How to get URL link on X (Twitter) App




 2/n Joint aspirated. Low clinical suspicion of septic arthritis, thus simultaneously injected with triamcinolone+lidocaine (rheumatology colleagues supported the decision).
2/n Joint aspirated. Low clinical suspicion of septic arthritis, thus simultaneously injected with triamcinolone+lidocaine (rheumatology colleagues supported the decision).

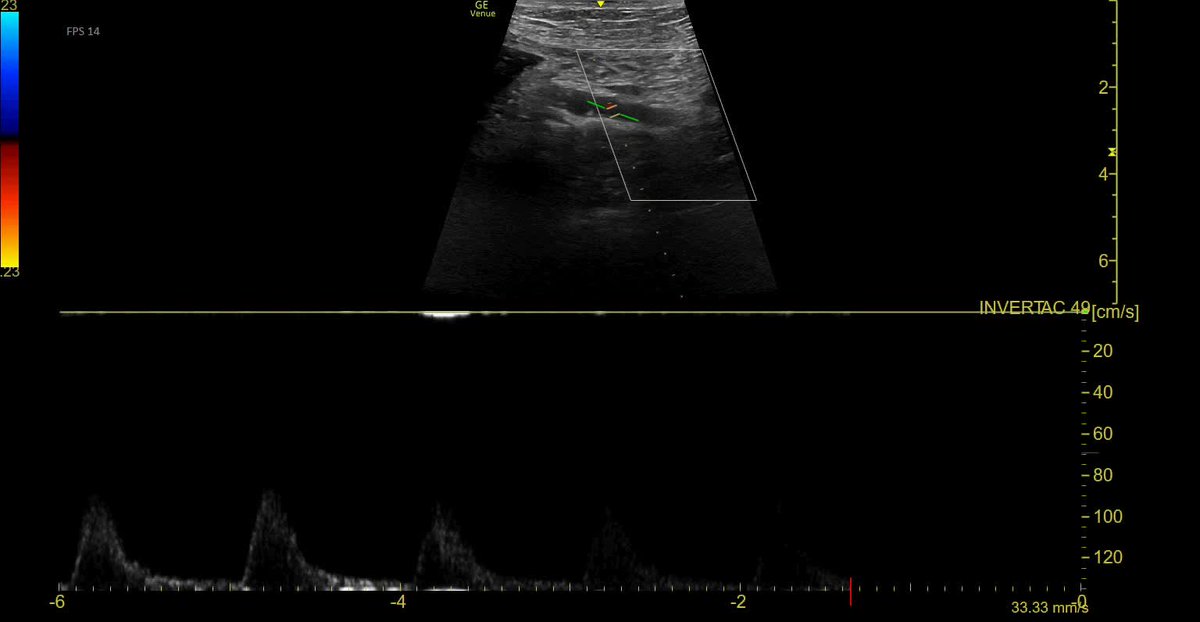
 2/n The normal (Left) testis - shows normal internal septal architecture with pulsatile blood flow on color power doppler, with normal overlying skin thickness.
2/n The normal (Left) testis - shows normal internal septal architecture with pulsatile blood flow on color power doppler, with normal overlying skin thickness.





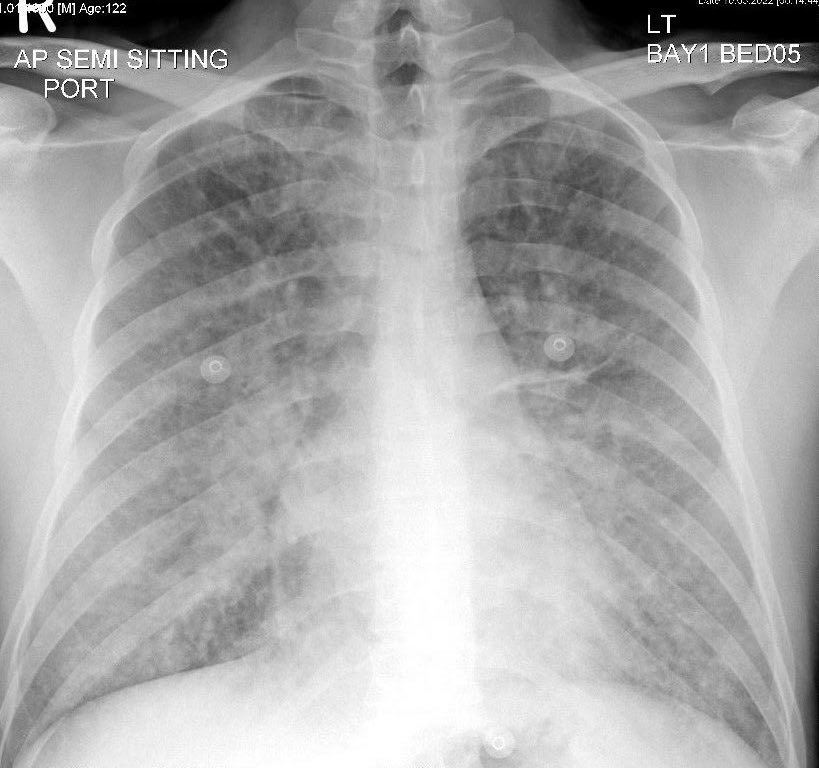
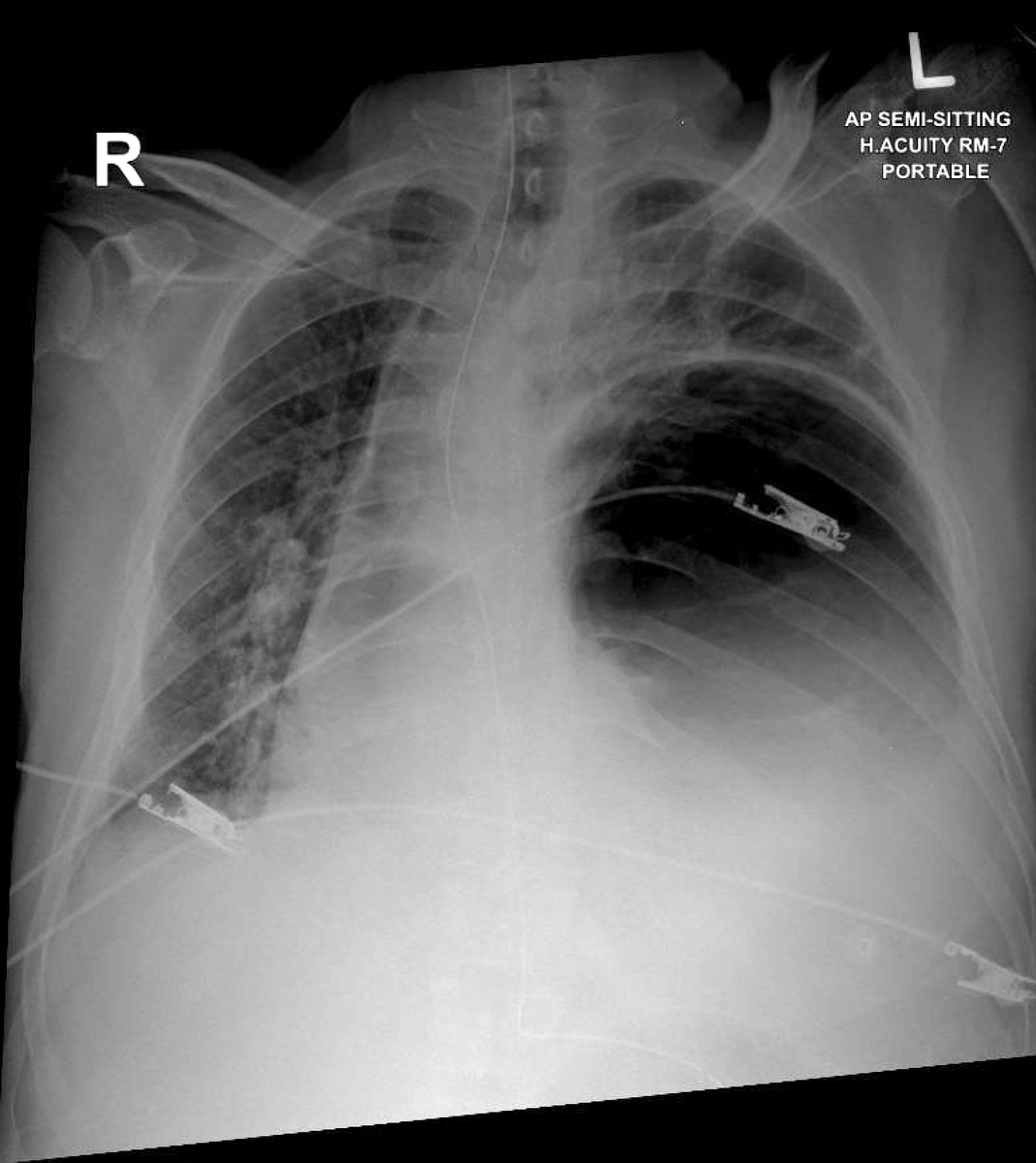
 2/n #POCUS all lung zones show B-lines as expected, but minimal left pleural effusion which is NOT common with COVID-19.
2/n #POCUS all lung zones show B-lines as expected, but minimal left pleural effusion which is NOT common with COVID-19.
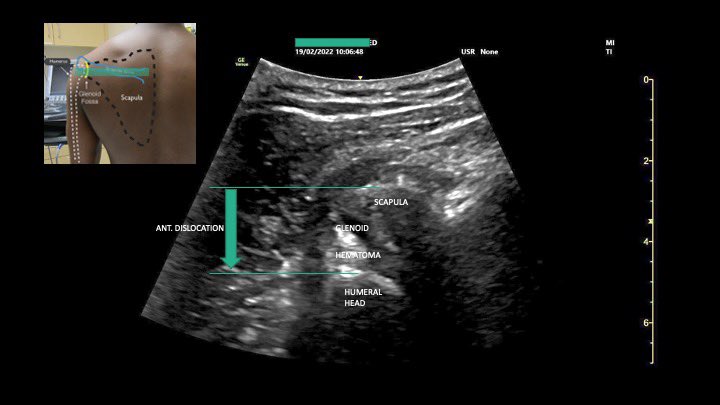
 2/3 Pain 10/10 to 0/10 within 5 min of interscalene block
2/3 Pain 10/10 to 0/10 within 5 min of interscalene block


 2/n #POCUS showed bilateral small basal consolidations, B-lines at right base with sub pleural consolidations. Right posterior basal region sub pleural consolidation -
2/n #POCUS showed bilateral small basal consolidations, B-lines at right base with sub pleural consolidations. Right posterior basal region sub pleural consolidation -