
Aerospace engineer by training, ME/CFS & Long COVID patient researcher, cofounder @amaticahealth. DMs open, rarely check follows - https://t.co/BvmsOvch0p
How to get URL link on X (Twitter) App

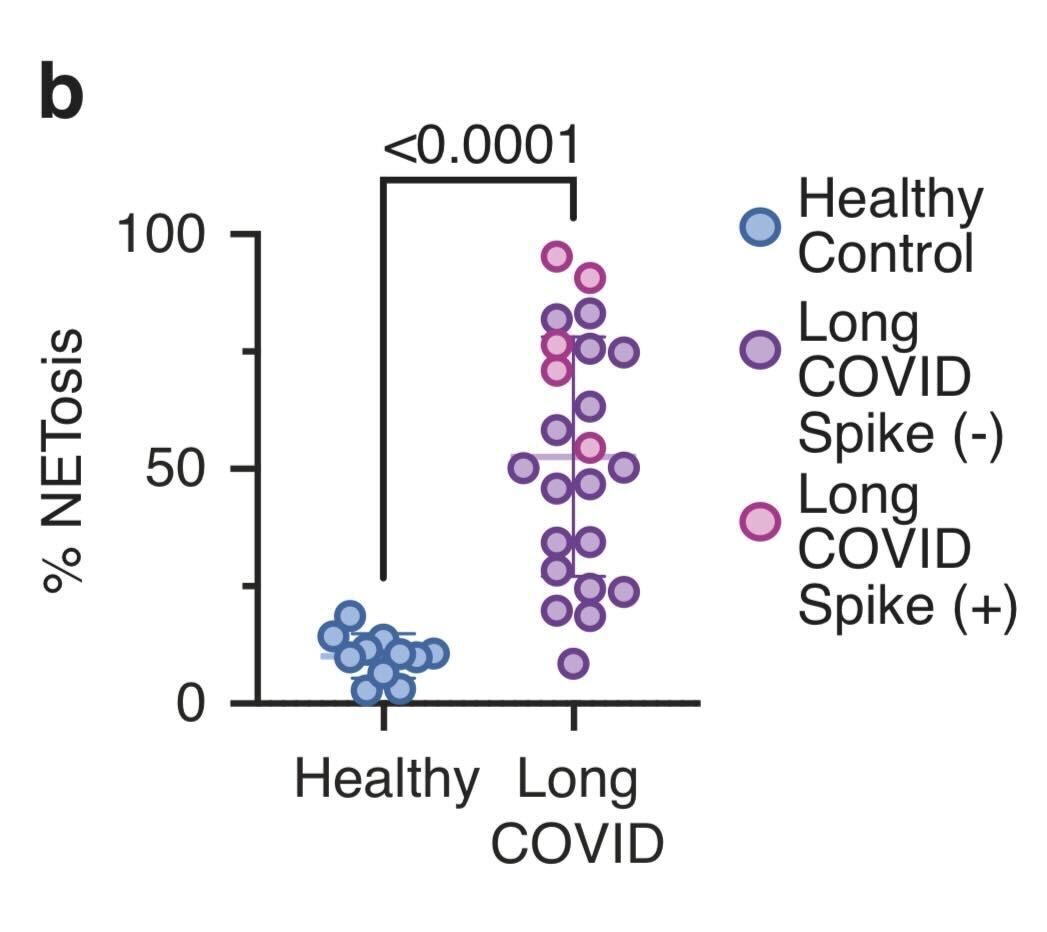
 The study included 84 people aged 25 or younger: 61 with long COVID and 23 healthy controls. The long COVID group had common circulation-type symptoms, including dizziness when standing, shortness of breath on stairs, and palpitations.
The study included 84 people aged 25 or younger: 61 with long COVID and 23 healthy controls. The long COVID group had common circulation-type symptoms, including dizziness when standing, shortness of breath on stairs, and palpitations.
