'Herd immunity' has been reached during previous epidemics of influenza, measles and seasonal coronaviruses. But it's subsequently been lost (and then regained). What are some of the reasons for this? 1/
Here we're using technical definition of 'herd immunity', i.e. sufficient immunity within a population to push R below 1 in absence of other control measures. But reaching this point doesn't mean R will stay below 1 forever. Here four things to be aware of... 2/
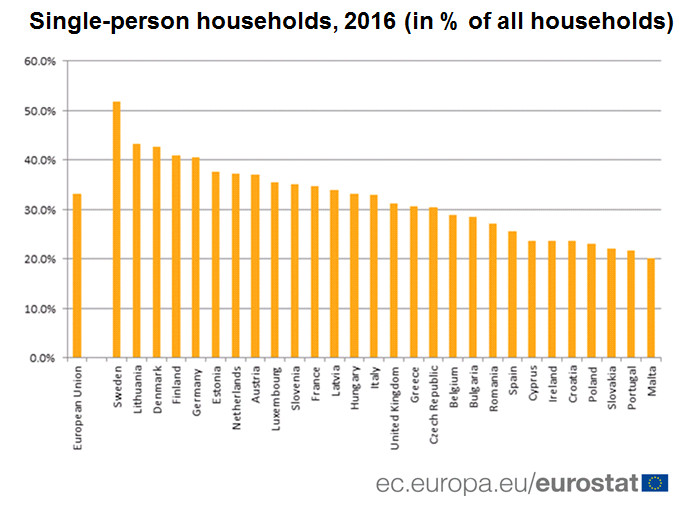
A: Population turnover. Over time, new births mean an increase in % of population susceptible. This will eventually lead to R>1 and new (but smaller) outbreaks - the more transmissible the infection, the sooner this recurrence will happen. More:
https://twitter.com/AdamJKucharski/status/1282975984338141185?s=203/
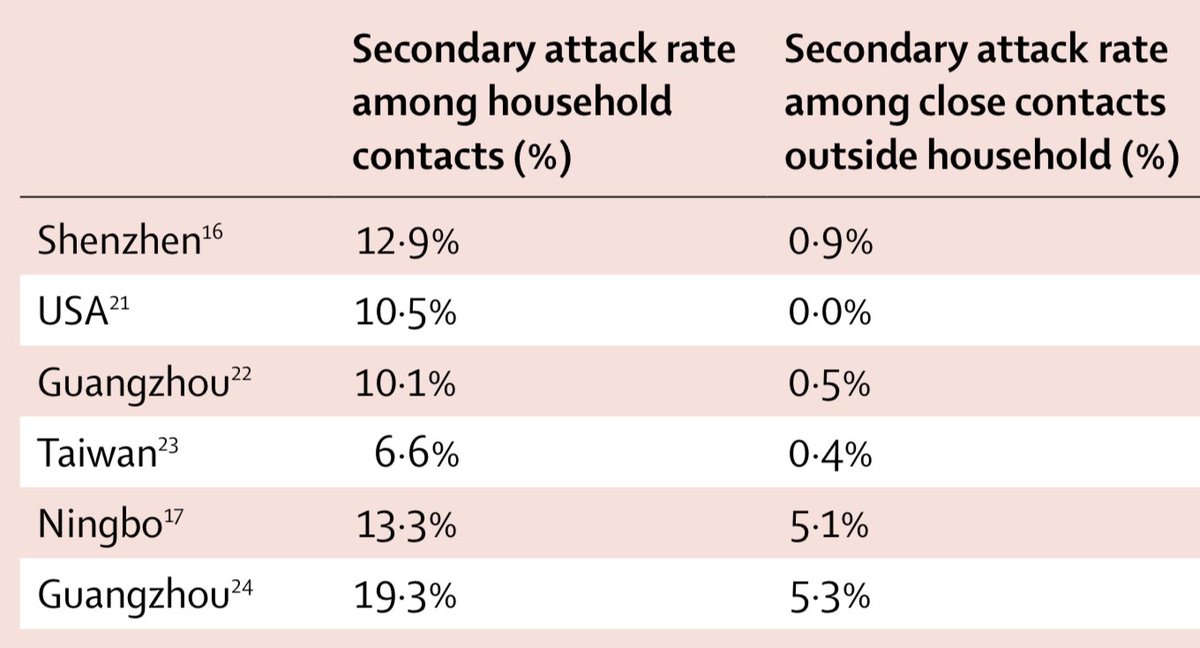
B: Waning. For seasonal coronaviruses, immunity can also wane (e.g. nature.com/articles/s4159… & nature.com/articles/s4146…). Again, this will result in increase in susceptibility over time, and hence potential for R>1 in future. 4/
However, it's worth noting that subsequent infections for seasonal coronaviruses can come with reduced severity, so although transmission still occurs, burden can be lower during subsequent epidemics:
https://twitter.com/AdamJKucharski/status/1294985940524507136?s=205/
C: Evolution. In the case of flu, antigenic evolution can mean immunity built against recent strains doesn't fully protect against new ones (nature.com/articles/nrmic…). Note: there's no evidence this is influencing SARS-CoV-2 dynamics so far (theconversation.com/coronavirus-mu…). 6/
D: Population migration. The immunity profile of a population may change over time as susceptible individuals arrive/leave. E.g. in 2014/15 there was mass cholera vaccination in IDP camp in South Sudan; by 2016, over 80% were susceptible (journals.plos.org/plosntds/artic…) 7/
The COVID-19 pandemic will eventually end because of accumulated immunity, either following infection or - ideally - from future vaccine. But even if this means R<1 initially, the above shows there are number of long-term possibilities to consider. 8/8
• • •
Missing some Tweet in this thread? You can try to
force a refresh