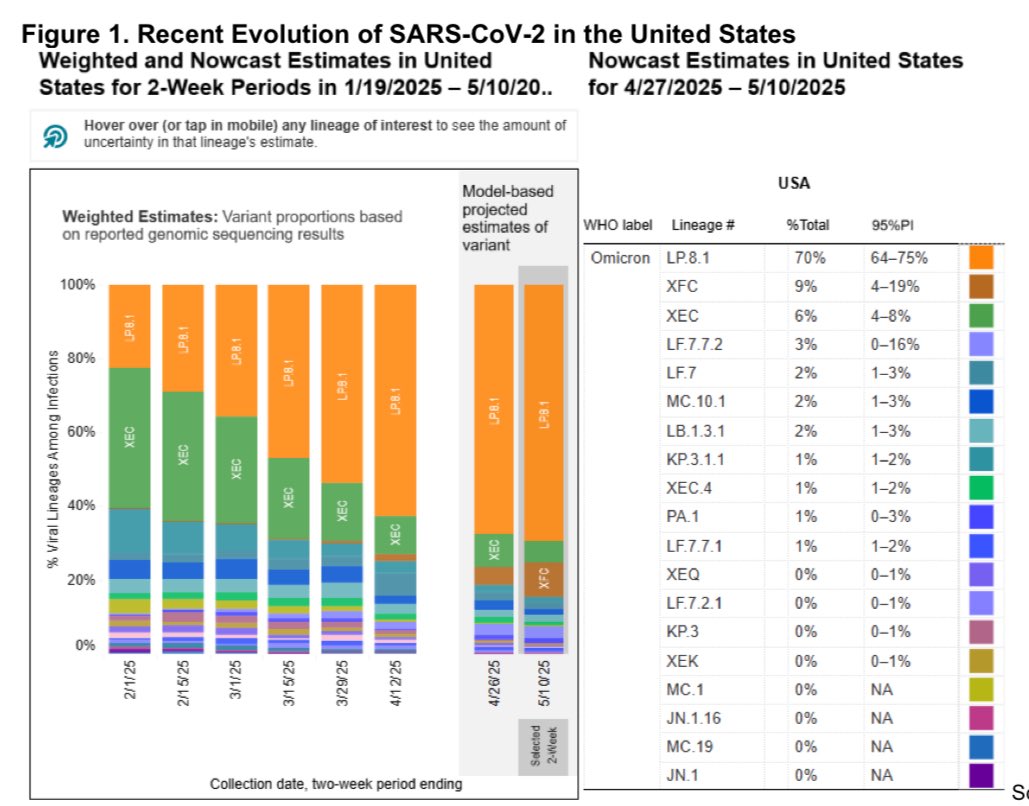
The FDA has recommended updating Fall 2025 COVID vaccines to target LP.8.1 which is the dominant variant in the United States now.
But, LP.8.1 is fairly different from NB.1.8.1 which is the dominant variant worldwide. 5/
nbcnews.com/news/amp/rcna2…
The FDA has recommended updating Fall 2025 COVID vaccines to target LP.8.1 which is the dominant variant in the United States now.
But, LP.8.1 is fairly different from NB.1.8.1 which is the dominant variant worldwide. 5/
nbcnews.com/news/amp/rcna2…
@TRyanGregory Last year’s Fall 2024 COVID vaccine targeted KP.2 for Moderna/Pfizer & JN.1 for Novavax. Although FDA’s advisory panel favored sticking with JN.1-based strains for Fall 2025, they agreed LP.8.1 is an appropriate alternative for 2025/2026 season 6/
fda.gov/media/186567/d…
fda.gov/media/186567/d…
@TRyanGregory And what about India?
No JN.1/adapted booster
The only Omicron-adapted vax is Gemcovac-OM based on BA.1
Even this isn’t freely available
The only category who need boosters in India: elderly w/ comorbidities or immunocompromised
So what’s the recs for Covid vax here👇 7/7
No JN.1/adapted booster
The only Omicron-adapted vax is Gemcovac-OM based on BA.1
Even this isn’t freely available
The only category who need boosters in India: elderly w/ comorbidities or immunocompromised
So what’s the recs for Covid vax here👇 7/7

• • •
Missing some Tweet in this thread? You can try to
force a refresh