Your guide to a healthy heart and body.
Evidence-based cardiology content..
Tweets are only for educational purposes.
How to get URL link on X (Twitter) App


 A 54-year-old woman was admitted with septic shock secondary to an intra-abdominal infection.
A 54-year-old woman was admitted with septic shock secondary to an intra-abdominal infection.
 2/ Main causes of AS:
2/ Main causes of AS: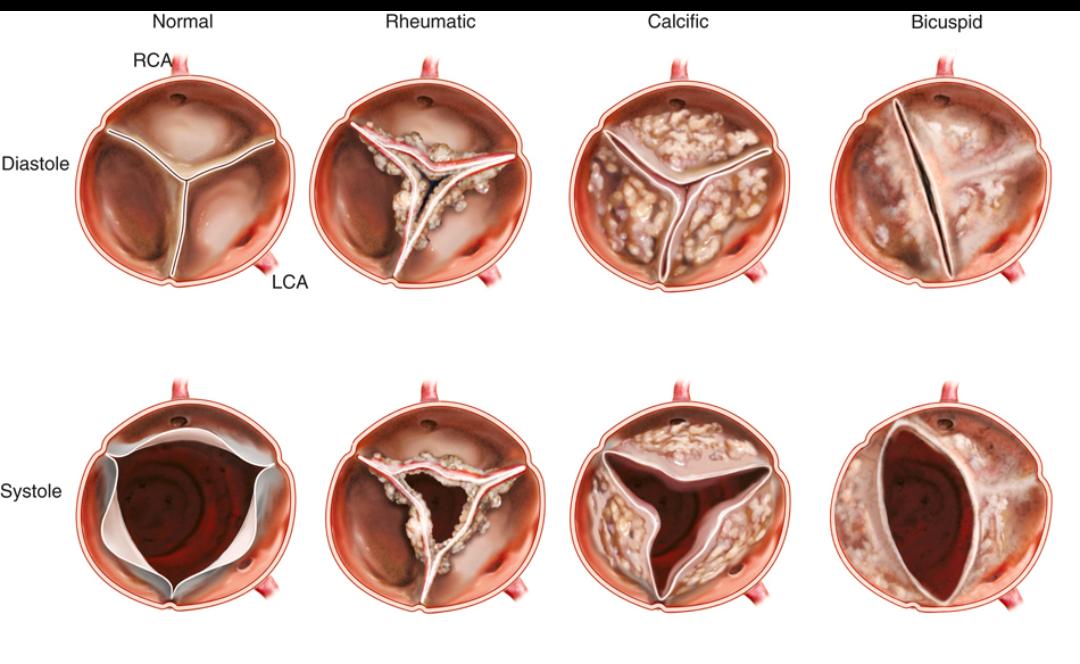

 1️⃣ When to Suspect RV Infarction?
1️⃣ When to Suspect RV Infarction?

 1/
1/
 Step 0: Initial Checks
Step 0: Initial Checks

 1/
