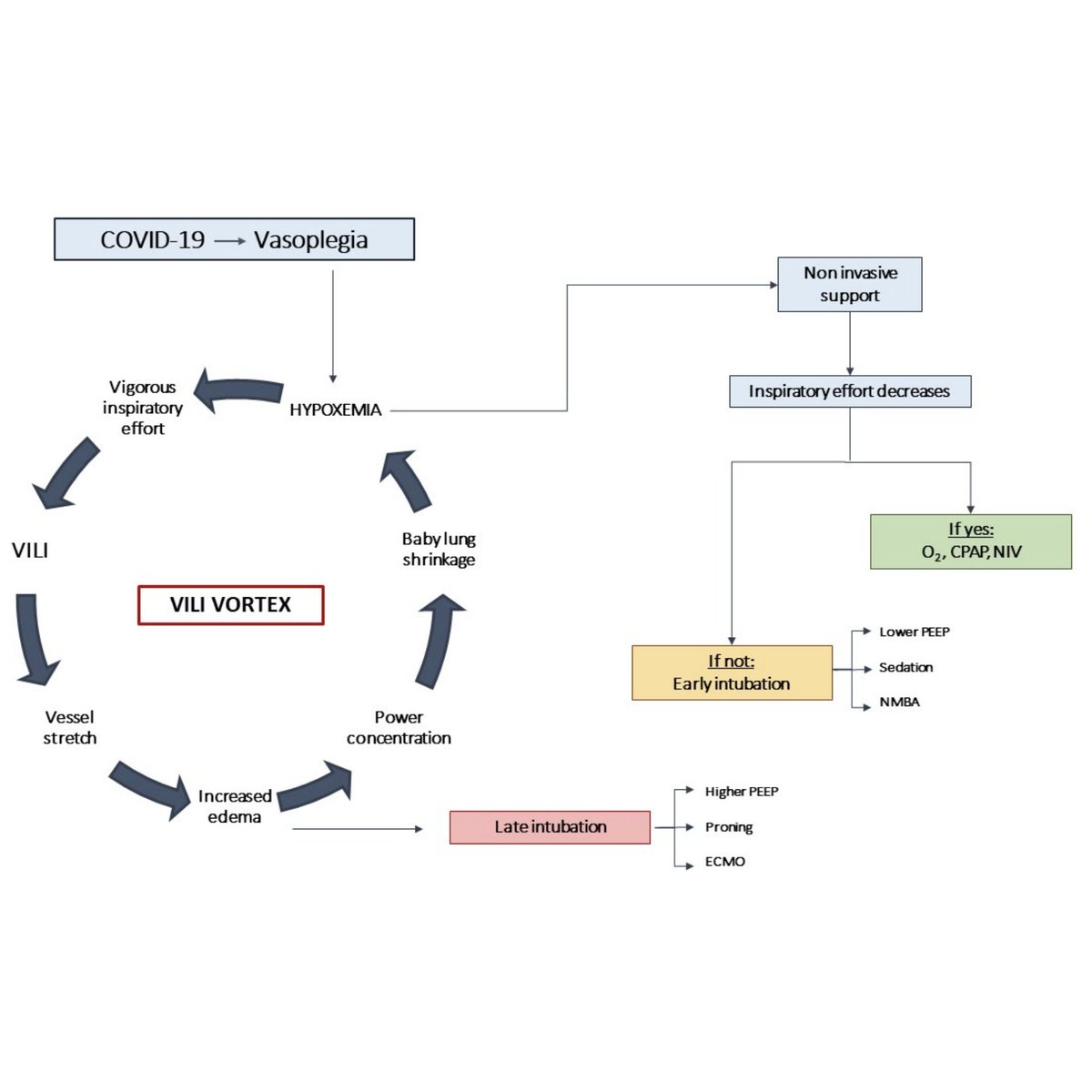
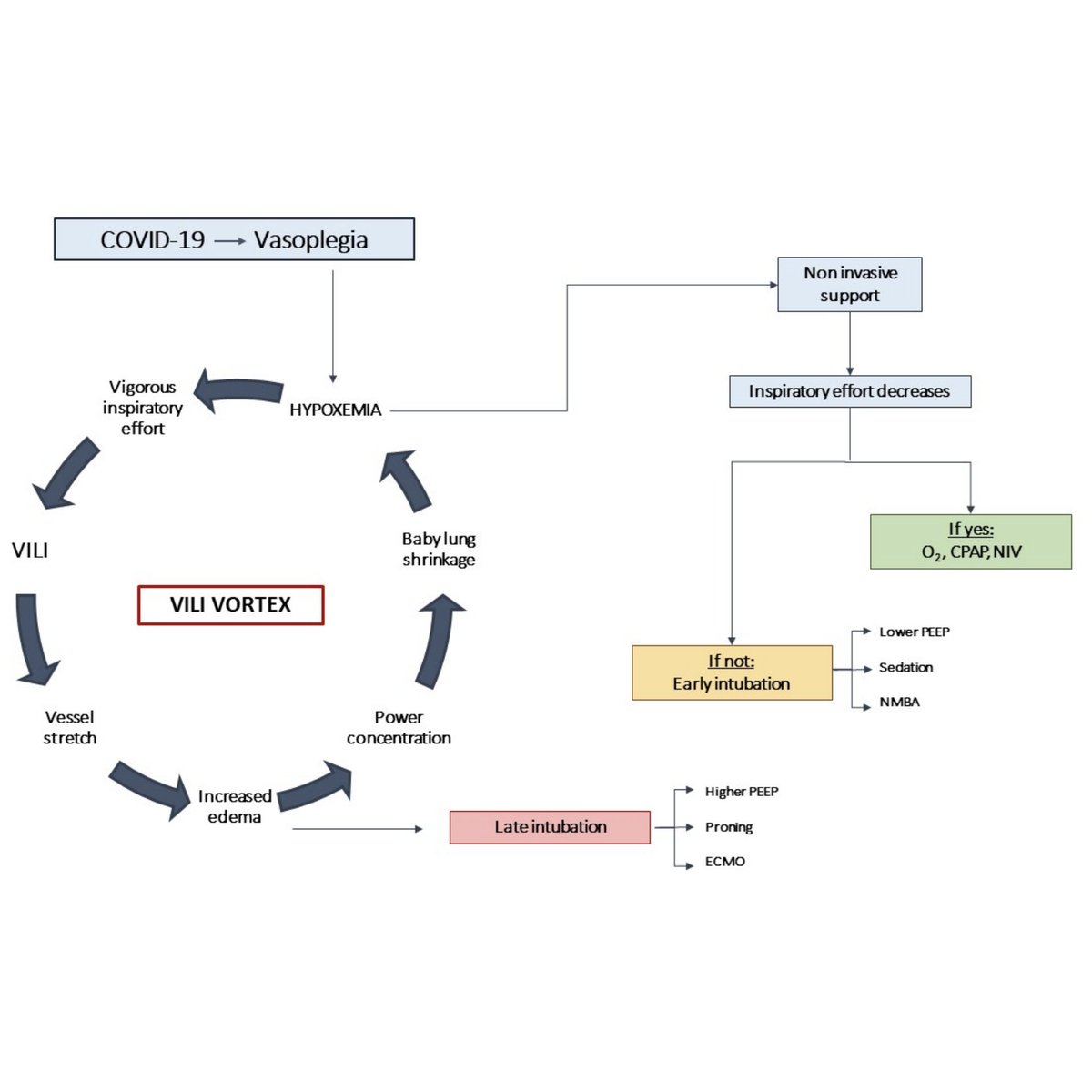
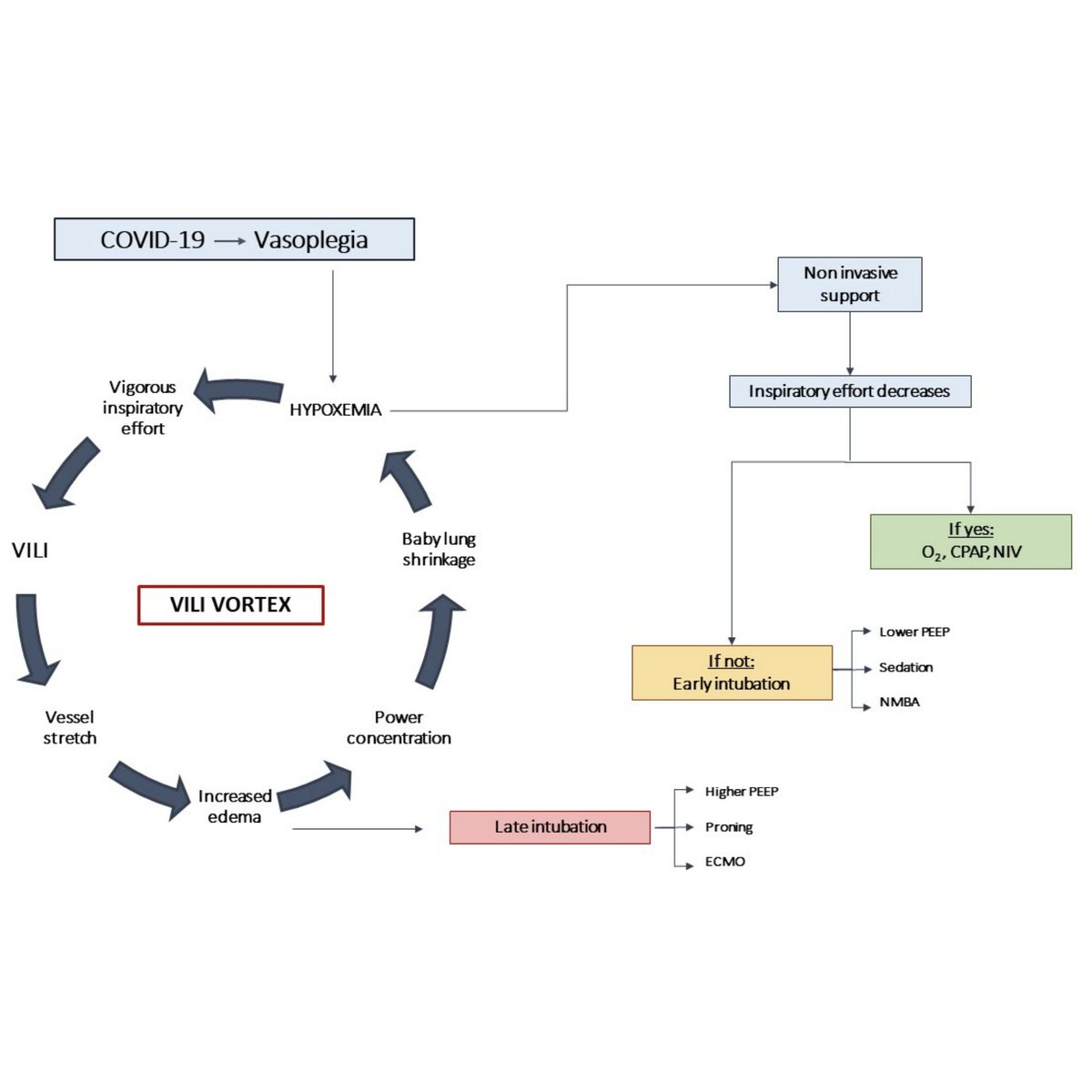
*Three* RCTs and a new @WHO meta-analysis add to #RECOVERY trial data that corticosteroids reduce mortality in critically ill #COVID19 patients
jamanetwork.com/journals/jama/…
i. Low-dose hydrocortisone didn't reduce death, persistent respiratory support at day 21 vs placebo among critically ill patients w #COVID19 and ARF, but the study was stopped early when RECOVERY trial findings were announced
ja.ma/31NqEDf
ii. IV #dexamethasone increased the number of ventilator-free days by day 28 vs standard care alone among patients with COVID19 and moderate or severe ARDS
