Incoming #MedTwitter #Tweetorial #HemOnc #heme #hematology
- Foreground: change in urine color.
- Middleground: recent-onset anemia?
- Distant background: no known anemia.
What has been going on for the past year? Why has urine been darker this past week?
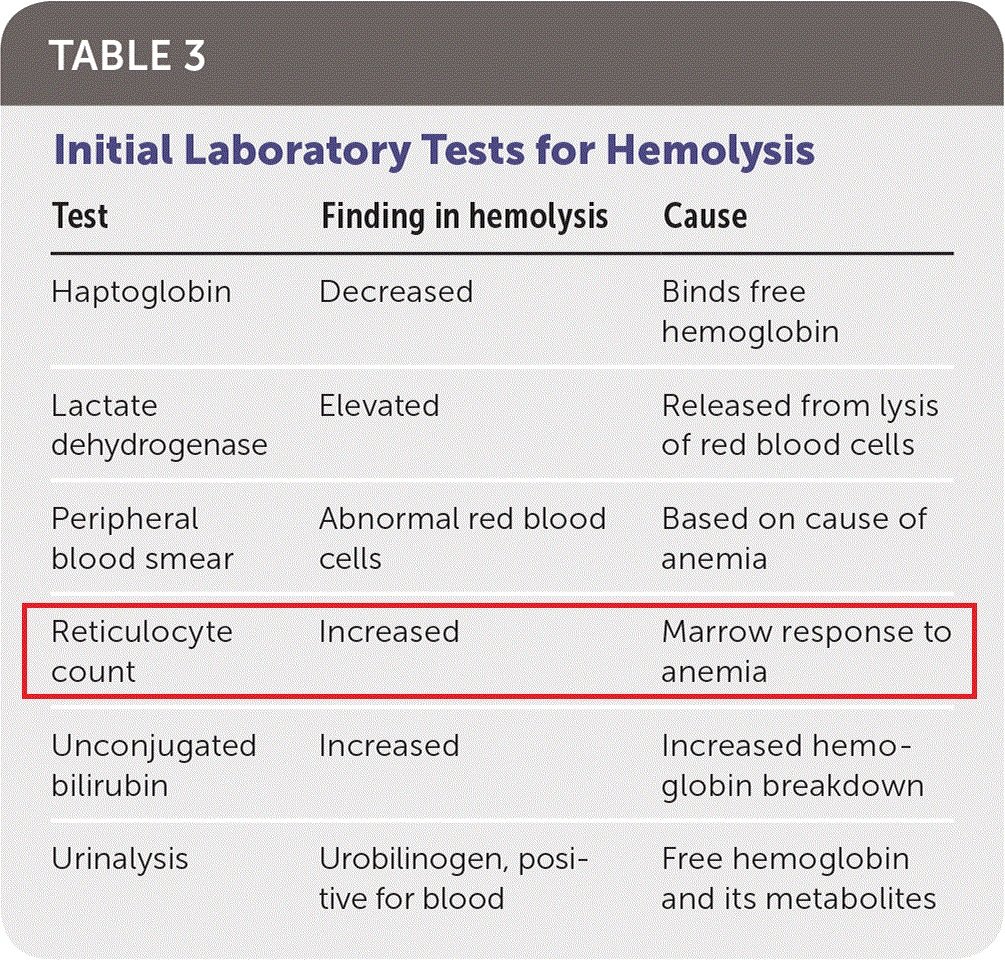
Labs: BMP normal. T bili 2.2 (D 0.7), D-dimer 1.8, fibrinogen 225, PTT 25.2, INR 1.42, CK 40, WBC 1.2 (24.7% N, 65% L, 0% E), Hgb 3.9, Hct 11.3, Plt 26.
More labs: MCV 107, haptoglobin<10, LDH> 2000, ferritin 506, TSAT 26%, reticulocytes 1.3%, RPI 0.14, peripheral smear with anisocytosis/some macrocytes/some elliptocytes.
In this case: RPI = (1.3 x (11.3/42))/2.5 = 0.14
You can use MDCalc to help with the process: mdcalc.com/absolute-retic…

Reticulocytosis (RPI>2) is a hallmark of hemolytic anemia (marrow responds to peripheral destruction of cells by⬆️reticulocyte production). Maybe pancytopenia holds the clue in this case?🤔
Direct Coombs test: negative/HIV 1/2 Ab + p24 Ag: negative/Folate: 11 (N: 7-31)/Copper, Zn: normal levels/ADAMTS13 activity>79%/PNH flow cytometry: negative
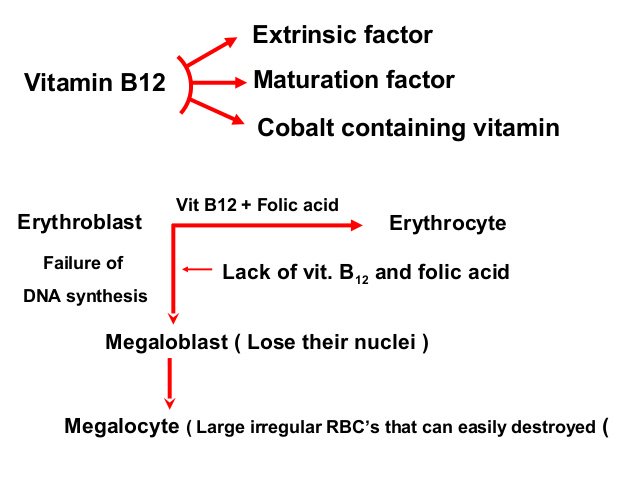
Vitamin B12 level was <150. Methylmalonic acid level was 64 (N<0.4).
Rapidly developing anemia = reticulocytopenia in the initial stages.
Gastrin: 108 (N: 0-115)/Anti-IF antibody: 2.4 (N<1.1)/Anti-parietal cell antibody: 33.8 (N<20).
He was diagnosed with pernicious anemia. Had a family history of auto-immune diabetes.
- While hemolysis is known to cause reticulocytosis (RPI>2), there are some exceptions: B12 deficiency (intramedullary maturation problem), chronic peripheral hemolysis with aplastic crisis, brisk hemolysis in the very early stages (bone marrow overwhelmed).
- A BMB (invasive) can be potentially avoided if anomalies respond to aggressive B12 supplementation
- shmabstracts.com/abstract/vitam…
- longdom.org/open-access/he…
- PRUTHI, R. K., & TEFFERI, A. (1994). Pernicious Anemia Revisited. Mayo Clinic Proceedings, 69(2), 144–150.