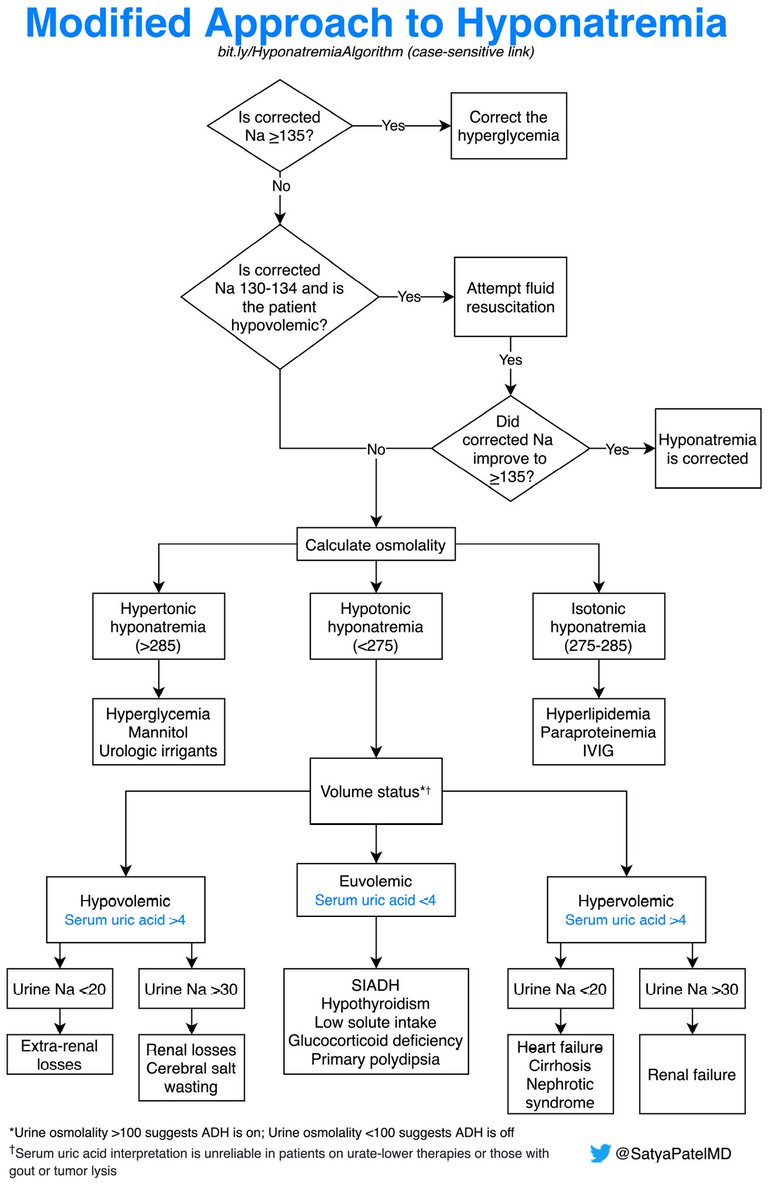
1/11 I like this flowchart, but my brain starts to melt. If yours does to, follow along and we'll take it from the top! This is my first #tweetorial on hypercortisolism!
#MedEd #MedTwitter #FOAMEd #MedStudentTwitter #EndoTwitter
bitly.ws/bDnZ
#MedEd #MedTwitter #FOAMEd #MedStudentTwitter #EndoTwitter
bitly.ws/bDnZ

2/11 Let's start with a question. Which of the following are TRUE?
a. Cushing disease = hypercortisolism
b. Cushing disease is a type of Cushing syndrome
c. Cushing syndrome is a type of Cushing disease
a. Cushing disease = hypercortisolism
b. Cushing disease is a type of Cushing syndrome
c. Cushing syndrome is a type of Cushing disease
4/11 Once we suspect hypercortisolism, the next step is to:
5/11 Take that history! Our goal is to figure out if the patient is taking any steroids (inhaled, oral, topical, injectable). If they are, this is EXOGENOUS hypercortisolism.
6/11 If you are concerned about ENDOGENOUS hypercortisolism, we have to start looking at tests, but before that, let's start getting our paradigm straightened out. 

7/11 Before we continue, we have to look at the HPA axis. Here is one of the clearest versions that I can find:
bitly.ws/bDo7
bitly.ws/bDo7

8/11 Let's go back to ENDOGENOUS hypercortisolism. We have two think of two types.
1. ACTH-dependent
2. ACTH-independent
1. ACTH-dependent
2. ACTH-independent
9/11 In ACTH-dependent hypercortisolism:
Something is ⬆️ circulating ACTH, leading to ⬆️ serum cortisol (go look at the HPA axis in tweet 7!)
Something is ⬆️ circulating ACTH, leading to ⬆️ serum cortisol (go look at the HPA axis in tweet 7!)

10/11 In ACTH-independent hypercortisolism
Something is ⬆️ circulating cortisol, leading to ⬇️ ACTH levels (go look at the HPA axis in tweet 7!)
Note: EXOGENOUS hypercortisolism is also ACTH-independent
Something is ⬆️ circulating cortisol, leading to ⬇️ ACTH levels (go look at the HPA axis in tweet 7!)
Note: EXOGENOUS hypercortisolism is also ACTH-independent

11/11 If we combine all of this, we get this paradigm for hypercortisolism. There is nuance with this, and we will get there in a stepwise fashion. As always, feedback is welcome! 

• • •
Missing some Tweet in this thread? You can try to
force a refresh