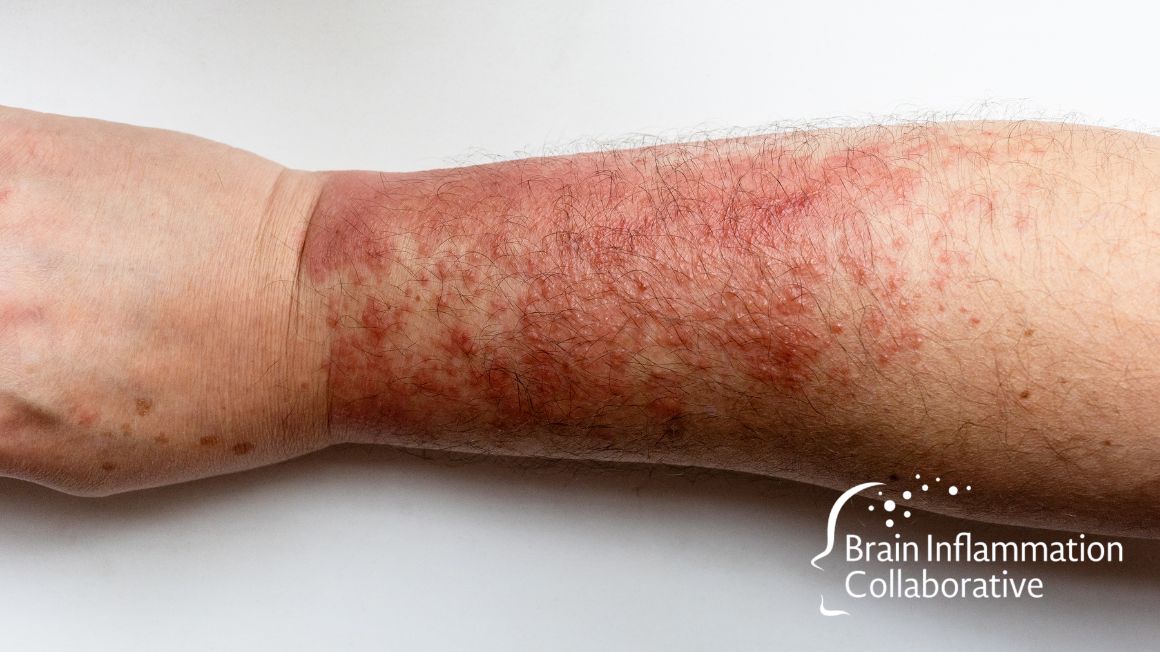
Long COVID in adults is characterized by (protein) markers of:
- inflammation
- blood vessel clotting
However, similar studies in pediatric cohorts are almost non-existent... until now.
This study suggests that pediatric Long COVID is characterized by unique pathophysiology and isn't stress- or anxiety-induced...🧵
- inflammation
- blood vessel clotting
However, similar studies in pediatric cohorts are almost non-existent... until now.
This study suggests that pediatric Long COVID is characterized by unique pathophysiology and isn't stress- or anxiety-induced...🧵

\ The Study:
Scientists from the University of Rome and Fondazione Policlinico Universitario discovered that 34 children and adolescents between the ages of 2 and 18 have an abundance of pro-inflammatory cytokines in their blood.
A subset of the cytokines have angiogenic (blood vessel growth-promoting) properties.
Read more: buff.ly/7NN1lyZ
Scientists from the University of Rome and Fondazione Policlinico Universitario discovered that 34 children and adolescents between the ages of 2 and 18 have an abundance of pro-inflammatory cytokines in their blood.
A subset of the cytokines have angiogenic (blood vessel growth-promoting) properties.
Read more: buff.ly/7NN1lyZ