1/
 1/
1/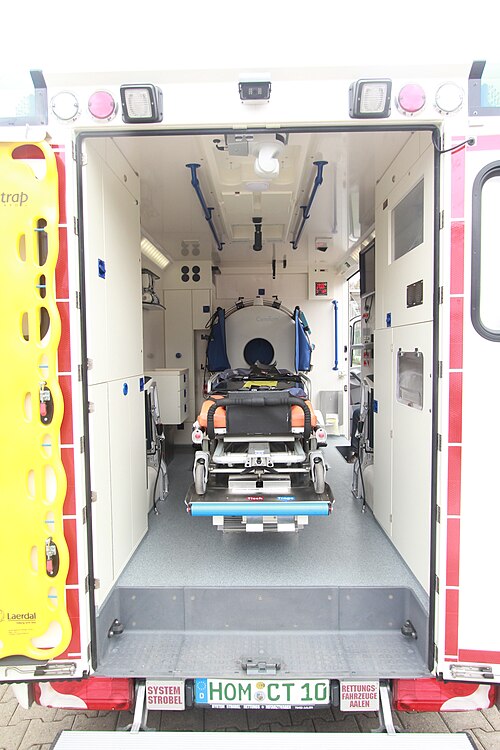

 1️⃣ Start earlier.
1️⃣ Start earlier.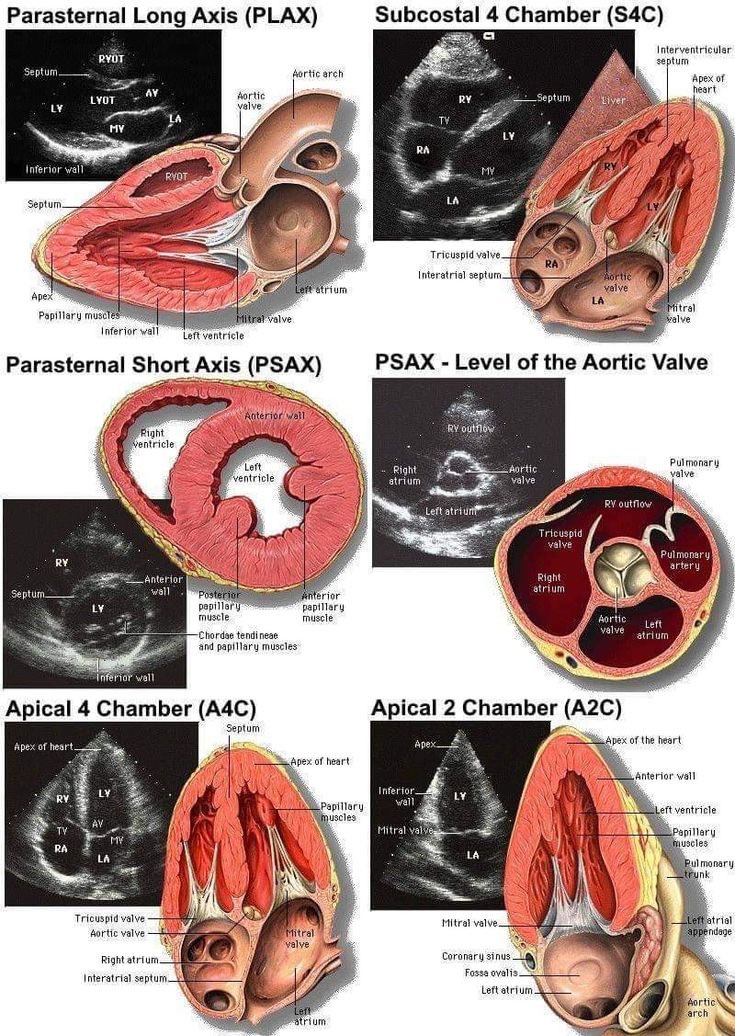
 2/
2/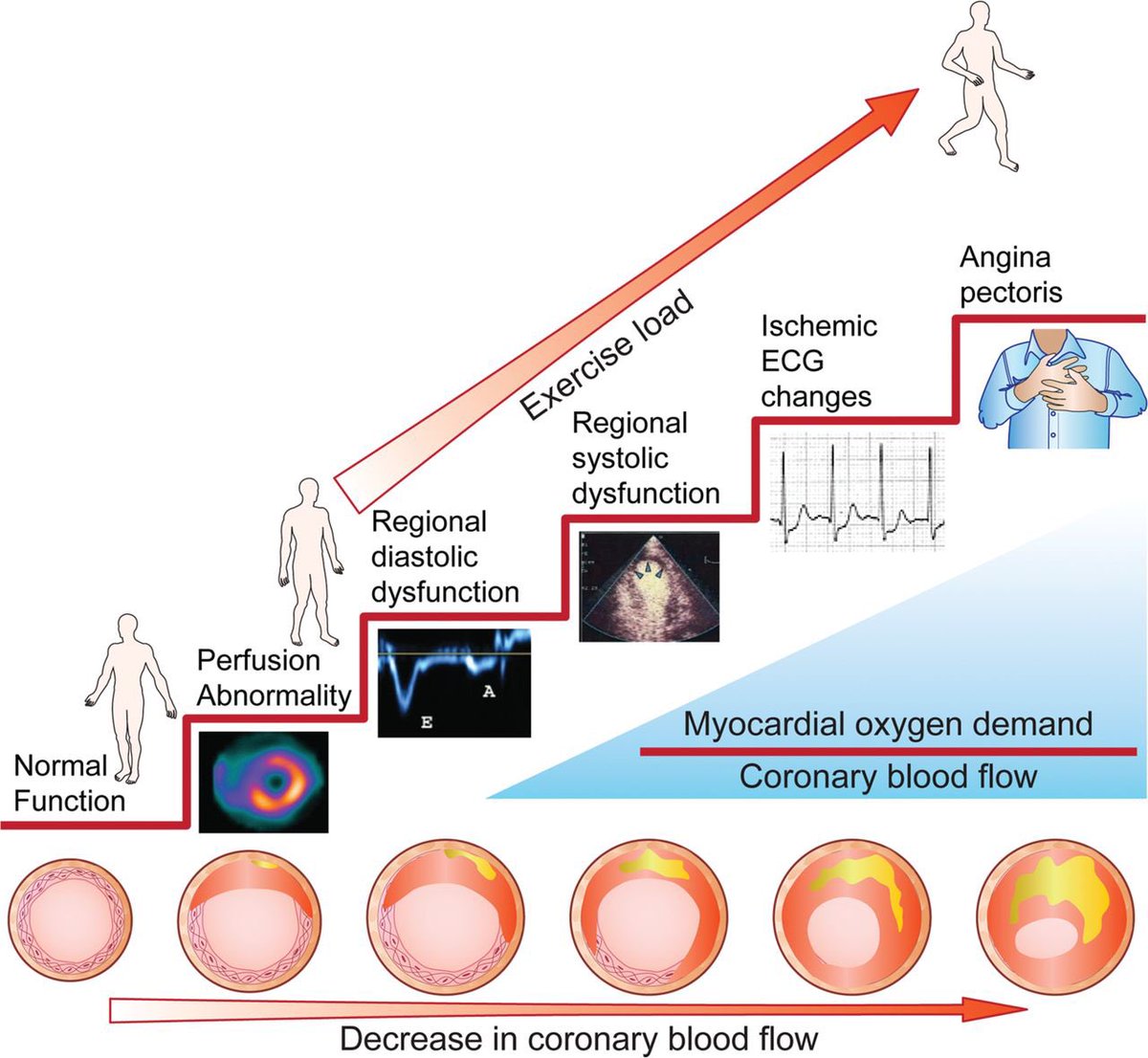
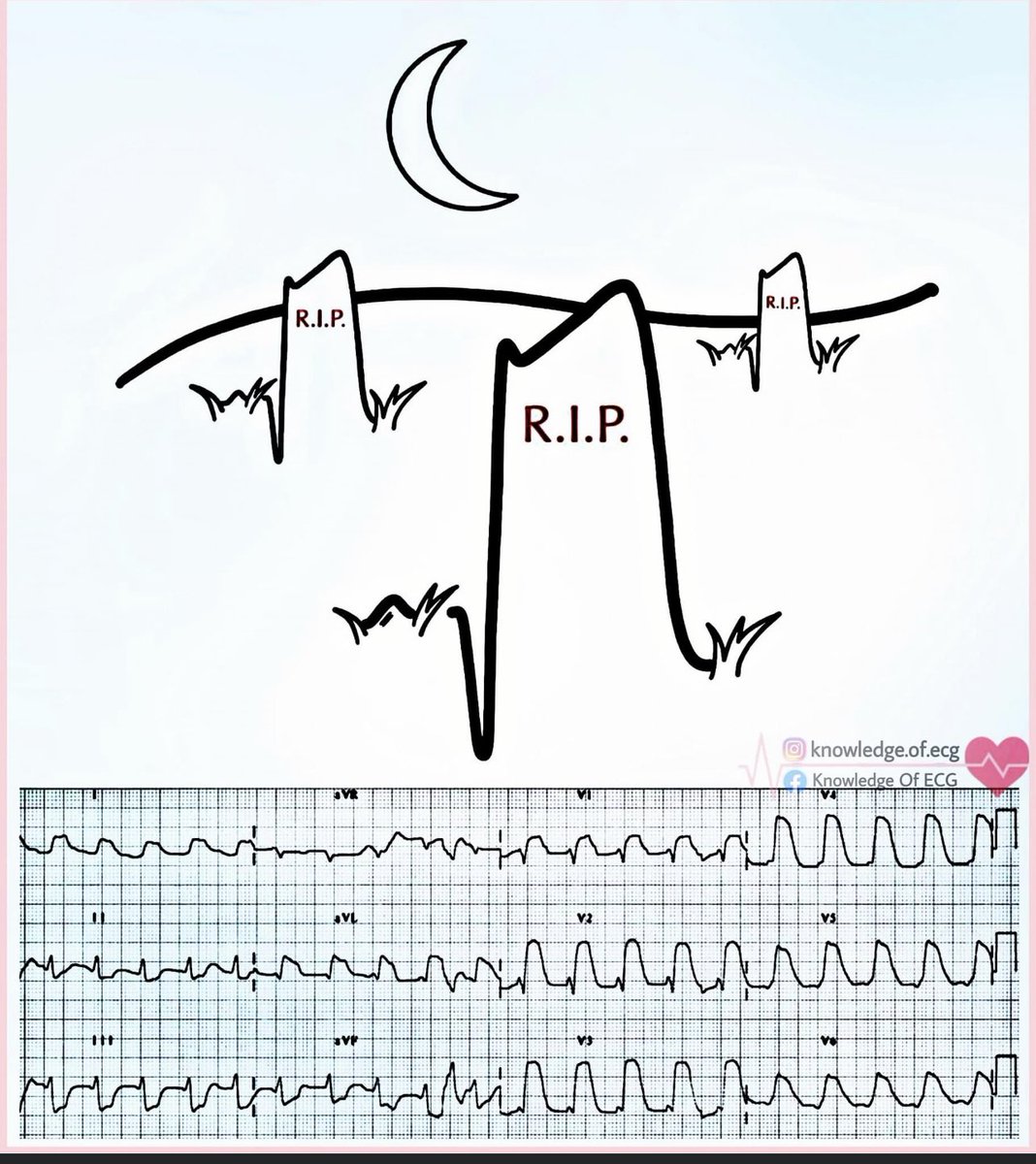
 1️⃣ Acute Coronary Occlusion (STEMI)