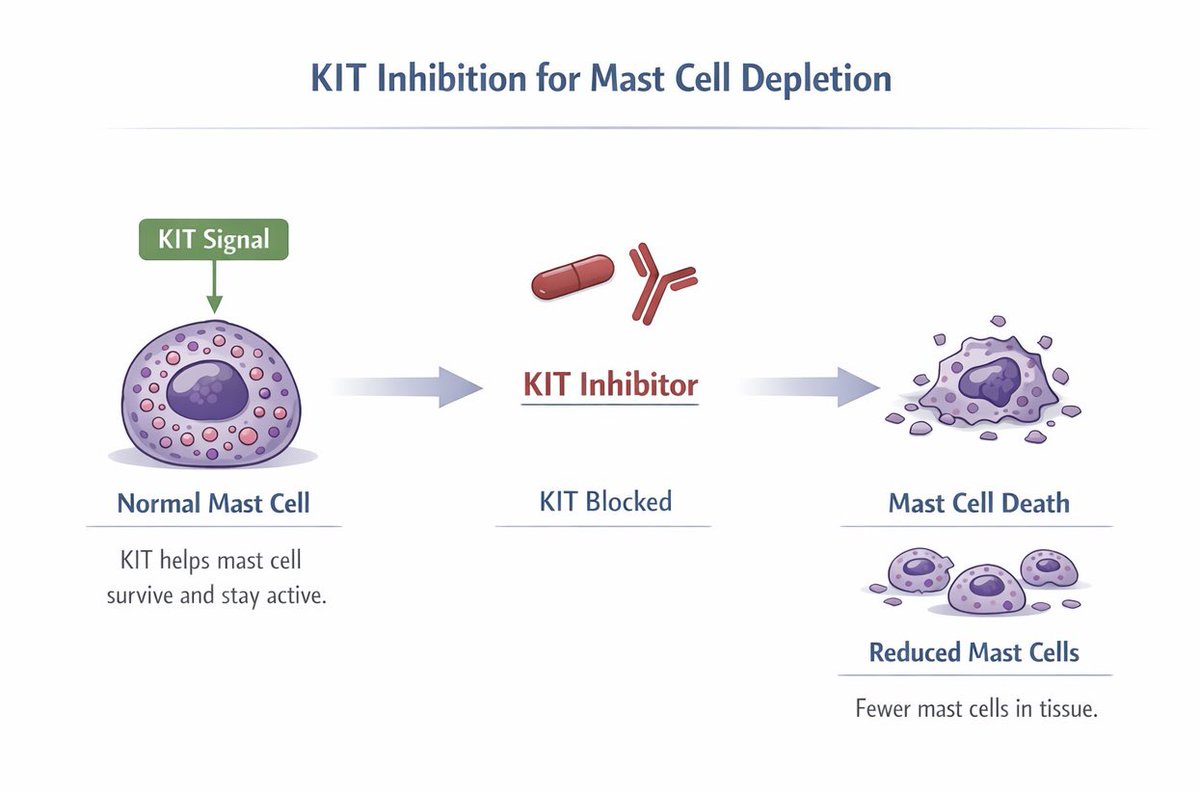
 CSU is chronic spontaneous urticaria.
CSU is chronic spontaneous urticaria. 
 Older ME/CFS brain scans often disagreed. The usual method can show change, but not clearly whether it means extra fluid, extra cells, damaged fibres, or something else. This also builds on earlier blood and brain-scan work that hinted at inflammation.
Older ME/CFS brain scans often disagreed. The usual method can show change, but not clearly whether it means extra fluid, extra cells, damaged fibres, or something else. This also builds on earlier blood and brain-scan work that hinted at inflammation.
 Those tiny particles are extracellular vesicles (EVs). EVs are small packages released by cells into the blood that can carry proteins and other material.
Those tiny particles are extracellular vesicles (EVs). EVs are small packages released by cells into the blood that can carry proteins and other material.
 Researchers wanted to test a simple question.
Researchers wanted to test a simple question.
 This pattern repeats:
This pattern repeats: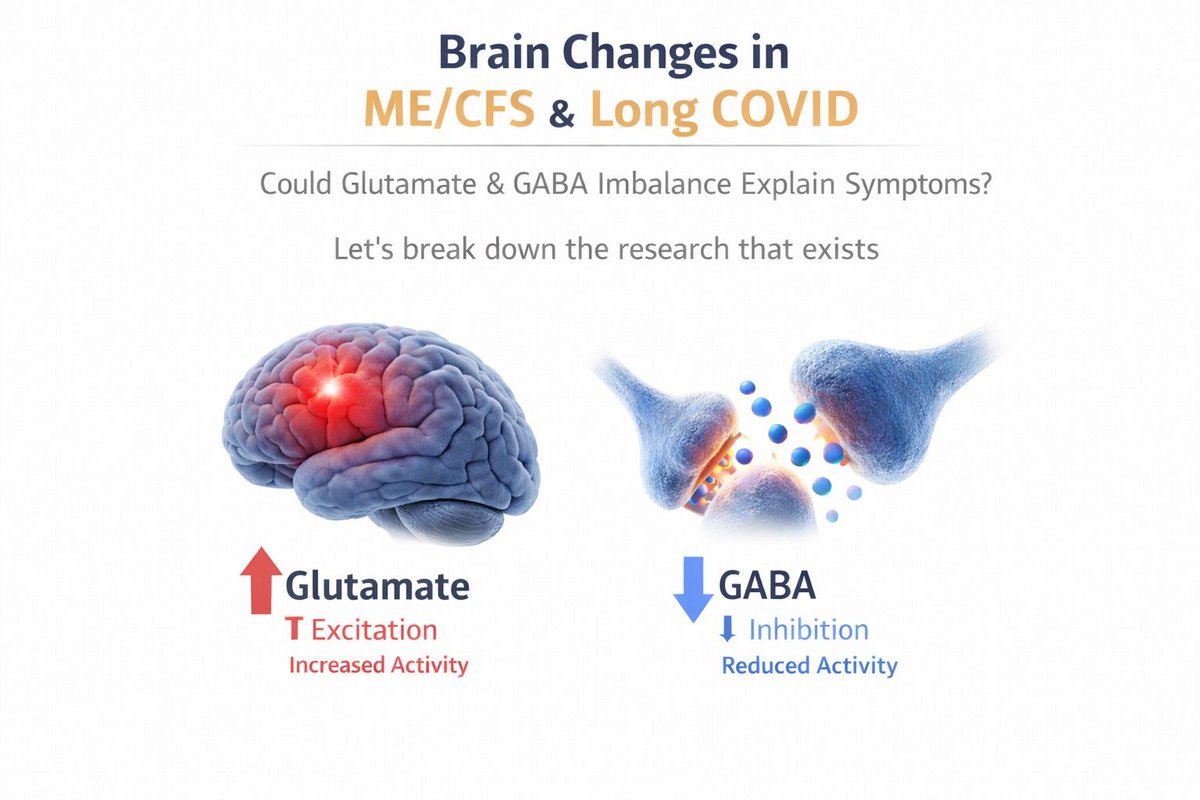
 Glutamate is a main brain signal that increases nerve cell activity.
