1. What proportion of the population needs to be vaccinated to achieve herd immunity? It depends on a number of factors, including how contagious a virus is, and how well a vaccine can prevent infection.
Even very contagious variants can be stopped if efficacy is high enough. 🧵
Even very contagious variants can be stopped if efficacy is high enough. 🧵

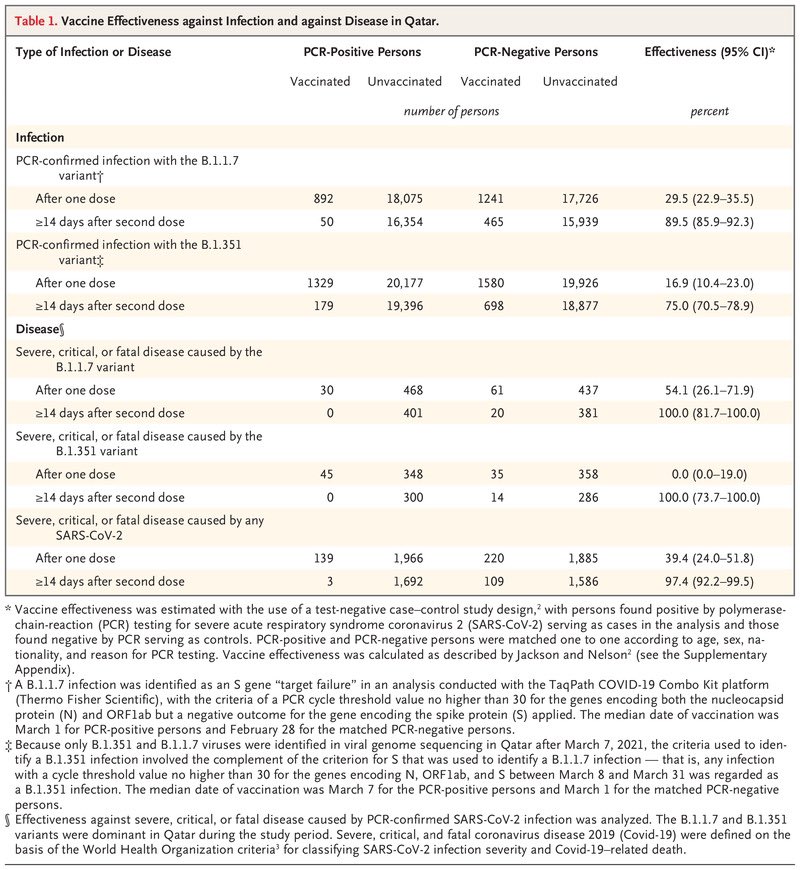
2. This is a very simple model with lots of assumptions, but gives a rough idea of what we need to aim for to achieve herd immunity against SARS-CoV-2.
Four theoretical vaccines are shown, with 60 to 90% efficacy against infection.
Four theoretical vaccines are shown, with 60 to 90% efficacy against infection.
3. Vertical lines mark estimates of the contagiousness of the original strain of SARS-CoV-2, the UK (B.1.1.7) variant, & the Indian (B.1.617.2) variant.
The proportion of people needing to be vaccinated (vertical axis) is the point where the vaccine & variant lines intersect.
The proportion of people needing to be vaccinated (vertical axis) is the point where the vaccine & variant lines intersect.
4. Herd immunity could be achieved with a vaccine that had 60% efficacy against the original strain, but it would require the entire population to be vaccinated (red line).
But a vaccine that had 90% efficacy might only require two-thirds of the population to be vaccinated.
But a vaccine that had 90% efficacy might only require two-thirds of the population to be vaccinated.
5. However, we're unfortunately not dealing with the original strain any more.
If you look at the black dashed line, you can see we'd probably need over 80% of people to be vaccinated to achieve herd immunity against the UK variant, and perhaps around 90% for the Indian variant.
If you look at the black dashed line, you can see we'd probably need over 80% of people to be vaccinated to achieve herd immunity against the UK variant, and perhaps around 90% for the Indian variant.

6. Does this mean there's no point being vaccinated with a moderate-efficacy vaccine? No!
All of the COVID-19 vaccines do a very good job of preventing people from getting really sick.
If you're offered the chance of vaccination, you should take it.
All of the COVID-19 vaccines do a very good job of preventing people from getting really sick.
If you're offered the chance of vaccination, you should take it.
7. However, if we don’t achieve herd immunity, there will still be some transmission of the virus in the community.
Most vaccinated people won't get seriously ill, but people who can't be vaccinated because of medical conditions will be at risk.
Most vaccinated people won't get seriously ill, but people who can't be vaccinated because of medical conditions will be at risk.
8. And while the vaccines are very good at preventing severe disease, they aren't 100% effective.
So if there's still some ongoing transmission, even some vaccinated people will get ill if herd immunity isn't achieved.
So if there's still some ongoing transmission, even some vaccinated people will get ill if herd immunity isn't achieved.
9. Ongoing transmission also provides opportunities for the virus to continue to evolve. The best defence against the emergence of new vaccine-resistant variants is to suppress transmission as much as possible with vaccination (& masks, ventilation, etc., while we're doing it).
10. Let's aim for herd immunity & eliminate COVID-19.
Stamping out the virus with public health measures and locking these gains in with vaccination provides the best outcomes in terms of health, social freedom, and the economy, over both the short and long-term.
Stamping out the virus with public health measures and locking these gains in with vaccination provides the best outcomes in terms of health, social freedom, and the economy, over both the short and long-term.
• • •
Missing some Tweet in this thread? You can try to
force a refresh