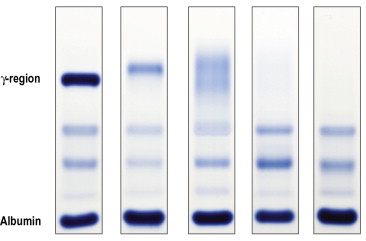
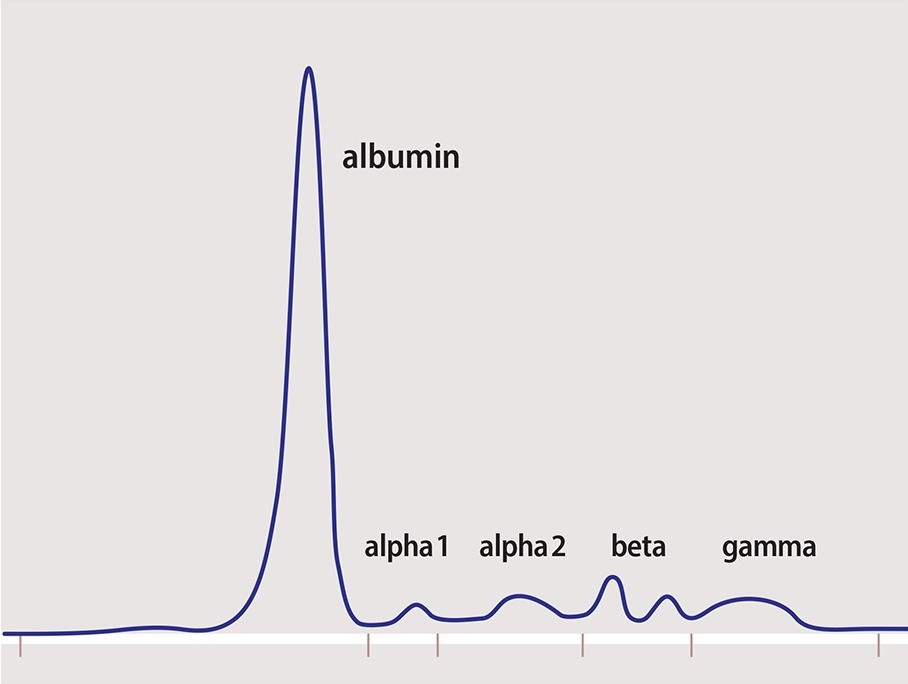
On presentation: BP 150/110, HR 134, RR 20, SpO2 98%, Tm 99.5F.
- Cough is acute (foreground). Wt loss + fatigue are chronic (background).
- Is cough the culmination of a chronic disease or a superimposed phenomenon?
- Wt loss + decent oral intake suggests calorie expenditure > calorie intake a.k.a. hypermetabolism.
