
Clinic Director @westlondonphys | Knee pain | Back Pain | Thoughts on health, pain, and injury.
How to get URL link on X (Twitter) App


 ⚠️ Why the 'Wear and Tear' Model Falls Short
⚠️ Why the 'Wear and Tear' Model Falls Short 
 🔬 Phase 1 (0–6 weeks): The Graft Is Dying Off
🔬 Phase 1 (0–6 weeks): The Graft Is Dying Off
 There was once a doctor with a keen apprentice. The apprentice had studied for years but was now impatient. He felt ready to treat patients on his own.
There was once a doctor with a keen apprentice. The apprentice had studied for years but was now impatient. He felt ready to treat patients on his own. 
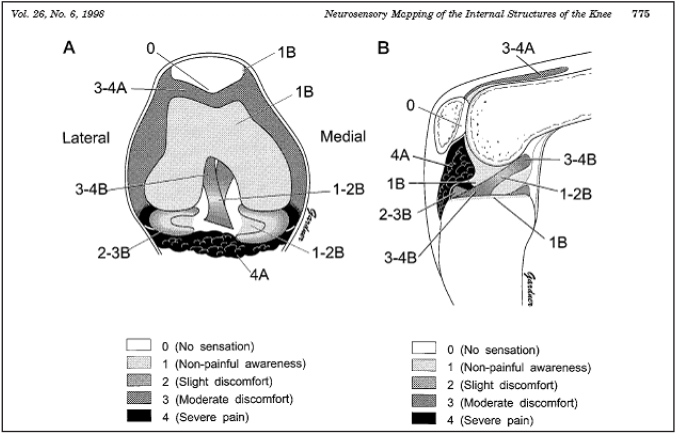
 From his previous work with patients he had observed:
From his previous work with patients he had observed: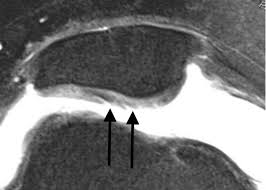
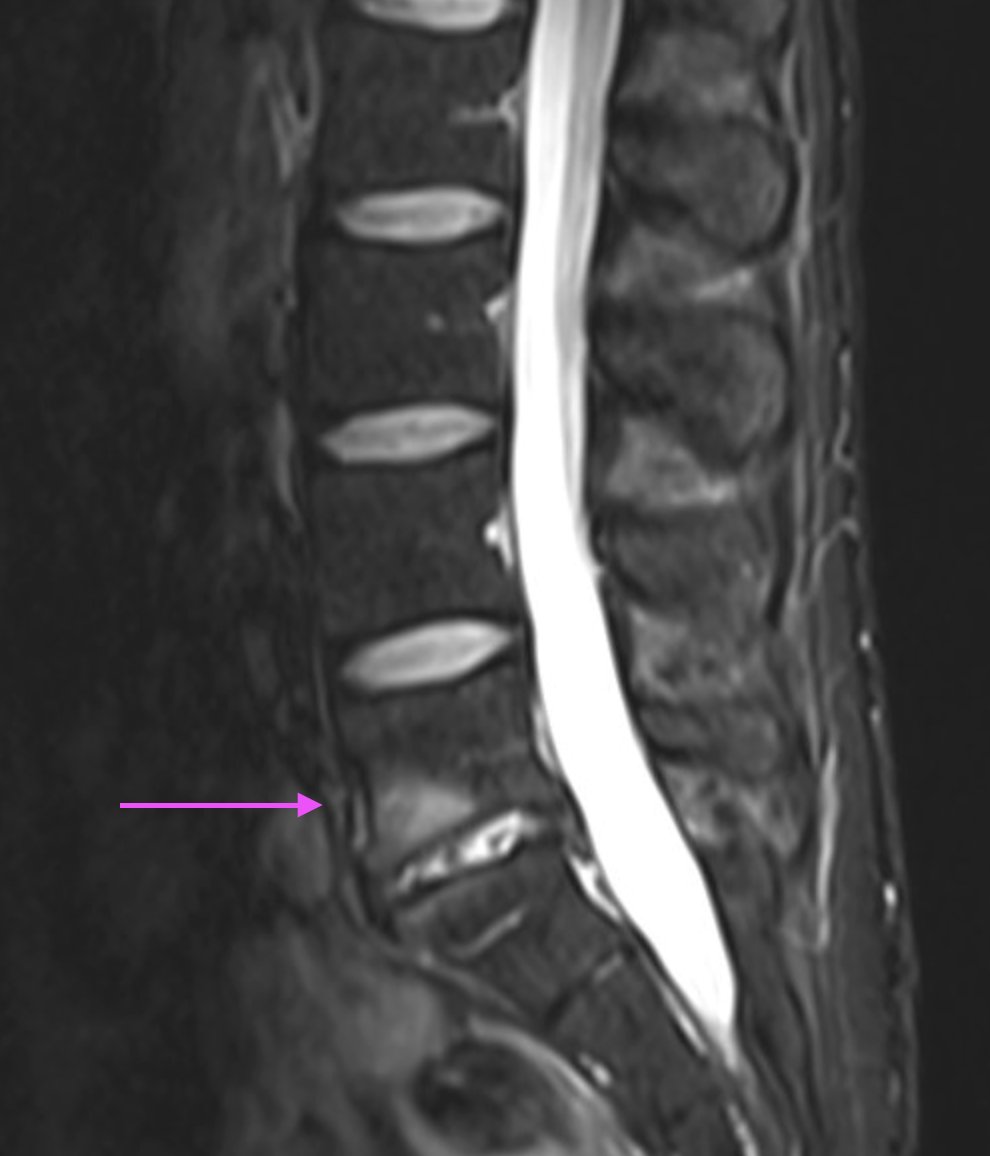
 Why are they called Modic changes? 🧐
Why are they called Modic changes? 🧐
 1. Consciously ‘contracting your core’ before movement is not how we work. Subconscious postural reflexes occur in anticipation of external force or movement. We can't consciously recruit with correct timing or force. To attempt to do so can cause more problems than it solves. 2/
1. Consciously ‘contracting your core’ before movement is not how we work. Subconscious postural reflexes occur in anticipation of external force or movement. We can't consciously recruit with correct timing or force. To attempt to do so can cause more problems than it solves. 2/
