
Geek before it became trendy. Performance, C#, Deep Learning and Financial Modeling. Former Founder of @Corvalius.
How to get URL link on X (Twitter) App

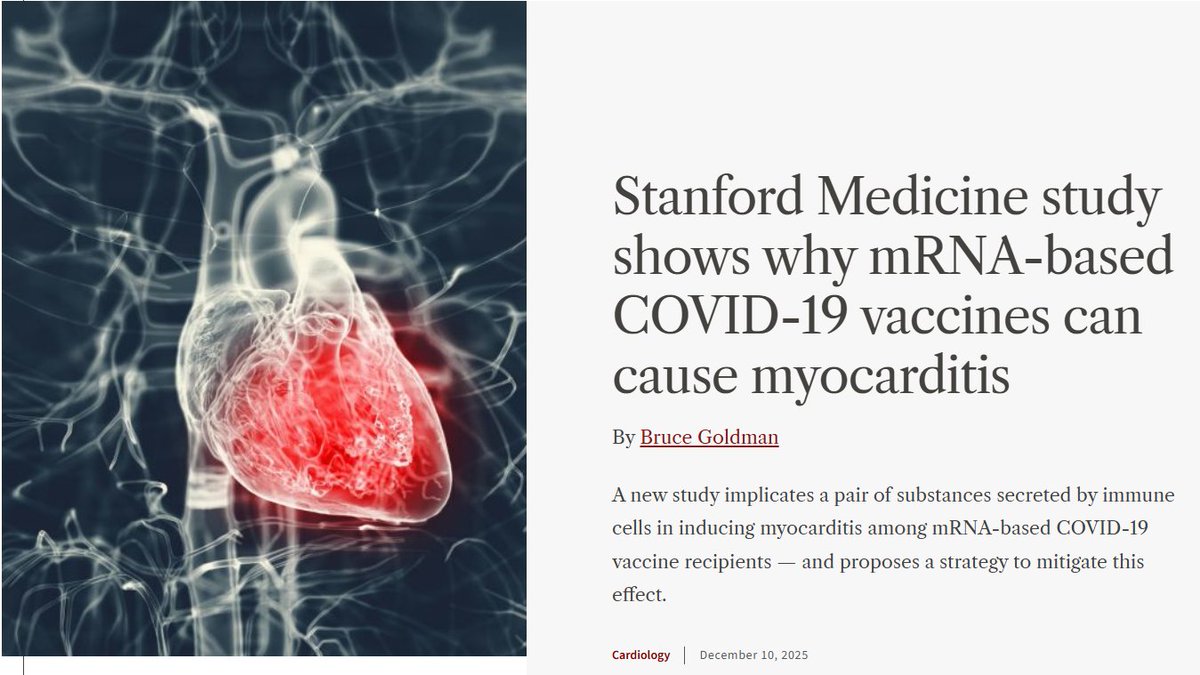
 Like, if instead of censoring us they would have been paying attention they would have known by early 2021.
Like, if instead of censoring us they would have been paying attention they would have known by early 2021. https://x.com/federicolois/status/1404201072814657537
https://twitter.com/federicolois/status/17826222503629702762/ Disclaimer: I am not a formally trained health researcher. More like a very curious and tenacious guy with a 15+ year background in research, development, & reproducibility in computer science (computer science).

https://twitter.com/aakashg0/status/1641976913165180929Normally that is an issue in general. Anyone that has done reinforcement learning had figure out (usually in the worst way) that you have to be incredible cautious with penalties. They are very prone to be gamed.

https://twitter.com/TheLeanAcademic/status/1637790306975326208

https://twitter.com/_akhaliq/status/16238591351323443202/ Since I am doing it by hand I started with a very simple prompt.

https://twitter.com/federicolois/status/1361902737265471491
https://twitter.com/federicolois/status/16204865549543997462/ Let me explain why I wrote that tweet and what the hypothesis is. The idea of the tweet was two-fold. First to test reachability velocity and second to see if it was possible to trick the algorithm to boost subsequent tweets.
https://twitter.com/LDjaparidze/status/1609008424339095552And to be fair, there are much earlier examples of that prediction because it was dead obvious.
https://twitter.com/LDjaparidze/status/1513167621549703172?t=b1uP8kINn0yVzD0TfsKHfw&s=08

https://twitter.com/federicolois/status/14292518838861291612/ Recently, the role of IgG4 in promoting antigen tolerance has come under scrutiny. However, the many ramifications and the complex mechanisms involved may be just too much for most people. jessicar.substack.com/p/igg4-and-can…
https://twitter.com/Kevin_McKernan/status/1468931104556130308

https://twitter.com/AlexEpstein/status/1606347326624215040The more we rely on this type of centrally controlled black boxes the worst this will become. I see a very interesting research opportunity into allowing distributed training to allow us to create our own models (even if based on 'faulty' ones).

