We provide psychiatry education for Psychiatrists, GPs & Mental Health Practitioners. • Join The Academy 👇
How to get URL link on X (Twitter) App

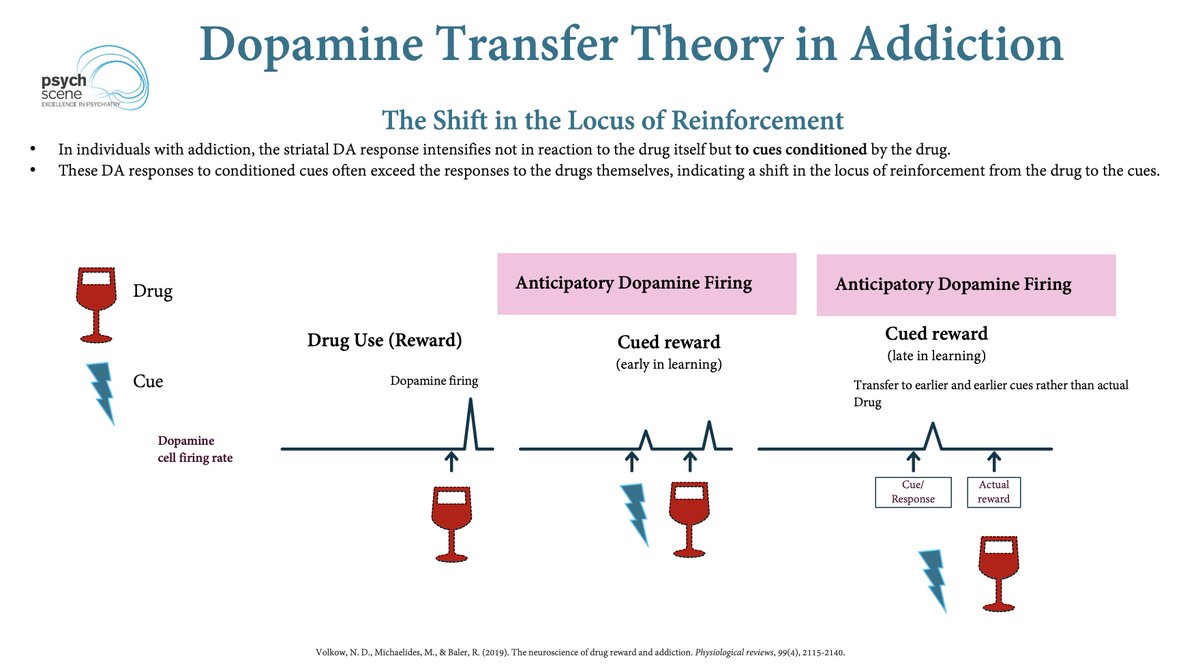
 To understand why, start with what repeated drug use teaches the brain.
To understand why, start with what repeated drug use teaches the brain.