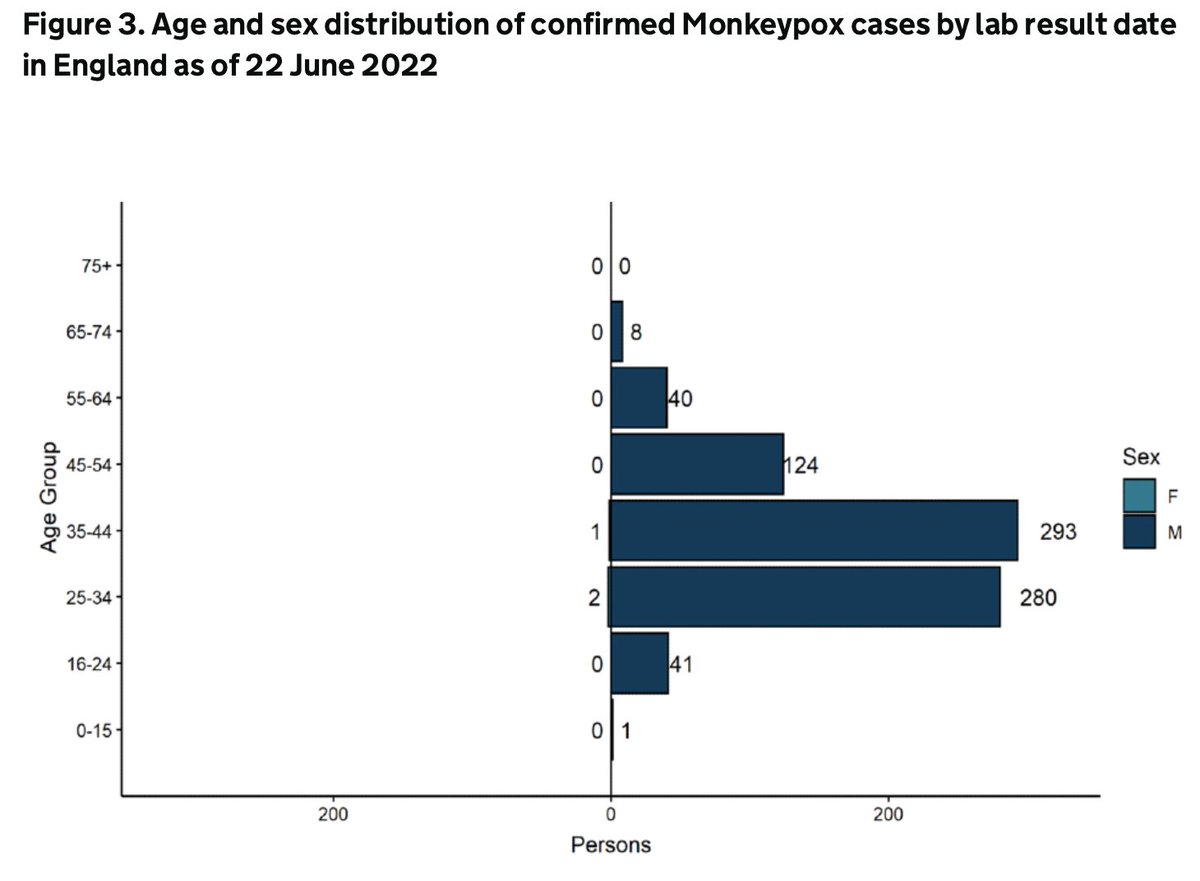
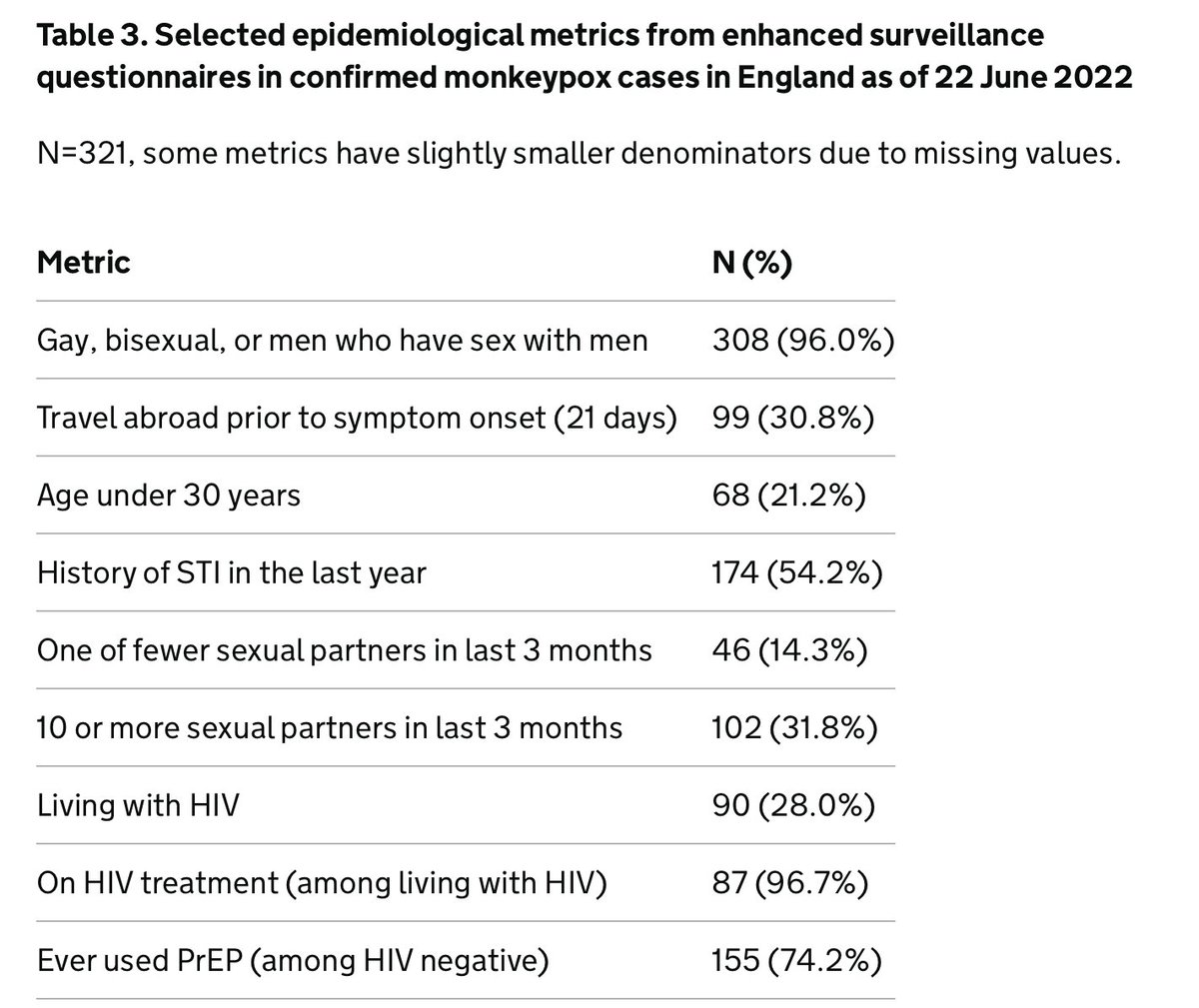
While I wait for the @WHO presser to start, I might as well share a few further comments on the recent decision not to declare the #monkeypox outbreak a public health emergency of international concern:
@WHO 1. I’ve talked to a lot more researchers and public health experts since the decision was announced and the overwhelming sentiment is that it was the wrong call.
@WHO Amongst the harshest was @MichaelWorobey who told me: "Right now PHEICs send the message that the WHO is the last institution to grasp that a newly identified outbreak is indeed a public health emergency of international concern."
@WHO @MichaelWorobey "The window may already have closed on stopping the establishment of a new sexually transmitted disease worldwide, but a PHEIC has not even been declared”, @MichaelWorobey told me.
@WHO @MichaelWorobey 2. @clarewenham told me that the emergency commitee's report basically outlined how all criteria for a PHEIC had been met and then still declined to declare one. It’s not just this panel: “There has been this inconsistent application of the criteria. And this is problematic."
@WHO @MichaelWorobey @clarewenham 3. We know very little about how effective PHEICs actually are.
That’s a problem too!
"To date there is no scientific evidence on the effect a PHEIC has,” @clarewenham told me. "We have been trying to get funding to do this research for years but without success."
That’s a problem too!
"To date there is no scientific evidence on the effect a PHEIC has,” @clarewenham told me. "We have been trying to get funding to do this research for years but without success."
@WHO @MichaelWorobey @clarewenham 4. As with so many of these issues, it would probably help to diversify who sits on these committees and include people with a background in international health law, ethics or political science.
• • •
Missing some Tweet in this thread? You can try to
force a refresh