https://twitter.com/federicolois/status/1361902737265471491
https://twitter.com/lexfridman/status/1245875520342032385That only covers the "Your mask protects me" part. And just in case we need to also dispel the other part of the myth. My mask does not protect you either [aka source control].
https://twitter.com/federicolois/status/1596118629506248704


https://twitter.com/JohnRTMonsonMD/status/1595893878879551489
 2/ Let's start with the basics. Ritter et al. [1975] “the wearing of a surgical face mask had no effect upon the overall operating room environmental contamination.” Oops.
2/ Let's start with the basics. Ritter et al. [1975] “the wearing of a surgical face mask had no effect upon the overall operating room environmental contamination.” Oops.https://twitter.com/davidfowl/status/1592249767366922240One then could argue the level of expertise required to achieve high performance code, and in that there is clearly some work to be done. I keep finding writing fast code easier over time, so it is not something that I believe it is done poorly or not been done.
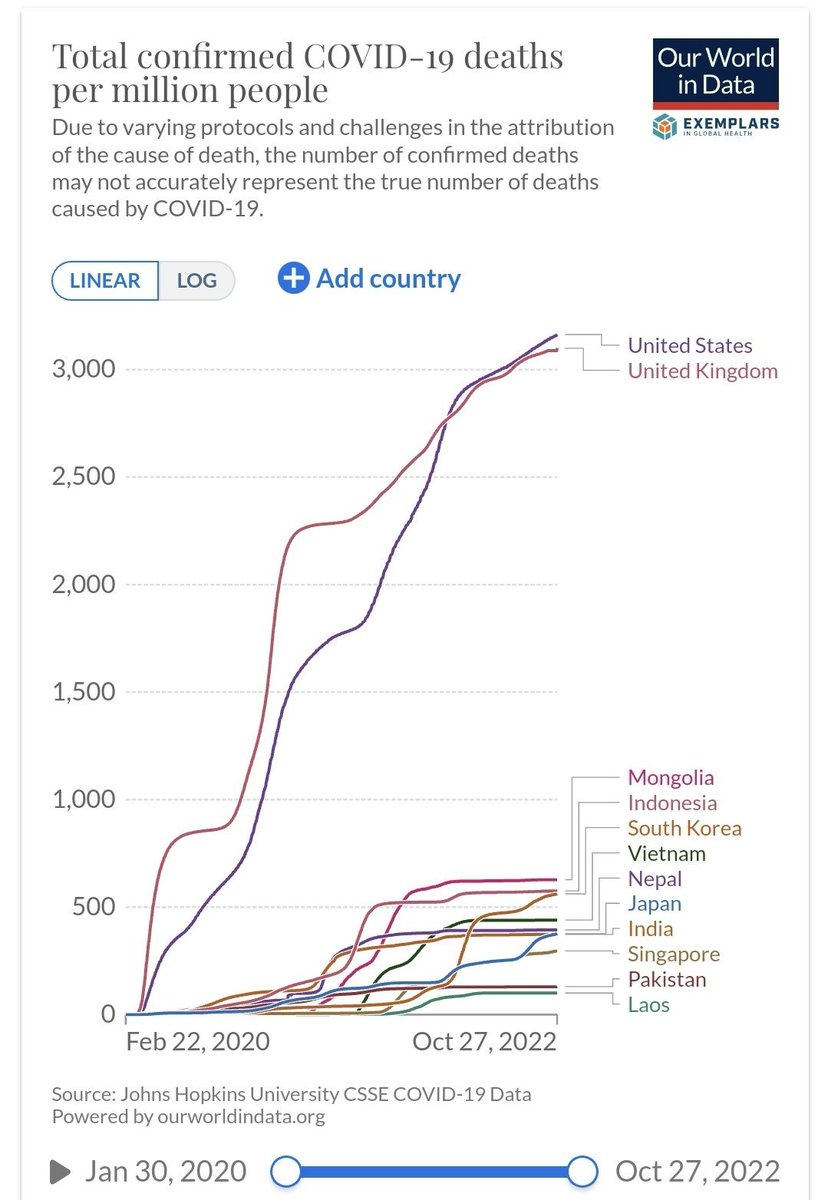
https://twitter.com/LDjaparidze/status/1590845479130206208But you may ask. Why is this paper so important? Because it gives clues about what might have transpired. It is a pretty well known 'secret' that something is rotten in not Denmark but the Asian Pacific. It is kinda difficult to explain how they are different.
