Hi hi hi. We see lots of red flags on a daily basis when we review labs.
One thing we see commonly is #lymphopenia. Should we care? When can we dismiss it and when should we work it up?
Let’s find out.
#MedEd #MedTwitter #IDTwitter #Tweetorial #oncology
- Lymphopenia assc w/ ⬆️risk of sepsis
- More common in elderly and w/ co-morbidities
- lymphs account for 20-40% of WBC, may go unnoticed when WBC checked w/o diff
- Primary- recurrent infxns in kids, CVID in adults
- Secondary-⬇️production; ⬆️destruction; hiding in tissue
What is the most common cause of lymphopenia in hospitalized patients?
In a large case series of 1042 hospitalized patients, lymphopenia was due to:
- bacterial or fungal sepsis (24%)
- recent surgery (22%)
- #malignancy (17%)
- #corticosteroid treatment (15%)
A low count persisted beyond six months in 6% patients.
ncbi.nlm.nih.gov/pubmed/9145181

After reviewing several articles, I compiled a table with common causes of lymphopenia, I hope this is helpful for others. There are too many causes to be all inclusive.
I want to highlight that one of the most common causes of lymphopenia world-wide is #malnutrition.

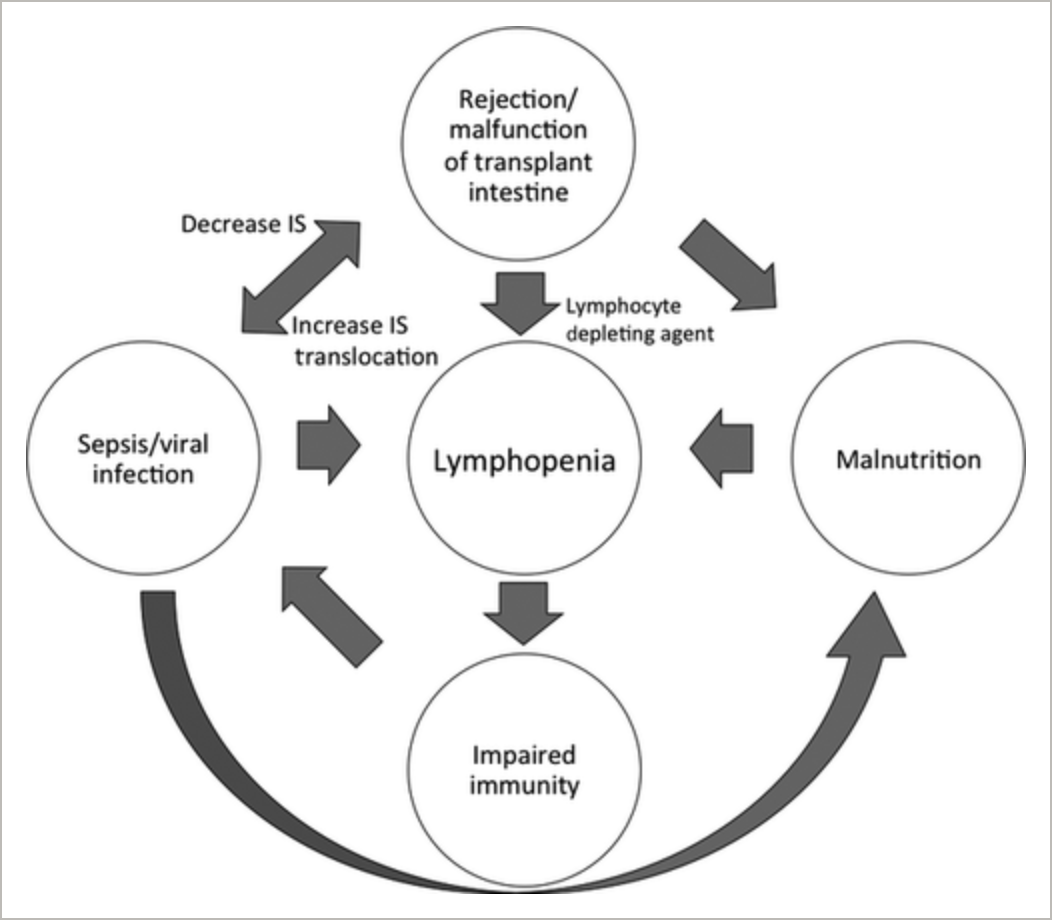
Lymphopenia can be both the cause and result of severe systemic diseases. This beautiful flow diagram is taken from an intestinal #transplantation journal, but the framework can be applied to other disease processes. #TxID
ncbi.nlm.nih.gov/pubmed/26095310
Now, changing gears to sepsis immunology.
