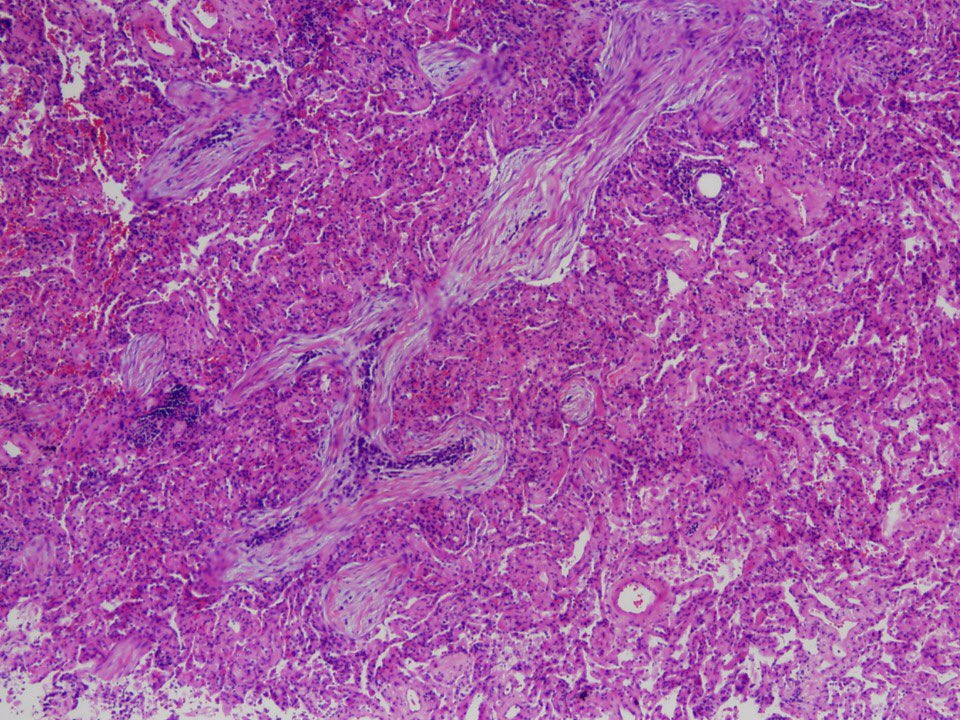
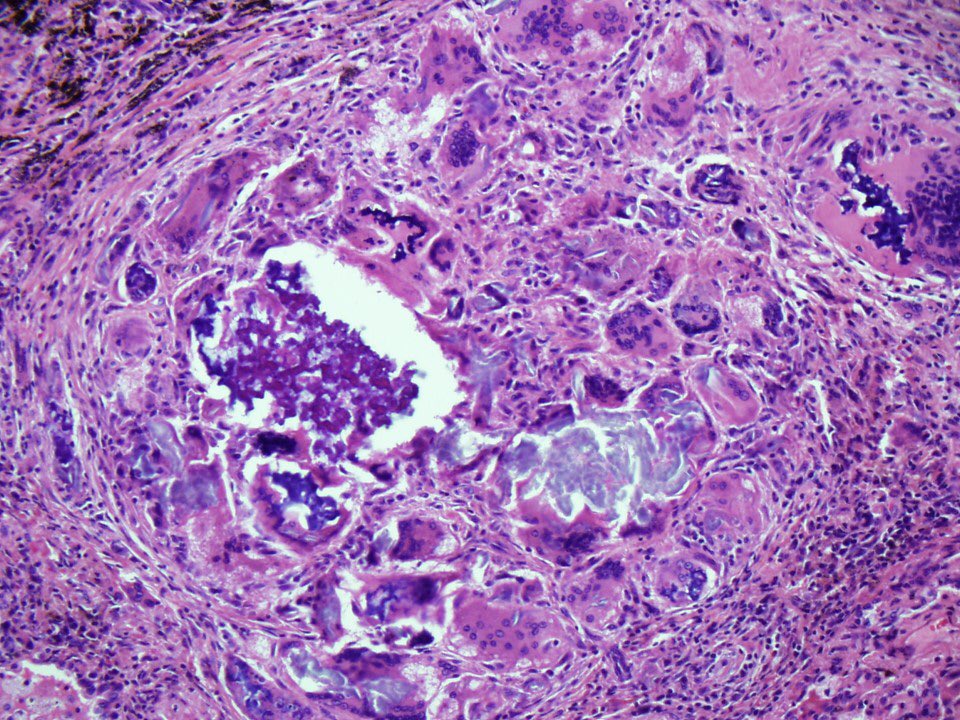
What happens after you inhale Histoplasma into your lungs? Is #histoplasmosis always a deadly disease?
