For my first #Tweetorial, I will start with a question:
Which of the following medications from the SGLT2 inhibitor class have been shown to decrease cardiovascular morbidity and mortality?
#Diabetes #EndoTwitter #MedEd #MedTwitter #DM2 #T2D #CardioTwitter
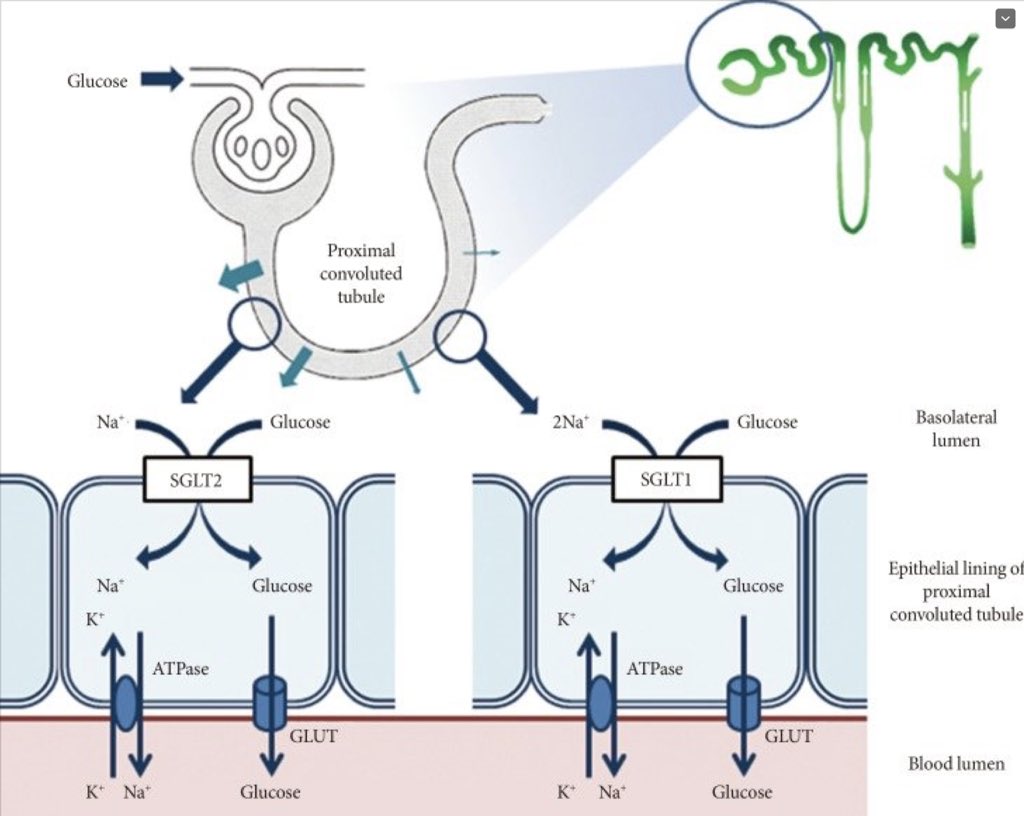
SGLT2 inhibitors block glucose reabsorption
➡️renal glucose excretion
➡️glucose levels⬇️
Because this has nothing to do with insulin, they usually don’t cause hypoglycemia or weight gain.
Actually, because of the osmotic diuresis, they decrease blood pressure & weight.
The EMPA-REG from @Boehringer & @LillyPad looked at 7K patients with DM2 and CVD, randomized to EMPAGLIFLOZIN or placebo. No surprise, these patients were also on many other meds for HTN, lipids, & DM (incl. metformin & insulin).

DECLARE-TIMI trial from @AstraZeneca & @BMSNews also looked at high-risk patients w/ DM2 & with CVD or at risk for CVD. Patients were randomized to DAPAGLIFLOZIN or placebo.
Important to note that fewer patients here had established CVD compared with the other 2 trials.

So, back to original question:
Which of the following #diabetes medications have been shown to decrease cardiovascular morbidity & mortality?
#EndoTwitter #MedTwitter #MedEd #CardioTwitter #DM2 #T2D