
Hepatologist @michiganliver @vaannarbor; #cirrhosis; encephalopathy; frailty; quality improvement; father; husband. #livertwitter Co-EIC of @HepCommJournal
How to get URL link on X (Twitter) App


 Milk Thistle, a history:
Milk Thistle, a history:





 ALT >1000 has a narrow differential diagnosis
ALT >1000 has a narrow differential diagnosishttps://twitter.com/ebtapper/status/1031555677095948289?s=20

https://twitter.com/ebtapper/status/1622263807128092674Ammonia is a biomarker of badness


https://twitter.com/ebtapper/status/1456954647214690312




 2/
2/ 
 First:
First:



 I don’t get the vitamin k thing. There is no known benefit (pubmed.ncbi.nlm.nih.gov/23080365/). And the harm is that It sends mixed signals. It undoes the teaching about the #cirrhosis coagulopathy. Because iv vit k is special and novel, it’s a consult rec that sticks. Needs reconsidering
I don’t get the vitamin k thing. There is no known benefit (pubmed.ncbi.nlm.nih.gov/23080365/). And the harm is that It sends mixed signals. It undoes the teaching about the #cirrhosis coagulopathy. Because iv vit k is special and novel, it’s a consult rec that sticks. Needs reconsidering

 2/
2/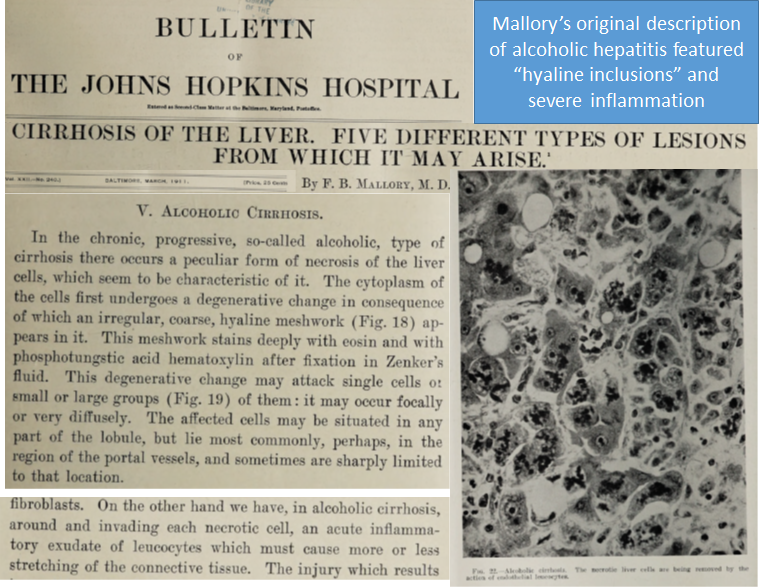

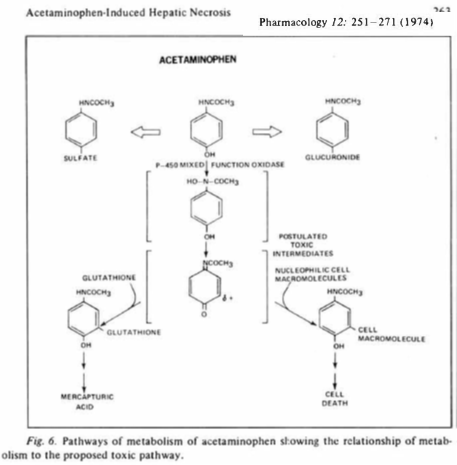
 2/
2/
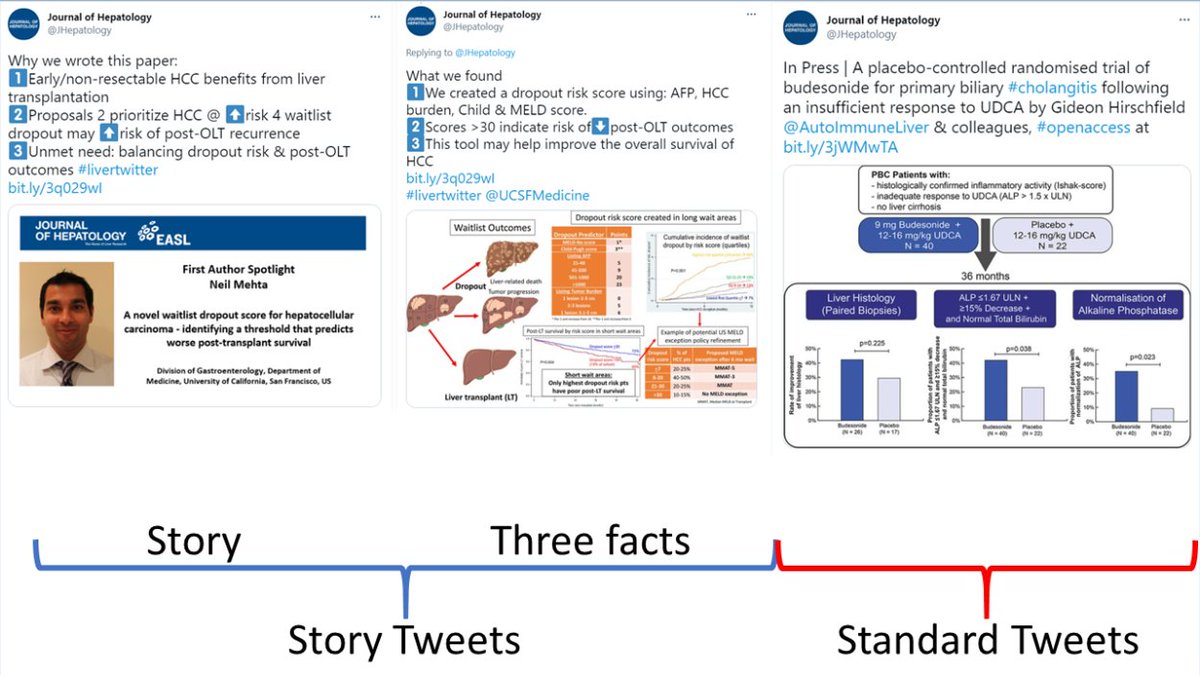
 We found that story tweets garnered more downloads and tweet impressions
We found that story tweets garnered more downloads and tweet impressions
 2/
2/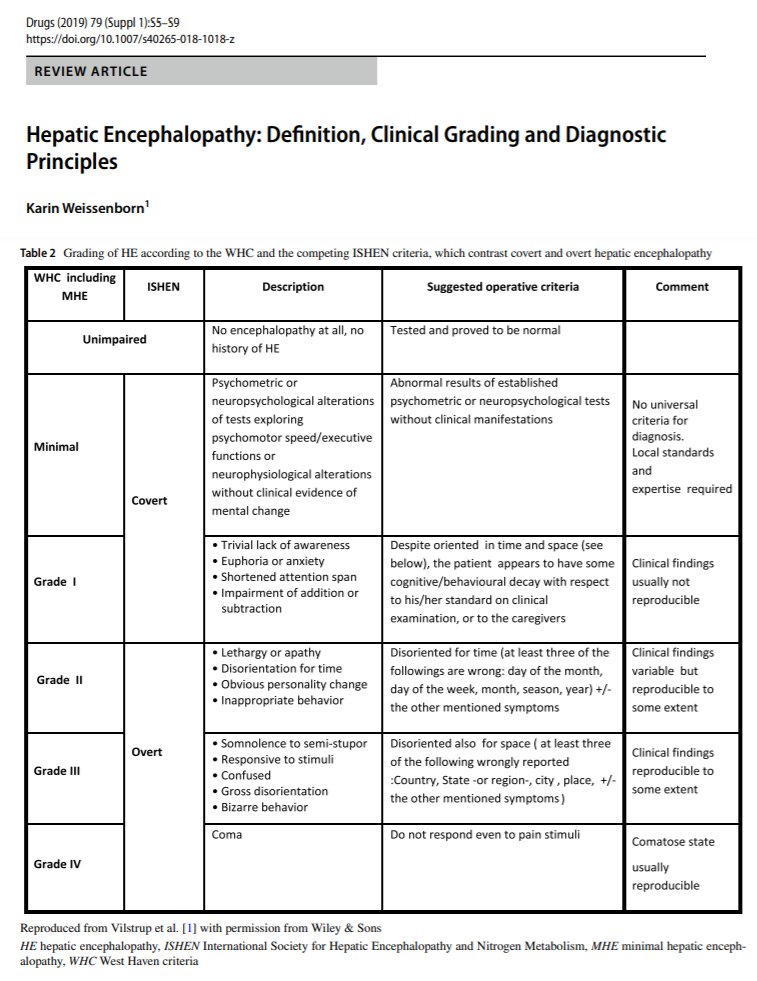

 2/
2/