Here’s a #tweetorial or #pathtweetorial
You are at risk if you live in the Ohio or Mississippi River valleys, go spelunking, or work with chicken coops
Many (maybe most) people who inhale Histoplasma remain asymptomatic. Many have symptoms that mimic “the flu” and are treated as such. Only a minority of immunocompetent folks are seriously and acutely ill at first exposure. This is called acute pulmonary histoplasmosis.
What do you think happens next in the vast majority of infected individuals?
You get sick, you get treated for the flu or common cold, you recover. This is what happens in the vast majority of people who get infected in endemic areas. They don’t even know it.
So how would you diagnose histoplasmosis at this acute stage?
Follow the thread...
First, you have to consider the possibility.
✅ maybe the patient’s friends who went spelunking also got sick
✅ the disease is more severe than the usual flu
✅ imaging is really weird
✅ hilar adenopathy
Serology or antigen testing can be diagnostic.
Acute histoplasmosis is very common but rarely serious enough to lead to a lung biopsy. We reported the lung pathology:
ncbi.nlm.nih.gov/pubmed/2035149…
✅ Inflammation rich in lymphocytes and histiocytes
✅ Tiny granulomas
✅ Necrosis
✅ Vasculitis mimicking LYG
✅ Bugs

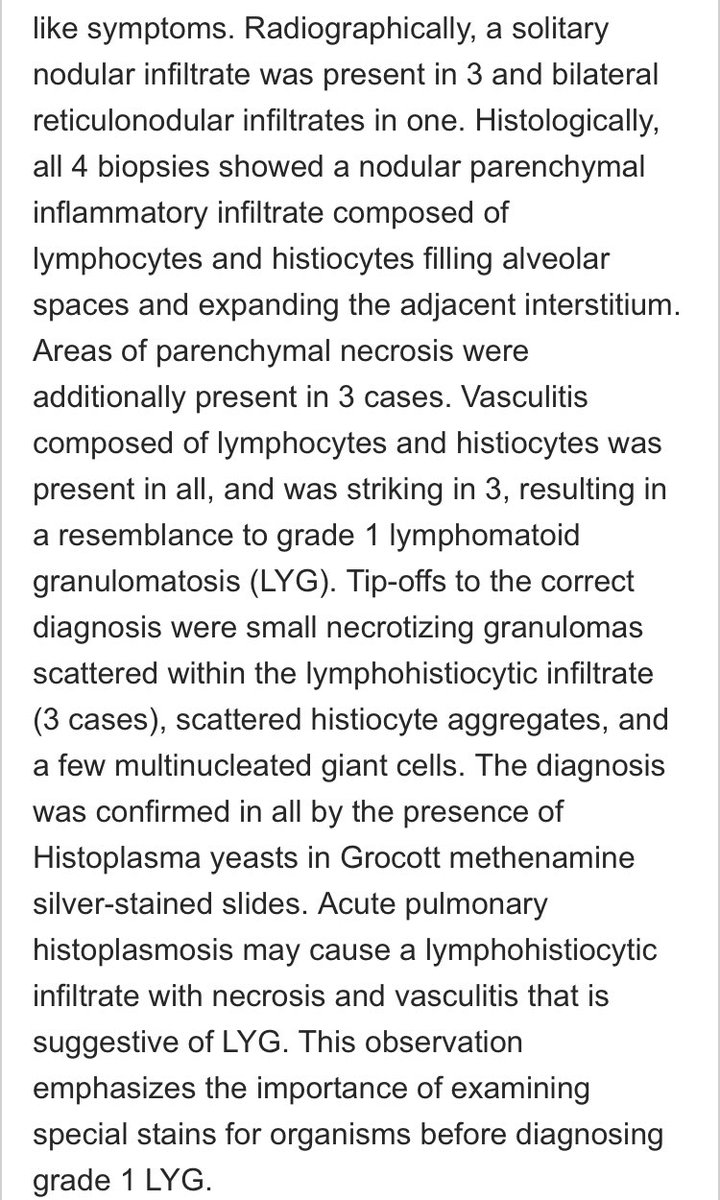
It is important to remember that “dissemination” of bugs throughout the body can occur at this stage but in immunocompetent people the bugs are destroyed wherever they go (Lymph nodes, Spleen, Liver, etc)
They are destroyed by necrotizing granulomas, the histologic hallmark
If you culture the infected tissues before the bugs are destroyed by an intact immune mechanism, cultures will be positive.
