
Learn point-of-care ultrasound (POCUS) and become a clinician of the modern era: https://t.co/z62WHlXJRW
How to get URL link on X (Twitter) App


 In a study of dialysis patients with and without severe pulmonary edema, lung crackles on auscultation were only 9% sensitive, detecting 9 out of every 100 cases.
In a study of dialysis patients with and without severe pulmonary edema, lung crackles on auscultation were only 9% sensitive, detecting 9 out of every 100 cases.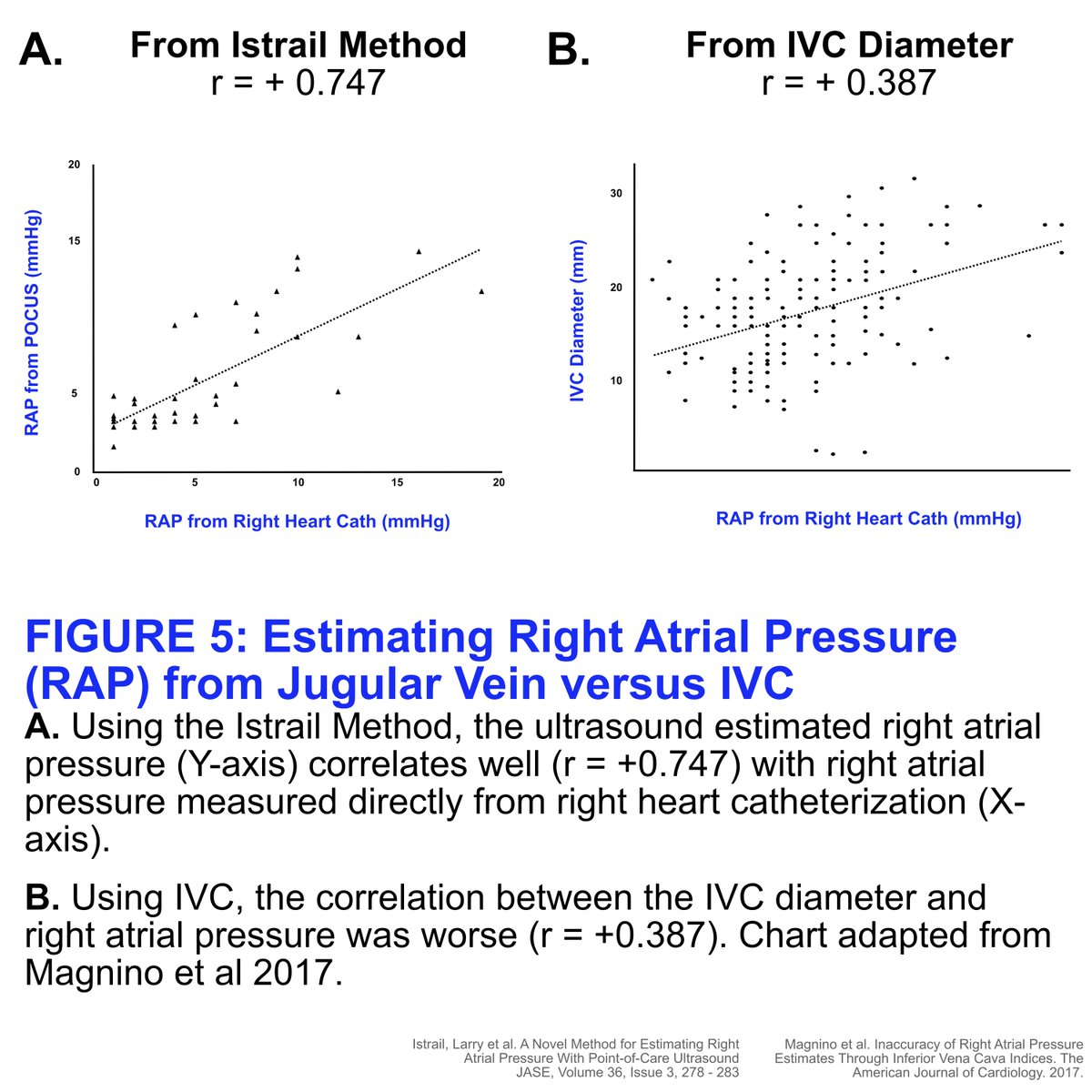