1️⃣ Acute Coronary Occlusion (STEMI)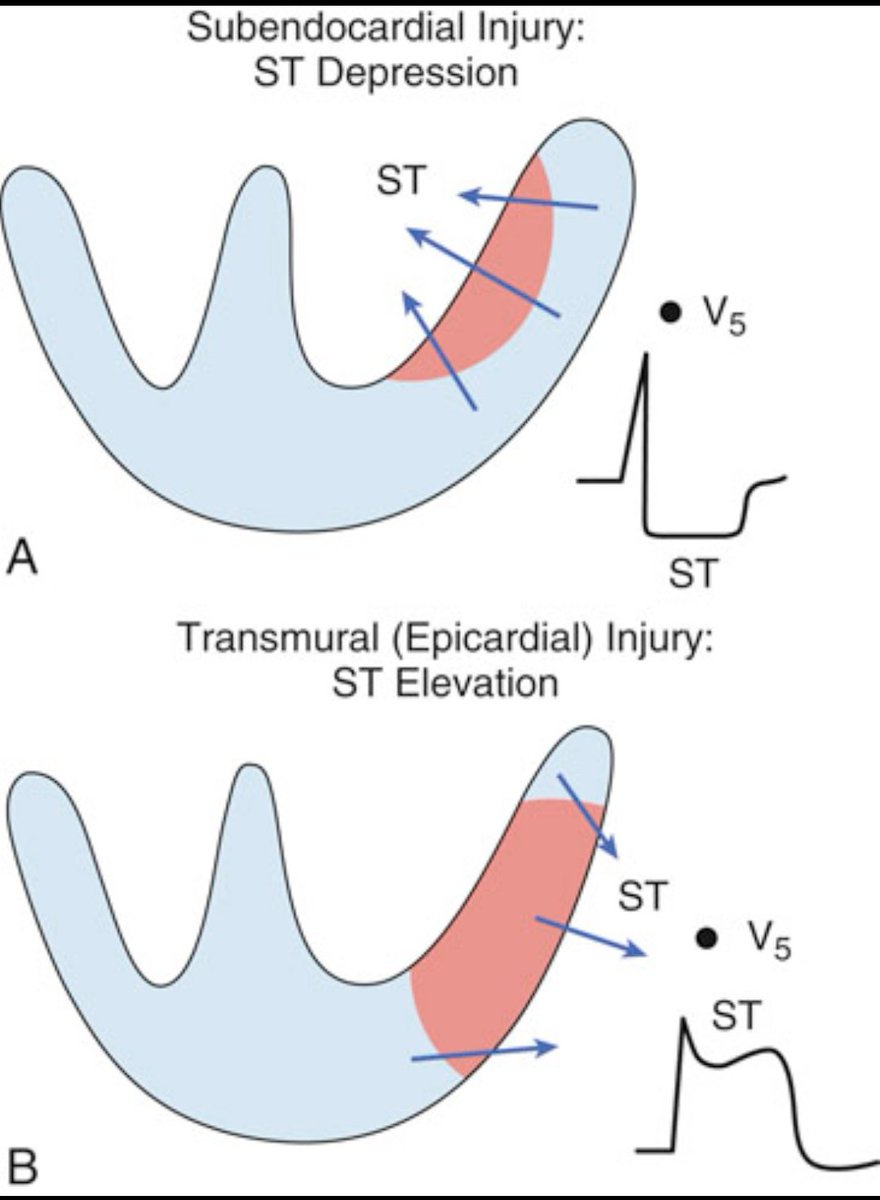

 1/ Holter Monitor
1/ Holter Monitor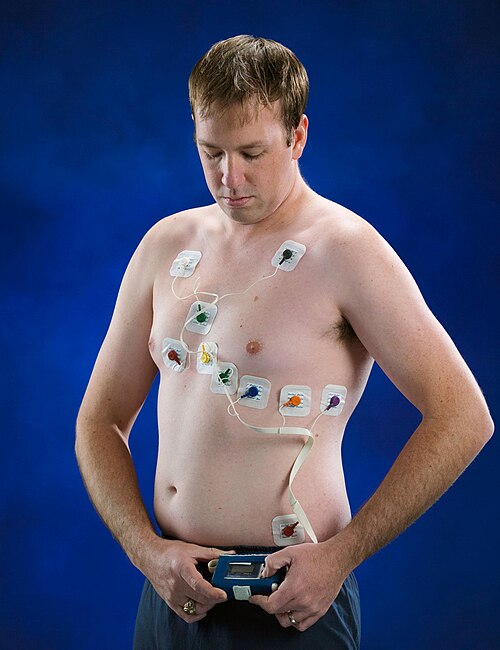
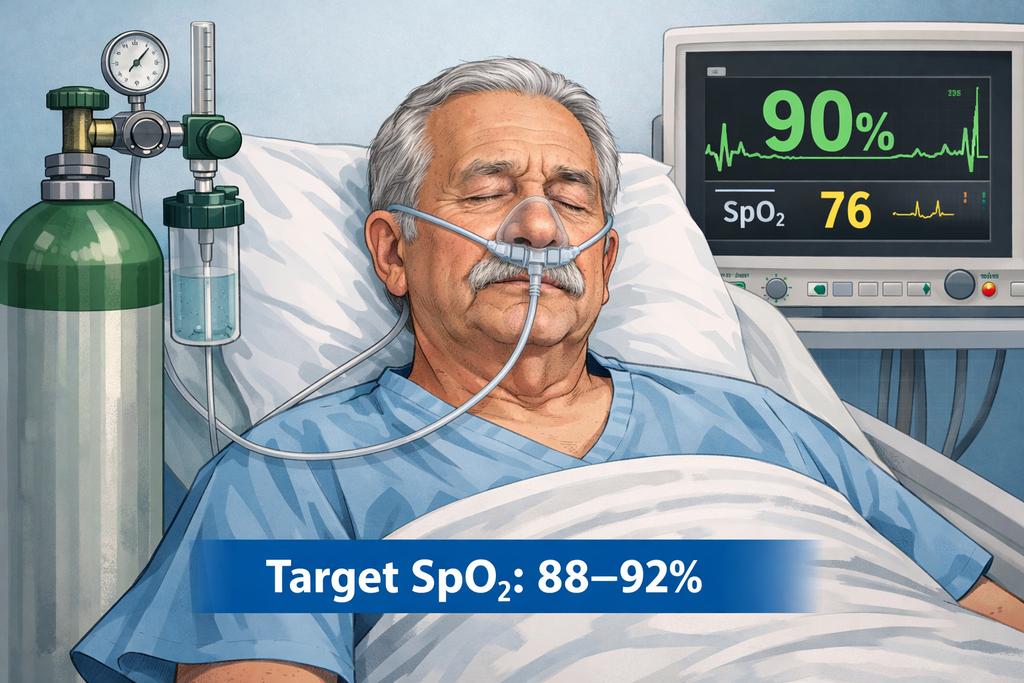
 Oxygen does NOT usually cause dangerous hypercapnia by stopping breathing.
