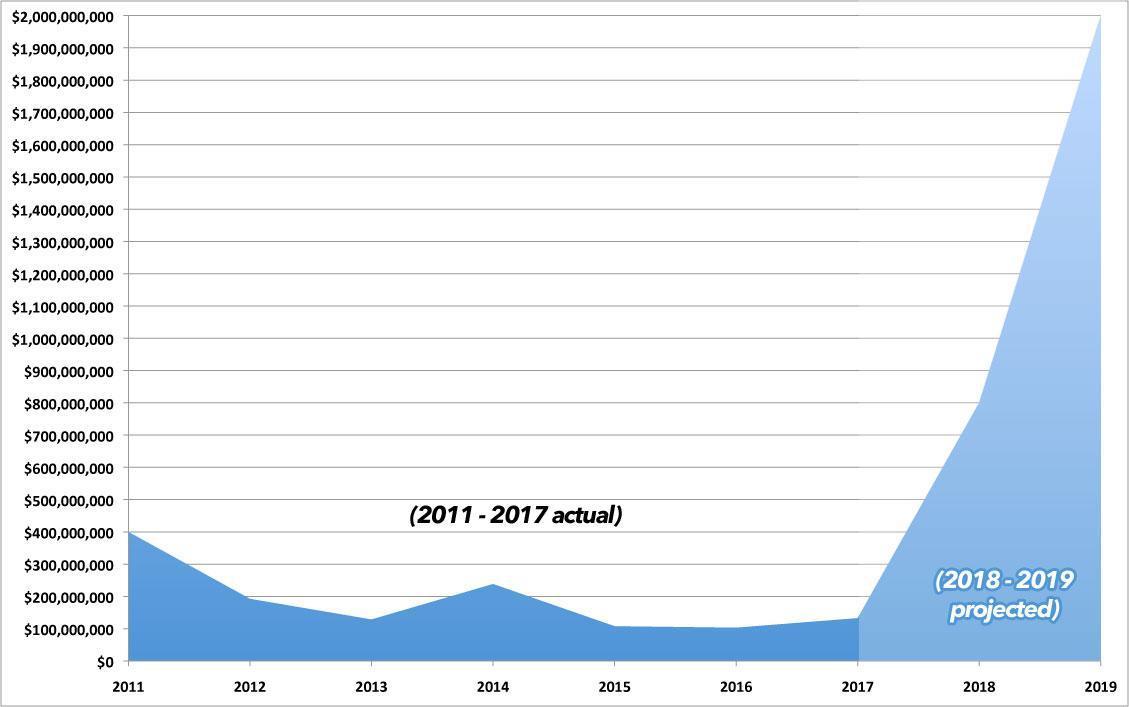
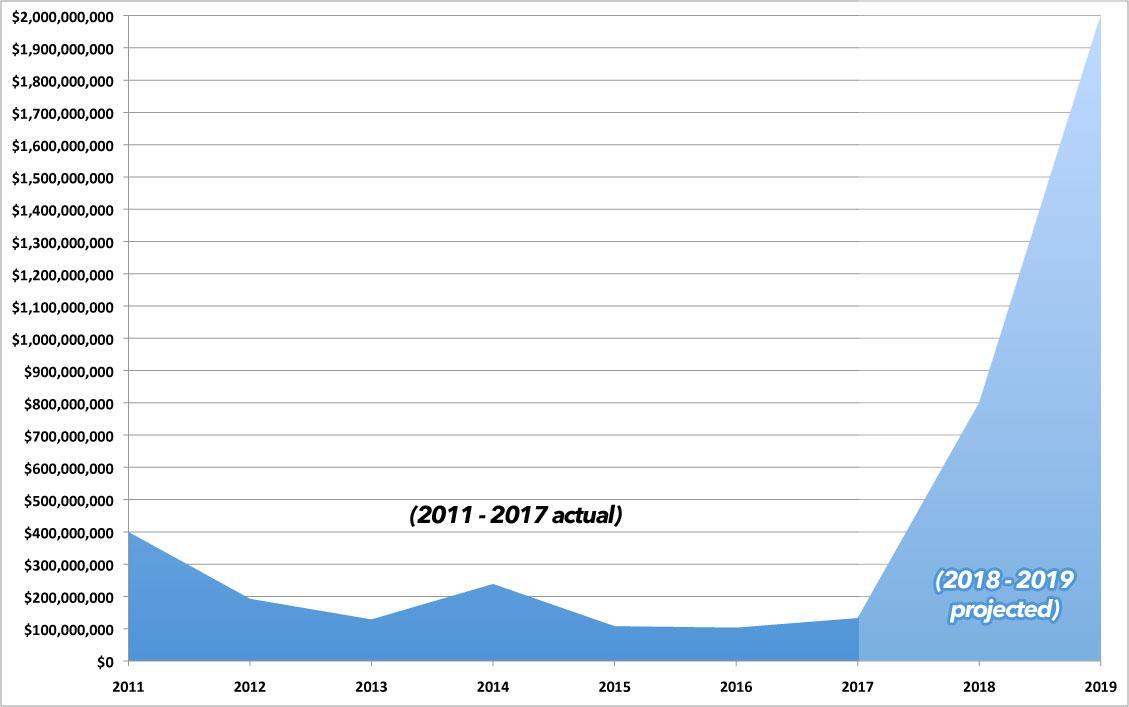
So, if they bring in $100M in premiums & only pay out $75M in claims, they have to rebate $5M. 2/
acasignups.net/19/08/29/impor…
acasignups.net/19/09/11/maine…
12/
13/
14/
15/
16/
acasignups.net/19/09/11/kentu…
Individual market enrollees of Blue Cross should keep an eye out next year, however.
acasignups.net/19/09/10/no-lo…
19/
20/
acasignups.net/19/09/11/monta…
21/
⚠️ IMPORTANT: THIS IS BY NO MEANS GUARANTEED. They might not have to pay back a dime.
