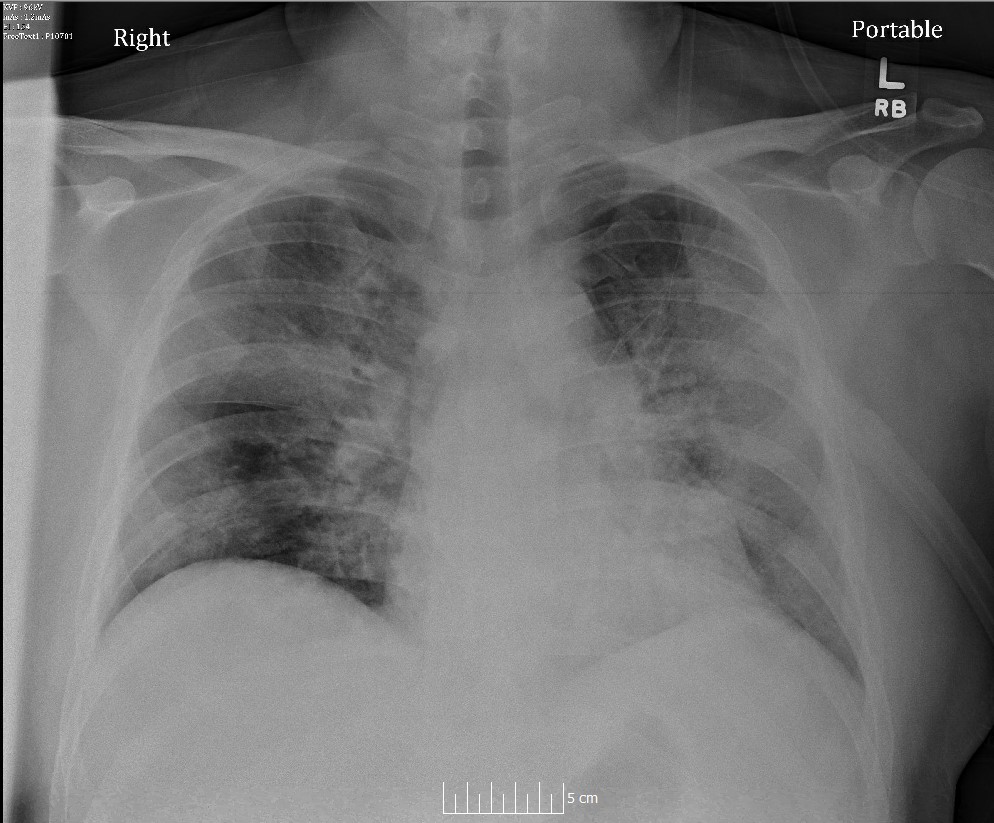
You're going to place a central line on a hypotensive patient. 💉
You got this 💪🏽
You put the ultrasound probe on their IJ to take a look 😷👀
And you see this👇🏾
😳😱😱
#FOAMed #FOAMus #FOAMcc
@POCUS_Society @UBemSono @EM_RESUS @MaimoUltrasound @EMUGs_ @SAEMAEUS @sinaiemus
You got this 💪🏽
You put the ultrasound probe on their IJ to take a look 😷👀
And you see this👇🏾
😳😱😱
#FOAMed #FOAMus #FOAMcc
@POCUS_Society @UBemSono @EM_RESUS @MaimoUltrasound @EMUGs_ @SAEMAEUS @sinaiemus
🌊 Turbulent Flow 🌊
Some of the many but not all causes include:
♦️Thrombi, Clots & Hypercoaguable States
♦️Vessel Stenosis & PVD (often from Atherosclerosis)
♦️Disorders affecting viscosity (PCV, Waldenstrom, etc)
♦️Sickle Cell
#FOAMed @UltrasoundMD @jeff_sono @grepmeded
Some of the many but not all causes include:
♦️Thrombi, Clots & Hypercoaguable States
♦️Vessel Stenosis & PVD (often from Atherosclerosis)
♦️Disorders affecting viscosity (PCV, Waldenstrom, etc)
♦️Sickle Cell
#FOAMed @UltrasoundMD @jeff_sono @grepmeded
In this patient, a clot further down the IJ prevented the CVC from being placed.😕
Use caution before attempting CVC placement in patients w/this much turbulent flow & consider some underlying causes!
#FOAMed @PittIMPOCUS @TempleEMUS @ultrasoundREL @ultrasoundpod @ACEP_EUS
Use caution before attempting CVC placement in patients w/this much turbulent flow & consider some underlying causes!
#FOAMed @PittIMPOCUS @TempleEMUS @ultrasoundREL @ultrasoundpod @ACEP_EUS
• • •
Missing some Tweet in this thread? You can try to
force a refresh