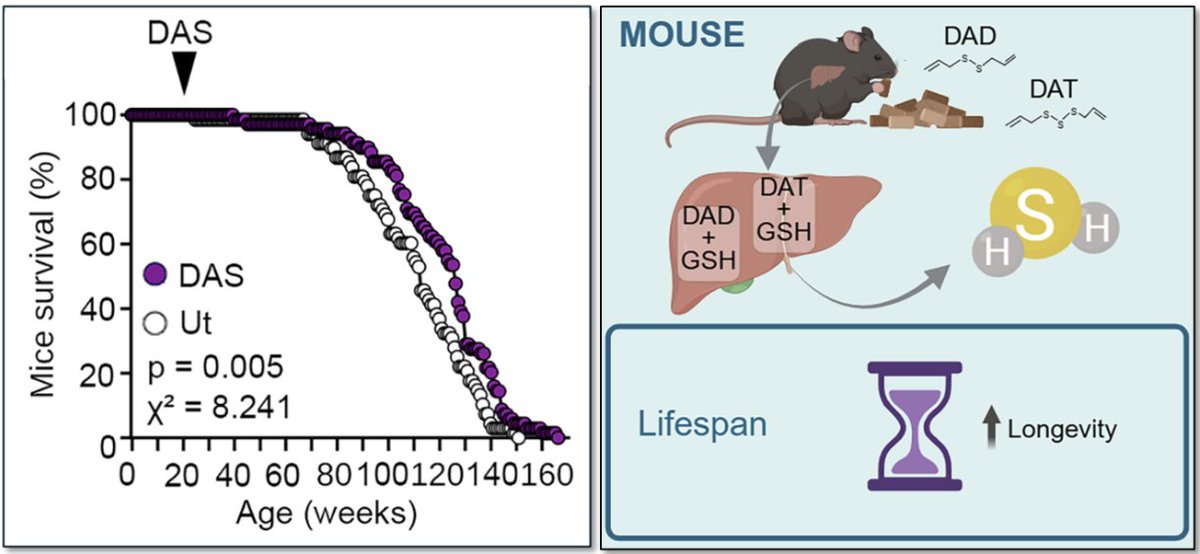
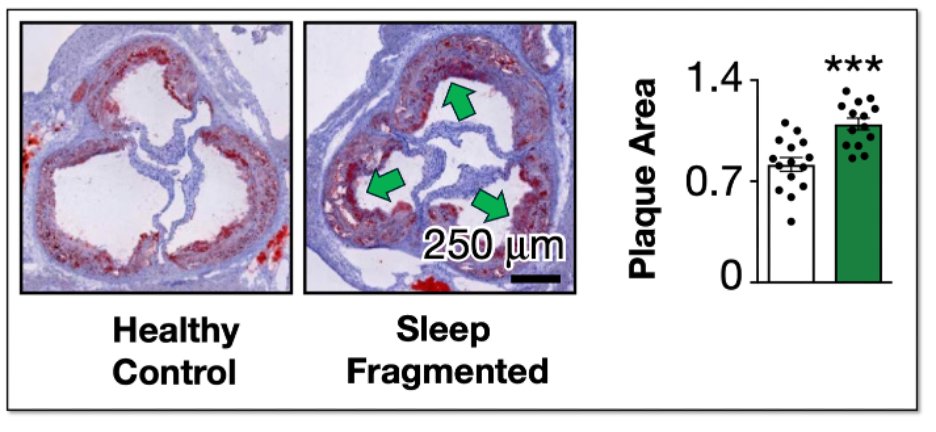
After 7 Years, I Changed My Mind on Cholesterol Meds (Or Did I?)
🚨You'll want to read this one all the way though. Link at the end🚨
1/7) After seven years of living with astronomically high cholesterol, I’ve decided to start two medications. Not statins, but ezetimibe and bempedoic acid.
But that’s NOT the real story. The real story is WHY… and it has nothing to do with cholesterol🤨🤔...
Quick preface: “cholesterol-lowering drugs” are named for one effect, not their full biological impact.
Molecules don’t respect our labels. These drugs can influence multiple systems, including metabolism and brain health.
And in this case, they likely do.

🚨You'll want to read this one all the way though. Link at the end🚨
1/7) After seven years of living with astronomically high cholesterol, I’ve decided to start two medications. Not statins, but ezetimibe and bempedoic acid.
But that’s NOT the real story. The real story is WHY… and it has nothing to do with cholesterol🤨🤔...