Once the bugs are dead, cultures will be negative. Histoplasma is unique in this regard; the bugs die once granulomas are allowed to do their job.
In contrast, bugs can be alive and viable within necrotizing granulomas in TB, NTM, cryptococcosis, etc.
If you culture an old TB granuloma, it might grow. If you culture an old Histoplasma granuloma, it will not grow anything.
ncbi.nlm.nih.gov/pubmed/1748816…
These necrotizing granulomas form nodules in various tissues. The necrosis eventually calcifies, providing radiologists a valuable diagnostic clue.
This is why calcified lung nodules are called “granulomas” on imaging, and splenic calcification is a clue to the diagnosis.
Another interesting twist in these necrotizing granulomas is that the bugs are dead but can be seen with a GMS (Grocott Methenamine Silver) stain within the necrosis. It’s like you’re seeing their skeletons. Sometimes MANY skeletons.
Pathologists who practice in histoplasmosis-endemic areas know that conventional tests suck at this stage. Cultures are negative. Serology has a low yield. It’s pathology or bust. Your pathologist MUST know how to approach granulomas.
archivesofpathology.org/doi/full/10.10…
The other common fungal stain (PAS) does not work well in this situation. Great for fungal hyphae and ok for disseminated histoplasmosis. NOT good for dead Histoplasma in necrotizing granulomas.
GMS ✅
PAS ❌
Next stage: the necrosis calcifies and you get calcified granulomas. Imaging picks up calcified nodules in lung, mediastinal nodes, spleen.
Interestingly, dead bugs can often be found in these lesions, like skeletons in a coffin.
Final stage in this saga: the bugs disintegrate completely and all that remains is a necrotizing granuloma. At this stage, bugs are undetectable, even with a GMS stain and the best pathologists. Not surprising that they do well even without Rx.
ncbi.nlm.nih.gov/pubmed/2355858…
In the lung, most necrotizing granulomas of this type are incidentally detected on imaging for other reasons. They can be spiculated and PET positive. They can grow and mimic malignancy. They might need to be biopsied or resected for diagnosis.
But they do NOT need Rx.
What happens in immunocompromised individuals is the exact opposite of what we’ve been discussing in this thread so far.
After the acute infection, dissemination occurs as expected, but the bugs are NOT killed off becayse the patient can’t form good granulomas...
Here’s what happens in the immunosuppressed:
✅ Histiocytes ingest Histoplasma but cannot kill it
✅ Yeasts proliferate unchecked within engorged histiocytes
✅ Histiocytes migrate and progressive dissemination ensues
This is disseminated #histoplasmosis
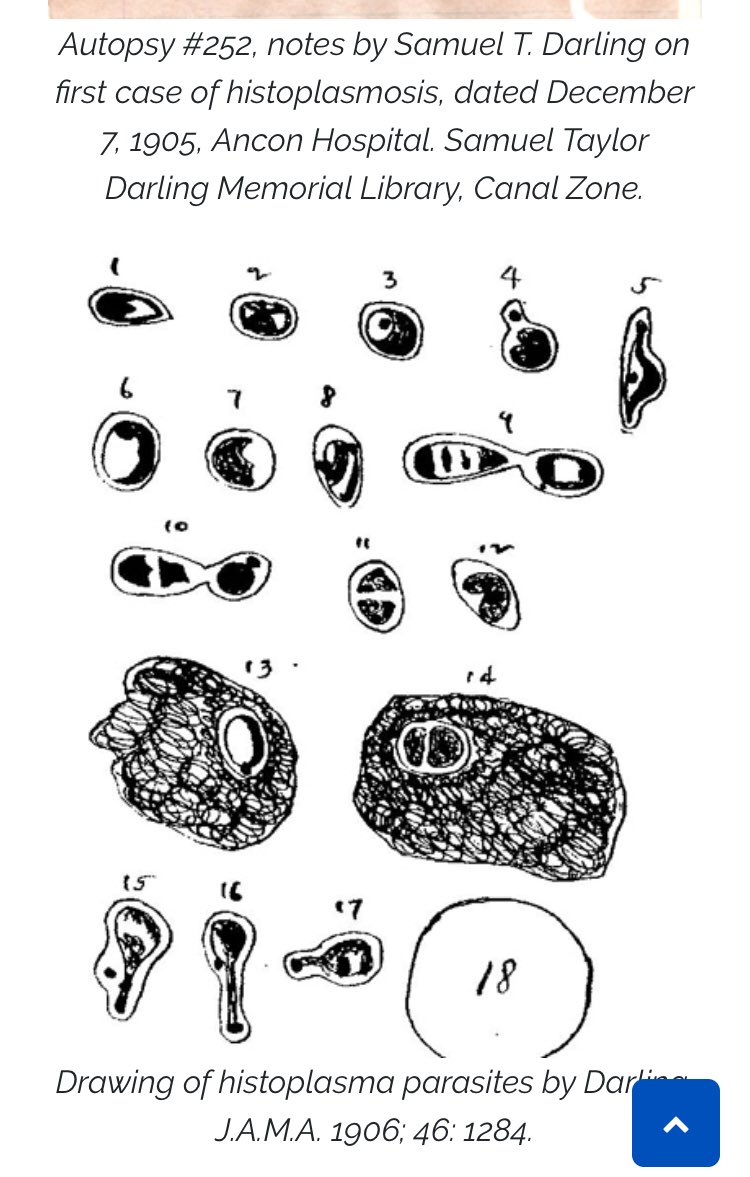
