
Researcher-Bioethics/Global Health/Policy; Adjunct Prof; Past Prez @IABioethics; Mentor @SangathIndia Bhopal; Dr. https://t.co/zu5UaKHVUY
How to get URL link on X (Twitter) App


https://twitter.com/QuintFit/status/1396822986997436431On 9 May, he became one of the youngest doctors to lose their lives to COVID-19.



 Source: cdsco.gov.in/opencms/opencm…
Source: cdsco.gov.in/opencms/opencm…

 The project is called DRISHTi (Developing capacity in health Research ethics Training) and the digital course will be targeted at health professionals as well as general public. The course is proposed to be 8-10 weeks long, completely digital in format and in the English language
The project is called DRISHTi (Developing capacity in health Research ethics Training) and the digital course will be targeted at health professionals as well as general public. The course is proposed to be 8-10 weeks long, completely digital in format and in the English language

 Dr T Jacob John also makes an argument in this regard, though also clarifying that there might have been some early safety data from those vaccinated in the phase 3 which is ongoing as well
Dr T Jacob John also makes an argument in this regard, though also clarifying that there might have been some early safety data from those vaccinated in the phase 3 which is ongoing as well 
https://twitter.com/RachnaDhingra/status/1345748641646923781This issue needs to be highlighted more as it shows us what poor oversight could mean, especially because we are now talking about expanded use of vaccines "in clinical trials mode" (not that I am sure anyone really knows what that means)

 Dr @RenuSwarup, Secretary @DBTIndia announces the renaming of the @THSTIFaridabad- @unescorcb cluster auditorium after Prof MK Bhan
Dr @RenuSwarup, Secretary @DBTIndia announces the renaming of the @THSTIFaridabad- @unescorcb cluster auditorium after Prof MK Bhan 