Quick preface: “cholesterol-lowering drugs” are named for one effect, not their full biological impact.
Molecules don’t respect our labels. These drugs can influence multiple systems, including metabolism and brain health.
And in this case, they likely do.
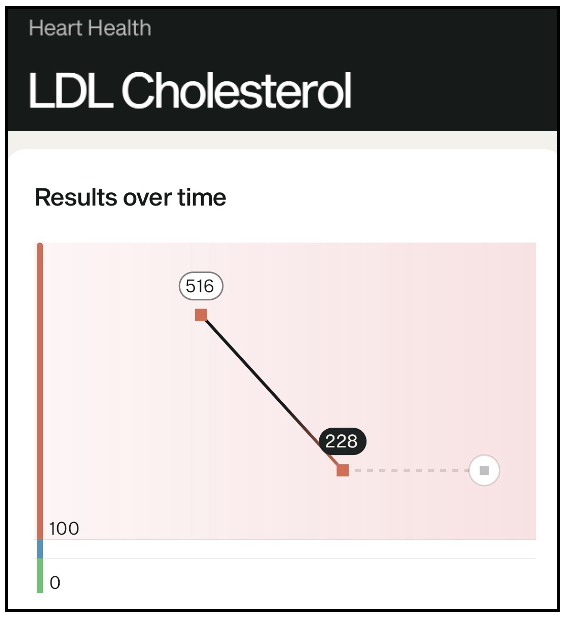
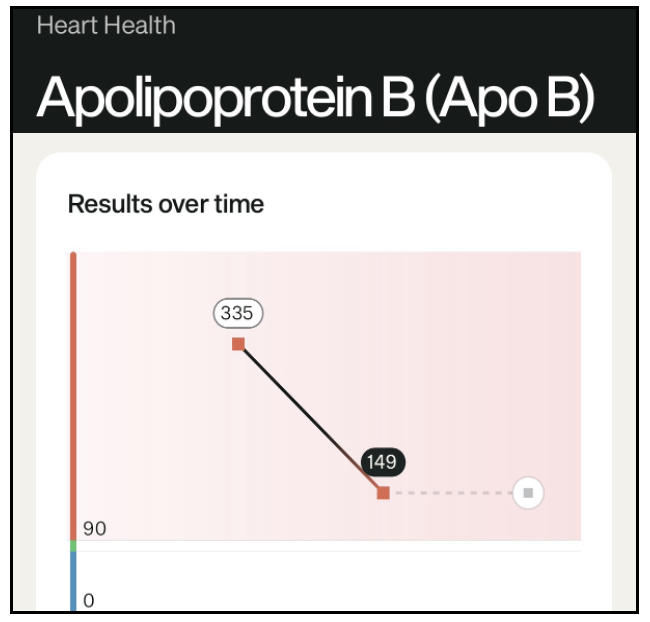
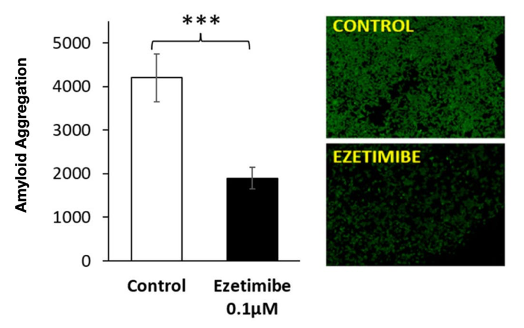
2/7) Take ezetimibe. Beyond lowering LDL, evidence suggests it crosses into the brain and influences neurobiology.
Specifically, is disrupts the interaction between 14-3-3 and hexokinase, reducing protein aggregation.
Full video:
Specifically, is disrupts the interaction between 14-3-3 and hexokinase, reducing protein aggregation.
Full video:
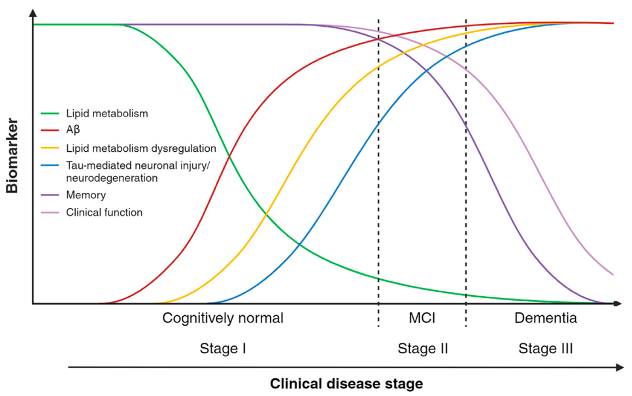
3/7) That means less amyloid, less tau, and even improved autophagy.