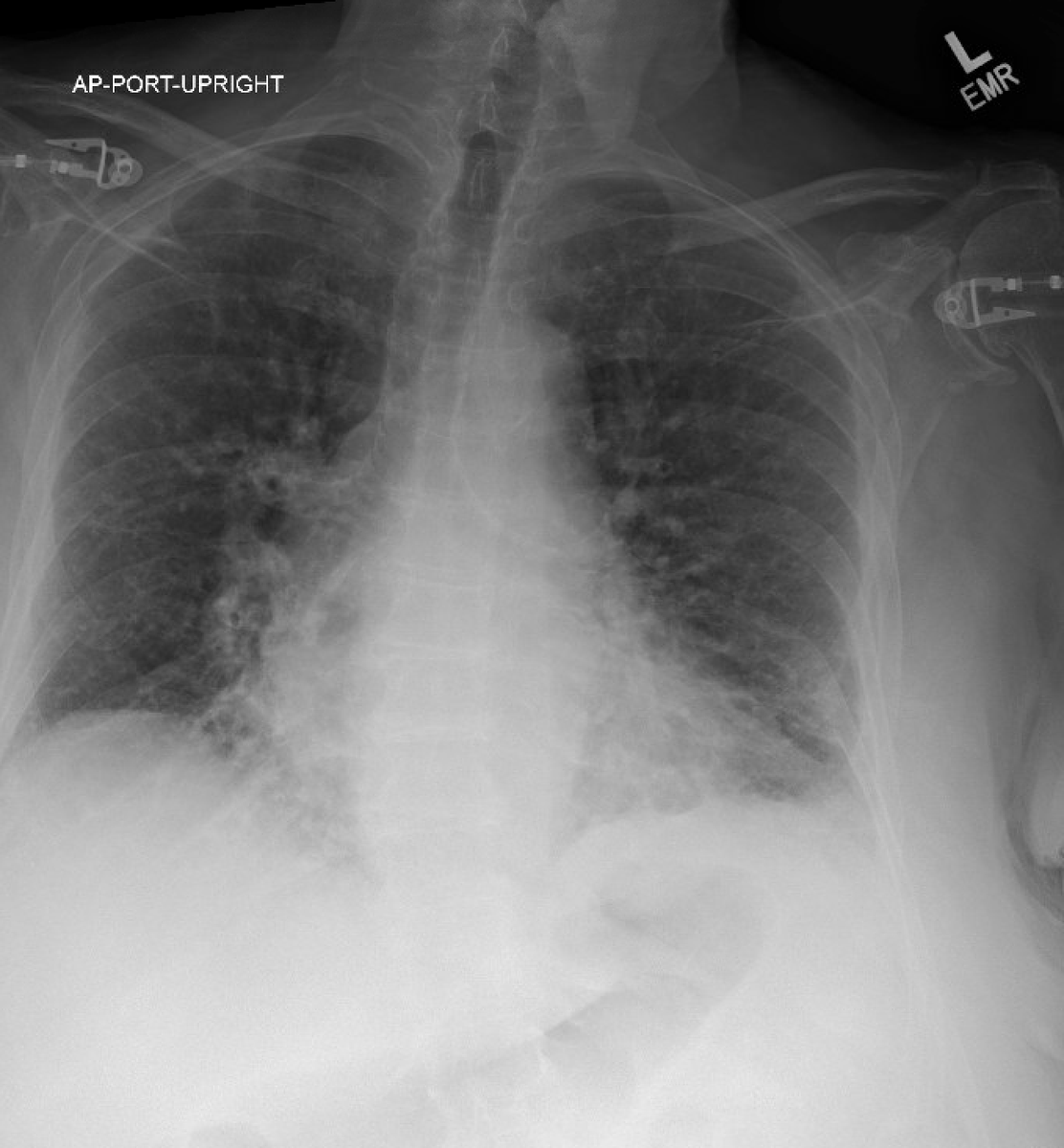
 Read as "Bibasilar atelectasis." She was started on antibiotics. The following morning had abdominal pain and CT chest abdomen and pelvis ordered. CT chest seen here:
Read as "Bibasilar atelectasis." She was started on antibiotics. The following morning had abdominal pain and CT chest abdomen and pelvis ordered. CT chest seen here:



 He knew that in heart failure there in “congestion of the veins” and when they become engorged can be detected on the neck.
He knew that in heart failure there in “congestion of the veins” and when they become engorged can be detected on the neck.