
Dermatologist/internist @ MGH- Love complex/onco-dermatology & MedEd | Harvard Derm APD | Dad | Husband | Recovering a cappella nerd. Tweets are mine & ≠ advice
How to get URL link on X (Twitter) App


 Reminder that Pemphigus is from an antibody targeting the Desmosome - which holds skin cells (keratinocytes) together.
Reminder that Pemphigus is from an antibody targeting the Desmosome - which holds skin cells (keratinocytes) together.

 Did you notice those two rings above? That's how it works.
Did you notice those two rings above? That's how it works.

 Let's start with the basics. What causes Lyme?
Let's start with the basics. What causes Lyme? 


 Let's go back to the basics. Syphilis is from an infection by the bacterium Treponema pallidum. Usually spread by sexual means, syphilis has three main stages of disease.
Let's go back to the basics. Syphilis is from an infection by the bacterium Treponema pallidum. Usually spread by sexual means, syphilis has three main stages of disease.



 What is Pemphigus Vegetans? This is where breaking down the terms can be super helpful. It's the diagnosis we give when pemphigus has the morphology of vegetative plaques.
What is Pemphigus Vegetans? This is where breaking down the terms can be super helpful. It's the diagnosis we give when pemphigus has the morphology of vegetative plaques.https://twitter.com/DrStevenTChen/status/1484569902744748032?s=20&t=rwSrCR-84l-No_-EwOFCVA