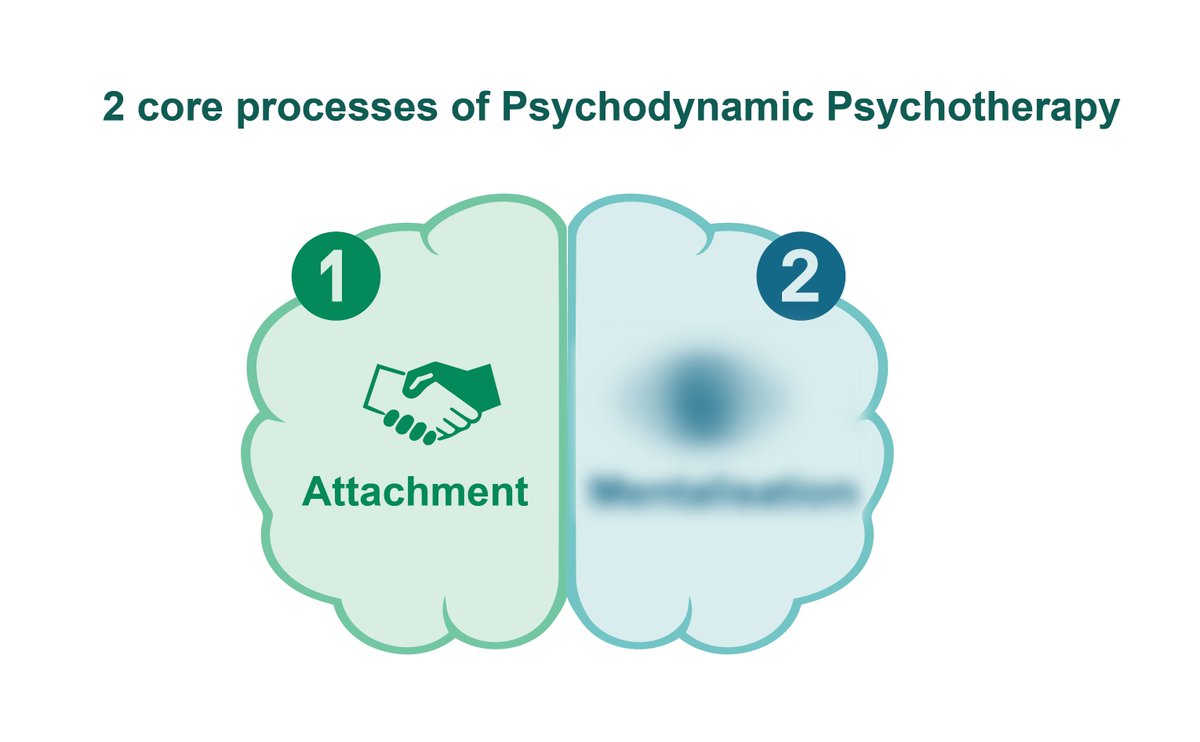
 1/ Attachment
1/ Attachment
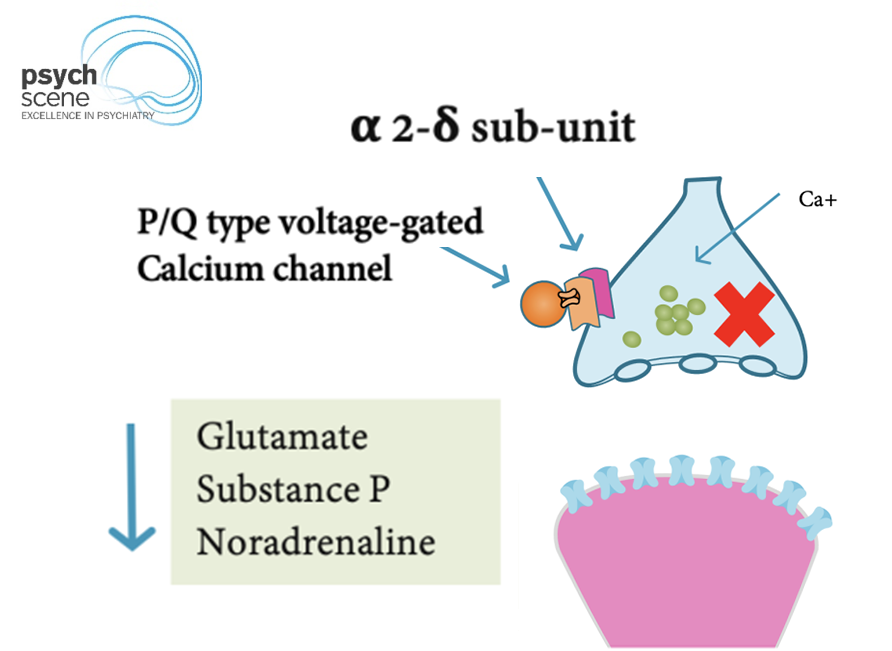
 Despite their structural similarity to GABA, gabapentin and pregabalin do not bind to GABA-A or GABA-B receptors.
Despite their structural similarity to GABA, gabapentin and pregabalin do not bind to GABA-A or GABA-B receptors.
