
Past President @BrHeartValveSoc
Father•Son•Husband•Cardiologist (Imaging)
Accredited Cardiology Expert Witness (Civil Law)
Founder of Get Published in Medicine
How to get URL link on X (Twitter) App


 What I had planned on saying:
What I had planned on saying:
 First troponin I is 358ng/L (normal <18)
First troponin I is 358ng/L (normal <18)


 On Sunday I wrote a thread about asymptomatic severe AS and what we knew already from RECOVERY & AVATAR RCTs and what the guidelines currently advocate
On Sunday I wrote a thread about asymptomatic severe AS and what we knew already from RECOVERY & AVATAR RCTs and what the guidelines currently advocatehttps://x.com/dr_benoy_n_shah/status/1850645694698135554?t=TAVDsW79WuDguZBGOutVBg&s=19




 #TCT2024
#TCT2024 


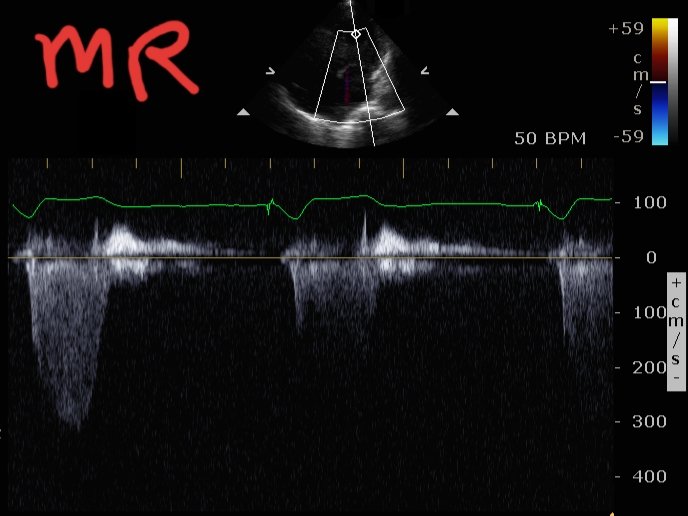

 Lots of excellent replies. A lot of information to glean from 'just' the CW Doppler traces
Lots of excellent replies. A lot of information to glean from 'just' the CW Doppler traces

 Before going further, we should clarify what PE actually is. Now, I am NOT a financial expert at all, but here goes...!
Before going further, we should clarify what PE actually is. Now, I am NOT a financial expert at all, but here goes...!

 Prior to this, 'stress testing' to evaluate cardiac function was performed using the Masters 2-step technique, first described in 1935. This crude but simple test involved repeated steps up & down over 90 seconds
Prior to this, 'stress testing' to evaluate cardiac function was performed using the Masters 2-step technique, first described in 1935. This crude but simple test involved repeated steps up & down over 90 seconds
https://twitter.com/denisamuraru/status/1701098650946912320
 We know now that it is perfectly possible for symptomatic individuals to have abnormal stress tests, with inducible ischaemia, but not have significant epicardial CAD on angiography
We know now that it is perfectly possible for symptomatic individuals to have abnormal stress tests, with inducible ischaemia, but not have significant epicardial CAD on angiography 
 The establishment of the NHS was the culmination of attempts to provide healthcare services to Britain’s citizens for at least a century
The establishment of the NHS was the culmination of attempts to provide healthcare services to Britain’s citizens for at least a century
 It starts off with a foreward from current NHS CEO Amanda Pritchard
It starts off with a foreward from current NHS CEO Amanda Pritchard

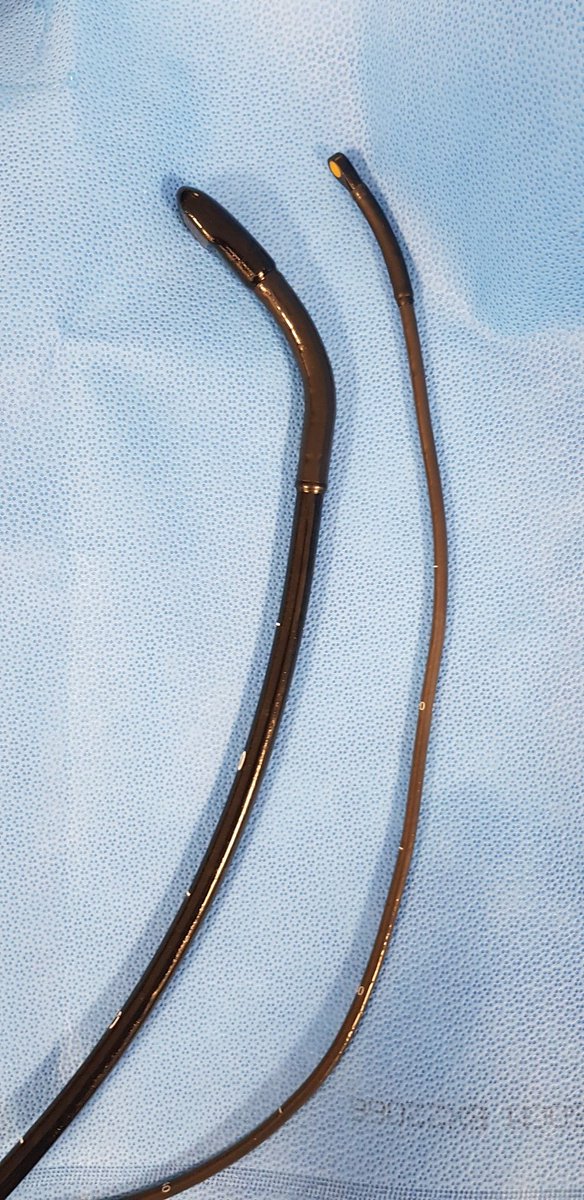
 TOE/TEE is actually one of the safer procedures we do, complications are less likely than with:
TOE/TEE is actually one of the safer procedures we do, complications are less likely than with:
 #EACVI2023
#EACVI2023 





 #ESCCongress
#ESCCongress 

 #ESCCongress
#ESCCongress 




