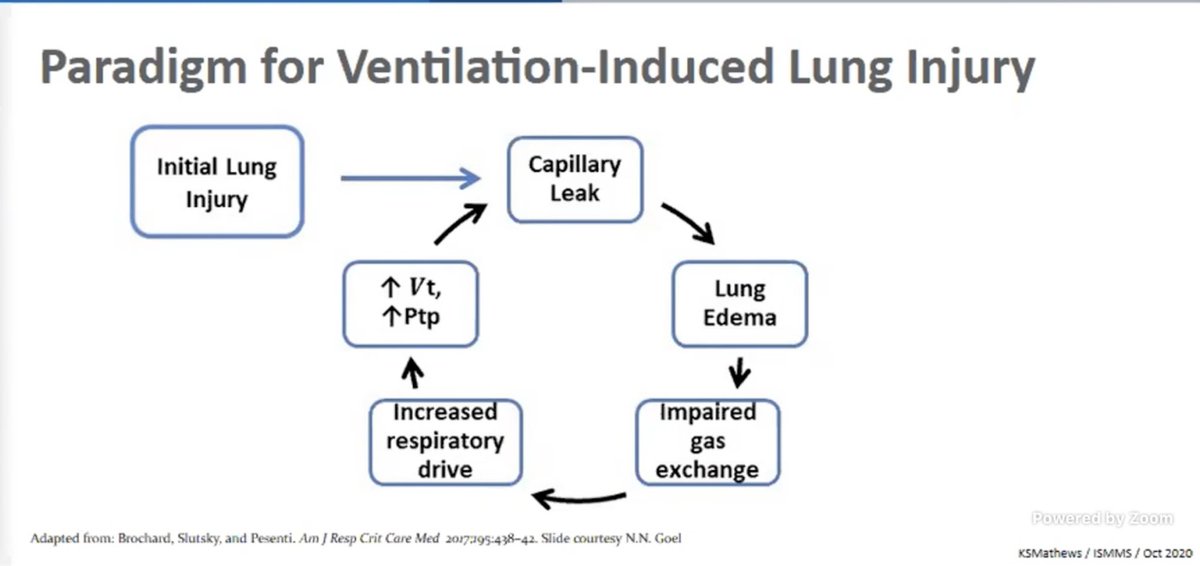
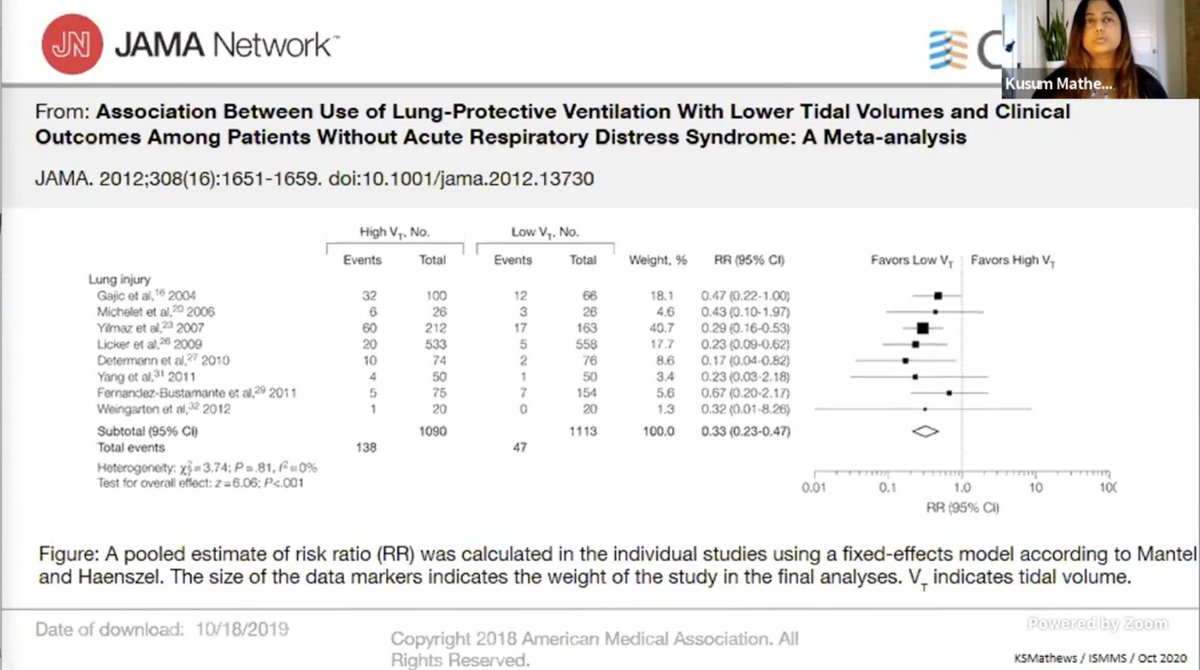
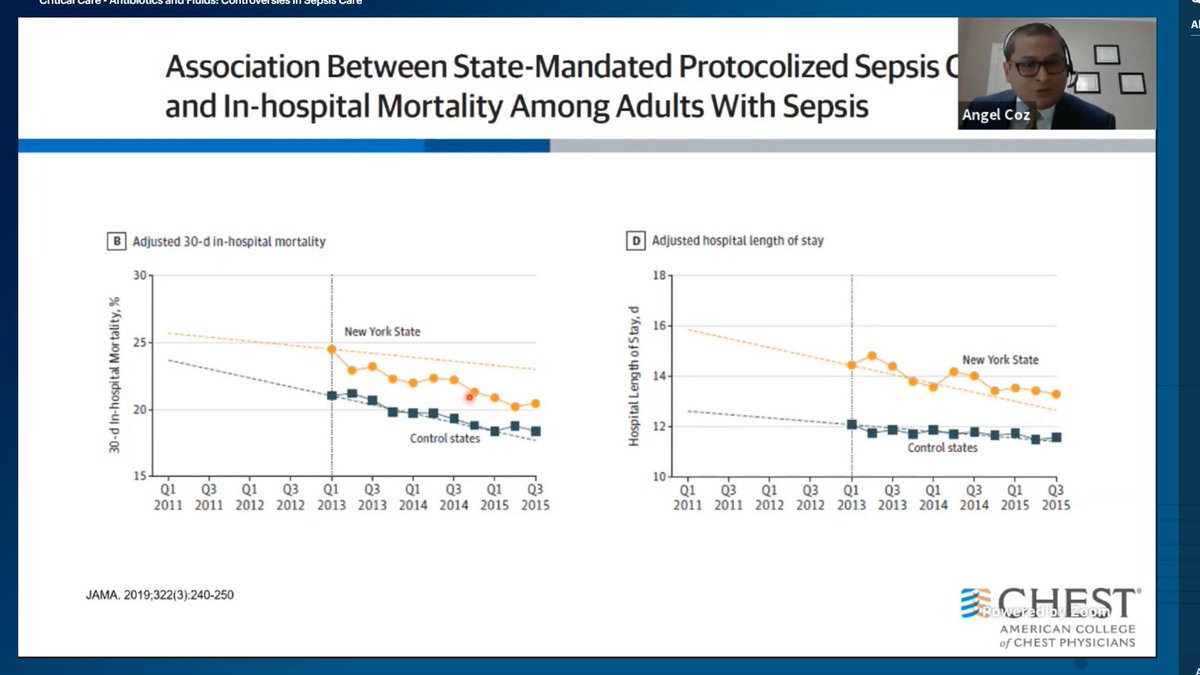
What does a TEG do? A 🧵
Several blood tests are used to assess clinical diagnosis of coagulopathies: PT, INR, APTT, platelet count, activated clotting time, bleeding time. Specific clotting factors can also be measured: Factor V, protein C and S, anti-thrombin III, anticardiolipin antibodies.
These tests are all very specific and useful in certain clinical scenarios (anticoagulation monitoring, investigation of unprovoked PE, for example), but they usually have a long turnaround time and rarely measure platelet function and the activity of the clotting cascade.
Thromboelastography (TEG) was developed and first described by Dr. Hellmut Hartert in 1948, in Germany. #chestcritcare @accpchest
pubmed.ncbi.nlm.nih.gov/18101974/
pubmed.ncbi.nlm.nih.gov/18101974/
TEG measures the ability of whole blood to form a clot, by detecting and quantifying dynamic changes of its viscoelastic properties under low shear stress.
#chestcritcare @accpchest
ncbi.nlm.nih.gov/books/NBK53706…
#chestcritcare @accpchest
ncbi.nlm.nih.gov/books/NBK53706…
Reaction time (R) is the time to the 1st detectable clot formation, depends on the concentration and function of the coagulation factors;
#chestcritcare @accpchest
#chestcritcare @accpchest
Kinetics (K) time from the beginning of clot formation to a clot w/ a certain level of strength, depends on the concentration of fibrinogen and its activation; alpha angle is the imaginary line from the time of clotting initiation to the max clot formation speed.
#chestcritcare
#chestcritcare
The alfa angle depends on fibrinogen concentration and to a lesser extend on platelets. Maximum amplitude (MA) is the maximal amplitude of the curve and reflects the maximal strength of the clot, depends on plt number, clotting factors interactions and fibrin cross-linking