 Let’s start with the definition.
Let’s start with the definition.
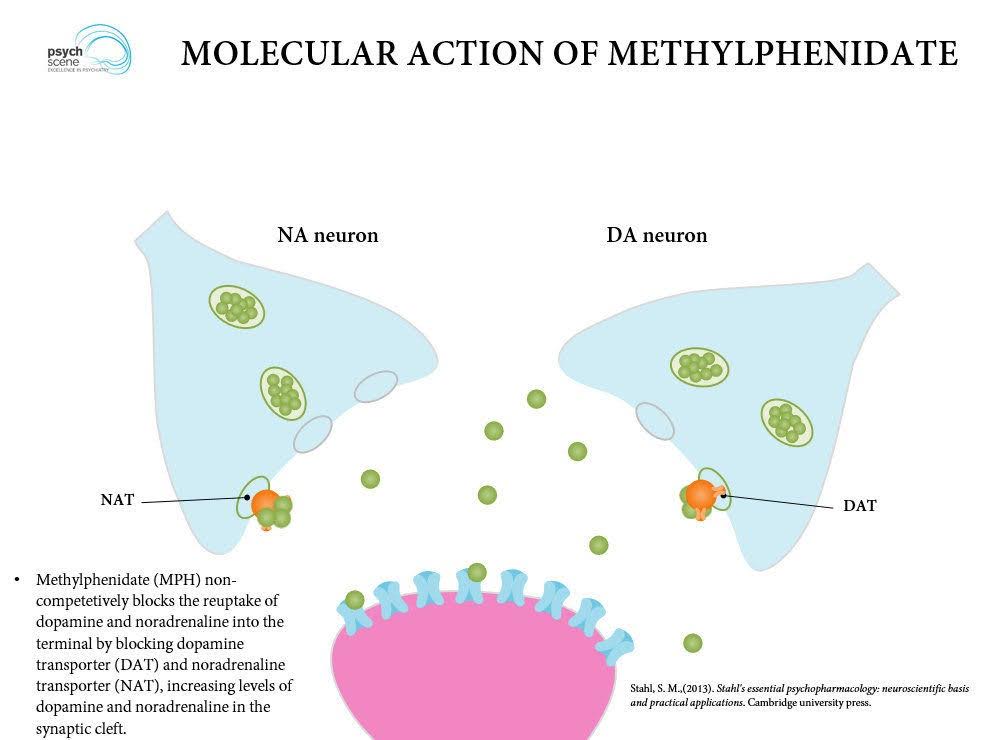
 Methylphenidate blocks the reuptake of:
Methylphenidate blocks the reuptake of: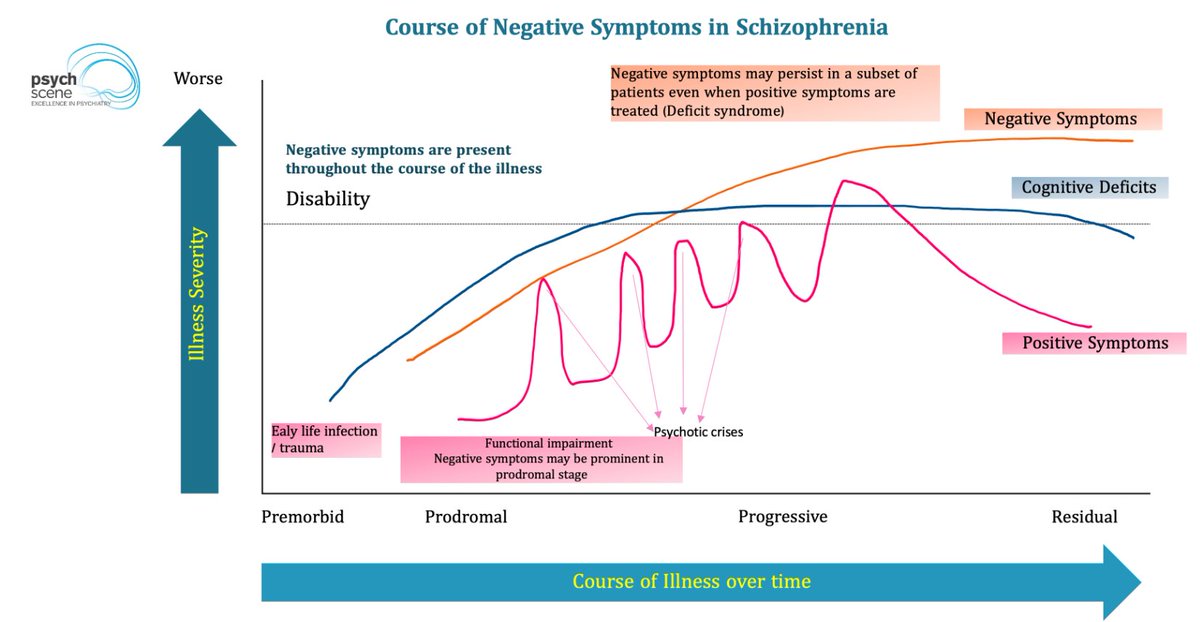
 This is the recovery gap in schizophrenia.
