here are my tl;dw notes if you don't have the time to watch:
- asian response to pandemic was informed by their experience with SARS. already common practice to wear masks in public, knew how to rapidly test & trace, isolation protocol planned & ready; thus, better curve flattening over US
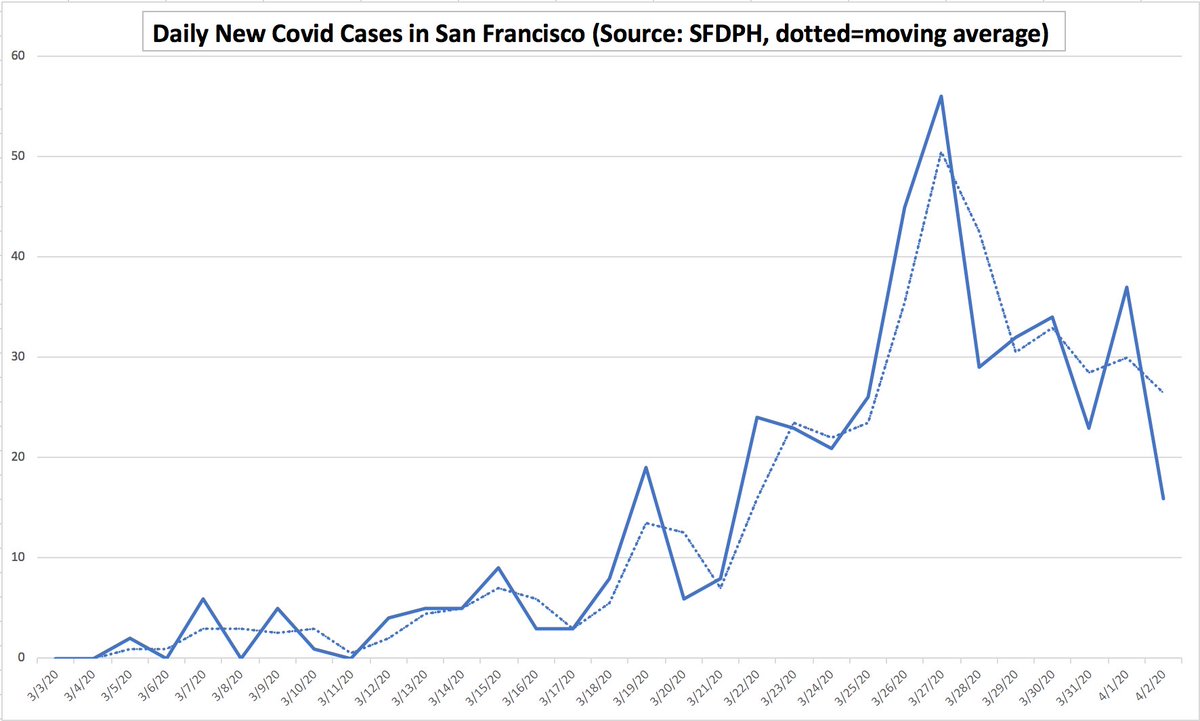
- key metric to watch is daily new cases per 1M pop
- china peaked at 10, spain steady over past week at 173, italy steady over past week at 100, US now at 90 rising every day (these are my calcs)
- definitely NOT seeing deaths in younger age groups
- US seeing more deaths in middle age groups likely due to sig higher prevalence of pre-existing conditions in US pop
- genetic analysis of virus in Bay Area patients indicates 3-4 unique strains.. Bay Area NOT just community spread but seems to have acquired virus from multiple land/sea/air vectors
- each action reduces transmission rates and R drops
- success in singapore,hongkong from combo isolation, testing, tracing, strategic antibody detection
- considers abbott and cepheid systems helpful in creating point-of-care <1 hr PCR detection (still hard to scale or address volume issues but helps in small hospital setting)
- sensitivity of PCR tests now measured based on swab type: oral 56%, nasal 76%, oral+nasal 84%
- sputum from lungs has highest viral content but hard to produce/isolate, thus double oral/nasal swab
- best case still 16% false negative w PCR
- taste and smell disorders in 34% of patients in a small study, mostly younger women and study was done later in disease course
- not clear how widespread smell/taste issues are at this point, mechanism not clearly understood
- anecdotally, smell/taste recovery likely
- ocular issues manifesting as conjunctivitis, WITHOUT co-infection typically, seen in about 32% of patients
- ICU mortality study comparison data interesting: china ~70%, US 48% -- better care, treatment, or ICU admission bias? is survival improving with learnings about care?
- can't draw any conclusions from published data on remdesivir at this point; 5 clinical trials underway -expecting readouts any day
- compassionate use program closed as expanded access program underway now for intubated patients w/o multi-organ failure
- most patients gets better and most patients see decline in viral load without treatment... the HCL series from France did not account for NO HCL as a treatment course
- 62 patient study showed 1-day reduction in fever/cough but generally this was not clear study
- hard to make any clear statement at this point on HCL -- good safety signals but no real data to draw conclusions at this point
- french study was people EXPECTED to do well so hard to say if HCL+zpak was useful
- big driver of COVID is immune-modulated inflammation - "cytokine storm"
- COVID-19 vaccine already being trialed
other q&a:
- yes, the general public should wear masks
- when do we stop isolation? need more testing - pcr and sero - to confirm de-isolation is viable
- if you have antibodies, it's not FULLY ANSWERED that you are immune, but some papers show that you can't be re-infected, w some anecdotal data of reinfection (unproven)
- virus itself not airborne, virus transmitted in droplet particles in the air and on surfaces
- treatment not needed with mild symptoms
- high-risk patients should consider HCL w tracking
course of disease:
- seeing cohort of patients do well in first week then rapidly progress in second week, dyspnea / breathing difficulties a good predictor here
- consistent observations with china, kirkland, italy.. older patients, not younger, co-morbities, not healthy; long ICU stay if admitted
- explains high ICU/ward ratio - high threshold for admission, longer time in bed vs ward not needing ICU simply leaving much quicker and not needing long care
- not seeing ventillator trade-off issues at UCSF today
- masking could lead to false sense of security (go outside more often than you should)