Glutamate is a main brain signal that increases nerve cell activity. 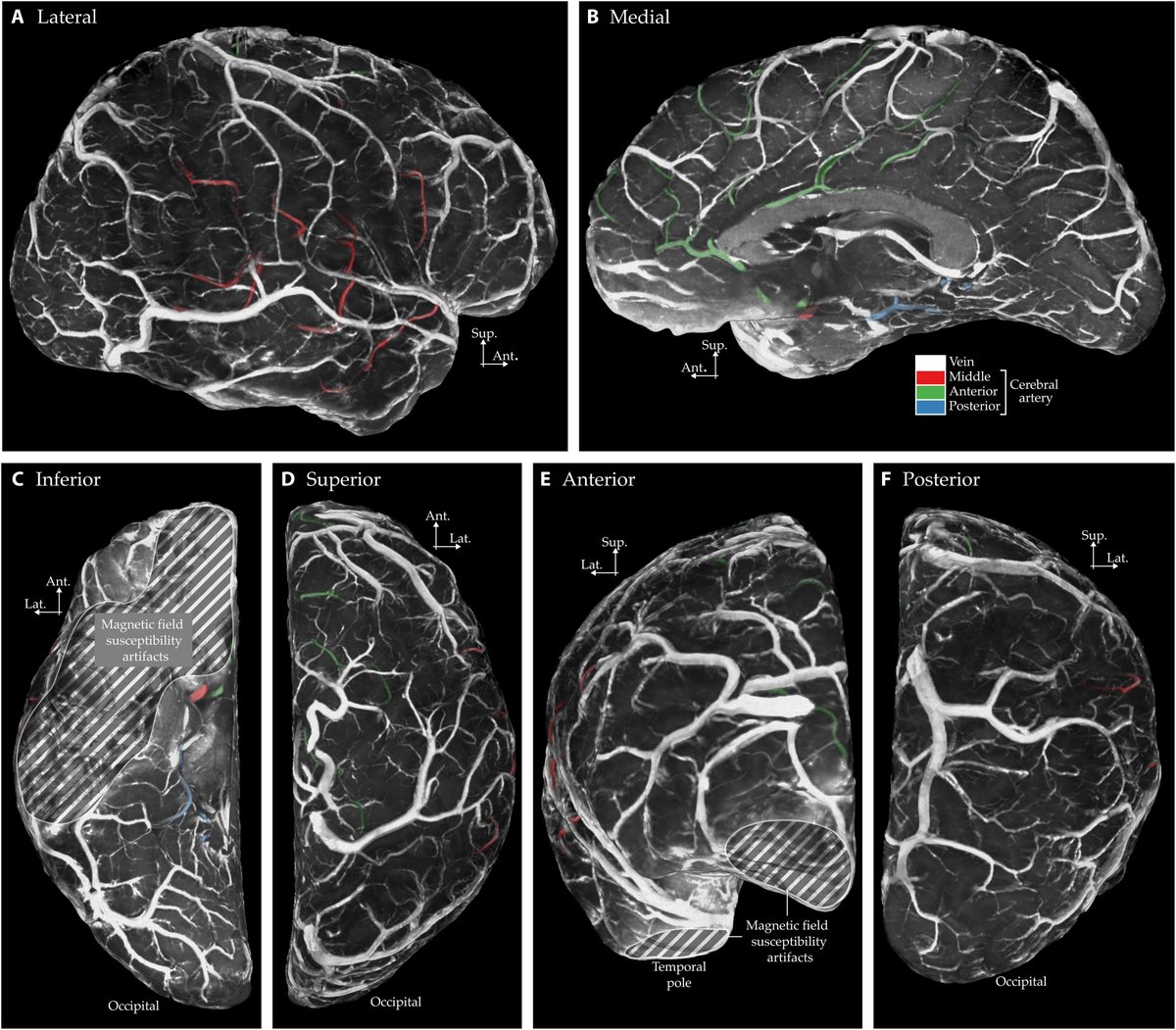
 The study used a very strong MRI scanner called 7-Tesla.
The study used a very strong MRI scanner called 7-Tesla.