Oxygen does NOT usually cause dangerous hypercapnia by stopping breathing.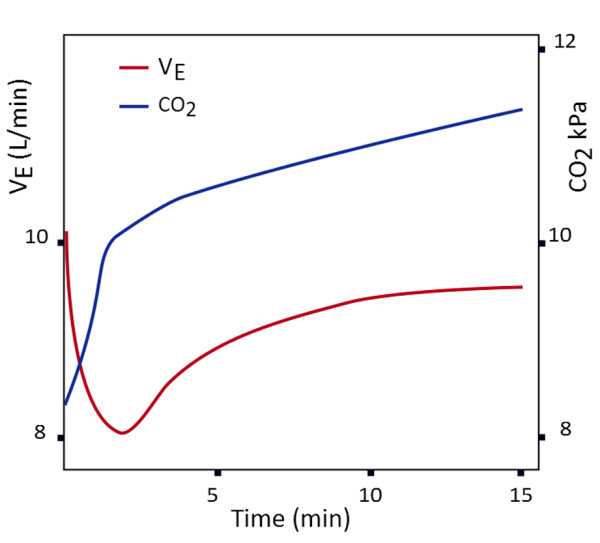

 1/
1/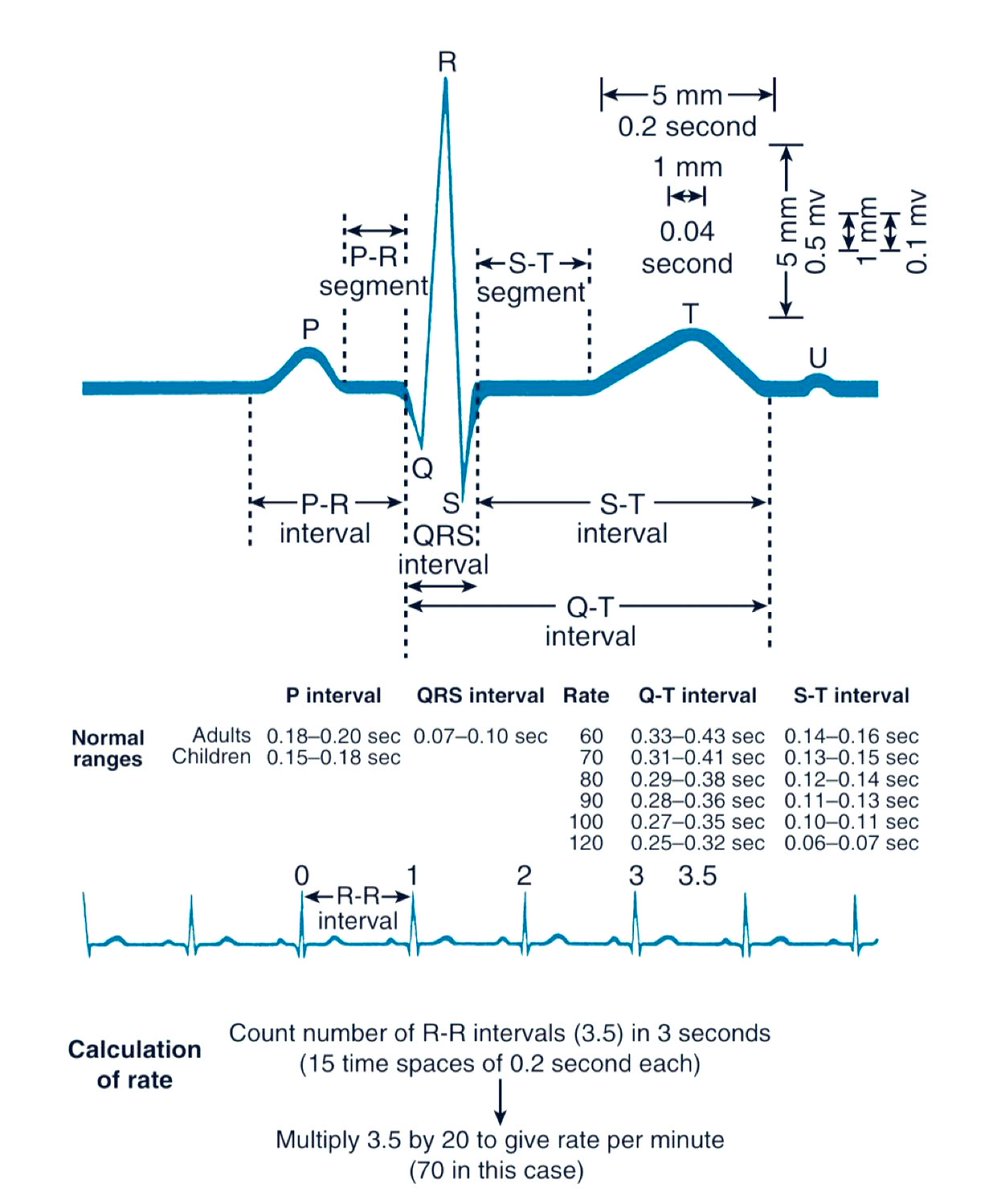
 Step 0: Initial Checks
Step 0: Initial Checks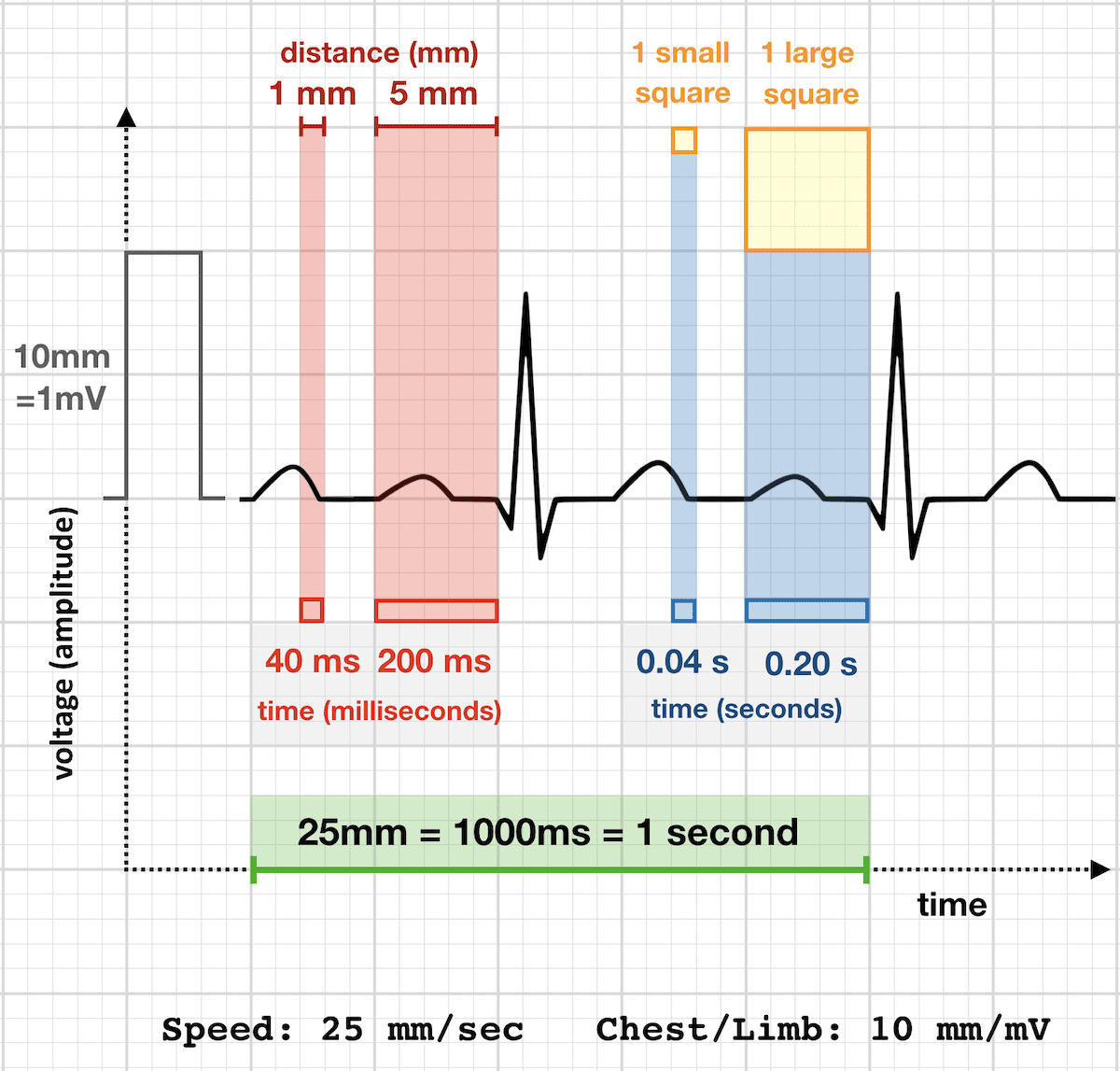
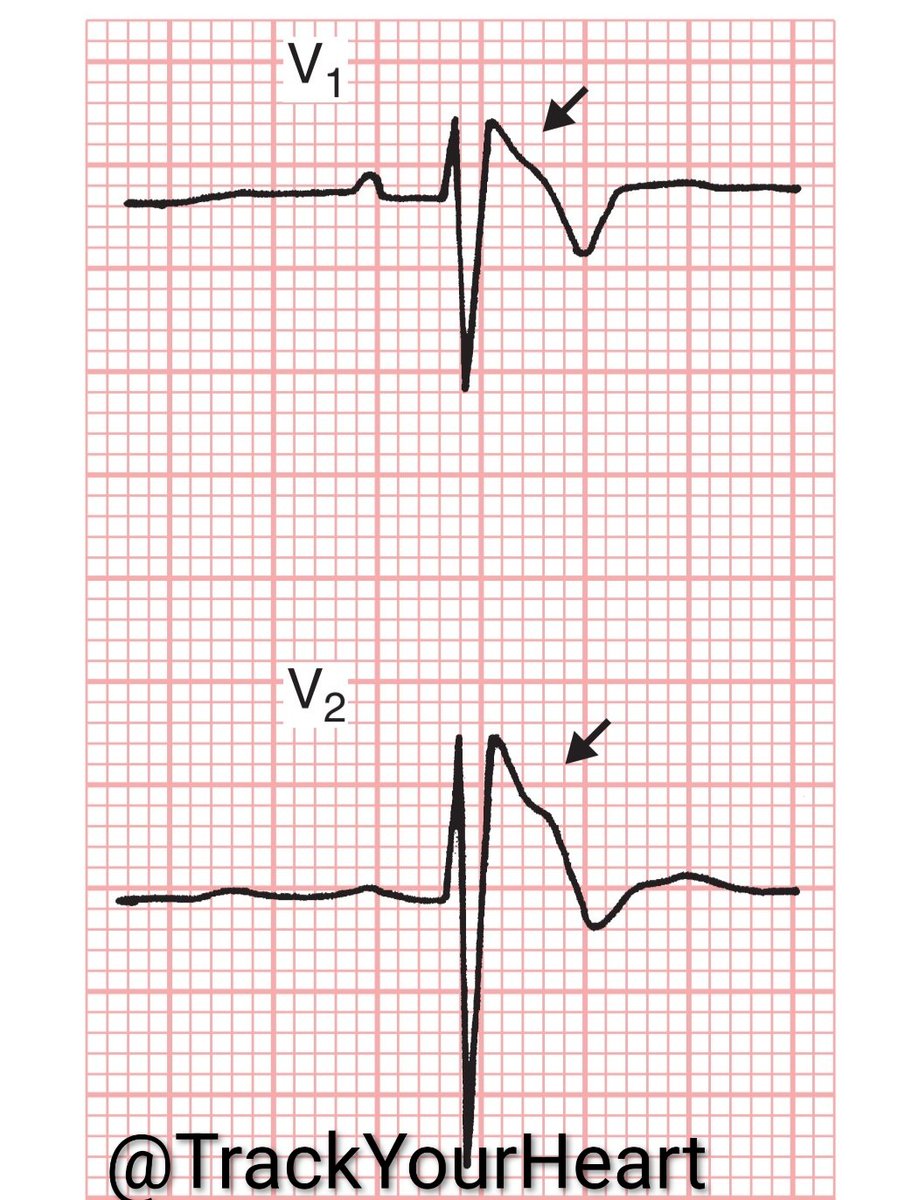
 2/
2/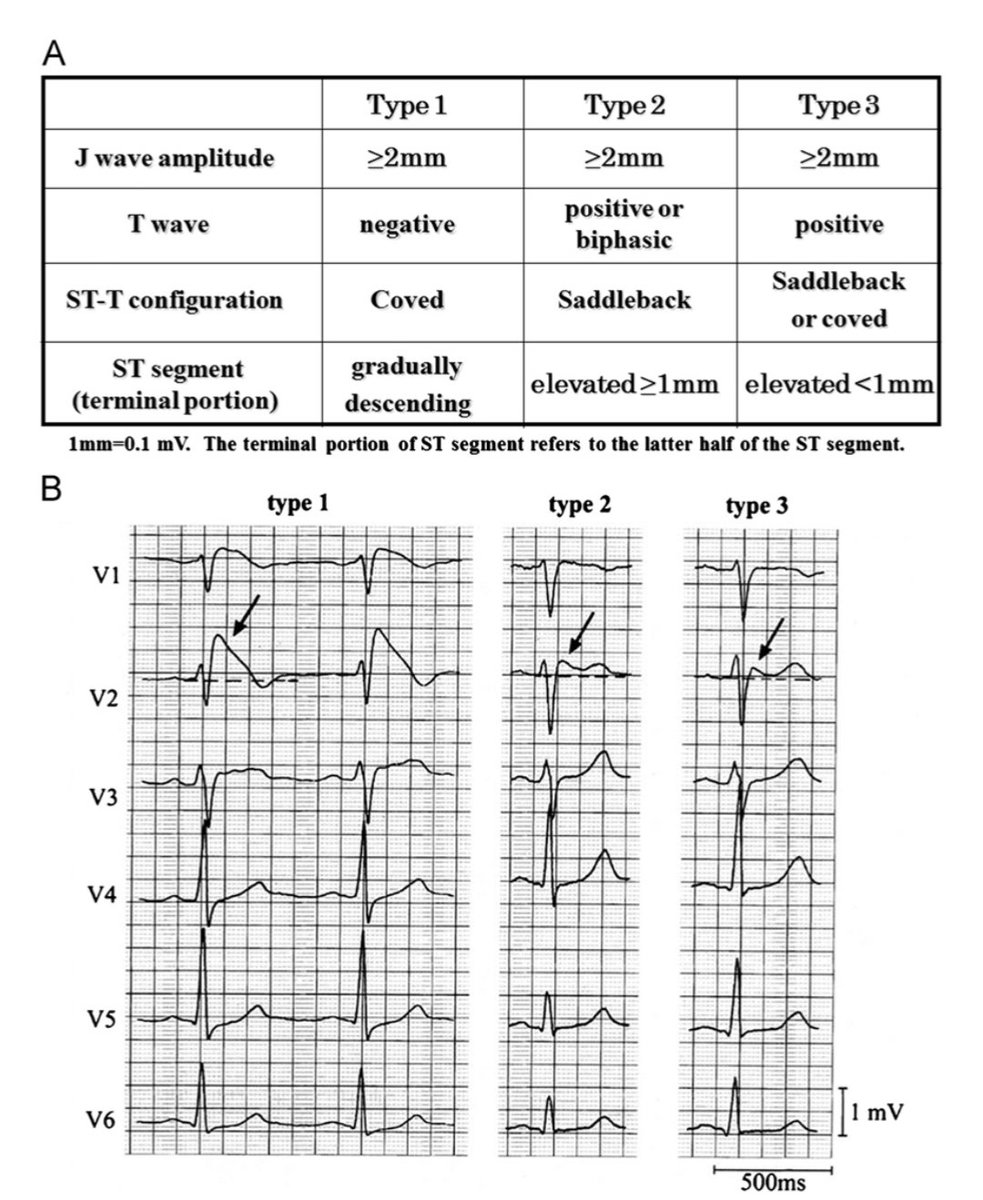