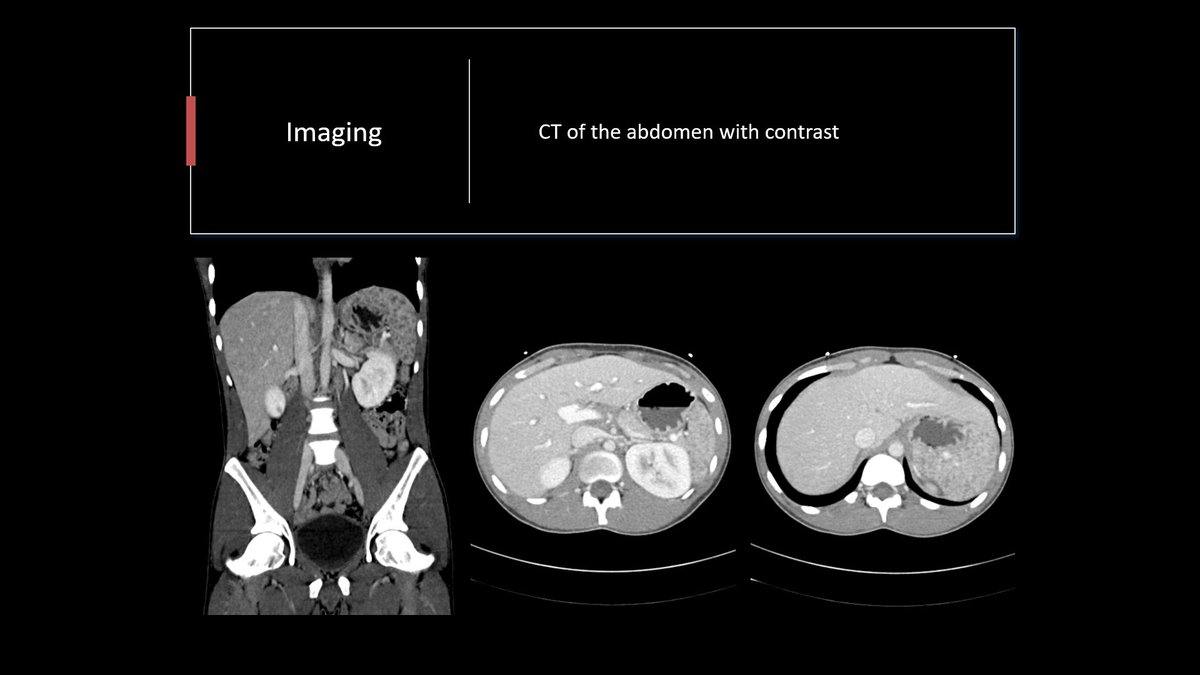
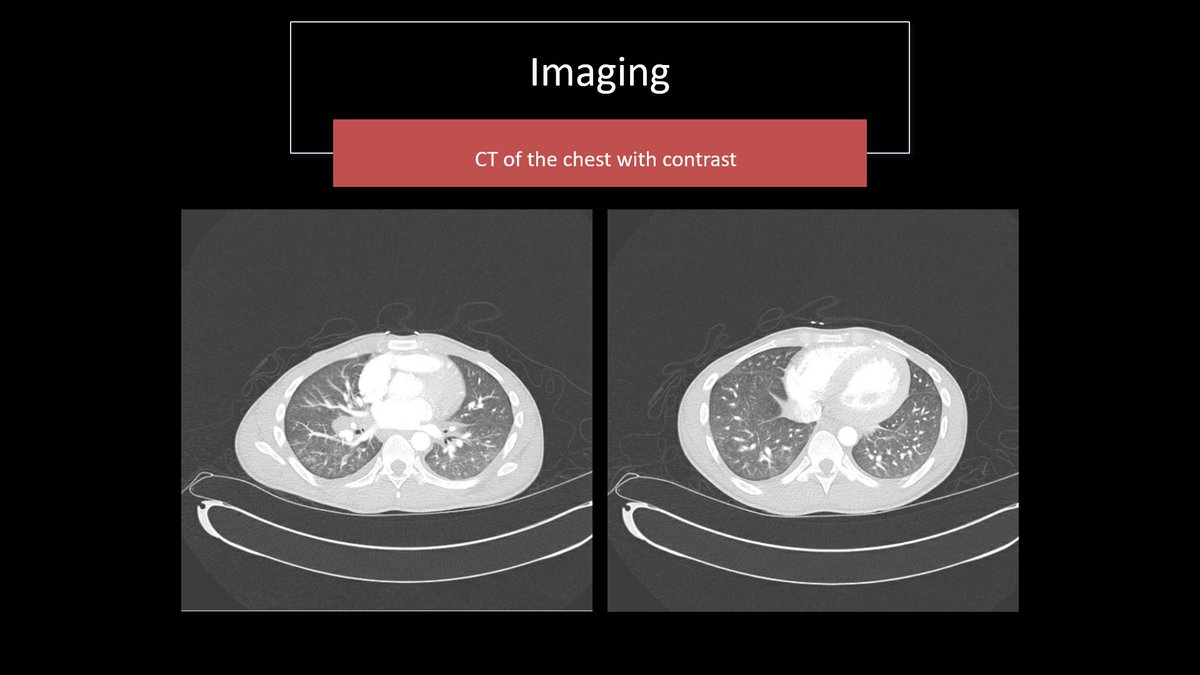
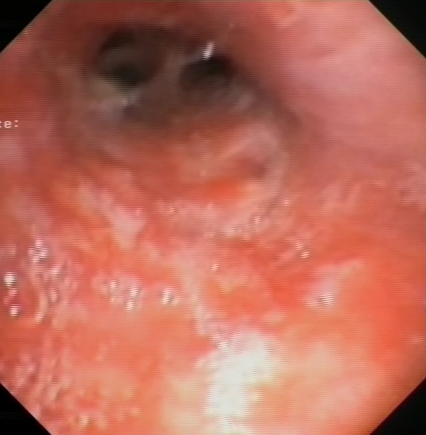
30-ish y.o. with history of T1DM and HTN presenting with acute dry cough and a background of wt loss & fatigue. Found to have tachycardia, inflammation, lactic acidosis and cholestatic liver injury. CT with