\ The Study Continued:
The signature of protein markers was distinct from children with the following:
- Multisystem inflammatory syndrome in children (MIS-C) (27 participants)
- Acute SARS-CoV-2 infection (32 participants)
- Healthy controls (19 participants)
*MIS-C is a rare but serious condition where different body parts can become inflamed, typically following a COVID-19 infection.
Here are the proteins in the blood that were changed.
The signature of protein markers was distinct from children with the following:
- Multisystem inflammatory syndrome in children (MIS-C) (27 participants)
- Acute SARS-CoV-2 infection (32 participants)
- Healthy controls (19 participants)
*MIS-C is a rare but serious condition where different body parts can become inflamed, typically following a COVID-19 infection.
Here are the proteins in the blood that were changed.
\ The Results:
The following were high in the pediatric Long COVID cohort:
OSM
CXCL1
CXCL5
CXCL6
CXCL8
CXCL11
TNFSF11
STAMBP1a
These cytokines are pro-inflammatory and pro-angiogenic (promote blood vessel growth).
They represent a unique proteomic profile (yellow dots below).
The following were high in the pediatric Long COVID cohort:
OSM
CXCL1
CXCL5
CXCL6
CXCL8
CXCL11
TNFSF11
STAMBP1a
These cytokines are pro-inflammatory and pro-angiogenic (promote blood vessel growth).
They represent a unique proteomic profile (yellow dots below).
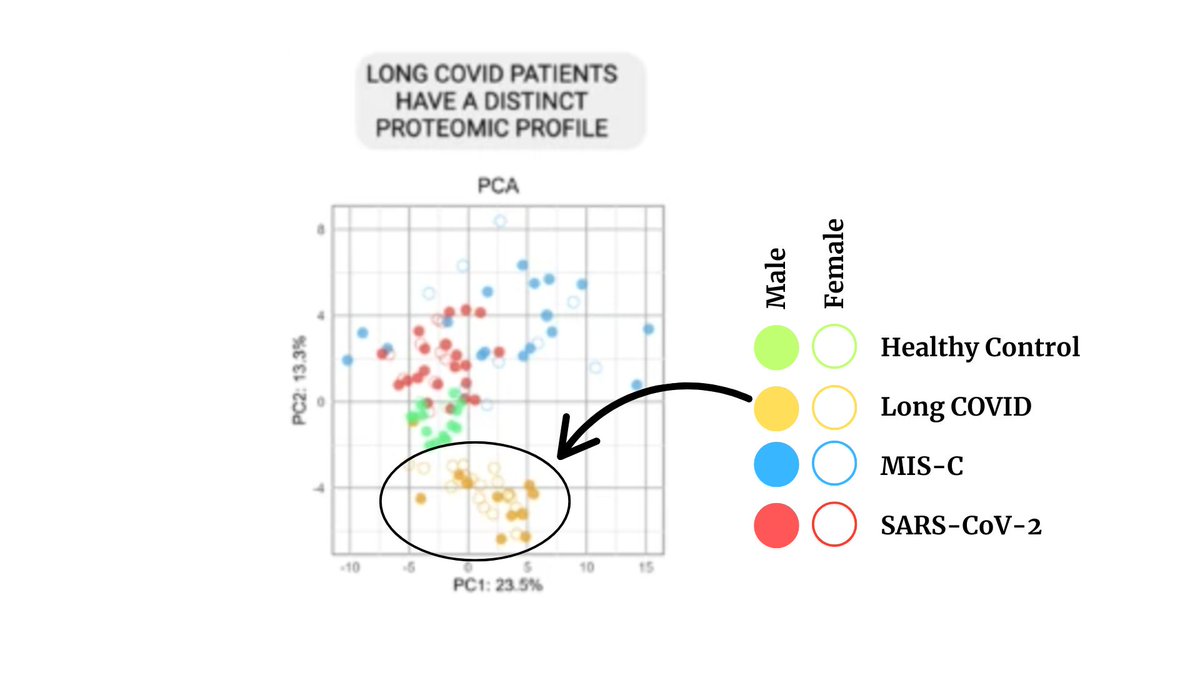
\ Significance:
This data suggests pediatric Long COVID is characterized by chronic inflammation and is NOT the result of a mental health condition caused by pandemic restrictions.
This proteomic profile identified pediatric Long COVID patients with an accuracy of 93%.
An AI-based blood test is being developed by the same group to diagnose pediatric Long COVID (👇 )
This data suggests pediatric Long COVID is characterized by chronic inflammation and is NOT the result of a mental health condition caused by pandemic restrictions.
This proteomic profile identified pediatric Long COVID patients with an accuracy of 93%.
An AI-based blood test is being developed by the same group to diagnose pediatric Long COVID (👇 )
Find out how we are remotely connecting geographically dispersed health professionals with pediatric cohorts.
This is designed to fast-track our understanding of pediatric neuroimmune axis conditions, such as pediatric Long COVID.
Check out our free newsletter (pinned post) to learn more.
This is designed to fast-track our understanding of pediatric neuroimmune axis conditions, such as pediatric Long COVID.
Check out our free newsletter (pinned post) to learn more.

• • •
Missing some Tweet in this thread? You can try to
force a refresh