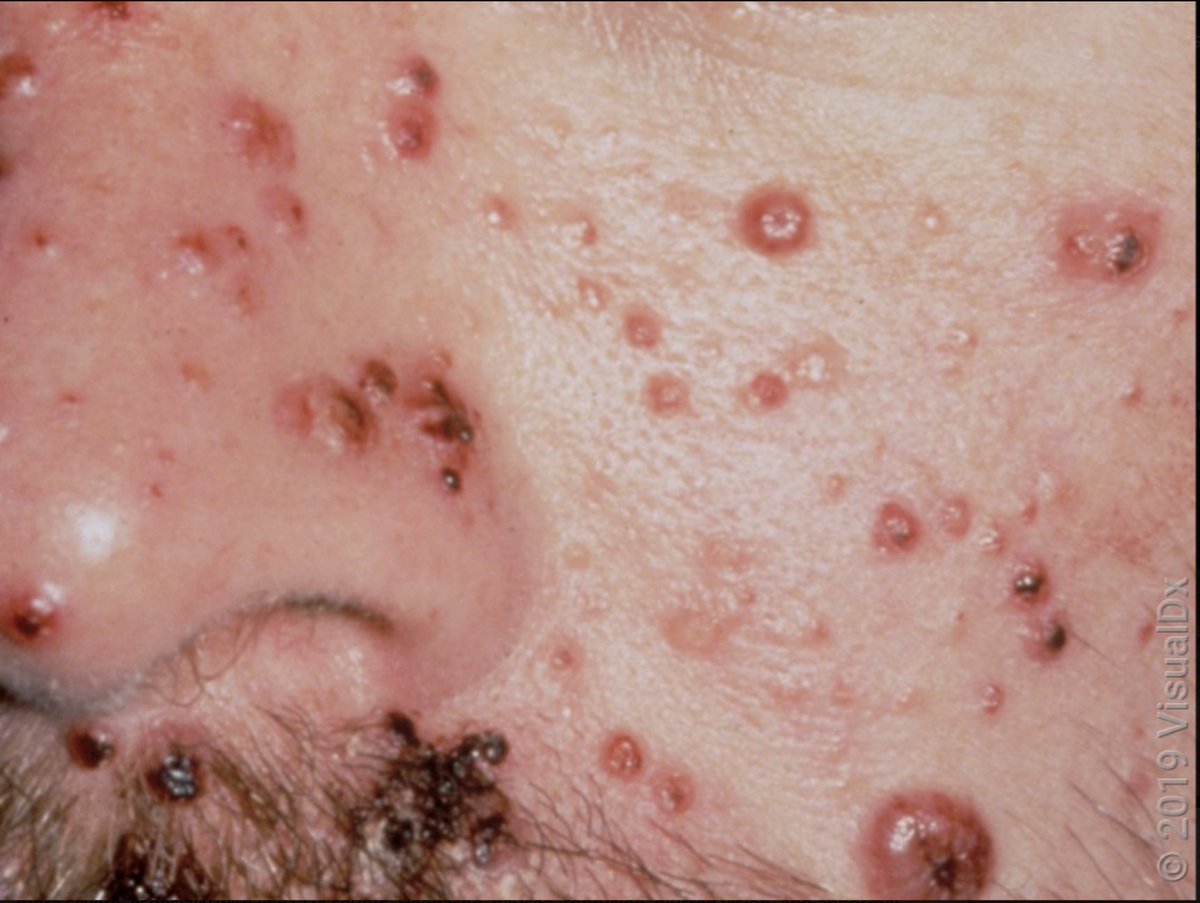
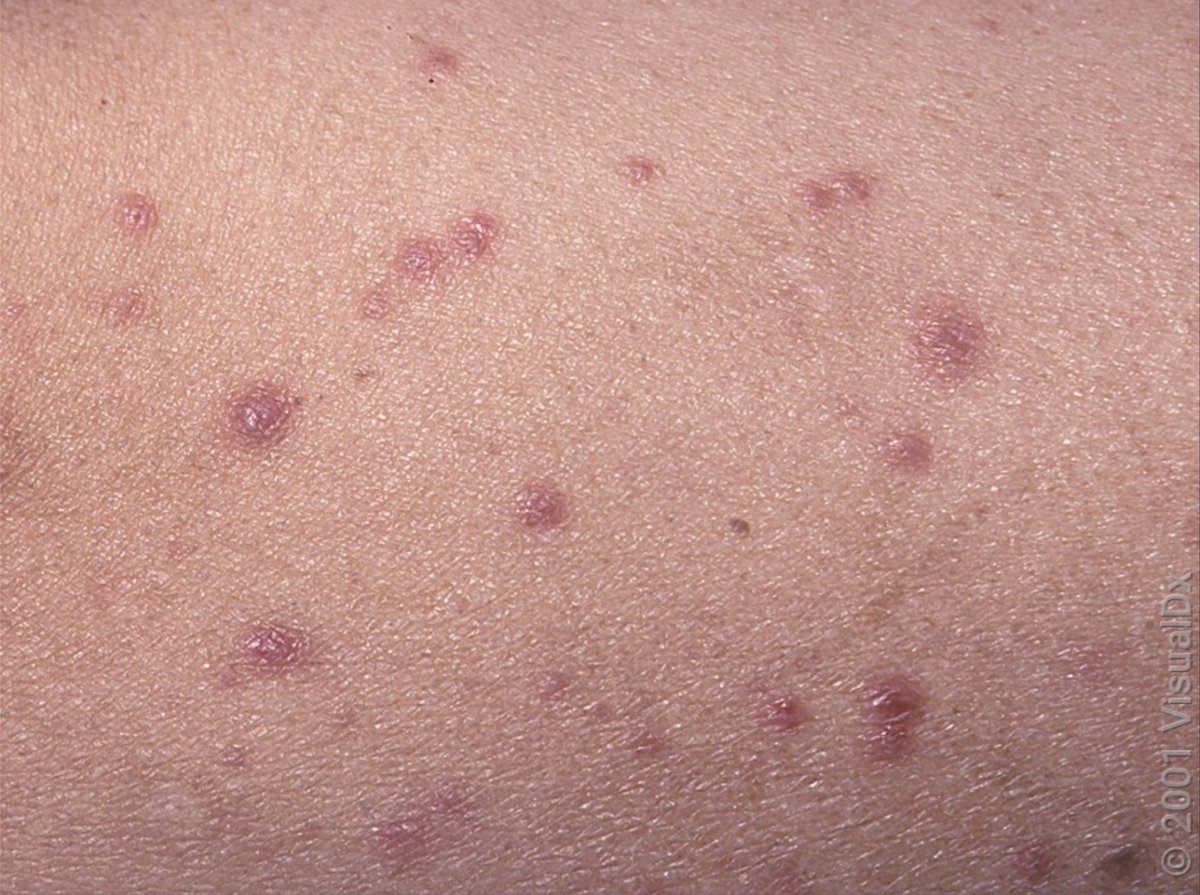
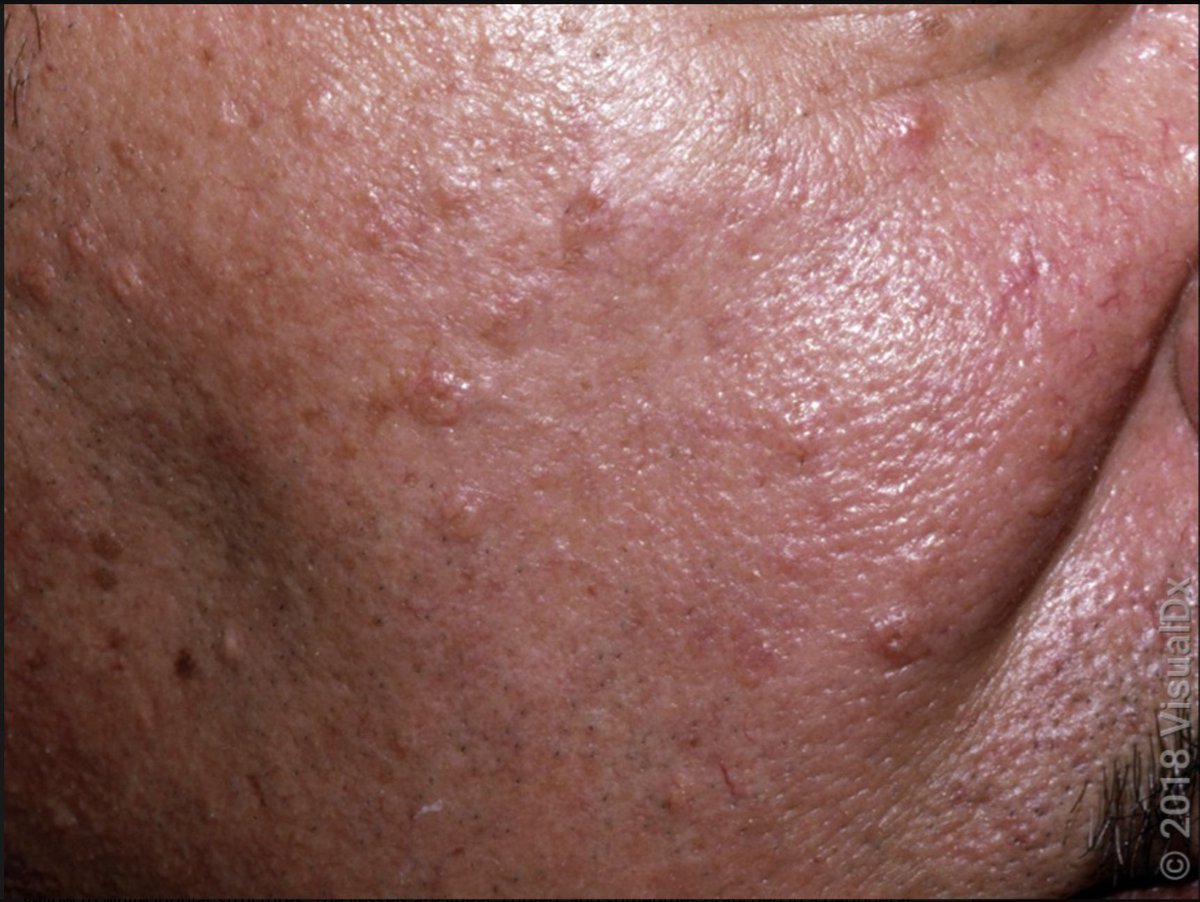 Well, the correct answer should be, "it depends."
Well, the correct answer should be, "it depends."