hepatosplenomegaly and small hypodense lesions.
Patient was treated with 4L of IV fluids and was started on broad spectrum antibiotics.
Despite this treatment, patient’s tachycardia persisted and his HR was up to mid-120s twelve hours later.
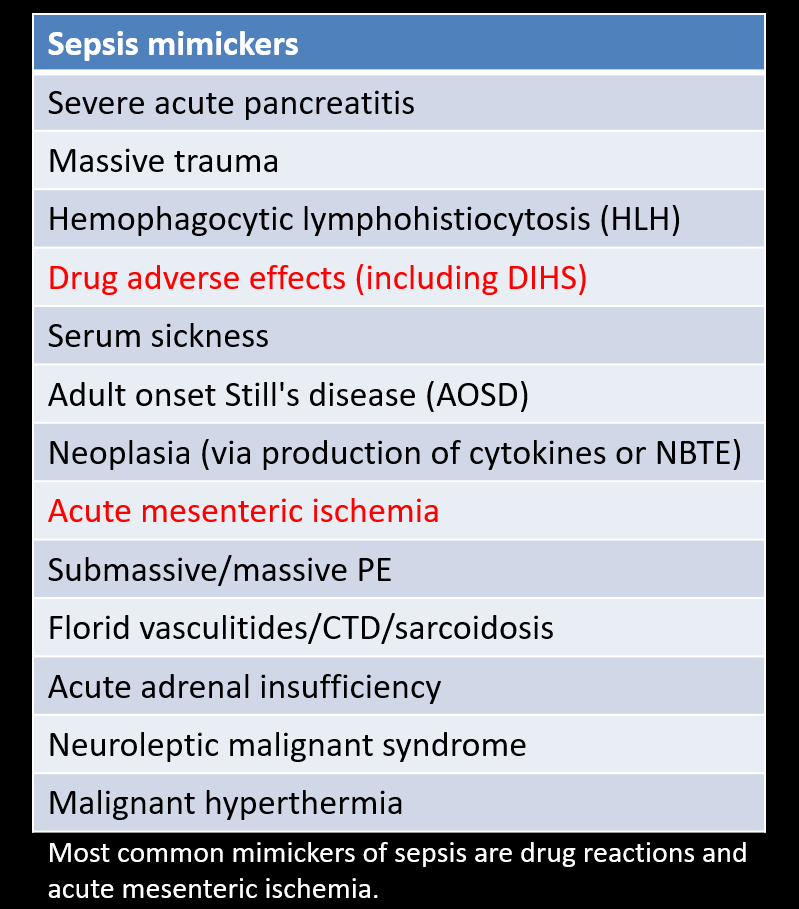
Not your typical sepsis illness script, eh?