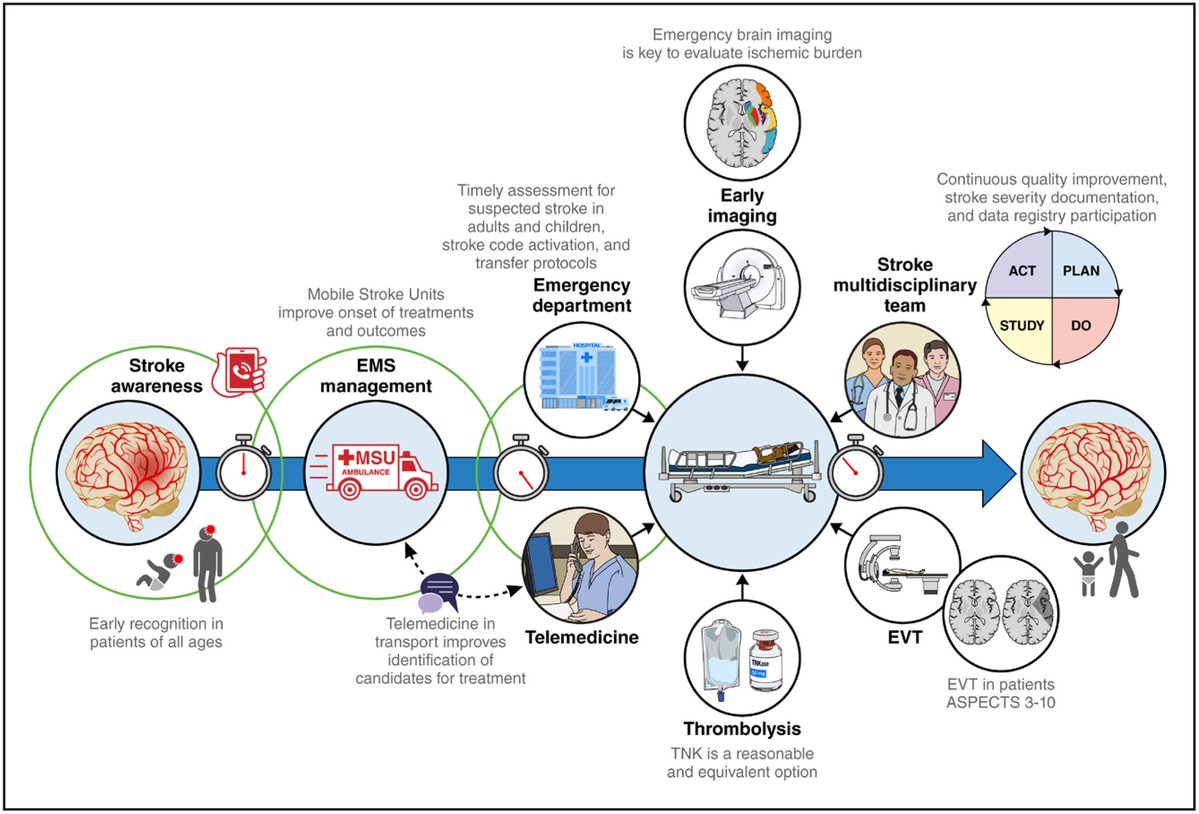
 1️⃣ Mobile Stroke Units (MSUs)
1️⃣ Mobile Stroke Units (MSUs)
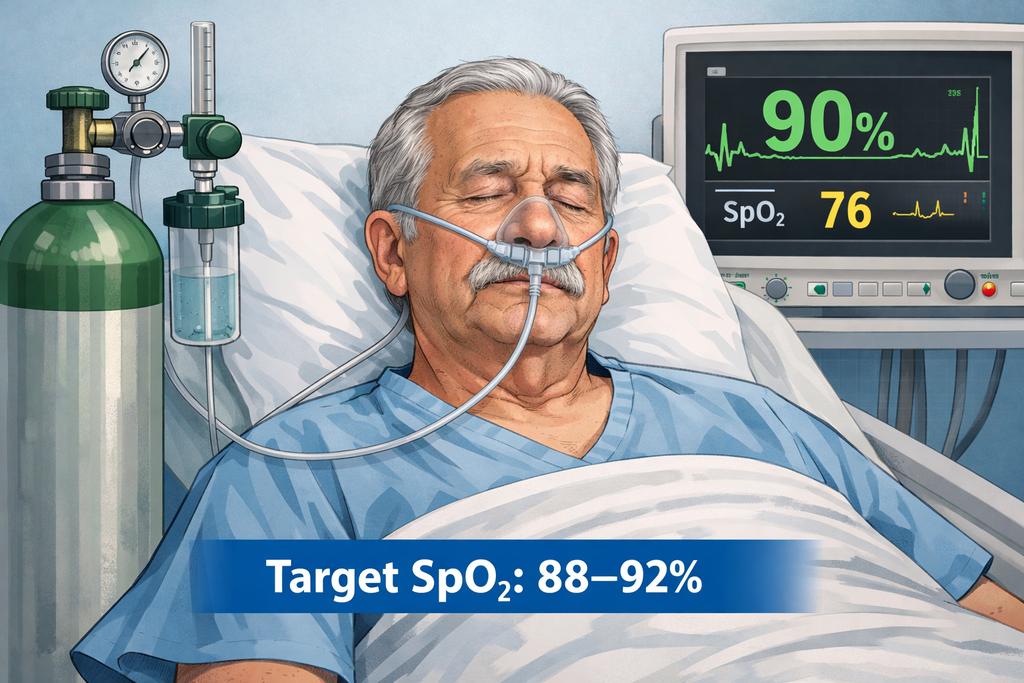
 Oxygen does NOT usually cause dangerous hypercapnia by stopping breathing.
Oxygen does NOT usually cause dangerous hypercapnia by stopping breathing.