This is the recovery gap in schizophrenia.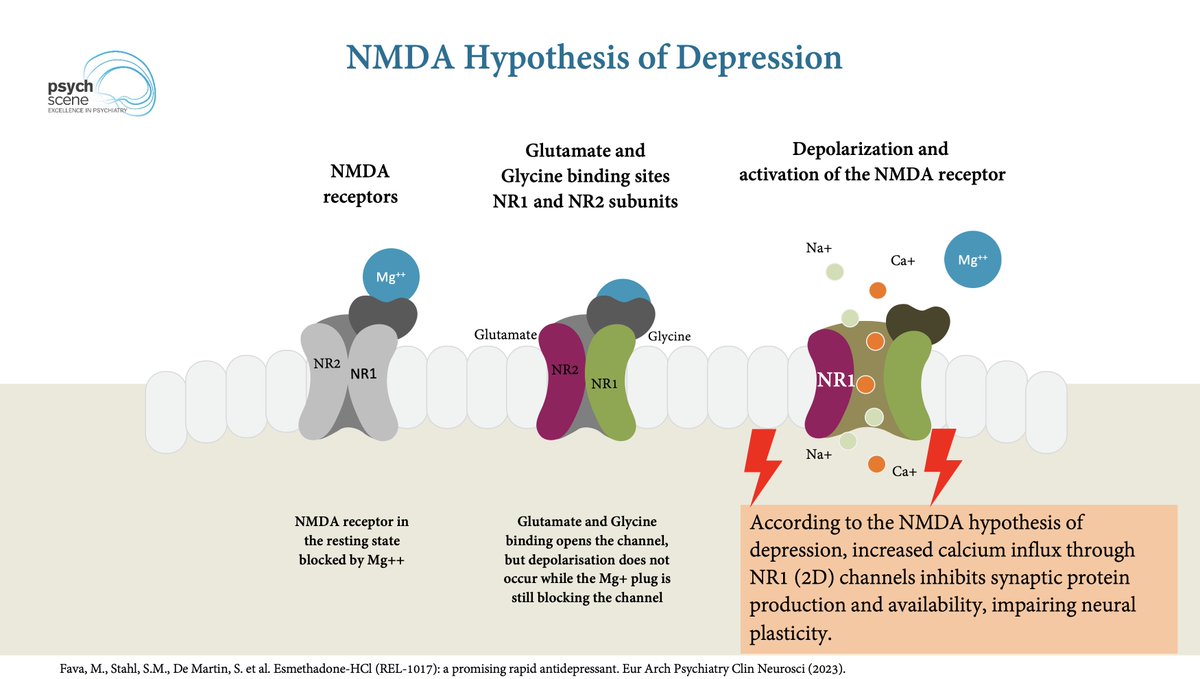
 For decades, antidepressants have largely targeted monoamine systems:
For decades, antidepressants have largely targeted monoamine systems:
 Both medications can be useful in ADHD when stimulants are:
Both medications can be useful in ADHD when stimulants are:
 This is where the Tripartite Model of Fronto-Striato-Limbic Circuits becomes useful.
This is where the Tripartite Model of Fronto-Striato-Limbic Circuits becomes useful.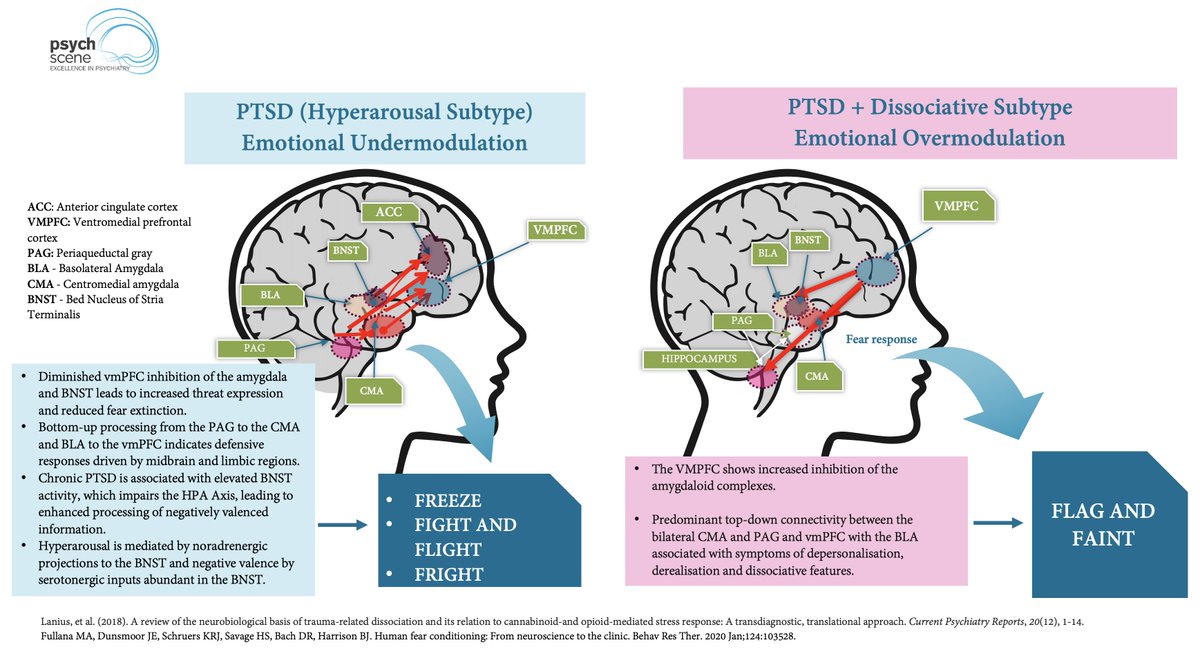
 Around 13–30% of individuals with PTSD meet criteria for the dissociative subtype.
Around 13–30% of individuals with PTSD meet criteria for the dissociative subtype.
 The dorsal striatum is not just a motor structure.