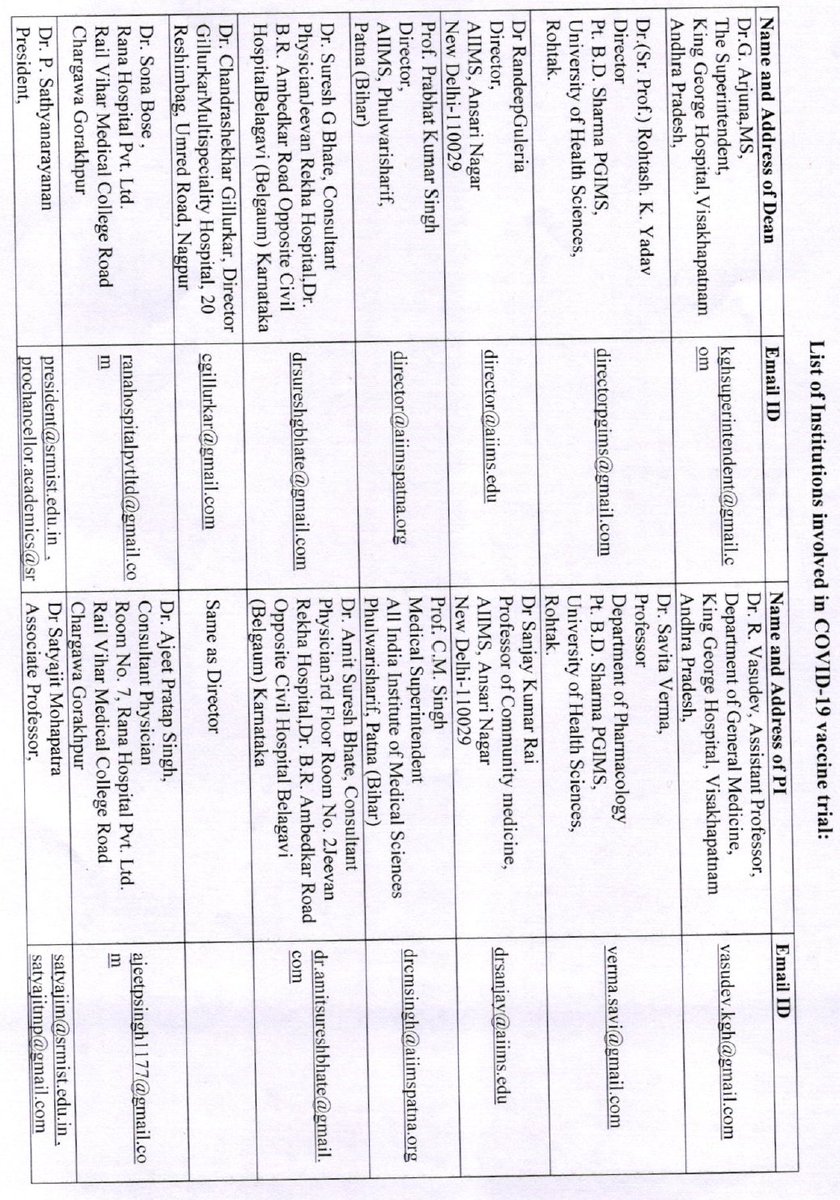
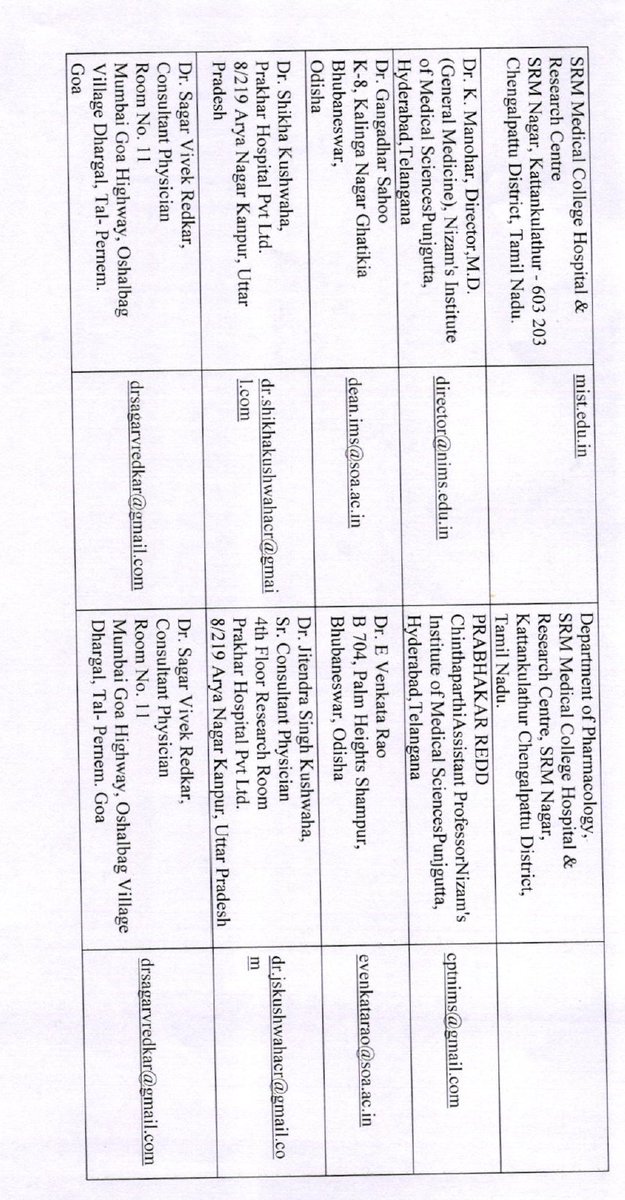 For a vaccine for which pre-clinical development is still ongoing, as per the letter itself, how can clinical trial recruitment be starting on 07th July?
For a vaccine for which pre-clinical development is still ongoing, as per the letter itself, how can clinical trial recruitment be starting on 07th July? 
 Related to this, the only information available in the public domain is this CTRI registration
Related to this, the only information available in the public domain is this CTRI registration 

 Equating the pandemic response to a war equates India’s healthcare workforce to members of the country’s Armed Forces. The same kind of stoicism and public silence that characterises our Armed Forces is now expected of physicians, nurses, CHWs and allied healthcare personnel.
Equating the pandemic response to a war equates India’s healthcare workforce to members of the country’s Armed Forces. The same kind of stoicism and public silence that characterises our Armed Forces is now expected of physicians, nurses, CHWs and allied healthcare personnel.
