#CELLULITIS - a #tweetorial/#medthread!
#MedEd #FOAMEd #dermtwitter #medtwitter #derm #dermatologia #dermatology PC:@dermnetnz
1/
3/
7/
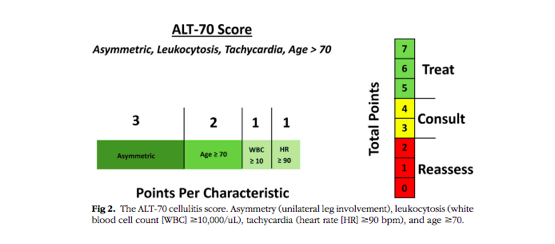
Asymmetry: 3 pts
Age>70: 2
WBC>10: 1
HR> 90: 1
5-7 pts: treat as cellulitis
3-4 pts: #derm consult
1-2: reassess
Great work from @AMostaghimi & others - jaad.org/article/S0190-…
8/
9/
10/
11/
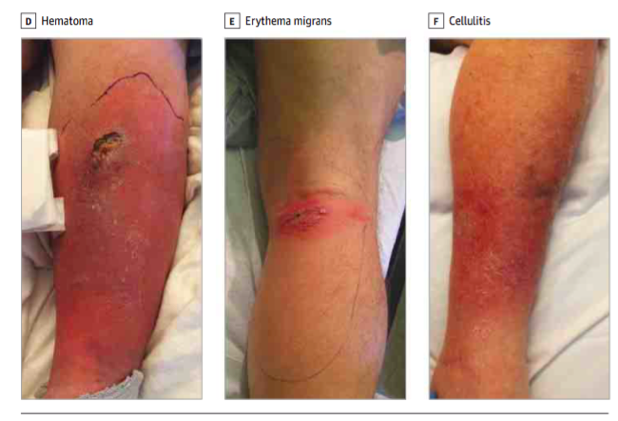
12/
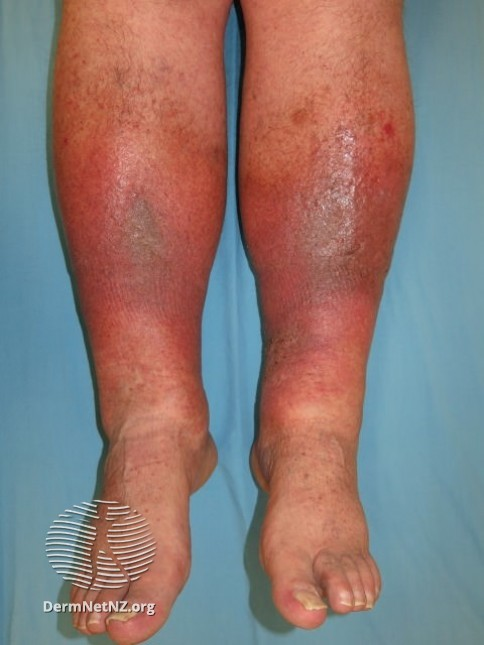
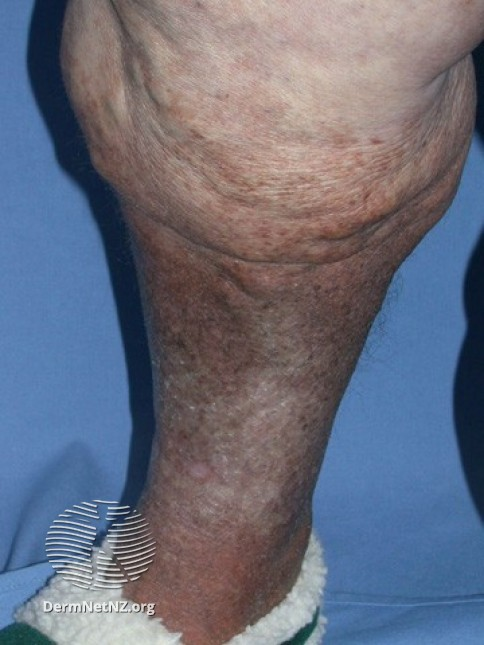
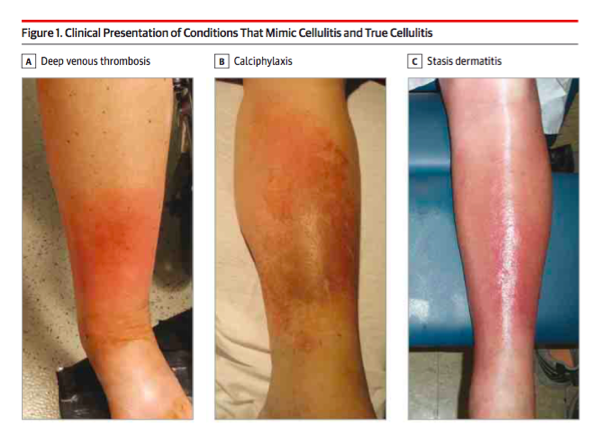
What do you think would happen if we gave these stasis patients some IV abx & admitted them?