The dorsal striatum is not just a motor structure.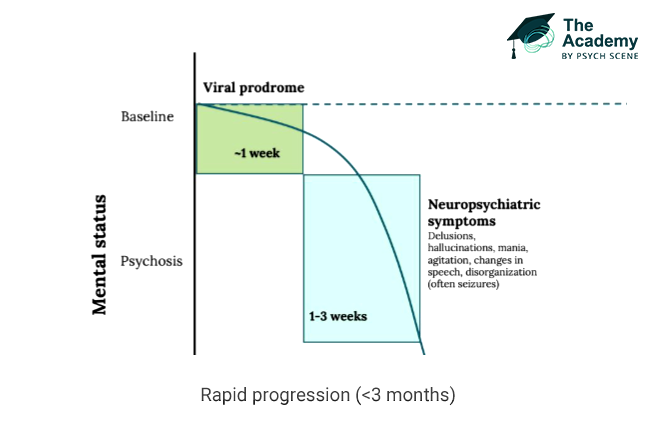
 AE diagnosis can be considered when all three of the following criteria are met.
AE diagnosis can be considered when all three of the following criteria are met.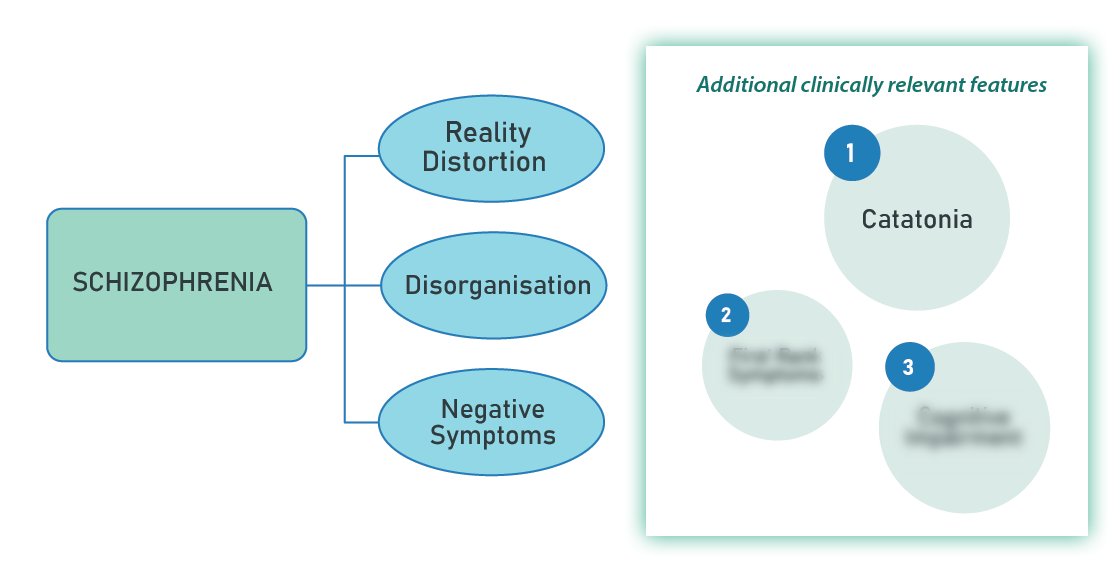
 1/ Catatonia
1/ Catatonia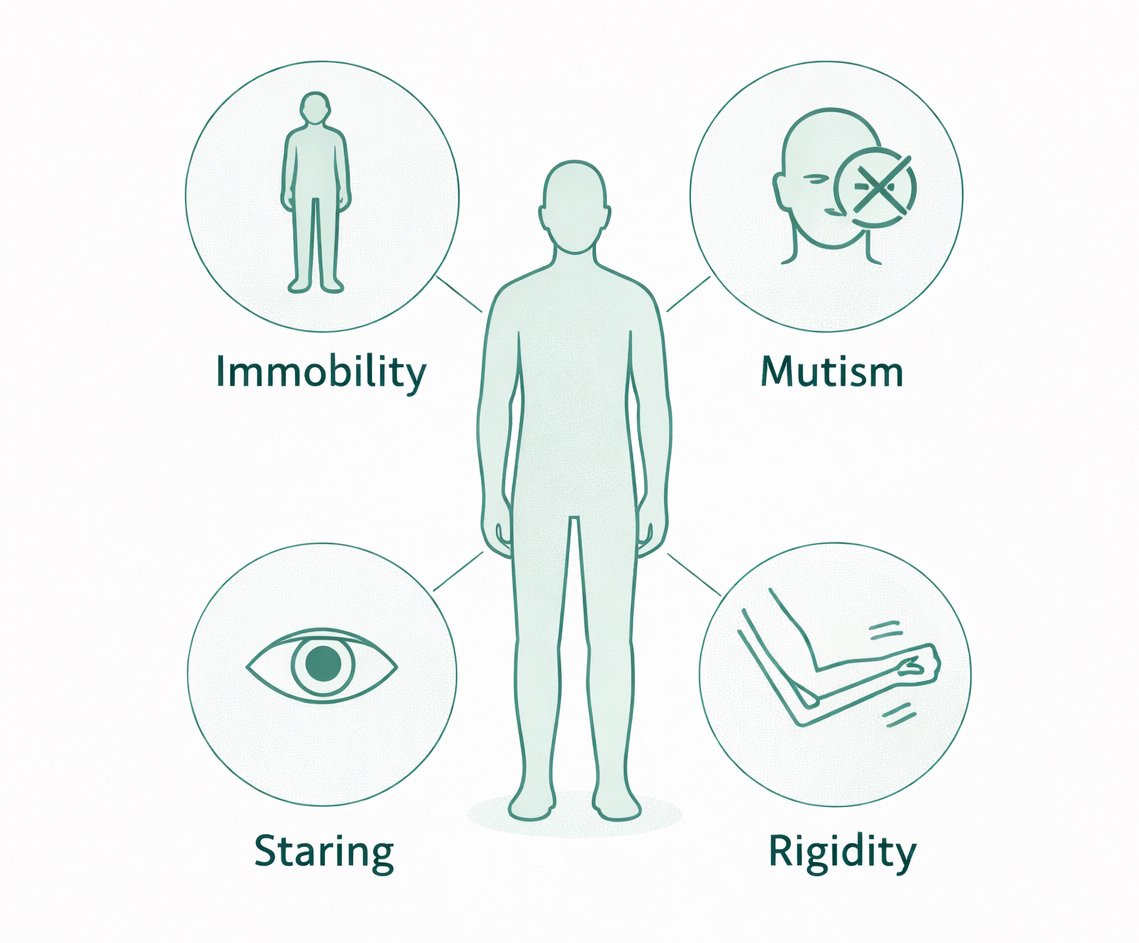