Even more interesting: retrospective analyses have found up to an ~8x lower risk of Alzheimer’s in patients on ezetimibe.
Not causal. Not definitive. But a signal worth paying attention to—especially in the right context.
Even more interesting: retrospective analyses have found up to an ~8x lower risk of Alzheimer’s in patients on ezetimibe.
Not causal. Not definitive. But a signal worth paying attention to—especially in the right context.
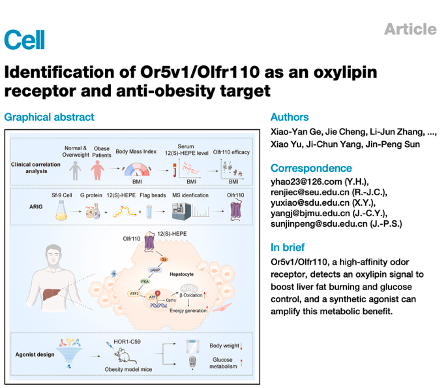
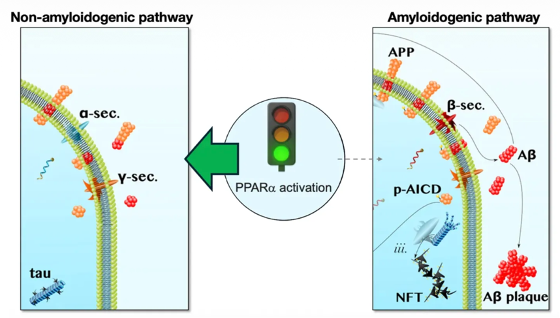
4/7) Then there’s bempedoic acid. New research (Cell Metabolism, May 2026) suggests even its “inactive” form is biologically active—binding PPAR-alpha.
That matters because PPAR-alpha can shift amyloid processing toward a neuroprotective pathway.
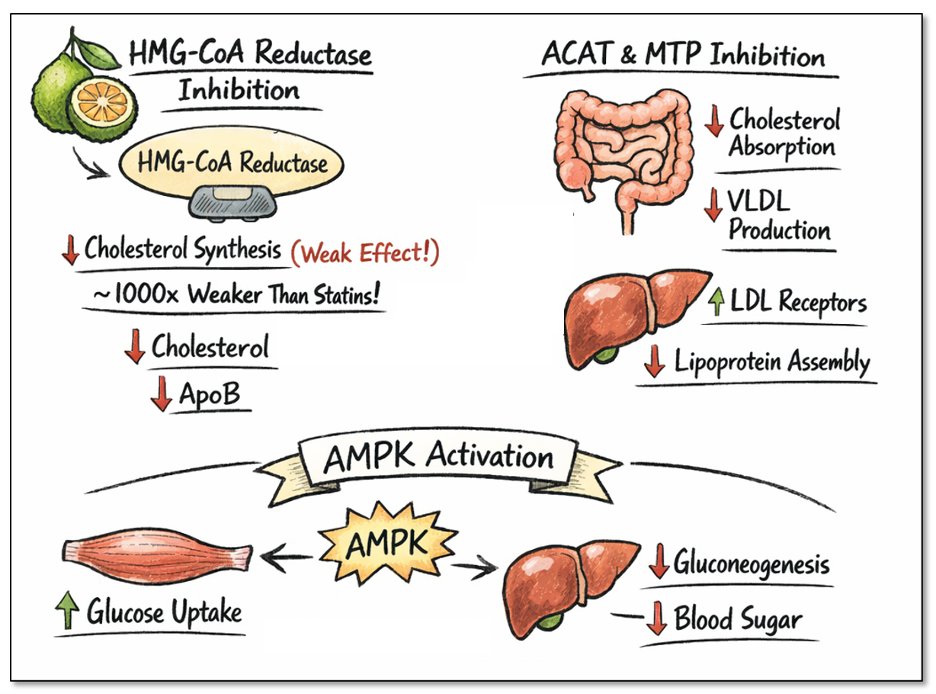
(image modified from Norwitz et al. 2019)
That matters because PPAR-alpha can shift amyloid processing toward a neuroprotective pathway.