ja.ma/3bjH2yt
@ICURevisited @FlaviaSepsis @israelmaia16
iii. Hydrocortisone (HC) 7d fixed- vs shock-dependent dosing led to 93% and 80% probability of superiority vs no HC in organ support–free days in pts w severe #COVID19, but the trial was stopped early
ja.ma/2DnIV0O
@remap_cap @PittCCM
@WHO meta-analysis of RCTs of critically ill patients with #COVID19: systemic corticosteroids vs usual care or placebo associated with lower 28-day all-cause mortality
ja.ma/2YSPUXa
@setiogi @jonathansterne of @BristolUni
"The #COVID19 pandemic may be a tipping point in the long saga of corticosteroid use in critical illness, when data supported a strong rec to treat most #ARDS patients with the drugs"
ja.ma/2QHsn6U
@HalliePrescott @toddrice_ICU
@WHO "Living Guidance" document
"Rec 1: We recommend systemic corticosteroids vs none for treatment of patients w severe and critical #COVID19 (strong recommendation based on moderate certainty evidence)"
apps.who.int/iris/bitstream…
@setiogi
@WHO "Living Guidance" document
"Rec 2: We suggest not using corticosteroids for treatment of patients with non-severe
#COVID19 (conditional recommendation, based on low certainty evidence)"
apps.who.int/iris/bitstream…
@setiogi