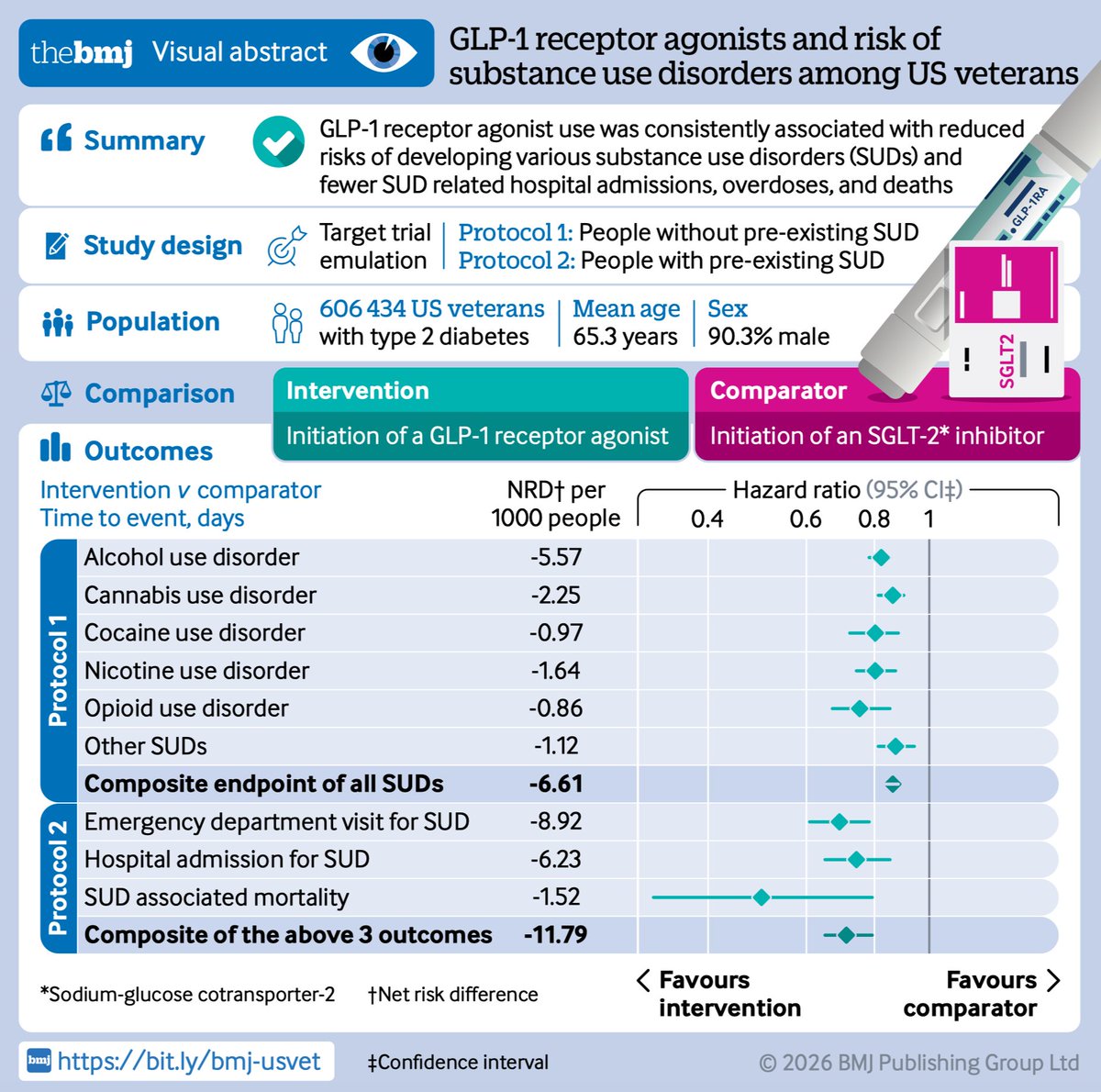
What happens to the heart when people stop GLP-1 drugs?