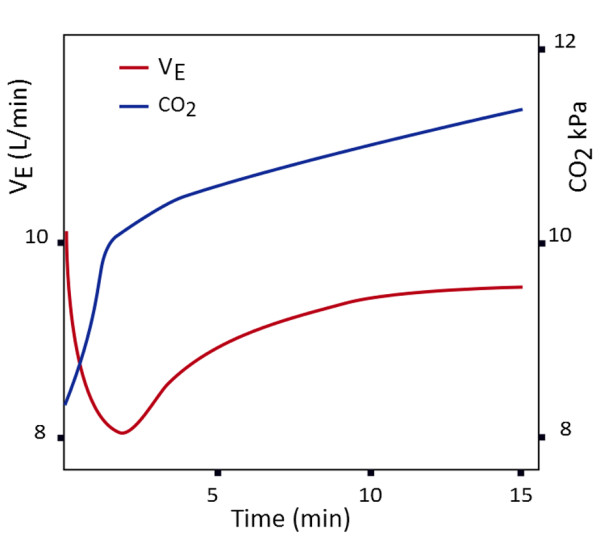
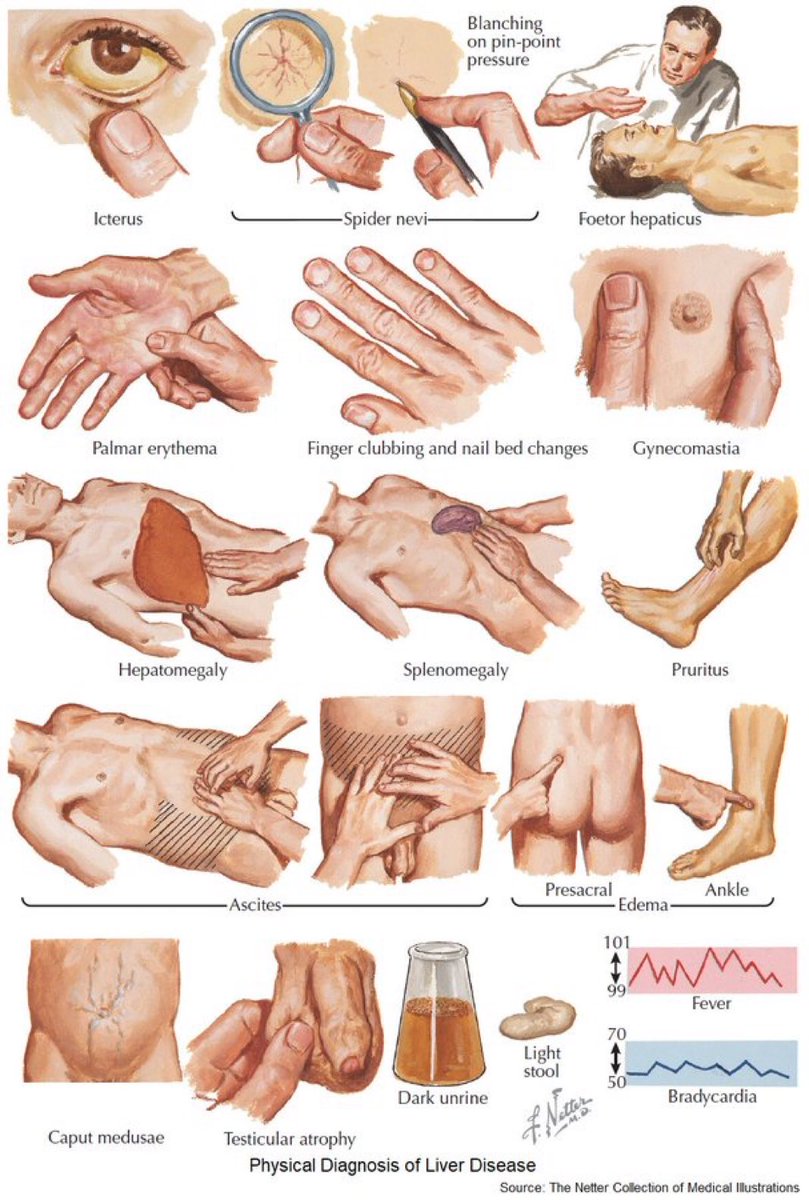
 🔵Icterus
🔵Icterus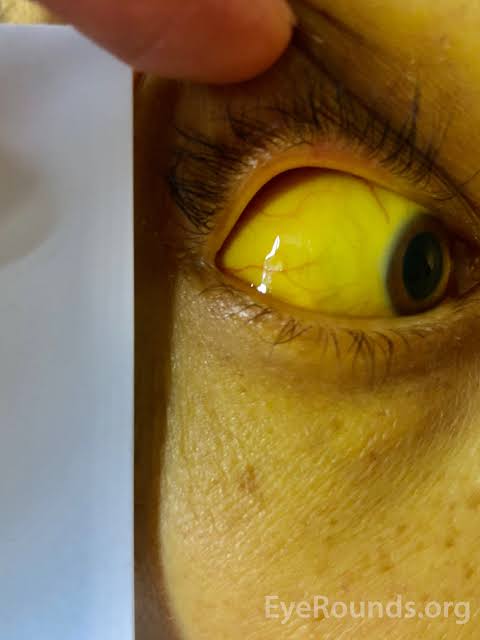
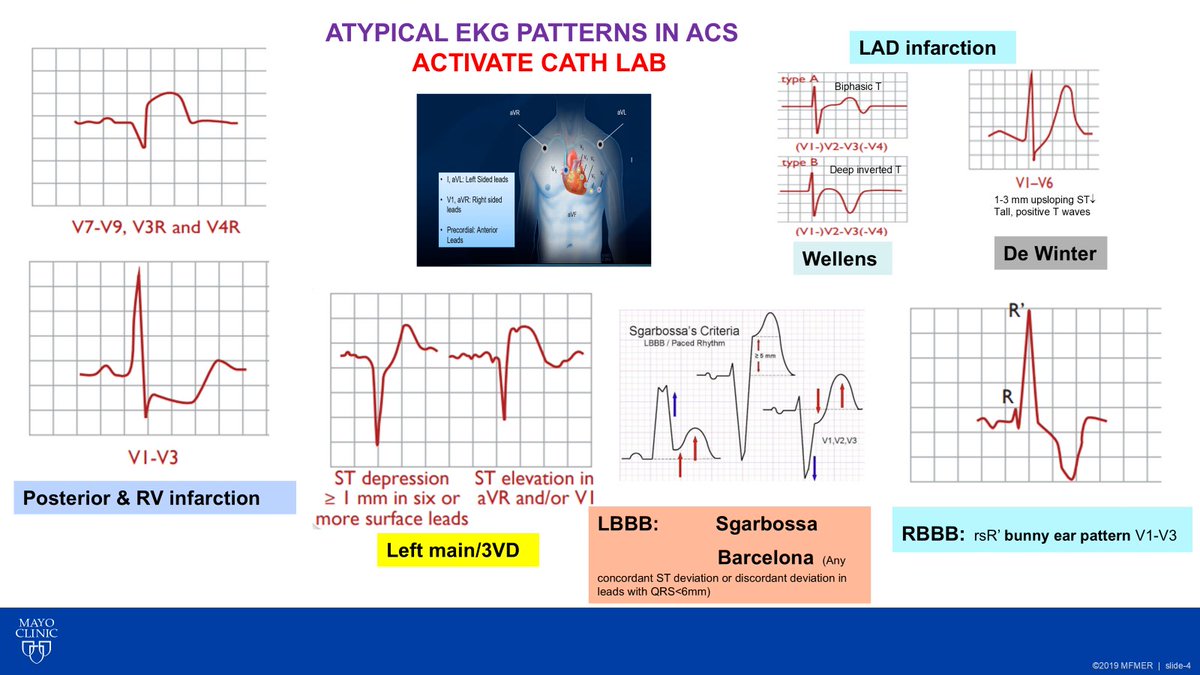
 🔵 Posterior MI & Right Ventricular MI