(image modified from Norwitz et al. 2019)
5/7) So no, this isn’t a story about “I changed my mind and lower cholesterol is better.”
It’s a story about nuance, mechanisms, and staying open to new evidence. Don’t let labels or dogma do your thinking for you.
But there’s more…
It’s a story about nuance, mechanisms, and staying open to new evidence. Don’t let labels or dogma do your thinking for you.
But there’s more…

6/7) But let me pause and make an important aside.
Speaking directly to those who have followed the research my colleagues and I have been doing on cholesterol, particularly in the context of the very real lean mass hyper-responder phenotype cc @PeterAttiaMD: I recognize that this work has raised a lot of questions… and just as many misrepresentations.
So let me be clear:
This is not a pivot. It’s not an attention grab.
For those who have actually been following the thread, the message has always been the same:
Interpret data with an open mind, and within your individual context.
And don’t let other people’s caricatures of what they think you believe dictate how you think.
In my case, I’m more than willing to look at molecules traditionally labeled as “cholesterol-lowering drugs,” recognize that they may have multiple biological effects, and use those effects as tools where appropriate.
That’s not inconsistency. That's perfect consistency if you've been following our work, rather than some manipulated cartoon version of it.
Now, of course, some will try to twist this message to fit their own narrative.
Because, frankly, much of modern cardiology—and medicine more broadly—still treats LDL cholesterol as the central pillar of health, rather than what it may actually be: one very small piece of a much larger and more complex system.
But let’s not let that kind of closed-mindedness spread.
Science is not settled. It never is. Stay open. Stay rigorous. And above all—stay genuinely curious.
Speaking directly to those who have followed the research my colleagues and I have been doing on cholesterol, particularly in the context of the very real lean mass hyper-responder phenotype cc @PeterAttiaMD: I recognize that this work has raised a lot of questions… and just as many misrepresentations.
So let me be clear:
This is not a pivot. It’s not an attention grab.
For those who have actually been following the thread, the message has always been the same:
Interpret data with an open mind, and within your individual context.
And don’t let other people’s caricatures of what they think you believe dictate how you think.
In my case, I’m more than willing to look at molecules traditionally labeled as “cholesterol-lowering drugs,” recognize that they may have multiple biological effects, and use those effects as tools where appropriate.
That’s not inconsistency. That's perfect consistency if you've been following our work, rather than some manipulated cartoon version of it.
Now, of course, some will try to twist this message to fit their own narrative.
Because, frankly, much of modern cardiology—and medicine more broadly—still treats LDL cholesterol as the central pillar of health, rather than what it may actually be: one very small piece of a much larger and more complex system.
But let’s not let that kind of closed-mindedness spread.
Science is not settled. It never is. Stay open. Stay rigorous. And above all—stay genuinely curious.
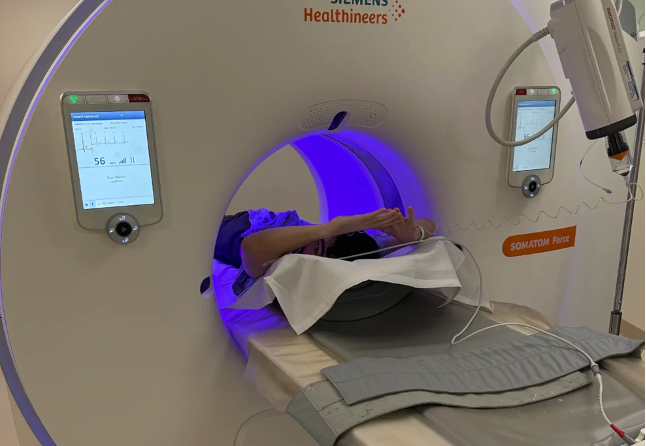
7/7) But now, for the moment of truth. Because for nearly 7 years, I’ve been running a natural experiment: total cholesterol ~700 and off-the-charts ApoB. If conventional thinking holds, my arteries should be full of plaque.
So, let’s test it. I’m getting an advanced coronary CT angiography with expert and AI analysis.
Let’s see what the data actually say. Any guesses?
Deep dive: staycuriousmetabolism.substack.com/p/im-finally-l…
So, let’s test it. I’m getting an advanced coronary CT angiography with expert and AI analysis.
Let’s see what the data actually say. Any guesses?
Deep dive: staycuriousmetabolism.substack.com/p/im-finally-l…
• • •
Missing some Tweet in this thread? You can try to
force a refresh