13/
14/
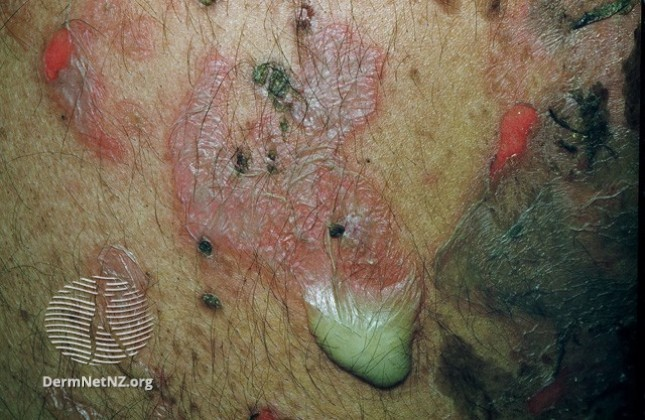
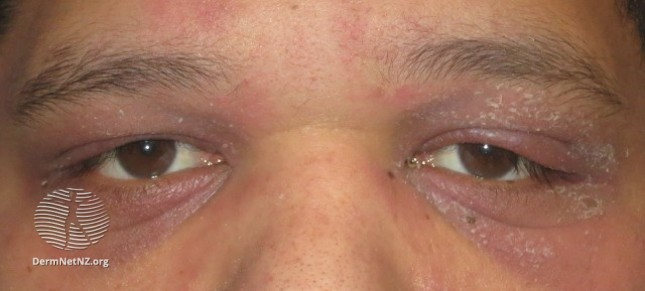
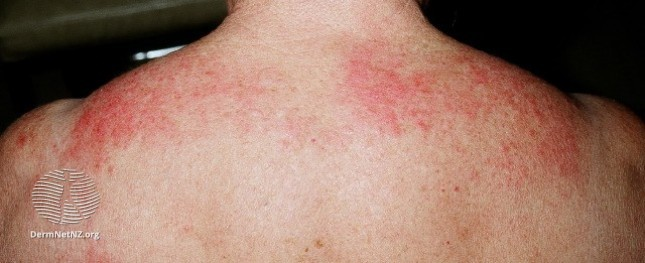
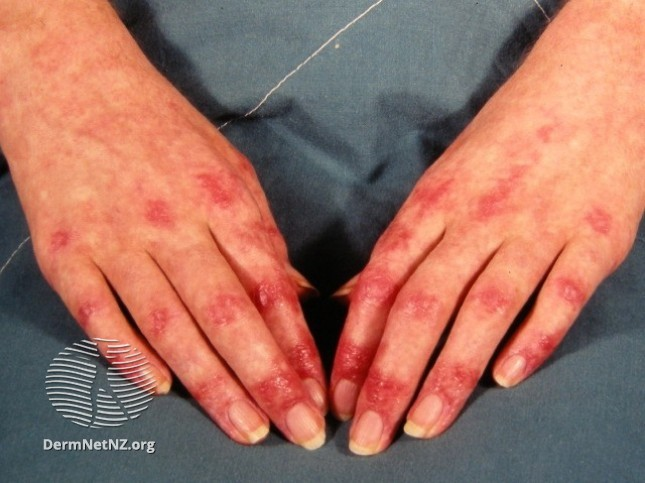
- Cellulitis: usually unilateral, painful, red, swollen, & warm
- It's a clinical dx. ALT-70 can help.
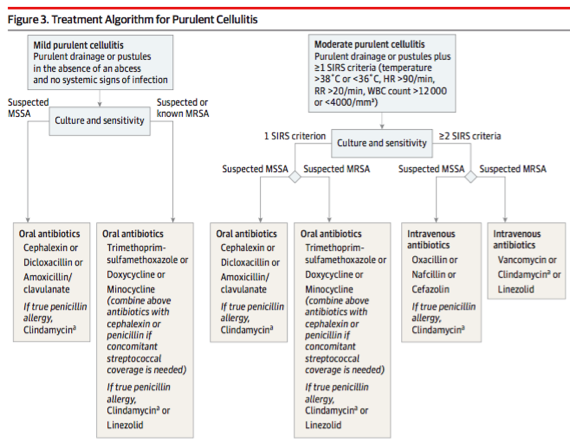
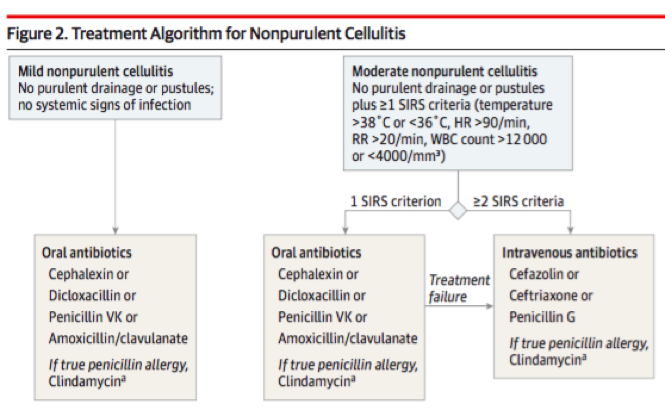
- If pt isn't sick: non-purulent ->oral MSSA/strep coverage; Purulent-> think MRSA.
- If no response, reconsider dx. IV abx can be tried.
Thanks for tuning in!
17/17