This produces the classic textbook histology of disseminated histoplasmosis that Samuel Darling recognized in 1906 and medical students learn in textbooks. This appearance is a marker of poor immunity and a predictor of disseminated disease.
In lung biopsies, the morphology shown in the previous tweet is a reliable indicator of disseminated disease, VERY different from healing/healed disease (necrotizing granulomas). Disseminated histoplasmosis needs urgent Rx.
ncbi.nlm.nih.gov/pubmed/2405472…
In disseminated histoplasmosis, organisms can end up almost anywhere, stuffed within their Trojan Horse histiocytes. Blood, bone marrow, spleen, liver, brain, adrenals, the list goes on.
Here’s a case in the blood posted by @AmyHDeekenMD
The diagnosis of disseminated histoplasmosis can be made by cultures, or positive serology, or blood or urine antigen testing, or pathology. All are valuable. Pathology can be quicker than the others.
The organisms are viable. The stakes are high.
Clinical “soft” clues to disseminated histoplasmosis?
🔴 immunocompromised state
🔴 fever
🔴 cytopenias
🔴 tiny bilateral lung nodules
🔴 elevated liver enzymes with high AST/ALT ratio
In mediastinal nodes, Histoplasma necrotizing granulomas can incite dense fibrosis. Too much of this, and you get a dense mass of fibrous tissue that compresses blood vessels and airways
It’s called fibrosing mediastinitis
In fibrosing mediastinitis you may or may not find the granulomas that triggered the fibrosis. It doesn’t matter if you do, because the organisms are invariably dead. Antifungals are NOT indicated.
Stenting the structures that are compressed is the only thing that works.
Let’s recap histoplasmosis Rx:
✅ Acute: no Rx for most
✅ Lung necrotizing granuloma: no Rx
✅ Fibrosing mediastinitis: no to antifungals, yes to stenting
✅ Disseminated disease: URGENT and aggressive antifungal Rx
✅ Cultures pos or immunosuppressed: should Rx
A note on microbiology: cultures are the gold standard for histoplasmosis, but are VERY slow. Can take 3-4 weeks to become positive. This sucks for sick patients. Biopsies give you results in 1-3 days.
Classic finding: “tuberculate macroconidia”
What are the cardinal features of Histoplasma on the GMS stain?
✅ smallest of the 4 major fungal yeasts
✅ round to oval
✅ narrow based budding
✅ yeasts are uniform in size
Most similar: Cryptococcus, Pneumocystis
Leishmaniasis can enter the differential for disseminated histoplasmosis. These are helpful:
✅ Endemic area very important
✅ Lung almost never leishmaniasis
✅ GMS pos in Histo, negative in Leish
✅ “kinetoplast” seen in Leish not in Histo
I hope this long thread didn’t drive you 🦇💩 crazy (🦇💩 is a source of histoplasmosis, by the way 😉). Thanks for staying till the bitter end.
#Histoplasmosis has many faces and is a fascinating disease.
🔴 end of #tweetorial 🔴