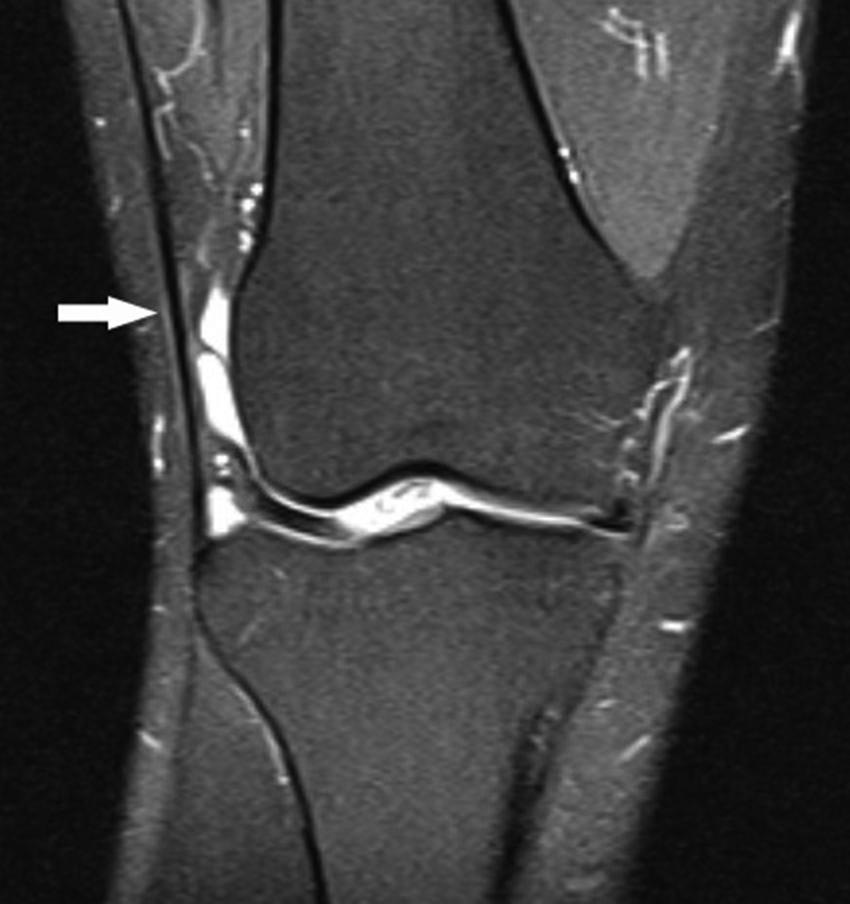
 Subjective: Pain sitting, Unable to 🚴♀️, Relief with🚶.
Subjective: Pain sitting, Unable to 🚴♀️, Relief with🚶.
 They intuit we don't know the cause of their problem. It stifles discussion, reduces trust, and facilitates poor outcomes in an environment from which chronic pain can more readily arise. Clinicians can compound the problem with technical language and poor diagnostic labels 2/
They intuit we don't know the cause of their problem. It stifles discussion, reduces trust, and facilitates poor outcomes in an environment from which chronic pain can more readily arise. Clinicians can compound the problem with technical language and poor diagnostic labels 2/

 Ortho surgeon advised he had a “failing knee”. Wait listed for arthroplasty and told to try physio in the interim. Physio included; one in person consult, a sheet of exercises, advice to walk more, and 6 group exercise classes. 3/12 later, no better and resigned to a TKR. 2/
Ortho surgeon advised he had a “failing knee”. Wait listed for arthroplasty and told to try physio in the interim. Physio included; one in person consult, a sheet of exercises, advice to walk more, and 6 group exercise classes. 3/12 later, no better and resigned to a TKR. 2/