The short answer: nothing good.
New from our team: a study of 330,000+ people in @BMJMedicine
🧵
The short answer: nothing good.
New from our team: a study of 330,000+ people in @BMJMedicine
🧵

About 1 in 8 U.S. adults has taken a GLP-1 drug. But 36–81% of users stop within the first year. Most studies have focused on weight regain after stopping. We focused on what happens to the heart. 
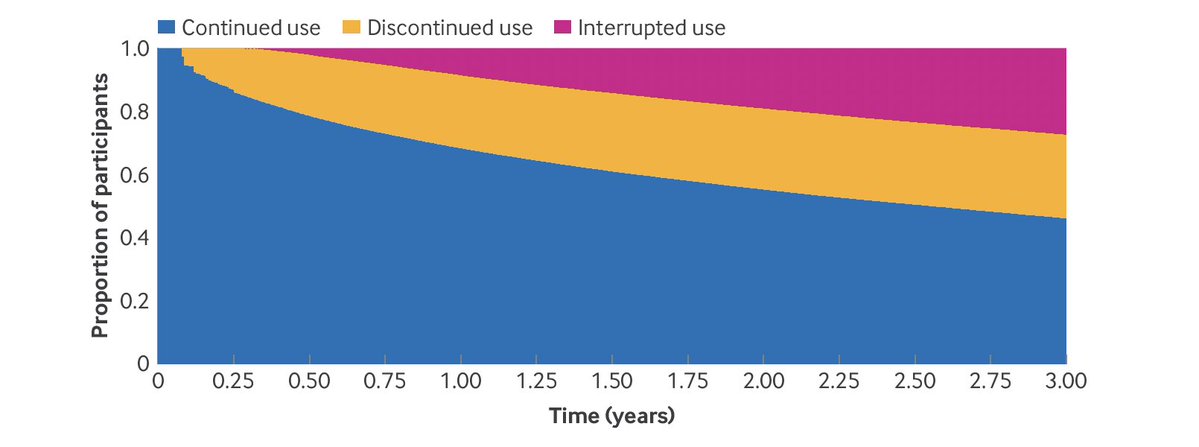
We followed 333,000+ adults with type 2 diabetes for 3 years, emulating a randomized trial across 16 treatment scenarios with different durations of use, discontinuation, and interruption.