Differentials include lymphoma, TB, atypical mycobacteriosis, endemic mycoses, sarcoidosis, amyloidosis. If immunosuppressed, can add nocardiosis, aspergillosis, cryptococcus
Non-necrotizing granulomas.
AFB and GMS were negative.
No evidence of malignancy seen.
Significant cholestatic liver injury attributed to liver infiltration. Lactic acidosis due to poor lactic acid clearance(?), cytokine-induced mitochondrial dysfunction(?).
Antibiotics were discontinued. No solid ground to call this syndrome "sepsis" was found.
Think of a non-septic SIRS when you have atypical features in presentation (Faget’s sign, lack of a source of infection & microbiological documentation within 24h, well-appearing and not feeling the fevers, lack of defervescence or change in hemodynamics despite AB
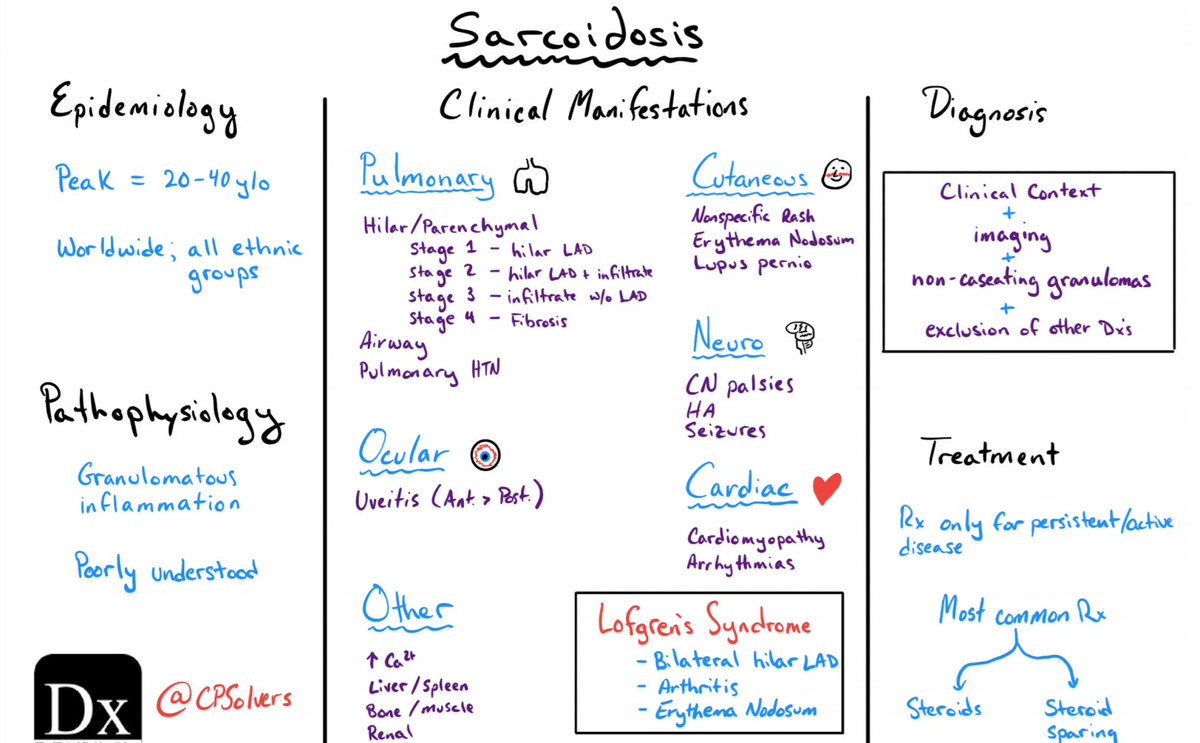
Thanks for tuning in. I leave you with a refresher schema from @CPSolvers on sarcoidosis: