School openings and children (0-18yo) have been the most complex and contested subject of the pandemic.
In this letter, we are calling for balanced and nuanced scientific and media coverage of this subject, which has been hyper-polarised and damages our public health response.
In this letter, we are calling for balanced and nuanced scientific and media coverage of this subject, which has been hyper-polarised and damages our public health response.
https://twitter.com/apsmunro/status/1304441422792327169
While we all agree in the fundamental argument that children, families, educators, and society deserve to have safer schools, the current info ecology switched from underplaying the threat to exaggerating the risks by reacting to the political climate. This is causing harm.
One would hope statistics should deliver a more objective view. But while solid data offers us insights, the numbers never speak for themselves. They, too, are shaped by our emotions, our politics and, perhaps above all, our preconceptions - @TimHarford
[ft.com/content/92f64e…]
[ft.com/content/92f64e…]
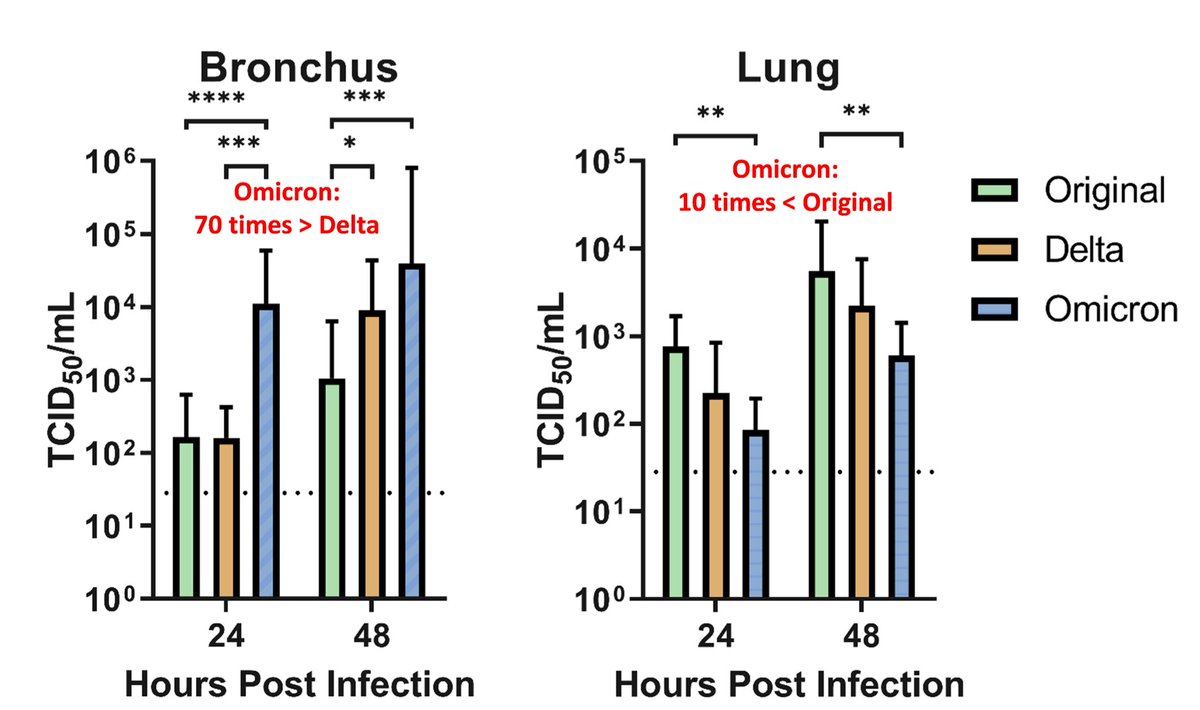
For instance, although emerging evidence suggests age differences in transmission, prior experience from influenza pandemics left many with strong beliefs re children’s role in propagating community spread that disturbs the interpretation of this data. medrxiv.org/content/10.110…
Some countries kept schools open throughout the pandemic, and many opened schools in April/May - so the argument that we do not have enough knowledge or experience in this regard is incorrect - we can learn a lot from their experience.
sciencemag.org/news/2020/07/s…
sciencemag.org/news/2020/07/s…
We are not suggesting kids are 'immune' or aren't transmitting at all, appropriate measures need to be taken. But sensationalised coverage of this topic esp by self-claimed experts & media causes distress for families, carers and children themselves.
https://twitter.com/zeynep/status/1293164662159298562?s=20
For example, almost on a daily basis, we are hearing that there is a positive kid in a school setting. But identifying a case does not mean a school outbreak. We need to be careful when reporting and interpreting this information.
https://twitter.com/AntibioticDoc/status/1303327551327096833?s=20
The complexity of the subject, therefore, demands a weighed expert review of the literature (by those who have background knowledge in the subject) that considers not only the epidemiological but also social, educational and public health concerns to accurately inform policy
For instance, school closures have brought social, economic, and racial injustice into sharp relief, with historically marginalized children and families — and the educators who serve them — suffering the most and being offered the least.
theguardian.com/education/2020…
theguardian.com/education/2020…
Many school-age children rely on their schools for free or reduced-price daily meals. Despite efforts by school districts to maintain these services, a majority of children have been unable to access the full nutritional benefits to which they’re entitled
https://twitter.com/Food_Foundation/status/1303284816738164737?s=20
While balancing values/principles are important, sadly nuance died some time ago.
"The potential costs of shunning such a nuanced approach are high. It can mean people fear small risks too much and big ones too little." @Mikepeeljourno
ft.com/content/caff8a…
"The potential costs of shunning such a nuanced approach are high. It can mean people fear small risks too much and big ones too little." @Mikepeeljourno
ft.com/content/caff8a…
Nevertheless, safely reopening schools full-time for children should be a top national priority during the pandemic - which may mean closing nonessential indoor services if necessary. We need to have nuanced and balanced discussions for this to happen.
nejm.org/doi/full/10.10…
nejm.org/doi/full/10.10…
"Our sense of responsibility toward children — at the very least, to protect them from the vicissitudes of life, including the poor decision making of adults who allow deadly infections to spiral out of control — is core to our humanity." - @meiralevinson nejm.org/doi/full/10.10… 

• • •
Missing some Tweet in this thread? You can try to
force a refresh