What specifically about sepsis and lymphopenia leads to increased mortality?
Although a massive loss of lymphocytes (both T and B) occurs at the onset of sepsis, its PERSISTENCE correlates with ⬆️mortality
Lymphopenia is caused by apoptosis mostly.
Also there is a ⬇️ number in circulation as lymphs go to inflamed tissue.
ncbi.nlm.nih.gov/pubmed/31630991
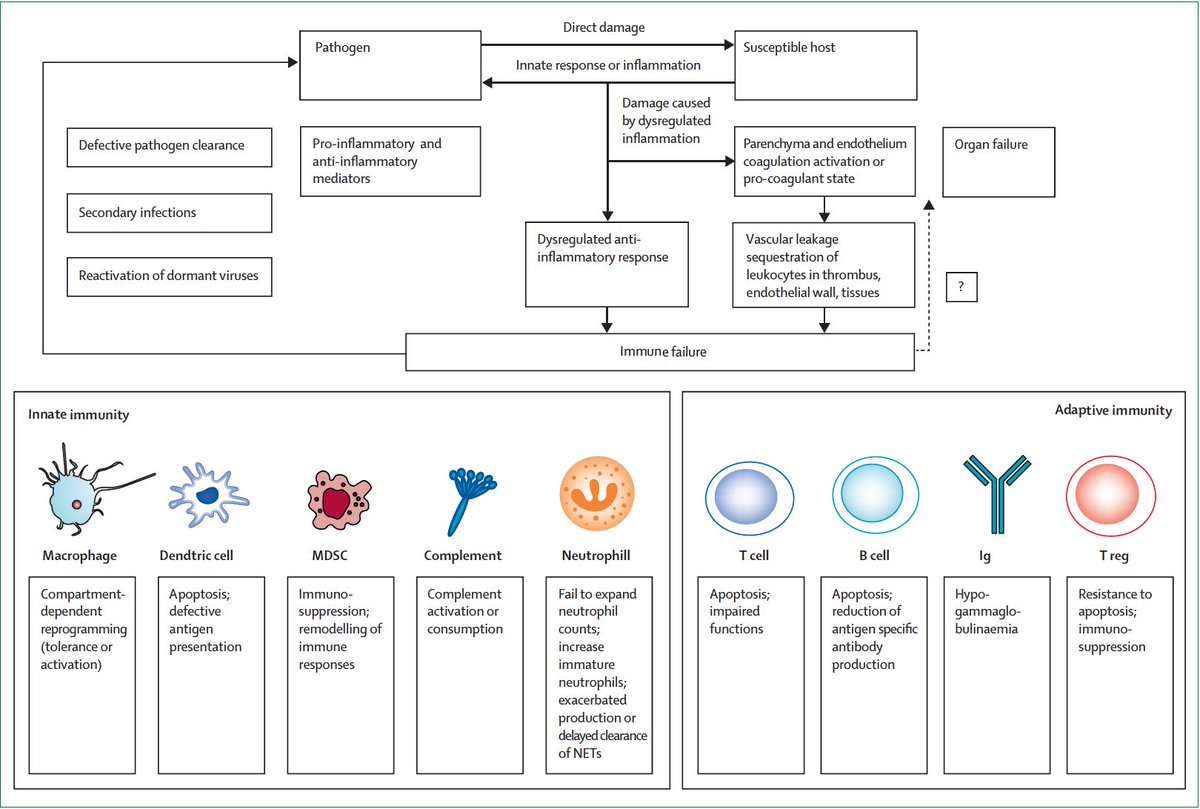
Pathogen & damage assc molecular patterns recog by TLRs➡️inflamm
W/ sepsis, dysreg host response➡️organ dysfxn & system activation (endothelium, complement➡️procoag state)
Loss of WBC and loss of blocking excess inflamm ➡️profound immune failure
ncbi.nlm.nih.gov/pubmed/31630991
#autoimmune disease can be induced by lymphopenia➡️expansion of autoreactive T cells
IL-7 can bind to IL-7R and⬆️signaling (anti-apoptotic pathway)
Seen in #lupus! Lymphopenia can be manifestation of disease activity & predictor of #SLE flares
ncbi.nlm.nih.gov/pubmed/27343993
With respect to labs and other studies, you should let the history and exam guide what to order.
You can use the following table to help, though not all the tests listed should be ordered to every patient...
other than #HIV of course!

Would love to hear feedback and see how others approach lymphopenia. @Anand_88_Patel @ShreyaTrivediMD @DxRxEdu @gradydoctor @tony_breu @Sharminzi @sargsyanz @LekshmiMD @rabihmgeha @DrPoorman @medrants @aoglasser @cjchiu @DRsonosRD @COREIMpodcast @thecurbsiders @CPSolvers