🔵 Posterior MI & Right Ventricular MI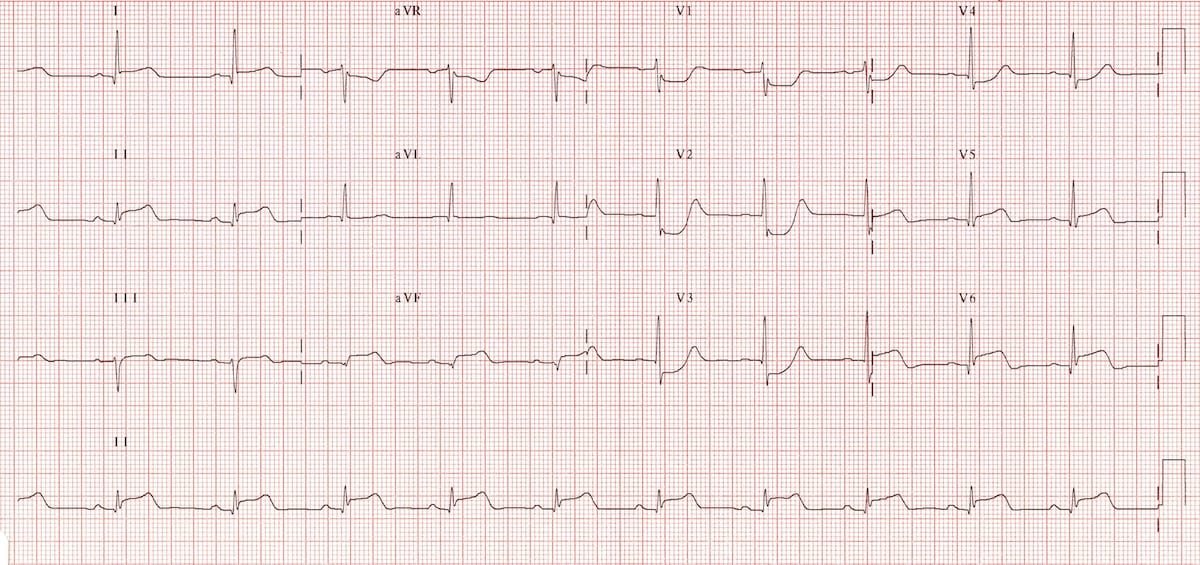

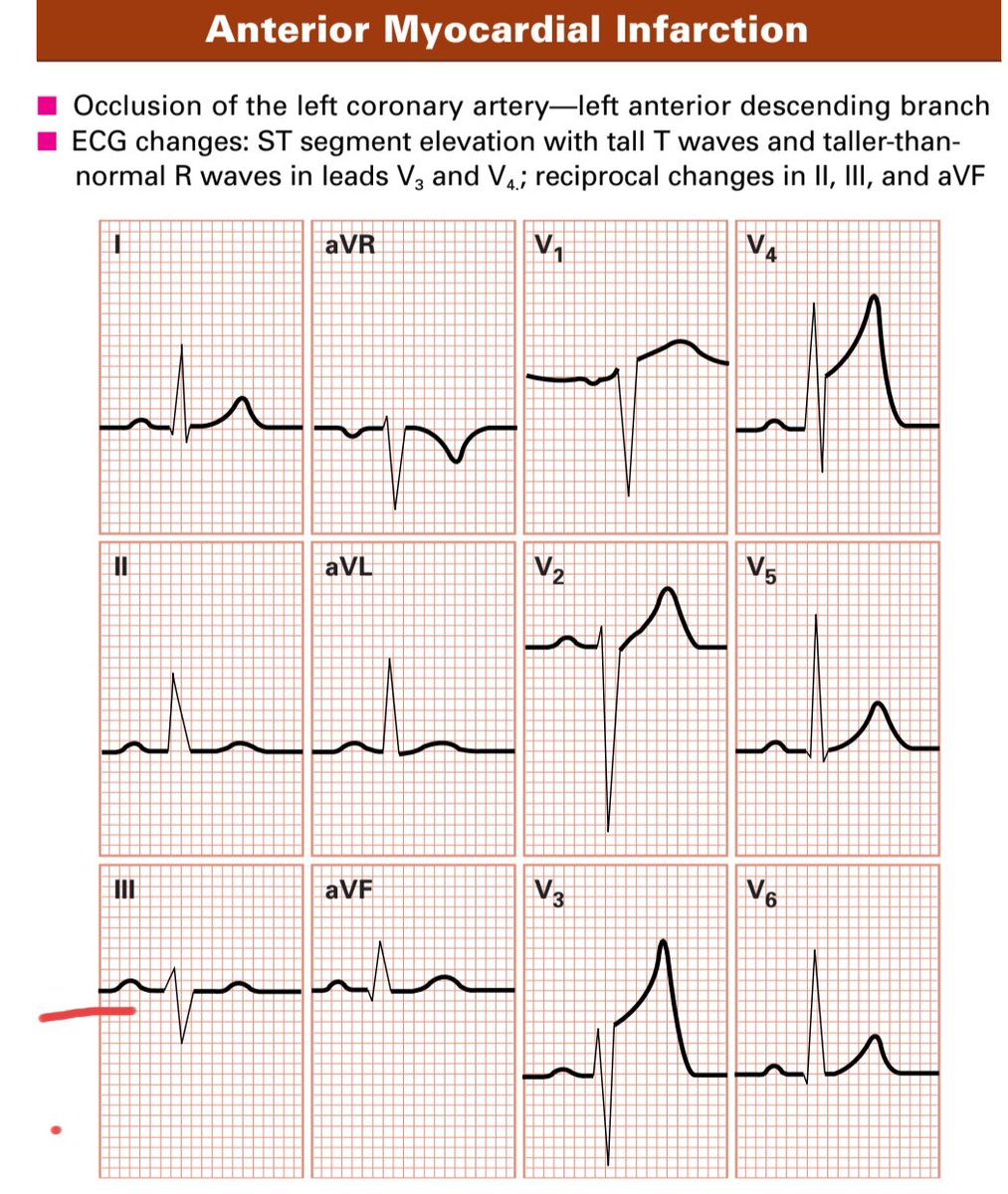

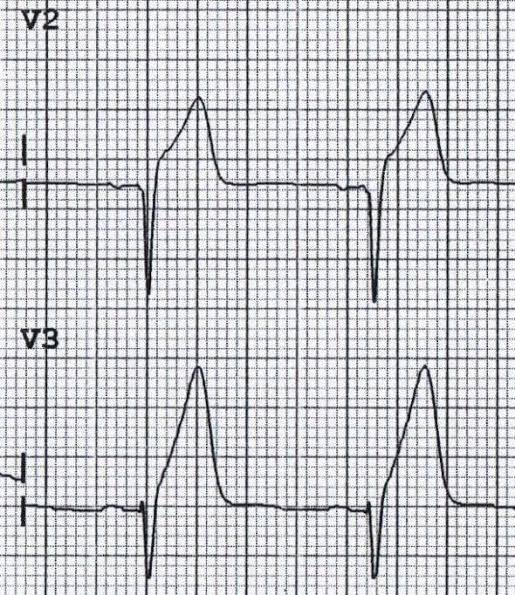
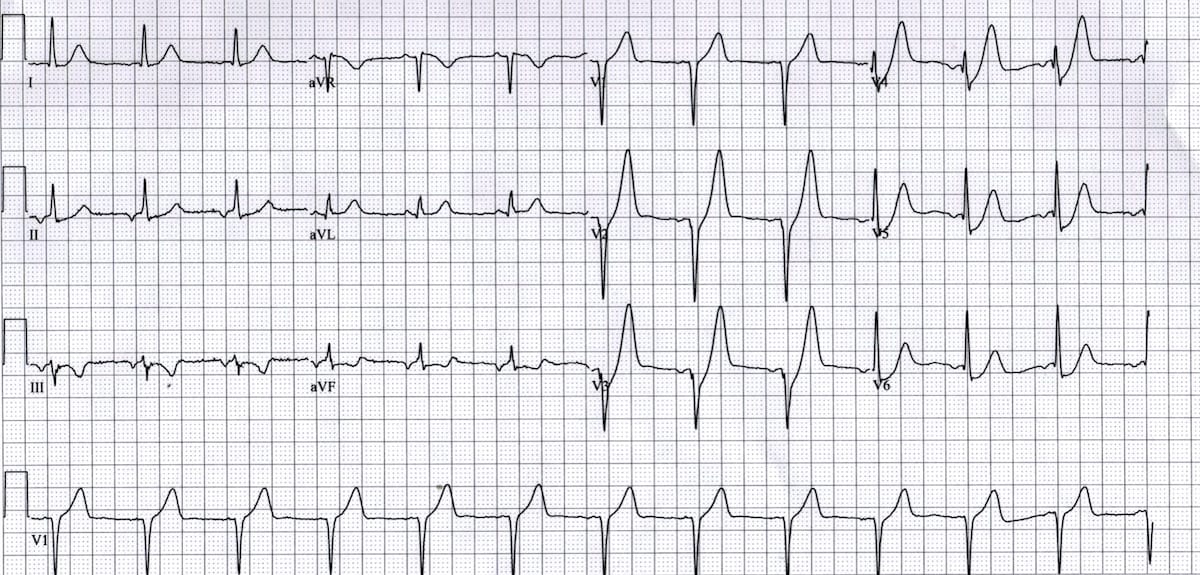
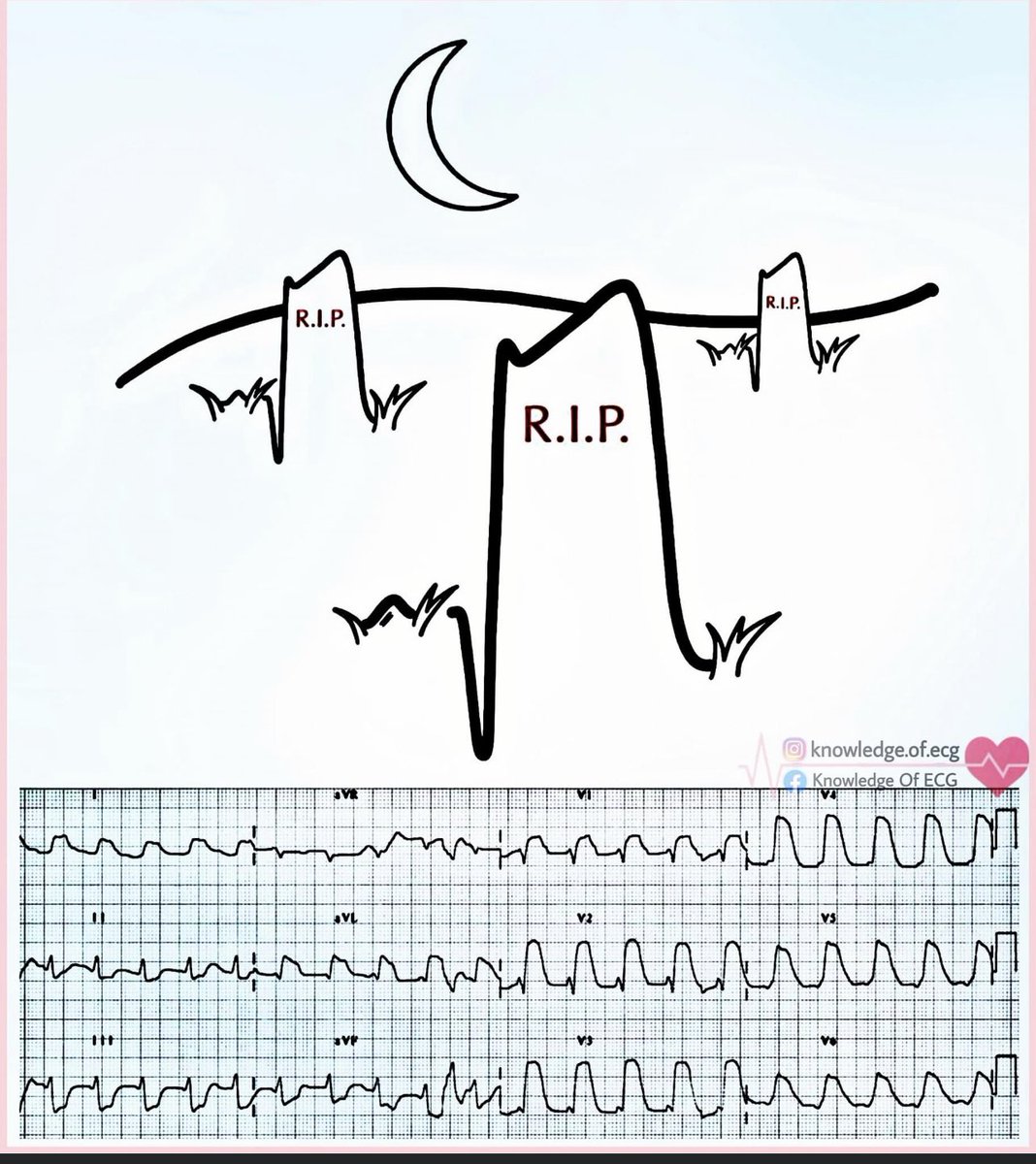
 1️⃣ Acute Coronary Occlusion (STEMI)
1️⃣ Acute Coronary Occlusion (STEMI)