Lysis at 30 minutes (LY30) is the percentage of the amplitude reduction 30 min after reaching max amplitude, depends on the presence of plasmin, plasminogen and its activation.
#chestcritcare @accpchest
#chestcritcare @accpchest
So when should a TEG be used? There is enough evidence for its use in cardiac surgery, improving patients' outcomes by decreasing blood product transfusion and the need for re-exploration #chestcritcare @accpchest
pubmed.ncbi.nlm.nih.gov/27363652/
pubmed.ncbi.nlm.nih.gov/27363652/
There is conflicting evidence for its use in bleeding from trauma. There is not enough data to favor the use of TEG over PT/INR in the diagnosis of traume-induced coagulopathy. @accpchest #chestcritcare
pubmed.ncbi.nlm.nih.gov/25686465/
pubmed.ncbi.nlm.nih.gov/25686465/
In major trauma, TEG is better in predicting the need for transfusion of FFP, RBCs, and platelets compared to conventional coagulation tests of PT, aPTT, INR, platelet count, and fibrinogen
@accpchest #chestcritcare
pubmed.ncbi.nlm.nih.gov/22868371/
@accpchest #chestcritcare
pubmed.ncbi.nlm.nih.gov/22868371/
In ECMO patients, a small RCT showed that TEG was better at guiding anticoagulation compared to APTT, reducing the dose of heparin used.
@accpchest #chestcritcare
pubmed.ncbi.nlm.nih.gov/29340875/
@accpchest #chestcritcare
pubmed.ncbi.nlm.nih.gov/29340875/
TEG has been found to be helpful in detecting intraoperative coagulopathy in liver transplant.
#chestcritcare @accpchest
pubmed.ncbi.nlm.nih.gov/20185519/
#chestcritcare @accpchest
pubmed.ncbi.nlm.nih.gov/20185519/
The use of TEG to guide blood products transfusion in critically ill patients outside of major trauma, cardiac surgery and liver Tx population still lacks evidence.
@accpchest #chestcritcare
@accpchest #chestcritcare
• • •
Missing some Tweet in this thread? You can try to
force a refresh