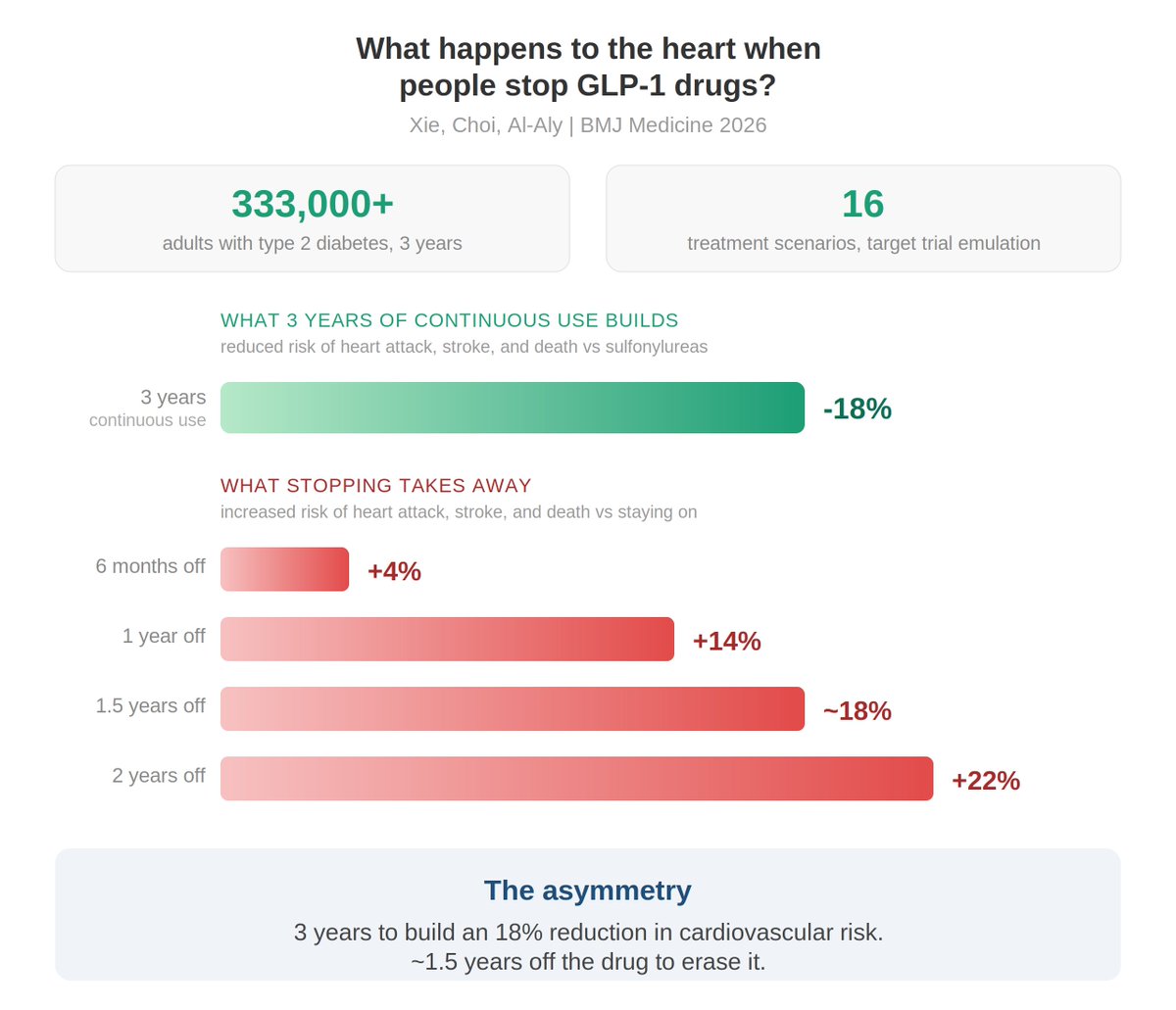
The core finding: Cardiovascular protection builds slowly. It took 3 years of continuous GLP-1 use to achieve an 18% reduction in heart attack, stroke, and death.
But that protection erodes fast.
But that protection erodes fast.
Stopping for 6 months: 4% increased risk
Stopping for 1 year: 14% increased risk
Stopping for 2 years: 22% increased risk
— all compared to staying on.
Stopping for 1 year: 14% increased risk
Stopping for 2 years: 22% increased risk
— all compared to staying on.
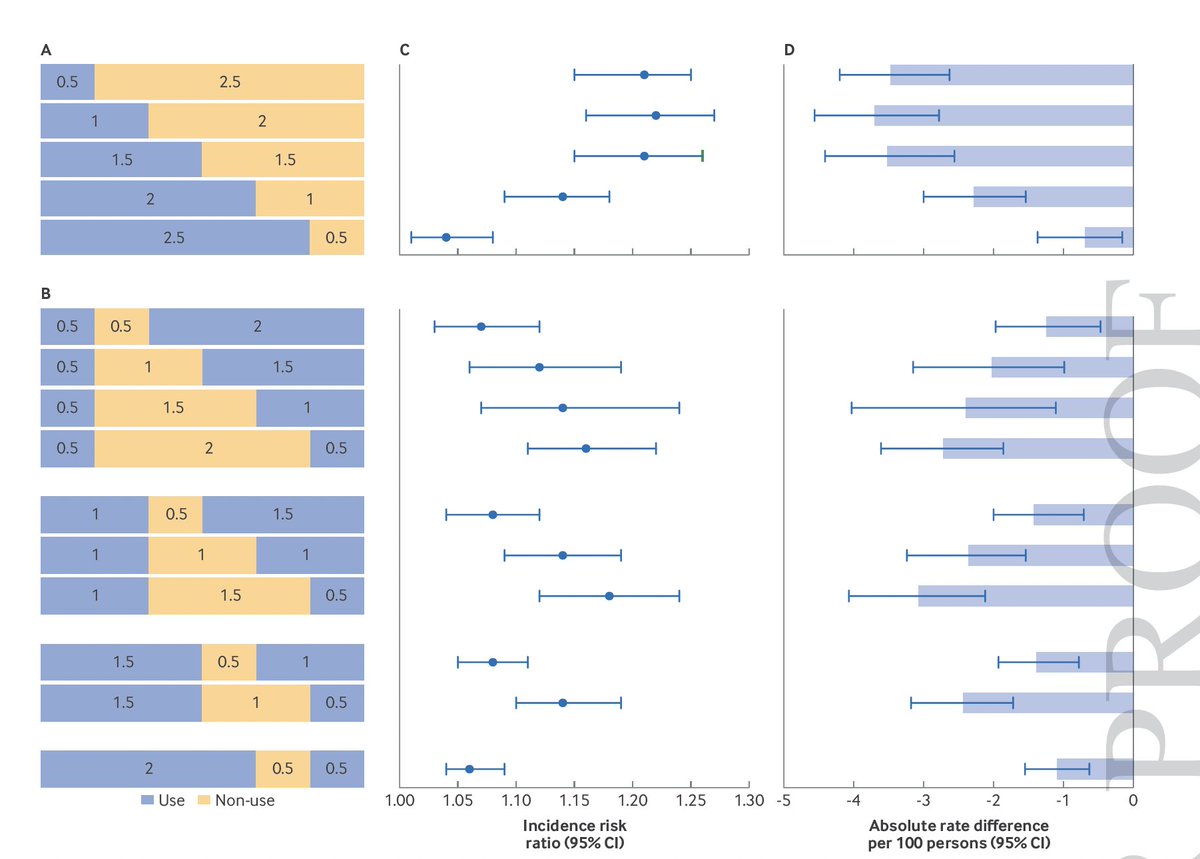
Here is the most striking finding:
What 3 years of continuous treatment builds, a year and a half off the drug can undo.
Protection accumulates slowly. It unravels quickly. That asymmetry may be the single most important clinical implication of this study.
What 3 years of continuous treatment builds, a year and a half off the drug can undo.
Protection accumulates slowly. It unravels quickly. That asymmetry may be the single most important clinical implication of this study.
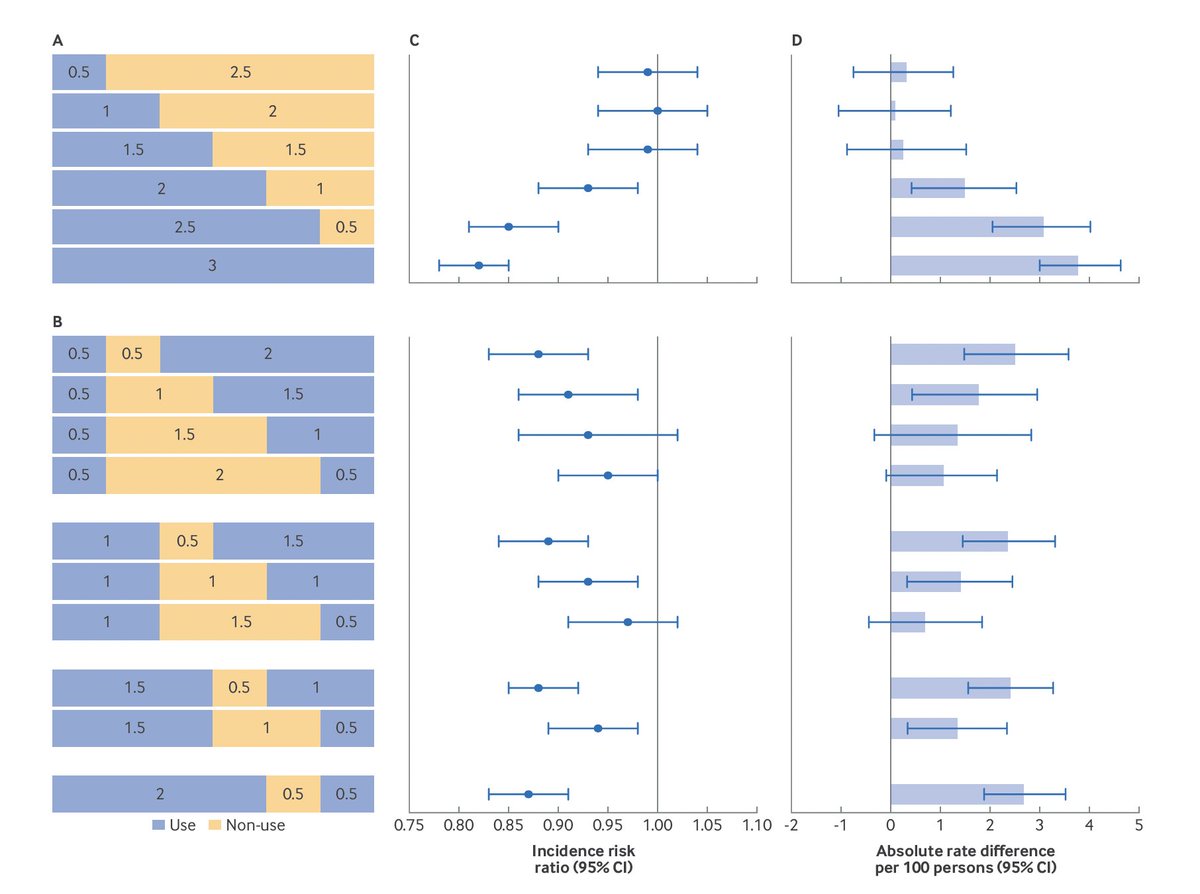
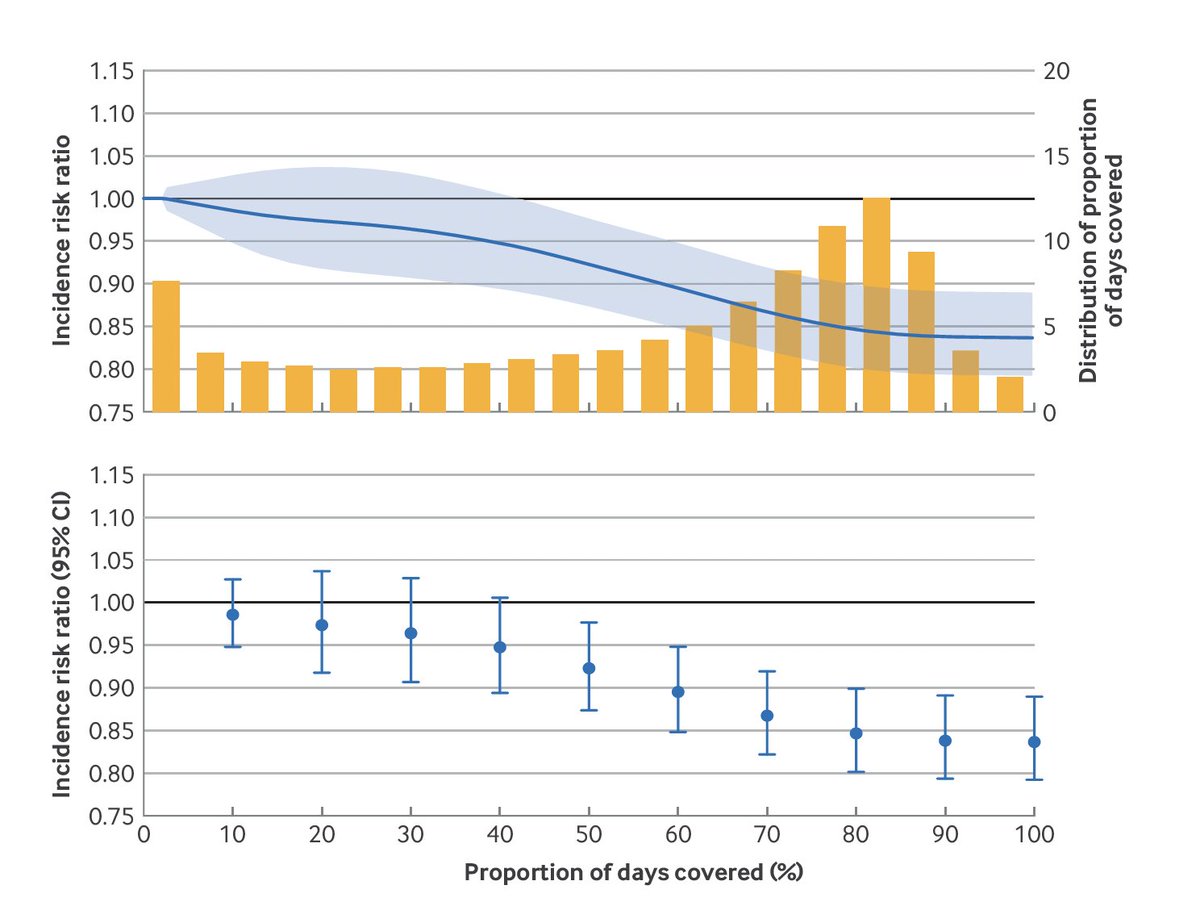
Using the drug for 0.5, 1, or even 1.5 years and then stopping produced no significant cardiovascular benefit at 3 years.
The risk ratios were close to 1.0 — as if the drug had never been taken.
The risk ratios were close to 1.0 — as if the drug had never been taken.
Restarting helped — but didn’t fully restore the protection of uninterrupted use.
Discontinuation leaves a lasting scar.
Discontinuation leaves a lasting scar.
This happened in the VA system, where copays are capped at $11/month. Over a quarter of users still discontinued entirely. Nearly another quarter had interruptions.
Cost matters — but it is far from the only reason people stop.
Cost matters — but it is far from the only reason people stop.
When people stop GLP-1 drugs, it’s not just weight that comes back. They experience a resurgence in inflammation, blood pressure, cholesterol, and insulin resistance.
Weight regain is visible. The metabolic reversal is not.
We think of this as a form of metabolic whiplash.
Weight regain is visible. The metabolic reversal is not.
We think of this as a form of metabolic whiplash.
GLP-1 drugs are not short-term treatments. They are long-term treatments, and patients, providers, and insurers all need to reckon with that. Stopping can undo years of accrued heart protection. 
Weight regain is visible. The metabolic reversal is not.
Stopping can undo years of heart protection.
Stopping can undo years of heart protection.

The heavy lifting here was done by the amazing @biostayan
Press release by the wonderful Shawn Ballard: medicine.washu.edu/news/stopping-…
@WashUMedicine @WashU @VAResearch
Paper:
bmjmedicine.bmj.com/content/5/1/e0…
Press release by the wonderful Shawn Ballard: medicine.washu.edu/news/stopping-…
@WashUMedicine @WashU @VAResearch
Paper:
bmjmedicine.bmj.com/content/5/1/e0…
• • •
Missing some Tweet in this thread? You can try to
force a refresh