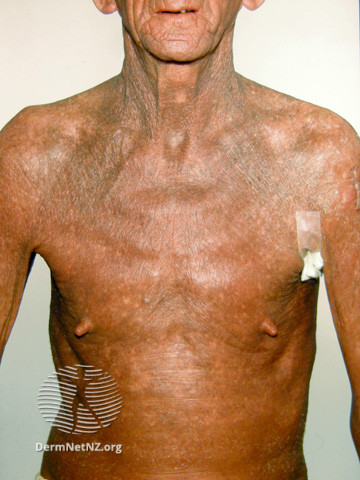

 Just a few years ago, Sezary Syndrome (SS) was thought to be the leukemic variant of Mycosis Fungoides (MF). We basically thought people had MF, it would keep getting worse, and then it would turn into SS.
Just a few years ago, Sezary Syndrome (SS) was thought to be the leukemic variant of Mycosis Fungoides (MF). We basically thought people had MF, it would keep getting worse, and then it would turn into SS.https://twitter.com/DrStevenTChen/status/1147926420468846592?s=20&t=97wFnOJX-F61l5EYZ1IoOQ


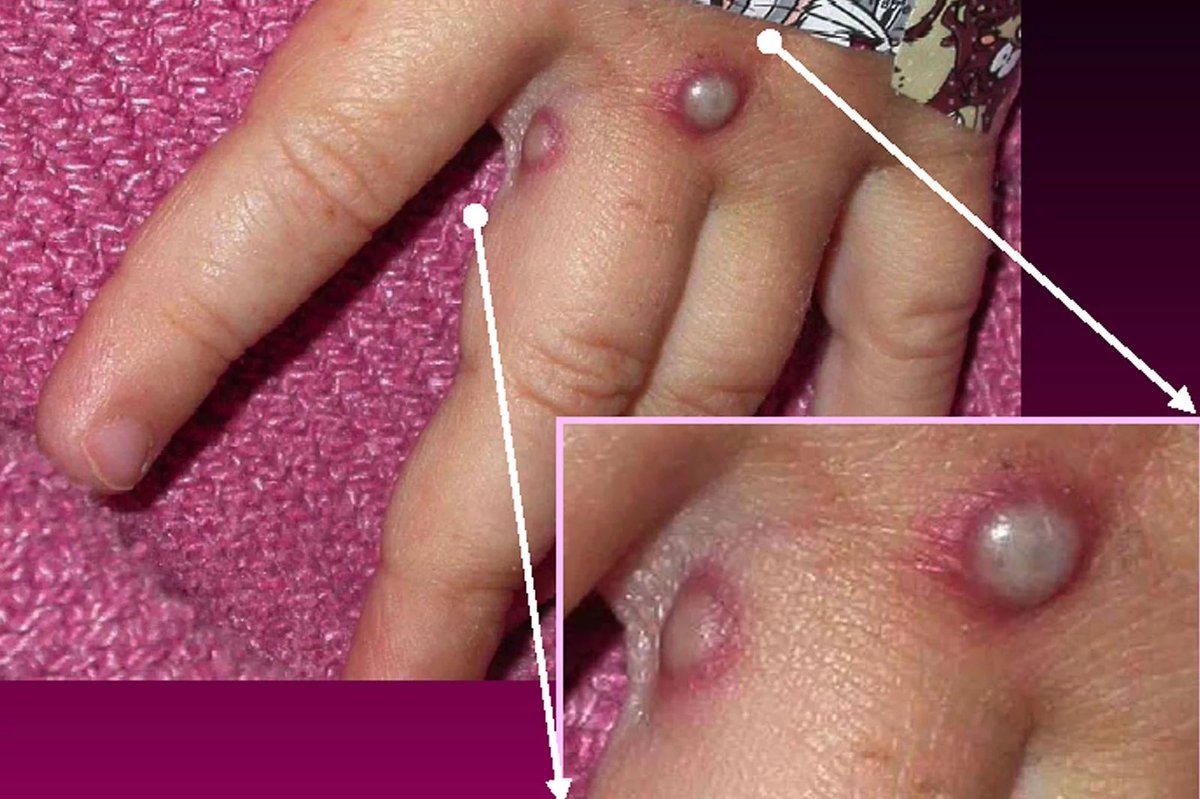
 Since #Monkeypox seems to transition from:
Since #Monkeypox seems to transition from:

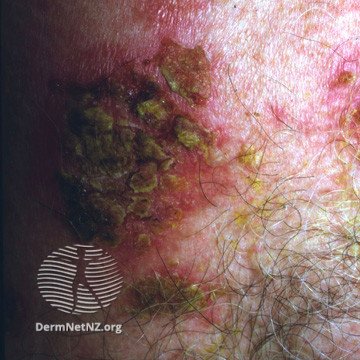
 2/
2/https://twitter.com/DrStevenTChen/status/1484569902744748032?s=20&t=UcJFMYPQV-6krKyEma748A

 2/
2/

https://twitter.com/DrStevenTChen/status/1180935098822201344?s=20

https://twitter.com/drsteventchen/status/1476268927722348544
https://twitter.com/DrStevenTChen/status/1444694854122938368?s=20

