But what do they really mean?
Here we attempt a #tweetorial presenting a way of thinking about common patterns seen on lung ultrasound.
See table here for a summary, and thread below for details
#POCUS
1/
65 y/o f w HFpEF, COPD admitted 4 days ago with acute pancreatitis (now resolved). You are prepping her for discharge but she is now short of breath/hypoxic requiring 4 L O2.
2/
Net positive 4L. HR 88 SpO2 90% 4L BP 165/90 RR 22 T 99.8. WBC 22 (from 12 a day ago).
JVP not seen RRR, +S1/S2, 2/6 SEM
Bibasilar crackles, No LE edema. BNP 150.
3/
-COPD exacerbation
-PE
-Pneumothorax
-Fluid overload with cardiogenic pulmonary edema
-ARDS from pancreatitis
-Aspiration pneumonitis
-Hospital acquired PNA
-Atelectasis
4/
5/
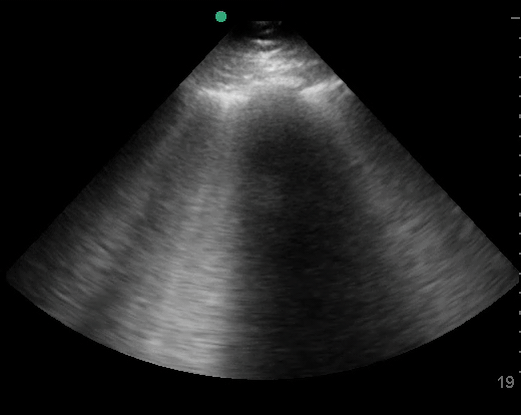
-A: air filled chest (ex: normal, COPD, PE, PTX, or non-pulmonary)
-B: interstitial edema or thickening (ex: CHF, ARDS, interstitial PNA, fibrosis)
-C: filled or collapsed alveoli (ex: PNA, aspiration, atelectasis, and more)
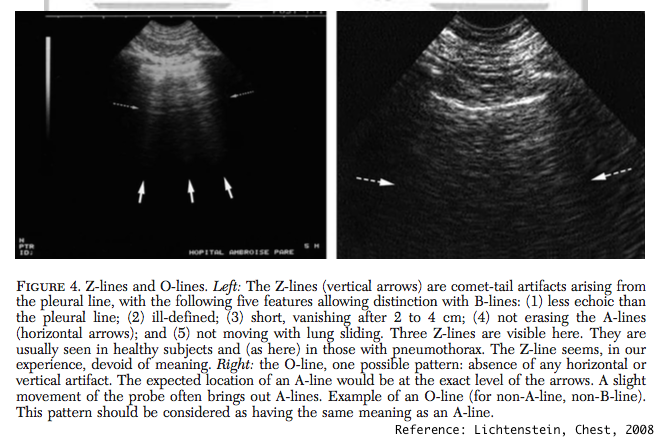
-O: Non-A non-B pattern: non-diagnostic
14/
Interested to hear other thoughts from #POCUS twitter on this!
15/