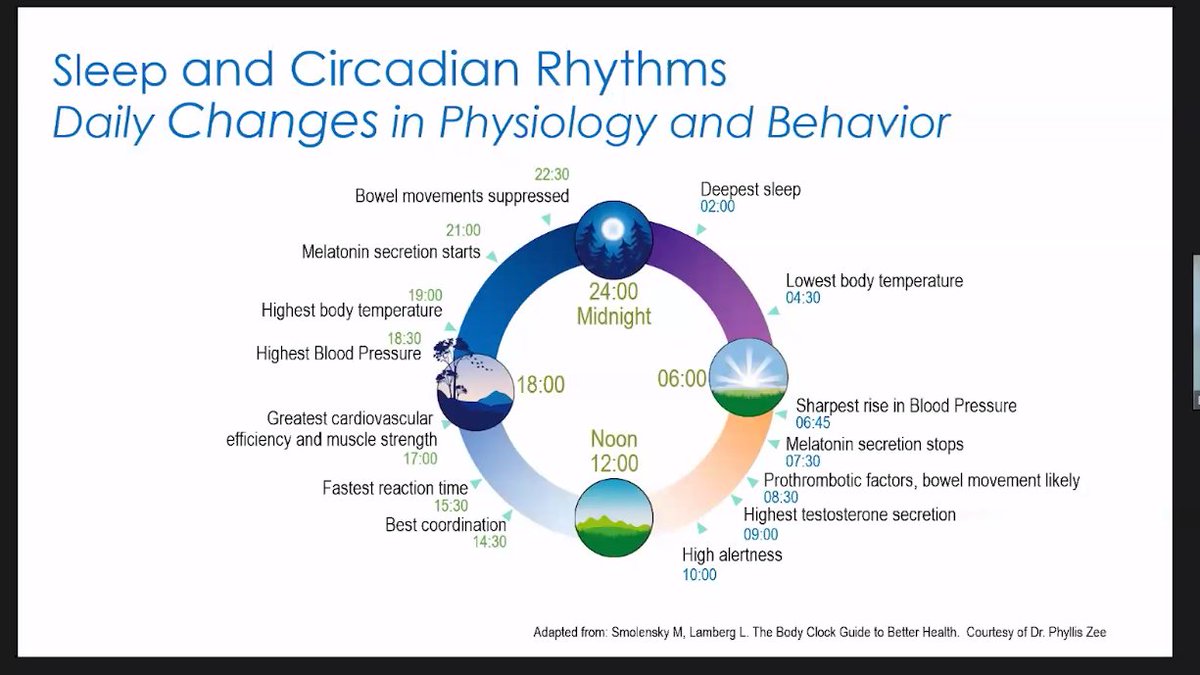
See talks sleep disruptions and fatigue: sleep disruptions cause issues with brain function, metabolism, increase oxidative stress, and inflammation. #fatigue (1/5) 
See talks sleep disruptions and fatigue: sleep disruptions cause issues with brain function, metabolism, increase oxidative stress, and inflammation. #fatigue (2/5)
Interestingly, fatigue and sleepiness are not necessarily even related. It’s refreshing to see these ideas teased apart. Feeling sleepy =/ fatigue as a symptom of disease. #fatigue (3/5) 

Interesting: someone with insomnia describes “wired but tired” … ‘exhausted but also like I’ve mainlined coffee’. Curious, #pwME and with #LongCovid … how many of you have sleep issues (insomnia, disturbed sleep, inverted or chaotic rhythm)? #fatigue (4/5)
”in a sleep clinic, if you’re not sleepy then we would say that you have fatigue. But we don’t measure fatigue. I would argue it’s important to differentiate.” (5/5)
Want to see the rest of the talks at this conference? Go here:
https://twitter.com/exceedhergrasp1/status/1442524343221698560.
• • •
Missing some Tweet in this thread? You can try to
force a refresh