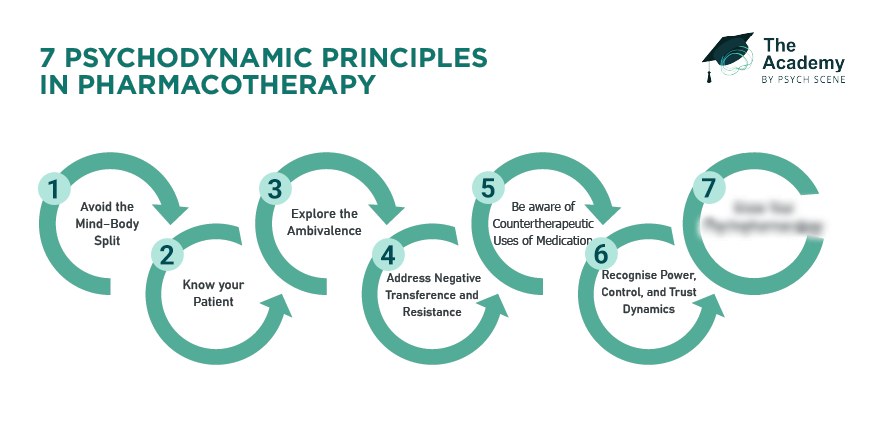
 1/ Avoid the Mind–Body Split
1/ Avoid the Mind–Body Split

 1/ Reward & Motivation
1/ Reward & Motivation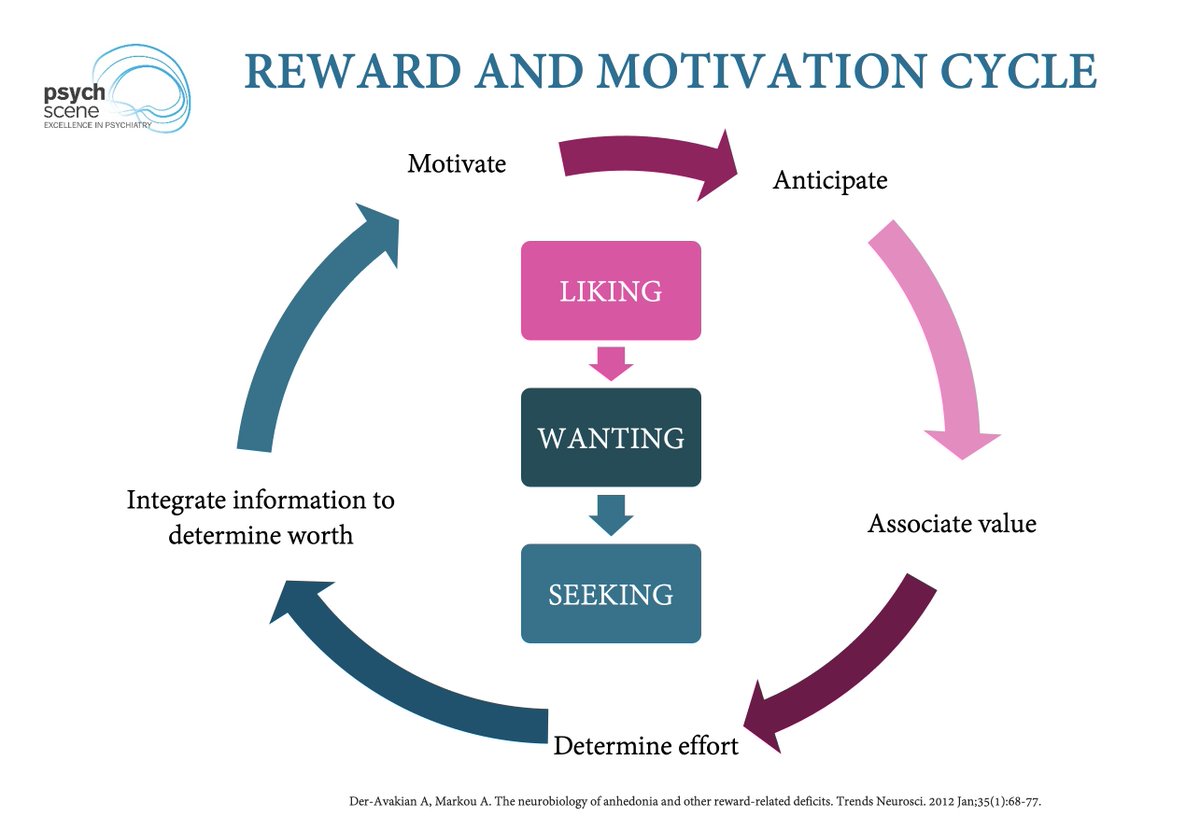

 The Intrinsic Receptor Deficit
The Intrinsic Receptor Deficit
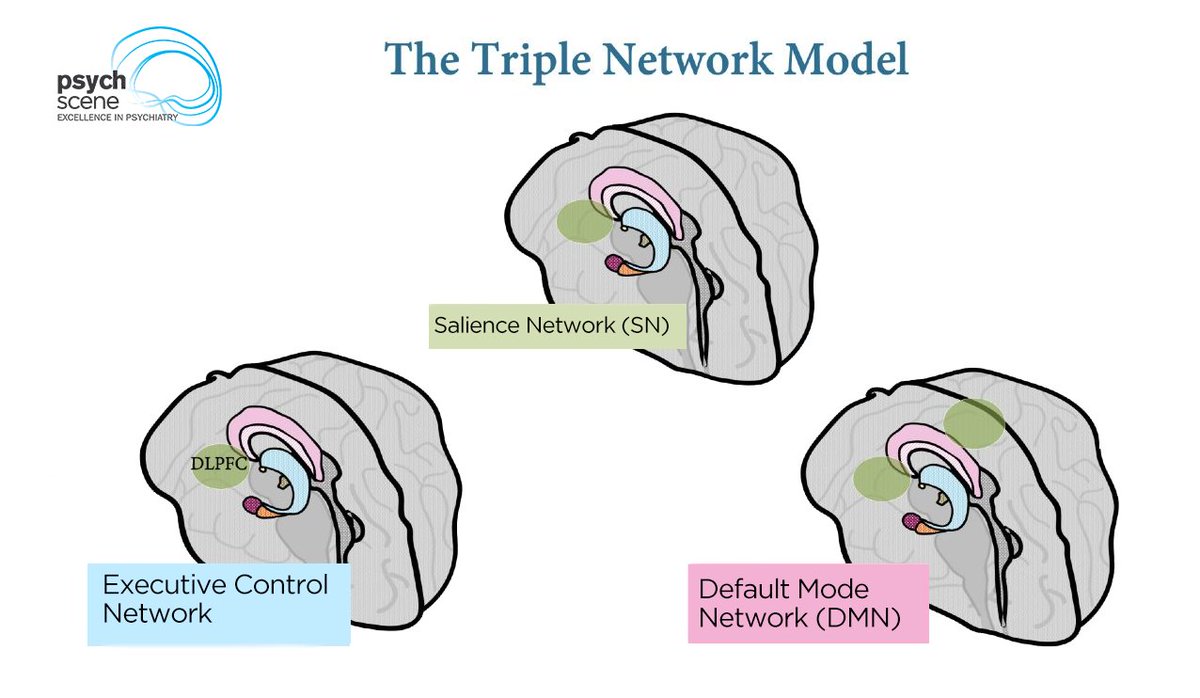
 The Triple Network Model frames depression as dysregulation within and between three major functional brain systems.
The Triple Network Model frames depression as dysregulation within and between three major functional brain systems.
 PTSD develops through a combination of psychological and biological mechanisms.
PTSD develops through a combination of psychological and biological mechanisms.