23/
My projections for the *2019* MLR rebates (which will go out *next* August/September) are VERY crude and may be missing some critical wonky data like Risk Adjustment transfers, etc. Please consider them *guidelines only*.
OK, moving on…
24/
25/
Keep an eye on Highmark next year, however…they hovered around the 80% threshold in 2017 & 2018.
26/
acasignups.net/19/09/10/exclu…
27/
28/
31/
acasignups.net/19/09/10/exclu…
32/
33/
DC’s *total* Lg. Group plan enrollment is nearly as large as their total population. Huh.
34/
acasignups.net/19/09/09/exclu…
35/
acasignups.net/19/09/11/exclu…
36/
for his help with this mystery and some other MLR insights:
insure.com/companies/unit…
37/
Keep an eye on BCBSSC next year, though!
38/
acasignups.net/19/09/10/exclu…
39/
NEXT year, however, could be VERY different: Up to $40 million:
acasignups.net/19/09/13/washi…
40/
378 individual market enrollees should get…$22,400.
acasignups.net/19/09/11/louis…
41/
acasignups.net/19/09/11/maryl…
42/
Keep an eye on BCBS of Michigan/Blue Care Network next year!
(This data *was* an ACASignups exclusive at the time I posted it…)
acasignups.net/19/09/07/exclu…
43/
Individual Market? Just $83,000.
acasignups.net/19/09/11/calif…
44/
45/
First, large group policyholders will receive $24 million in rebates; on the individual market, it’s just $87,000.
acasignups.net/19/09/11/new-y…
46/
47/
48/
(This year, the only reason those 60,000 NY residents are getting their $1.46 apiece is due to the extra 2% threshold.)
49/
Keep an eye on Buckeye Community next year!
acasignups.net/19/09/12/ohio-…
50/
All told, $5.3 million in MLR rebates.
acasignups.net/19/09/11/exclu…
51/
(remember, that’s an *average* only).
$2.4 million total.
acasignups.net/19/09/11/iowa-…
52/
Industry-wide? $16 million.
acasignups.net/19/09/12/oklah…
53/
That means each recipient will get over $200 on average.
acasignups.net/19/09/13/utah-…
54/
acasignups.net/19/09/10/no-lo…
Industry-wide total: $19.5 million.
55/
acasignups.net/19/09/09/exclu…
56/
acasignups.net/19/09/08/exclu…
57/
acasignups.net/19/09/09/exclu…
Grand total: $19.4 million
58/
Industry-wide total: $16.2 million.
acasignups.net/19/09/09/exclu…
59/
Yep, that’s *$580* apiece on average.
acasignups.net/19/09/11/new-m…
60/
61/
62/
It’s being divided among 580,000 people, however, so the per-person average is just $36.
Group market rebates bring the total to over $107 million, though.
acasignups.net/19/09/07/exclu…
63/
Between Celtic and “Matthew Thornton”, 65,800 enrollees are getting over $24 million in rebates.
acasignups.net/19/09/11/new-h…
64/
acasignups.net/19/09/11/misso…
65/
IF ACCURATE, however…HOLY CRAP: $25.5 million being paid out to just 17,000 enrollees…for a per-person average of $1,476!
acasignups.net/19/09/11/kansa…
66/
acasignups.net/19/09/11/missi…
67/
There’s something else VERY important here, however…
acasignups.net/19/09/11/massa…
68/
That’s right…health insurers have to operate on a 12% *gross* margin (vs. the ACA’s 20%).
And yet MA still has the *lowest* ACA exchange premiums of any state!
69/
MA seems to counter this claim completely??
70/
$50 MILLION to 56,000 people…for a per-person average rebate of $889 apiece!!
More stunning: HMO Minnesota enrollees will avg. $1,523, proving Kansas’ numbers could be real.
acasignups.net/19/09/11/minne…
BlueCross BlueShield of TN and Cigna Health & Life are paying out nearly $57 million to 174,000 enrollees.
acasignups.net/19/09/13/tenne…
73/
REMINDER: If the #ACA is struck down by the GOP’s #TexasFoldEm lawsuit, those rebates would be gone.
acasignups.net/19/09/07/exclu…
74/
At $69.5 million, the Keystone State doesn’t have the highest *total* 2018 Indy Market rebates (it’s in 4th place), but check out HMO of NE PA’s per-enrollee average.
Go ahead, I’ll wait.
acasignups.net/19/09/13/penns…
75/
Not only is HCSC (Blue Cross Blue Shield of TX) paying out $75 million in rebates (the total w/other carriers is $80.3 million), check out the POTENTIAL rebates *next* year.
acasignups.net/19/09/13/texas…
76/
$92.3 million from Health Net of AZ, or $959/enrollee
acasignups.net/19/09/08/exclu…
77/
acasignups.net/19/09/13/virgi…
You’re reading that correctly: Optima Health Plan has to pay back nearly $99 MILLION in excess premiums to their 57,000 enrollees.
That’s an AVERAGE of $1,739 apiece.
This is no coincidence.
78/
acasignups.net/17/09/26/virgi…
79/
acasignups.net/18/09/17/virgi…
80/
This left them with a 64% 3-year average MLR…thus, they have to pay $99 million back.
81/
I don’t do this often these days, but if you find my work useful & can afford to do so, please consider supporting it, thanks!
acasignups.net/donate
/END