
AI applied to cardiometabolic prevention & multimodality cardiovascular imaging; Posts may be my opinions & are not medical advice; RT≠endorse
How to get URL link on X (Twitter) App

https://twitter.com/venkmurthy/status/1610333094619549696A baseball will deposit that energy in a smaller surface area than a human head generally will. The concentration of that energy is required because if parts of it are not over the heart they won't cause a cardiac problem
https://twitter.com/jeremyfaust/status/1408948777675890691Why is this a bad take:





https://twitter.com/DrAMcCullough/status/1304436564223762432First, the pericardial effusions do not seem to be clearly more than physiologic.
https://twitter.com/mugander/status/1302143741369618432?s=19
https://twitter.com/ProfDFrancis/status/1299988378147000320As @ADAlthousePhD points out baseline differences in RCTs really are not a thing to worry about.
https://twitter.com/ProfDFrancis/status/1294370975702822914TBH I'm not a football guy so whether they put off a year doesn't really affect me, but the Big 10 is a majorly respected organization and many Americans get their news from @espn.

 Authors' response:
Authors' response:
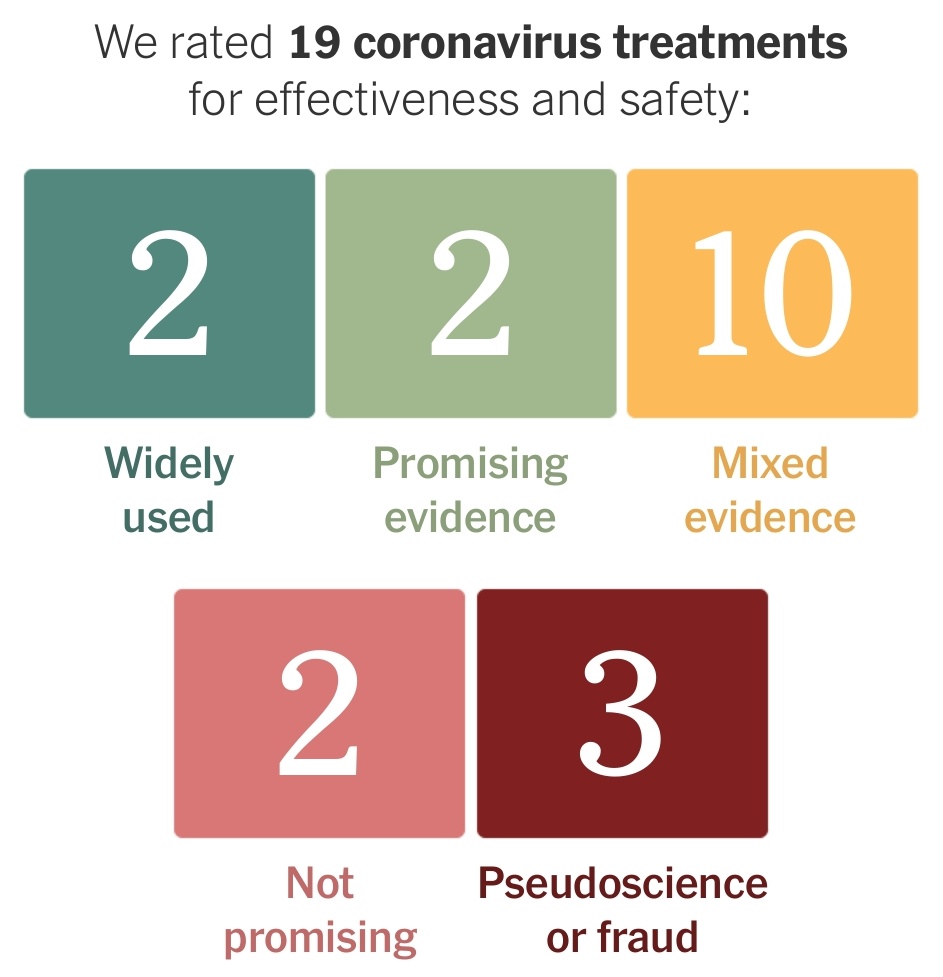
https://twitter.com/venkmurthy/status/1283864900603871232

 They have eliminated strong evidence category.
They have eliminated strong evidence category.https://twitter.com/ashishkjha/status/1277049395456823296We admit people with MI to the hospital who aren't in that high risk of dying because we have specific hospital based therapies (anticoagulation, angiography) that can reduce mortality and morbidity.