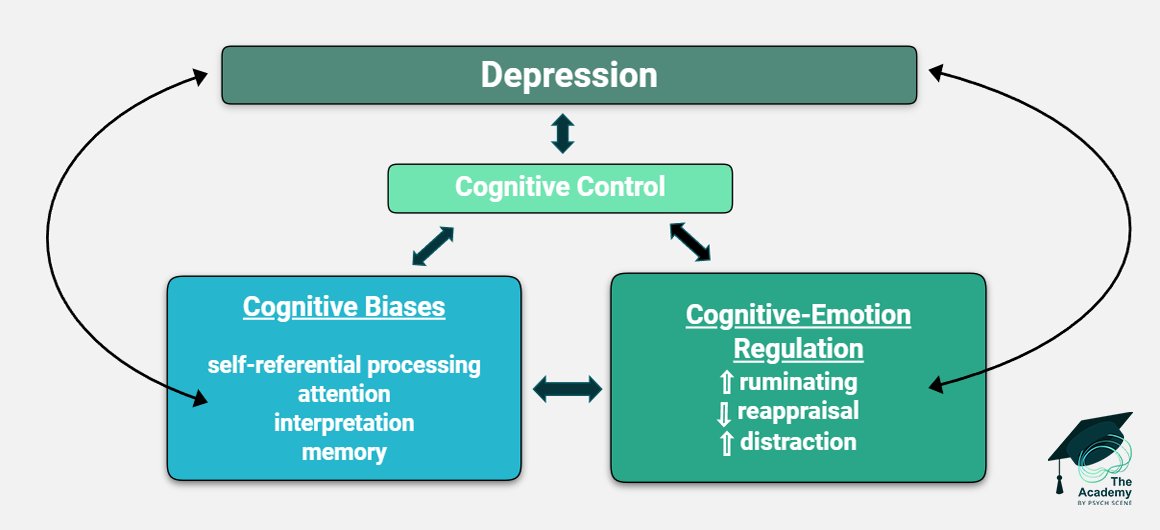
 Cognition has long been recognised as part of MDD, with impairments in areas such as attention, working memory, and processing speed already linked to poorer function and poorer treatment outcomes.
Cognition has long been recognised as part of MDD, with impairments in areas such as attention, working memory, and processing speed already linked to poorer function and poorer treatment outcomes.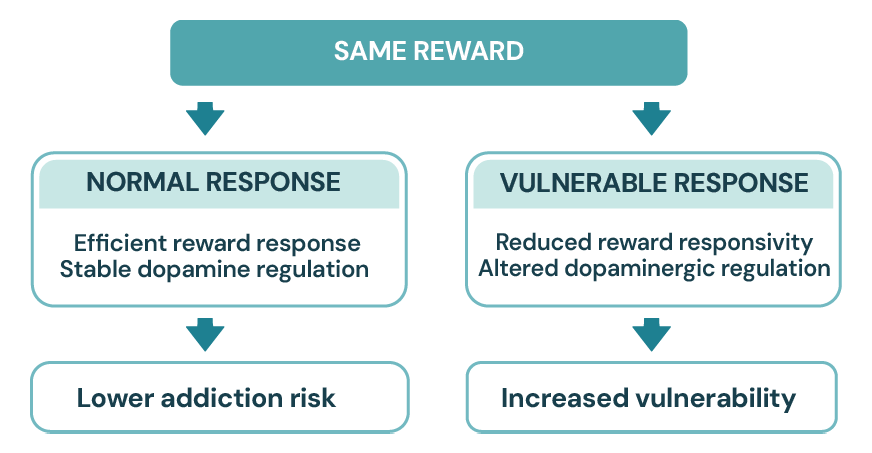
 The Polygenic Architecture of Vulnerability
The Polygenic Architecture of Vulnerability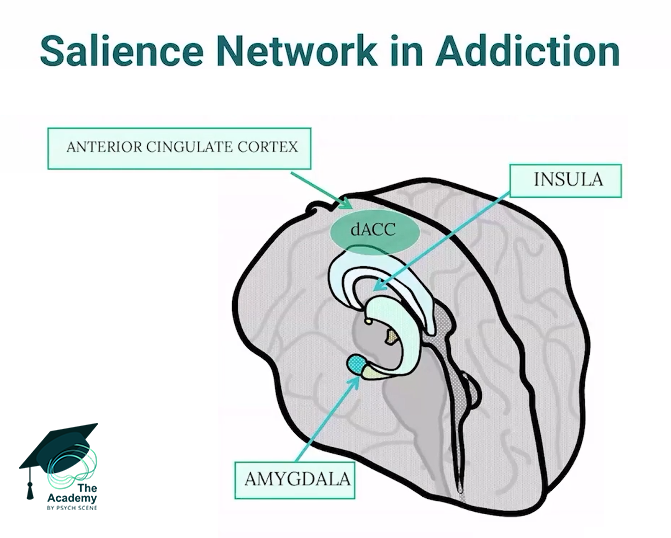

 Stage 0: Trauma Exposed & Asymptomatic
Stage 0: Trauma Exposed & Asymptomatic